Abstract
Objective
This study was designed to detect the role of Toll-like receptor 4 (TLR4) signaling in the dysfunction of cardiac microvascular endothelial cells (CMECs) after hypoxia/reoxygenation (H/R).
Methods
The cell viability of CMECs was measured by MTT assay. The migration of CMECs was detected by cell scratch wound assay. The expressions of TLR4, nuclear factor-kappa B (NF-κB) and eNOS were analyzed by Western blot. Secretions of nitric oxide (NO) and tumor necrosis factor-alpha (TNF-α) and interleukin-6 (IL-6) were determined by NO detection kit and ELISA.
Results
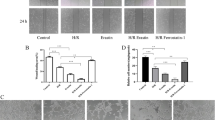
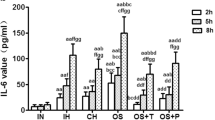
Lipopolysaccharide (LPS) incubation increased the expressions of TLR4, NF-κB, IL-6 and TNF-α in CMECs (P < 0.05 vs. control). The CMECs after H/R injury had impaired cell viability (P < 0.01 vs. control) and migration ability (P < 0.05 vs. control). Moreover, the expressions of TLR4, NF-κB, IL-6 and TNF-α were elevated after H/R in CMECs (P < 0.01 vs. control), while NO and the eNOS expression were significantly decreased. In contrast, administration of the TLR4-neutralizing antibody MTS510 prior to H/R injury down-regulated the expressions of IL-6 and TNF-α and attenuated the dysfunction of CMECs.
Conclusion
TLR4 and its signaling components can be activated by LPS and H/R in CMECs. Blocking the TLR4 signal pathway before H/R injury attenuates CMEC dysfunction.





Similar content being viewed by others
References
Sohn HY, Krotz F, Gloe T, Keller M, Theisen K, Klauss V, et al. Differential regulation of xanthine and NAD(P)H oxidase by hypoxia in human umbilical vein endothelial cells. Role of nitric oxide and adenosine. Cardiovasc Res. 2003;58:638–46.
Sodha NR, Boodhwani M, Clements RT, Feng J, Xu SH, Sellke FW. Coronary microvascular dysfunction in the setting of chronic ischemia is independent of arginase activity. Microvasc Res. 2008;75:238–46.
Li J-M, Mullen AM, Shah AM. Phenotypic properties and characteristics of superoxide production by mouse coronary microvascular endothelial cells. J Mol Cell Cardiol. 2001;33:1119–31.
Scarabelli T, Stephanou A, Rayment N, Pasini E, Comini L, Curello S, et al. Apoptosis of endothelial cells precedes myocyte cell apoptosis in ischemia/reperfusion injury. Circulation. 2001;104:253–6.
Rossig L, Dimmeler S, Zeiher AM. Apoptosis in the vascular wall and atherosclerosis. Basic Res Cardiol. 2001;96:11–22.
Akira S. Toll-like receptor signaling. J Biol Chem. 2003;278:38105–8.
Johnson GB, Brunn GJ, Platt JL. Activation of mammalian toll-like receptors by endogenous agonists. Crit Rev Immunol. 2003;23:15.
Kaczorowski DJ, Nakao A, Mollen KP, Vallabhaneni R, Sugimoto R, Kohmoto J, et al. Toll-like receptor 4 mediates the early inflammatory response after cold ischemia/reperfusion. Transplantation. 2007;84:1279–87.
Cha J, Wang Z, Ao L, Zou N, Dinarello CA, Banerjee A, et al. Cytokines link toll-like receptor 4 signaling to cardiac dysfunction after global myocardial ischemia. Ann Thorac Surg. 2008;85:1678–85.
Takeishi Y, Kubota I. Role of Toll-like receptor mediated signaling pathway in ischemic heart. Front Biosci. 2009;14:2553–8.
Chao W. Toll-like receptor signaling: a critical modulator of cell survival and ischemic injury in the heart. Am J Physiol Heart Circ Physiol. 2009;296:H1–12.
Oyama J Jr, Blais C, Liu X, Pu M, Kobzik L, Kelly RA, et al. Reduced myocardial ischemia-reperfusion injury in Toll-like receptor 4-deficient mice. Circulation. 2004;109:784–9.
Kim SC, Ghanem A, Stapel H, Tiemann K, Knuefermann P, Hoeft A, et al. Toll-like receptor 4 deficiency: smaller infarcts, but no gain in function. BMC Physiol. 2007;7:5.
Stapel H, Kim SC, Osterkamp S, Knuefermann P, Hoeft A, Meyer R, et al. Toll-like receptor 4 modulates myocardial ischaemia-reperfusion injury: role of matrix metalloproteinases. Eur J Heart Fail. 2006;8:665–72.
Shimamoto A, Chong AJ, Yada M, Shomura S, Takayama H, Fleisig AJ, et al. Inhibition of toll-like receptor 4 with eritoran attenuates myocardial ischemia–reperfusion injury. Circulation. 2006;114:I270–4.
