Abstract
Background
Ischemia–reperfusion injury (IRI) after lung transplantation remains a significant cause of morbidity and mortality. Lung IRI induces nitric oxide synthesis (iNOS) and reactive nitrogen species, decreasing nitric oxide bioavailability. We hypothesized that ischemia-induced iNOS intensifies with reperfusion and contributes to IRI-induced pulmonary arterial regulatory dysfunction, which may lead to early graft failure and cause pulmonary edema. The aim of this study was to determine whether ischemia–reperfusion alters inducible and endothelial nitric oxide synthase expression, potentially affecting pulmonary perfusion. We further evaluated the role of iNOS in post-transplantation pulmonary arterial disorder.
Methods
We randomized 32 Sprague–Dawley rats into two groups. The control group was given a sham operation whilst the experimental group received orthotropic lung transplants with a modified three-cuff technique. Changes in lung iNOS, and endothelial nitric oxide synthase expression were measured after lung transplantation by enzyme-linked immunosorbent assay (ELISA). Vasoconstriction in response to exogenous phenylephrine and vasodilation in response to exogenous acetylcholine of pulmonary arterial rings were measured in vitro as a measure of vascular dysfunction. To elucidate the roles of iNOS in regulating vascular function, an iNOS activity inhibitor (N6-(1-iminoethyl)-L-lysine, L-NIL) was used to treat isolated arterial rings. In order to test whether iNOS inhibition has a therapeutic effect, we further used L-NIL to pre-treat transplanted lungs and then measured post-transplantation arterial responses.
Results
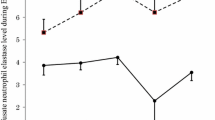
Lung transplantation caused upregulation of iNOS expression. This was also accompanied by suppression of both vasoconstriction and vasodilation of arterial rings from transplanted lungs. Removal of endothelium did not interfere with the contraction of pulmonary arterial rings from transplanted lungs. In contrast, iNOS inhibition rescued the vasoconstriction response to exogenous phenylephrine of pulmonary arterial rings from transplanted lungs. In addition, lung transplantation led to suppression of PaO2/FiO2 ratio, increased intrapulmonary shunt (Q s/Q t), and increase of lung wet to dry ratio (W/D), malondialdehyde and myeloperoxidase levels, all of which were reversed upon iNOS inhibition. Furthermore, inhibition of iNOS significantly rescued vascular function and alleviated edema and inflammatory cell infiltration in the transplanted lung.
Conclusions
Our data suggest that lung transplantation causes upregulation of iNOS expression, and pulmonary vascular dysfunction. iNOS inhibition reverses the post-transplantational pulmonary vascular dysfunction.




Similar content being viewed by others
References
Thabut G, Christie JD, Kremers WK, Fournier M, Halpern SD. Survival differences following lung transplantation among US transplant centers. JAMA. 2010;304:53–60.
Fiser SM, Tribble CG, Long SM, Kaza AK, Kern JA, Jones DR, et al. Ischemia-reperfusion injury after lung transplantation increases risk of late bronchiolitis obliterans syndrome. Ann Thorac Surg. 2002;73:1041–7 discussion 1047–8.
Reignier J, Mazmanian M, Detruit H, Chapelier A, Weiss M, Libert JM, et al. Reduction of ischemia-reperfusion injury by pentoxifylline in the isolated rat lung. Paris-Sud University Lung Transplantation Group. Am J Respir Crit Care Med. 1994;150:342–7.
Chapelier A, Reignier J, Mazmanian M, Detruit H, Dartevelle P, Parquin F, et al. Pentoxifylline and lung ischemia-reperfusion injury: application to lung transplantation. Universite Paris-Sud Lung Transplant Group. J Cardiovasc Pharmacol. 1995;25(Suppl 2):S130–3.
Yerebakan C, Ugurlucan M, Bayraktar S, Bethea BT, Conte JV. Effects of inhaled nitric oxide following lung transplantation. J Card Surg. 2009;24:269–74.
