Abstract
Background
Observational studies have shown that Helicobacter pylori (H. pylori) infection and H. pylori antibodies are associated with an increased risk of stroke. However, which and how H. pylori antibodies serve as the causal determinant of the development of stroke remains largely unknown.
Methods
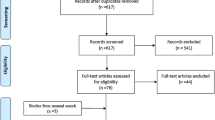
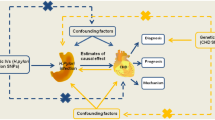
Genome-wide association studies (GWAS) on seven different antibodies of H. pylori-specific proteins, stroke, and stroke subtypes were included in this study. Mendelian randomization (MR) and multivariable MR (MVMR) analysis were performed to assess the causal associations between H. pylori antibodies and the development of stroke and to determine the potential mechanisms underlying the associations.
Results
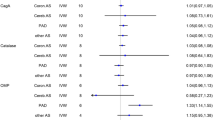
Genetically predicted serum H. pylori vacuolating cytotoxin-A (VacA) antibody level was associated with an increased risk of all-cause stroke (odds ratio [OR] = 1.04, 95% CI 1.01–1.07, P = 0.017) and cardioembolic stroke (CES, OR = 1.11, 95% CI 1.04–1.18, P = 0.001). The results of multivariable MR (MVMR) showed that C-reactive protein (CRP), but not monocyte chemoattractant protein-1 and peptic ulcer, mediated the causal effects of VacA-positive H. pylori infection on all-cause stroke and CES. No strong causal associations were found between other H. pylori antibodies and stroke and its subtypes.
Conclusions
Our results demonstrate that H. pylori VacA antibody is the only causal determinant associated with the risk of stroke in the spectrum of H. pylori-related antibodies, in which CRP may mediate the association. This study suggests that inhibition of the CRP signaling pathway may reduce the risk of stroke in patients with VacA-positive H. pylori infection.


Similar content being viewed by others
Data availability
The GWAS summary statistics data used in this MR study is available in OpenGWAS (https://gwas.mrcieu.ac.uk/) and Catalog GWAS (https://www.ebi.ac.uk/gwas/home/).
References
Feigin VL, Brainin M, Norrving B, Martins S, Sacco RL, Hacke W, et al. World Stroke Organization (WSO): global stroke fact sheet 2022. Int J Stroke. 2022;17:18–29.
Naghavi M, Abajobir AA, Abbafati C, Abbas KM, Abd-Allah F, Abera SF, et al. Global, regional, and national age-sex specific mortality for 264 causes of death, 1980–2016: a systematic analysis for the Global Burden of Disease Study 2016. The Lancet. 2017;390:1151–210.
Kumar KP, Wong CH. Imbalance in the force: the dark side of the microbiota on stroke risk and progression. Curr Opin Neurobiol. 2020;62:10–6.
Shindler-Itskovitch T, Chodick G, Shalev V, Muhsen K. Helicobacter pylori infection and prevalence of stroke. Helicobacter. 2019;24: e12553.
Mezmale L, Coelho LG, Bordin D, Leja M. Review: epidemiology of Helicobacter pylori. Helicobacter. 2020;25(Suppl 1): e12734.
Hooi JKY, Lai WY, Ng WK, Suen MMY, Underwood FE, Tanyingoh D, et al. Global prevalence of Helicobacter pylori infection: systematic review and meta-analysis. Gastroenterology. 2017;153:420–9.
Yuan C, Adeloye D, Luk TT, Huang L, He Y, Xu Y, et al. The global prevalence of and factors associated with Helicobacter pylori infection in children: a systematic review and meta-analysis. Lancet Child Adolesc Health. 2022;6:185–94.
Butler-Laporte G, Kreuzer D, Nakanishi T, Harroud A, Forgetta V, Richards JB. Genetic determinants of antibody-mediated immune responses to infectious diseases agents: a genome-wide and HLA association study. In Open forum infectious diseases. 2020; Oxford University Press US. ofaa450.
Nejati S, Karkhah A, Darvish H, Validi M, Ebrahimpour S, Nouri HR. Influence of Helicobacter pylori virulence factors CagA and VacA on pathogenesis of gastrointestinal disorders. Microb Pathog. 2018;117:43–8.
Longo-Mbenza B, Nsenga JN, Mokondjimobe E, Gombet T, Assori IN, Ibara JR, et al. Helicobacter pylori infection is identified as a cardiovascular risk factor in Central Africans. Vascular Health Risk Manag. 2012;8:455.