Curtiss LK, Tobias PS. Emerging role of toll-like receptors in atherosclerosis. J Lipid Res. 2009;50(Suppl):S340–5.
Erickson B, Sperber K, Frishman WH. Toll-like receptors: new therapeutic targets for the treatment of atherosclerosis, acute coronary syndromes, and myocardial failure. Cardiol Rev. 2008;16:273–9.
Riad A, Jager S, Sobirey M, Escher F, Yaulema-Riss A, Westermann D, et al. Toll-like receptor-4 modulates survival by induction of left ventricular remodeling after myocardial infarction in mice. J Immunol. 2008;180:6954–61.
Satoh M, Shimoda Y, Maesawa C, Akatsu T, Ishikawa Y, Minami Y, et al. Activated toll-like receptor 4 in monocytes is associated with heart failure after acute myocardial infarction. Int J Cardiol. 2006;109:226–34.
Methe H, Kim JO, Kofler S, Weis M, Nabauer M, Koglin J. Expansion of circulating toll-like receptor 4-positive monocytes in patients with acute coronary syndrome. Circulation. 2005;111:2654–61.
Nishida M, Carley WW, Gerritsen ME, Ellingsen O, Kelly RA, Smith TW. Isolation and characterization of human and rat cardiac microvascular endothelial cells. Am J Physiol. 1993;264:H639–52.
Wei L, Yin Z, Yuan Y, Hwang A, Lee A, Sun D, et al. A PKC-beta inhibitor treatment reverses cardiac microvascular barrier dysfunction in diabetic rats. Microvasc Res. 2010;80:158–65.
Hu Q, Ziegelstein RC. Hypoxia/reoxygenation stimulates intracellular calcium oscillations in human aortic endothelial cells. Circulation. 2000;102:2541–7.
Yin T, Ma X, Zhao L, Cheng K, Wang H. Angiotensin II promotes NO production, inhibits apoptosis and enhances adhesion potential of bone marrow-derived endothelial progenitor cells. Cell Res. 2008;18:792–9.
Yang B, Graham L, Dikalov S, Mason RP, Falck JR, Liao JK, et al. Overexpression of cytochrome P450 CYP2J2 protects against hypoxia-reoxygenation injury in cultured bovine aortic endothelial cells. Mol Pharmacol. 2001;60:310–20.
Wei L, Sun D, Yin Z, Yuan Y, Hwang A, Zhang Y, et al. A PKC-beta inhibitor protects against cardiac microvascular ischemia reperfusion injury in diabetic rats. Apoptosis. 2010;15:488–98.
Faure E, Thomas L, Xu H, Medvedev A, Equils O, Arditi M. Bacterial lipopolysaccharide and IFN-gamma induce toll-like receptor 2 and Toll-like receptor 4 expression in human endothelial cells: role of NF-kappa B activation. J Immunol. 2001;166:2018–24.
Ichikawa H, Flores S, Kvietys PR, Wolf RE, Yoshikawa T, Granger DN, et al. Molecular mechanisms of anoxia/reoxygenation-induced neutrophil adherence to cultured endothelial cells. Circ Res. 1997;81:922–31.
Lum H, Barr DA, Shaffer JR, Gordon RJ, Ezrin AM, Malik AB. Reoxygenation of endothelial cells increases permeability by oxidant-dependent mechanisms. Circ Res. 1992;70:991–8.
Frantz S, Ertl G, Bauersachs J. Mechanisms of disease: Toll-like receptors in cardiovascular disease. Nat Clin Pract Cardiovasc Med. 2007;4:444–54.
Thompson JE, Phillips RJ, Erdjument-Bromage H, Tempst P, Ghosh S. I kappa B-beta regulates the persistent response in a biphasic activation of NF-kappa B. Cell. 1995;80:573–82.
Schmidt C, Peng B, Li Z, Sclabas GM, Fujioka S, Niu J, et al. Mechanisms of proinflammatory cytokine-induced biphasic NF-kappaB activation. Mol Cell. 2003;12:1287–300.
Frantz S, Kobzik L, Kim YD, Fukazawa R, Medzhitov R, Lee RT, et al. Toll4 (TLR4) expression in cardiac myocytes in normal and failing myocardium. J Clin Invest. 1999;104:271–80.
Acknowledgments
This study was supported by grants from the National Natural Science Foundation of China (NSFC, No. 30970845, 30770784) and Xijing Research Boosting Program (No. XJZT08Z04 XJZT07Z05).
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Responsible Editor: Kumar Visvanathan.
Z. Zhang, W. Li and D. Sun contributed equally to this work.
Rights and permissions
About this article
Cite this article
Zhang, Z., Li, W., Sun, D. et al. Toll-like receptor 4 signaling in dysfunction of cardiac microvascular endothelial cells under hypoxia/reoxygenation. Inflamm. Res. 60, 37–45 (2011). https://doi.org/10.1007/s00011-010-0232-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00011-010-0232-2