Shen W, Zhang X, Zhao G, Wolin MS, Sessa W, Hintze TH. Nitric oxide production and NO synthase gene expression contribute to vascular regulation during exercise. Med Sci Sports Exerc. 1995;27:1125–34.
Geller DA, Billiar TR. Molecular biology of nitric oxide synthases. Cancer Metastasis Rev. 1998;17:7–23.
Pfeilschifter J, Eberhardt W, Huwiler A. Nitric oxide and mechanisms of redox signalling: matrix and matrix-metabolizing enzymes as prime nitric oxide targets. Eur J Pharmacol. 2001;429:279–86.
Liu M, Tremblay L, Cassivi SD, Bai XH, Mourgeon E, Pierre AF, et al. Alterations of nitric oxide synthase expression and activity during rat lung transplantation. Am J Physiol Lung Cell Mol Physiol. 2000;278:L1071–81.
Anggard E. Nitric oxide: mediator, murderer, and medicine. Lancet. 1994;343:1199–206.
Sedoris KC, Gozal E, Ovechkin AV, Theile AR, Roberts AM. Interplay of endothelial and inducible nitric oxide synthases modulates the vascular response to ischaemia-reperfusion in the rabbit lung. Acta Physiol. 2012;204:331–43.
Ovechkin AV, Lominadze D, Sedoris KC, Robinson TW, Tyagi SC, Roberts AM. Lung ischemia-reperfusion injury: implications of oxidative stress and platelet-arteriolar wall interactions. Arch Physiol Biochem. 2007;113:1–12.
Yaylak F, Canbaz H, Caglikulekci M, Dirlik M, Tamer L, Ogetman Z, et al. Liver tissue inducible nitric oxide synthase (iNOS) expression and lipid peroxidation in experimental hepatic ischemia reperfusion injury stimulated with lipopolysaccharide: the role of aminoguanidine. J Surg Res. 2008;148:214–23.
Kadkhodaee M, Zahmatkesh M, Sadeghipour HR, Eslamifar A, Taeb J, Shams A, et al. Proteinuria is reduced by inhibition of inducible nitric oxide synthase in rat renal ischemia-reperfusion injury. Transpl Proc. 2009;41:2907–9.
Chlopicki S, Olszanecki R, Jakubowski A, Lomnicka M, Gryglewski RJ. L-N6-(1-iminoethyl)-lysine (L-NIL) but not S-methylisothiourea sulphate (SMT) displays selectivity towards NOS-2. Pol J Pharmacol. 1999;51:443–7.
Wu J, Wei J, You X, Chen X, Zhu H, Zhu X, et al. Inhibition of hydrogen sulfide generation contributes to lung injury after experimental orthotopic lung transplantation. J Surg Res. 2013;182:e25–33.
Kohn DF. Anesthesia and analgesia in laboratory animals. San Diego: Academic Press; 1997.
Sun X, Ma S, Zang YM, Lu SY, Guo HT, Bi H, et al. Vasorelaxing effect of U50,488H in pulmonary artery and underlying mechanism in rats. Life Sci. 2006;78:2516–22.
Cardell LO, Hjert O, Uddman R. The induction of nitric oxide-mediated relaxation of human isolated pulmonary arteries by PACAP. Br J Pharmacol. 1997;120:1096–100.
Anaid S, Petkov V, Baykuscheva-Gentscheva T, Hoeger H, Painsipp E, Holzer P, et al. Involvement of endothelial NO in the dilator effect of VIP on rat isolated pulmonary artery. Regul Pept. 2007;139:102–8.
Furchgott RF, Zawadzki JV. The obligatory role of endothelial cells in the relaxation of arterial smooth muscle by acetylcholine. Nature. 1980;288:373–6.