Yang X, Gao Y, Zhao X, Tang Y, Su Y. Chronic Helicobacter pylori infection and ischemic stroke subtypes. Neurol Res. 2011;33:467–72.
Yu M, Zhang Y, Yang Z, Ding J, Xie C, Lu N. Association between Helicobacter pylori infection and stroke: a meta-analysis of prospective observational studies. J Stroke Cerebrovasc Dis. 2014;23:2233–9.
Doheim MF, Altaweel AA, Elgendy MG, Elshanbary AA, Dibas M, Ali AAHA, et al. Association between Helicobacter pylori infection and stroke: a meta-analysis of 273,135 patients. J Neurol. 2021;268:3238–48.
Fewell Z, Davey Smith G, Sterne JA. The impact of residual and unmeasured confounding in epidemiologic studies: a simulation study. Am J Epidemiol. 2007;166:646–55.
Xu Z, Wang L, Lin Y, Wang Z, Zhang Y, Li J, et al. The impacts of peptic ulcer on stroke recurrence. J Stroke Cerebrovasc Dis. 2018;27:2106–11.
Kelly PJ, Lemmens R, Tsivgoulis G. Inflammation and stroke risk: a new target for prevention. Stroke. 2021;52:2697–706.
Emdin CA, Khera AV, Kathiresan S. Mendelian randomization. Jama. 2017;318:1925–6.
Malik R, Chauhan G, Traylor M, Sargurupremraj M, Okada Y, Mishra A, et al. Multiancestry genome-wide association study of 520,000 subjects identifies 32 loci associated with stroke and stroke subtypes. Nat Genet. 2018;50:524–37.
Woo D, Falcone GJ, Devan WJ, Brown WM, Biffi A, Howard TD, et al. Meta-analysis of genome-wide association studies identifies 1q22 as a susceptibility locus for intracerebral hemorrhage. Am J Hum Genet. 2014;94:511–21.
Ligthart S, Vaez A, Võsa U, Stathopoulou MG, De Vries PS, Prins BP, et al. Genome analyses of> 200,000 individuals identify 58 loci for chronic inflammation and highlight pathways that link inflammation and complex disorders. Am J Hum Genet. 2018;103:691–706.
Folkersen L, Gustafsson S, Wang Q, Hansen DH, Hedman ÅK, Schork A, et al. Genomic and drug target evaluation of 90 cardiovascular proteins in 30,931 individuals. Nat Metab. 2020;2:1135–48.
Guo X, Tang P, Hou C, Liu Y, Li R. Impaired pulmonary function mediates the impact of preterm birth on later-life stroke: a 2-step, multivariable Mendelian randomization study. Epidemiol Health 2023; e2023031.
Kotilea K, Bontems P, Touati E. Epidemiology, diagnosis and risk factors of Helicobacter pylori infection. Adv Exp Med Biol. 2019;1149:17–33.
Boehme AK, Esenwa C, Elkind MS. Stroke risk factors, genetics, and prevention. Circ Res. 2017;120:472–95.
Hemani G, Zheng J, Elsworth B, Wade KH, Haberland V, Baird D, et al. The MR-Base platform supports systematic causal inference across the human phenome. elife, 2018;7.
Guo X, Chong L, Zhang X, Li R. Immunosuppressants contribute to a reduced risk of Parkinson’s disease in rheumatoid arthritis. Int J Epidemiol. 2022;51:1328–38.
Verbanck M, Chen C-Y, Neale B, Do R. Detection of widespread horizontal pleiotropy in causal relationships inferred from Mendelian randomization between complex traits and diseases. Nat Genet. 2018;50:693–8.
Kang M-H, Eyun S-i, Park Y-Y. Estrogen-related receptor-gamma influences Helicobacter pylori infection by regulating TFF1 in gastric cancer. Biochem Biophys Res Commun. 2021;563:15–22.
Wang B, Yu M, Zhang R, Chen S, Xi Y, Duan G. A meta-analysis of the association between Helicobacter pylori infection and risk of atherosclerotic cardiovascular disease. Helicobacter. 2020;25: e12761.
Xiang Z, Censini S, Bayeli PF, Telford JL, Figura N, Rappuoli R, et al. Analysis of expression of CagA and VacA virulence factors in 43 strains of Helicobacter pylori reveals that clinical isolates can be divided into two major types and that CagA is not necessary for expression of the vacuolating cytotoxin. Infect Immun. 1995;63:94–8.
Palframan SL, Kwok T, Gabriel K. Vacuolating cytotoxin A (VacA), a key toxin for Helicobacter pylori pathogenesis. Front Cell Infect Microbiol. 2012;2:92.