Stojic D, Radenkovic M, Krsljak E, Popovic J, Pesic S, Grbovic L. Influence of the endothelium on the vasorelaxant response to acetylcholine and vasoactive intestinal polypeptide in the isolated rabbit facial artery. Eur J Oral Sci. 2003;111:137–43.
Jin Y, Zhao X, Li H, Wang Z, Wang D. Effects of sevoflurane and propofol on the inflammatory response and pulmonary function of perioperative patients with one-lung ventilation. Exp Ther Med. 2013;6:781–5.
Alexiou K, Matschke K, Westphal A, Stangl K, Dschietzig T. Relaxin is a candidate drug for lung preservation: relaxin-induced protection of rat lungs from ischemia-reperfusion injury. J Heart Lung Transplant. 2010;29:454–60.
Yang T, Mao YF, Liu SQ, Hou J, Cai ZY, Hu JY, et al. Protective effects of the free radical scavenger edaravone on acute pancreatitis-associated lung injury. Eur J Pharmacol. 2010;630:152–7.
Papalambros E, Sigala F, Georgopoulos S, Paraskevas KI, Andreadou I, Menenakos X, et al. Malondialdehyde as an indicator of oxidative stress during abdominal aortic aneurysm repair. Angiology. 2007;58:477–82.
Dodd-o JM, Hristopoulos ML, Faraday N, Pearse DB. Effect of ischemia and reperfusion without airway occlusion on vascular barrier function in the in vivo mouse lung. J Appl Physiol. 2003;95:1971–8.
Chu Y, Wu YC, Chou YC, Chueh HY, Liu HP, Chu JJ, et al. Endothelium-dependent relaxation of canine pulmonary artery after prolonged lung graft preservation in University of Wisconsin solution: role of l-arginine supplementation. J Heart Lung Transplant. 2004;23:592–8.
Carden DL, Granger DN. Pathophysiology of ischaemia-reperfusion injury. J Pathol. 2000;190:255–66.
Fullerton DA, Mitchell MB, McIntyre RC Jr, Banerjee A, Campbell DN, Harken AH, et al. Cold ischemia and reperfusion each produce pulmonary vasomotor dysfunction in the transplanted lung. J Thorac Cardiovasc Surg. 1993;106:1213–7.
Darra E, Rungatscher A, Carcereri de Prati A, Podesser BK, Faggian G, Scarabelli T, et al. Dual modulation of nitric oxide production in the heart during ischaemia/reperfusion injury and inflammation. Thromb Haemost. 2010;104:200–6.
Sedoris KC, Ovechkin AV, Gozal E, Roberts AM. Differential effects of nitric oxide synthesis on pulmonary vascular function during lung ischemia-reperfusion injury. Arch Physiol Biochem. 2009;115:34–46.
Raj JU, Toga H, Ibe BO, Anderson J. Effects of endothelin, platelet activating factor and thromboxane A2 in ferret lungs. Respir Physiol. 1992;88:129–40.
Shirai M, Ikeda S, Min KY, Shimouchi A, Kawaguchi AT, Ninomiya I. Segmental differences in vasodilatation due to basal NO release in in vivo cat pulmonary vessels. Respir Physiol. 1999;116:159–69.
Shirai M, Shimouchi A, Kawaguchi AT, Sunagawa K, Ninomiya I. Inhaled nitric oxide: diameter response patterns in feline small pulmonary arteries and veins. Am J Physiol. 1996;270:H974–80.
Ikeda S, Shirai M, Shimouchi A, Min KY, Ohsawa N, Ninomiya I. Pulmonary microvascular responses to inhaled prostacyclin, nitric oxide, and their combination in anesthetized cats. Jpn J Physiol. 1999;49:89–98.
Watson KE, Dovi WF, Conhaim RL. Evidence for active control of perfusion within lung microvessels. J Appl Physiol. 2012;112:48–53.
Roberts AM, Slaaf DW, Joshua IG. Potentiation of pulmonary arteriolar vasoconstriction to endothelin-1 by inhibition of nitric oxide synthesis in the intact lung. Microcirculation. 1998;5:289–98.
Sauzeau V, Rolli-Derkinderen M, Lehoux S, Loirand G, Pacaud P. Sildenafil prevents change in RhoA expression induced by chronic hypoxia in rat pulmonary artery. Circ Res. 2003;93:630–7.
Delbin MA, Moraes C, Camargo E, Mussi RK, Antunes E, de Nucci G, et al. Influence of physical preconditioning on the responsiveness of rat pulmonary artery after pulmonary ischemia/reperfusion. Comp Biochem Physiol A Mol Integr Physiol. 2007;147:793–8.
Shibamoto T, Wang HG, Yamaguchi Y, Hayashi T, Saeki Y, Tanaka S, et al. Effects of thromboxane A2 analogue on vascular resistance distribution and permeability in isolated blood-perfused dog lungs. Lung. 1995;173:209–21.
Houweling B, Merkus D, Dekker MM, Duncker DJ. Nitric oxide blunts the endothelin-mediated pulmonary vasoconstriction in exercising swine. J Physiol. 2005;568:629–38.
Sauvageau S, Thorin E, Caron A, Dupuis J. Evaluation of endothelin-1-induced pulmonary vasoconstriction following myocardial infarction. Exp Biol Med (Maywood). 2006;231:840–6.
Winn R, Harlan J, Nadir B, Harker L, Hildebrandt J. Thromboxane A2 mediates lung vasoconstriction but not permeability after endotoxin. J Clin Invest. 1983;72:911–8.
Turnage RH, LaNoue JL, Kadesky KM, Meng Y, Myers SI. Thromboxane A2 mediates increased pulmonary microvascular permeability after intestinal reperfusion. J Appl Physiol. 1997;82:592–8.
Friedman M, Johnson RG, Wang SY, Dai HB, Thurer RL, Weintraub RM, et al. Pulmonary microvascular responses to protamine and histamine. Effects of cardiopulmonary bypass. J Thorac Cardiovasc Surg. 1994;108:1092–9.
Coggins MP, Bloch KD. Nitric oxide in the pulmonary vasculature. Arterioscler Thromb Vasc Biol. 2007;27:1877–85.
Liaudet L, Soriano FG, Szabo C. Biology of nitric oxide signaling. Crit Care Med. 2000;28:N37–52.
Rubbo H, Tarpey M, Freeman BA. Nitric oxide and reactive oxygen species in vascular injury. Biochem Soc Symp. 1995;61:33–45.
Ilangovan G, Osinbowale S, Bratasz A, Bonar M, Cardounel AJ, Zweier JL, et al. Heat shock regulates the respiration of cardiac H9c2 cells through upregulation of nitric oxide synthase. Am J Physiol Cell Physiol. 2004;287:C1472–81.
Kupatt C, Dessy C, Hinkel R, Raake P, Daneau G, Bouzin C, et al. Heat shock protein 90 transfection reduces ischemia-reperfusion-induced myocardial dysfunction via reciprocal endothelial NO synthase serine 1177 phosphorylation and threonine 495 dephosphorylation. Arterioscler Thromb Vasc Biol. 2004;24:1435–41.
Fujimura N, Jitsuiki D, Maruhashi T, Mikami S, Iwamoto Y, Kajikawa M, et al. Geranylgeranylacetone, heat shock protein 90/AMP-activated protein kinase/endothelial nitric oxide synthase/nitric oxide pathway, and endothelial function in humans. Arterioscler Thromb Vasc Biol. 2012;32:153–60.
Takahashi S, Mendelsohn ME. Calmodulin-dependent and -independent activation of endothelial nitric-oxide synthase by heat shock protein 90. J Biol Chem. 2003;278:9339–44.
Ovechkin AV, Lominadze D, Sedoris KC, Gozal E, Robinson TW, Roberts AM. Inhibition of inducible nitric oxide synthase attenuates platelet adhesion in subpleural arterioles caused by lung ischemia-reperfusion in rabbits. J Appl Physiol. 2005;99:2423–32.