Link A, Langner C, Schirrmeister W, Habendorf W, Weigt J, Venerito M, et al. Helicobacter pylori vacA genotype is a predominant determinant of immune response to Helicobacter pylori CagA. World J Gastroenterol. 2017;23:4712.
Pan KF, Formichella L, Zhang L, Zhang Y, Ma JL, Li ZX, et al. Helicobacter pylori antibody responses and evolution of precancerous gastric lesions in a Chinese population. Int J Cancer. 2014;134:2118–25.
Bergonzelli GE, Granato D, Pridmore RD, Marvin-Guy LF, Donnicola D, Corthésy-Theulaz IE. GroEL of Lactobacillus johnsonii La1 (NCC 533) is cell surface associated: potential role in interactions with the host and the gastric pathogen Helicobacter pylori. Infect Immun. 2006;74:425–34.
Yamaguchi H, Osaki T, Kai M, Taguchi H, Kamiya S. Immune response against a cross-reactive epitope on the heat shock protein 60 homologue of Helicobacter pylori. Infect Immun. 2000;68:3448–54.
Rustgi SD, Oh A, Hur C. Testing and treating Helicobacter pylori Infection in individuals with family history of gastric cancer is cost-effective. Gastroenterology. 2021;161(2051–2052): e2054.
Georgakis MK, Malik R, Björkbacka H, Pana TA, Demissie S, Ayers C, et al. Circulating monocyte chemoattractant protein-1 and risk of stroke: meta-analysis of population-based studies involving 17 180 individuals. Circ Res. 2019;125:773–82.
Hong S-I, Kim J-S, Bae HJ, Kim WY. C-reactive protein for stroke detection in the emergency department in patients with dizziness without neurological deficits. Front Neurol. 2021;12: 662510.
Zhang XG, Xue J, Yang WH, Xu XS, Sun HX, Hu L, et al. Inflammatory markers as independent predictors for stroke outcomes. Brain Behav. 2021;11: e01922.
Di Napoli M, Papa F, Bocola V. C-reactive protein in ischemic stroke: an independent prognostic factor. Stroke. 2001;32:917–24.
Del Giudice M, Gangestad SW. Rethinking IL-6 and CRP: Why they are more than inflammatory biomarkers, and why it matters. Brain Behav Immun. 2018;70:61–75.
Dix C, Zeller J, Stevens H, Eisenhardt SU, Shing K, Nero TL, et al. C-reactive protein, immunothrombosis and venous thromboembolism. Front Immunol. 2022;13:1002652.
Cermak J, Key NS, Bach RR, Balla J, Jacob HS, Vercellotti GM. C-reactive protein induces human peripheral blood monocytes to synthesize tissue factor. Blood. 1993;82:513–20.
Tam V, Patel N, Turcotte M, Bossé Y, Paré G, Meyre D. Benefits and limitations of genome-wide association studies. Nat Rev Genet. 2019;20:467–84.
Acknowledgements
The MEGASTROKE project received funding from sources specified at http://www.megastroke.org/acknowledgments.html. The authors thank all the participants, investigators, and consortiums who contributed to this study.
Funding
This study was supported by the Project for Sanqin Academic Innovation Team in Shaanxi Province (SQ0157) and the Fundamental Research Funds for the Central Universities, Xi’an Jiaotong University (XZY012022136). The funding agency had no role in the design, implementation or interpretation of this study.
Author information
Authors and Affiliations
Contributions
X.G. and R.L. conceived and designed the project. X.G., P.T., and X.Z. collected and analyzed the data. X.G. and P.T. drafted the manuscript. R.L. revised the manuscript. All authors approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest relevant to this article to disclose.
Ethics approval
There were no patients directly involved in the overall process of our study. This study was performed based on publicly available data and no separate ethical approval was required. All human studies included in this analysis were conducted according to the Declaration of Helsinki.
Consent for publication
All authors have read, validated the accuracy of the data, and approved the final manuscript.
Additional information
Responsible Editor: John Di Battista.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
11_2023_1740_MOESM1_ESM.xlsx
Supplementary file1 (XLSX 97 KB) Supplementary data sheet. List of harmonized instrumental variables for each exposure-outcome pair used in MR analysis.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Guo, X., Tang, P., Zhang, X. et al. Causal associations of circulating Helicobacter pylori antibodies with stroke and the mediating role of inflammation. Inflamm. Res. 72, 1193–1202 (2023). https://doi.org/10.1007/s00011-023-01740-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00011-023-01740-0