Chatterjee PK, Patel NS, Kvale EO, Cuzzocrea S, Brown PA, Stewart KN, et al. Inhibition of inducible nitric oxide synthase reduces renal ischemia/reperfusion injury. Kidney Int. 2002;61:862–71.
Wei T, Chen C, Hou J, Xin W, Mori A. Nitric oxide induces oxidative stress and apoptosis in neuronal cells. Biochim Biophys Acta. 2000;1498:72–9.
Gursoy-Ozdemir Y, Bolay H, Saribas O, Dalkara T. Role of endothelial nitric oxide generation and peroxynitrite formation in reperfusion injury after focal cerebral ischemia. Stroke. 2000;31:1974–80 discussion 1981.
Hirabayashi H, Takizawa S, Fukuyama N, Nakazawa H, Shinohara Y. Nitrotyrosine generation via inducible nitric oxide synthase in vascular wall in focal ischemia-reperfusion. Brain Res. 2000;852:319–25.
Lakshminrusimha S, Suresh MV, Knight PR, Gugino SF, Davidson BA, Helinski JD, et al. Role of pulmonary artery reactivity and nitric oxide in injury and inflammation following lung contusion. Shock. 2013;39:278–85.
Joles JA, Vos IH, Grone HJ, Rabelink TJ. Inducible nitric oxide synthase in renal transplantation. Kidney Int. 2002;61:872–5.
Goldstein S, Merenyi G. The chemistry of peroxynitrite: implications for biological activity. Methods Enzymol. 2008;436:49–61.
Feelisch M. The chemical biology of nitric oxide: an outsider’s reflections about its role in osteoarthritis. Osteoarthritis Cartilage. 2008;16(Suppl 2):S3–13.
Wolin MS. Interactions of oxidants with vascular signaling systems. Arterioscler Thromb Vasc Biol. 2000;20:1430–42.
Balazy M, Kaminski PM, Mao K, Tan J, Wolin MS. S-Nitroglutathione, a product of the reaction between peroxynitrite and glutathione that generates nitric oxide. J Biol Chem. 1998;273:32009–15.
Shah MR, Wedgwood S, Czech L, Kim GA, Lakshminrusimha S, Schumacker PT, et al. Cyclic stretch induces inducible nitric oxide synthase and soluble guanylate cyclase in pulmonary artery smooth muscle cells. Int J Mol Sci. 2013;14:4334–48.
Koesling D, Russwurm M, Mergia E, Mullershausen F, Friebe A. Nitric oxide-sensitive guanylyl cyclase: structure and regulation. Neurochem Int. 2004;45:813–9.
Zheng B, Zheng T, Wang L, Chen X, Shi C, Zhao S. Aminoguanidine inhibition of iNOS activity ameliorates cerebral vasospasm after subarachnoid hemorrhage in rabbits via restoration of dysfunctional endothelial cells. J Neurol Sci. 2010;295:97–103.
Acknowledgments
The authors thank Dr. Wei-gang Guo, Dr. Qiang Tan and Yi-qingYang for their advice and helpful suggestions. This work was supported by Shanghai Natural Science Foundation No. 12ZR1428700, “1050” Foundation for the Talents by Shanghai Chest Hospital and Shanghai Joint development project for Municipal hospitals (SHDC12010222).
Dr. Wu and Zhu contributed equally to this work.
Author information
Authors and Affiliations
Corresponding author
Additional information
Responsible Editor: John Di Battista.
Rights and permissions
About this article
Cite this article
Wu, Jx., Zhu, Hw., Chen, X. et al. Inducible nitric oxide synthase inhibition reverses pulmonary arterial dysfunction in lung transplantation. Inflamm. Res. 63, 609–618 (2014). https://doi.org/10.1007/s00011-014-0733-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00011-014-0733-5