Abstract
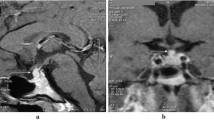
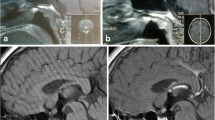
Central nervous system (CNS) involvement and, in particular, hypothalamic-pituitary involvement are well described features of Langerhans cell histiocytosis (LCH). The actual incidence of CNS-LCH disease is unknown and the natural history is poorly understood. Diabetes insipidus (DI) is reported to be the most common and well described manifestation of hypothalamic-pituitary involvement (up to 50%). Anterior pituitary dysfunction has been reported in up to 20% of patients with LCH, and occurs almost exclusively concurrently with DI. In the current paper we describe our experience with 7 patients (6 females and 1 male) in whom hypothalamic-pituitary involvement was a major feature of LCH. Diagnosis was made in 4 patients during childhood or adolescence, and 3 patients were over 18 years old at the time of diagnosis. Our series exemplifies the wide spectrum of LCH-induced hypopituitarism, and demonstrates some unique features, including a higher incidence of CRH/ACTH deficiency compared to other reports (4/7 patients), and massive obesity in 2 of our patients. Endocrine function was not improved in any of our patients following medical treatment of LCH with chemotherapy and glucocorticoids. We conclude that pituitary-hypothalamic dysfunction is a common feature of LCH, and therefore all LCH patients should undergo a thorough endocrine evaluation periodically.
Similar content being viewed by others
References
Schmitz L., Favara B.E. Nosology and pathology of Langerhans cell histiocytosis. Hematol. Oncol. Clin. North Am. 1998, 12: 221–245.
Willman C.L., McClain K.L. An update on clonality, cytokines, and viral etiology in Langerhans cell histiocytosis. Hematol. Oncol. Clin. North Am. 1998, 12: 407–416.
Nicholson H.S., Egeler R.M., Nesbit M.E. The epidemiology of Langerhans cell histiocytosis. Hematol. Oncol. Clin. North Am. 1998, 12: 379–384.
Arico M., Egeler M. Clinical aspects of Langerhans cell histiocytosis. Hematol. Oncol. Clin. North Am. 1998, 12: 247–258.
Malpas J.S. Langerhans cell histiocytosis in adults. Hematol. Oncol. Clin. North Am. 1998, 12: 259–268.
Lieberman P.H., Jones C.R., Steinman R.M., Erlandson R.A., Smith J., Gee T., Huvos A., Garin-Chesa P., Filipa D.A., Urmacher C., Gangi M.D., Sperber M. Langerhans cell (eosinophilic) granulomatosis. Am. J. Surg. Pathol. 1996, 20: 519–552.
Favara B.E., Feller A.C., and members of the WHO committee on histiocytic/reticulum cell proliferations. Contemporary classification of histiocytic disorders. Med. Pediatr. Oncol. 1997, 29: 157–166.
Grois N.G., Favara B.E., Mostbeck G.H., Prayer D. Central nervous system involvement in Langerhans cell histiocytosis. Hematol. Oncol. Clin. North Am. 1998, 12: 287–305.
Grois N., Flucher-Wolfram B., Heitger A., Mostbeck G.H., Hofmann J., Gadner H. Diabetes insipidus in Langerhans cell histiocytosis: results from the DAL-HX study. Med. Pediatr. Oncol. 1995, 24: 248–256.
Kilpatrick S.E., Wenger D.E., Gilchrist G.S., Shives T.C., Wollan P.C., Unni K.K. Langerhans cell histiocyosis (histiocytosis X) of bone. Cancer 1995, 76: 2471–2484.
Maghnie M., Genovese E., Arico M., Villa A., Beluffi G., Campani R., Severi F. Evolving pituitary hormone deficiency is associated with pituitary vasculopathy: dynamic MR study in children with hypopituitarism, diabetes insipidus, and Langerhans cell histiocytosis. Radiology 1994, 193: 493–499.
Rosenzweig K.E., Arceci R.J., Tarbell N.J. Diabetes insipidus secondary to Langerhans cell histiocytosis: is radiation therapy indicated? Med. Pediatr. Oncol. 1997, 29: 36–40.
Donadieu J., for the French LCH Study Group. A multicenter retrospective survey of Langerhans cell histiocytosis: 348 cases observed between 1983 and 1993. Arch. Dis. Child. 1996, 75: 17–24.
Broadbent V., Gadner H. Current therapy for Langerhans cell histiocytosis. Hematol. Oncol. Clin. North Am. 1998, 12: 327–338.
Braunstein G.D., Kohler P.O. Endocrine manifestations of histiocytosis. Am. J. Pediatr. Hematol. Oncol. 1981, 3: 67–75.
Latorre H., Kennedy F.M., Lahey M.E., Drash A. Short stature and growth hormone deficiency in histiocytosis X. J. Pediatr. 1974, 85: 813–816.
Sims D.G. Histiocytosis X. Follow-up of 43 cases. Arch. Dis. Child. 1977, 52: 433–440.
Maghnie M., Bossi G., Klersy C., Cosi G., Genovese E., Arico M. Dynamic endocrine testing and magnetic resonance imaging in the long term follow-up of childhood Langerhans cell histiocytosis. J. Clin. Endocrinol. Metab. 1998, 83: 3089–3094.
Willis B., Ablin A., Weinberg V., Zoger S., Wara W.M., Matthay K.K. Disease course and late sequelae of Langerhans cell histiocytosis: 25-year experience at the university of California, San Francisco. J. Clin. Oncol. 1996, 14: 2073–2082.
Bernard J.D., Aguilar M.J. Localized hypothalamic histiocytosis X. Arch. Neurol. 1969, 20: 368–372.
Smolic E.A., Devecerski M., Nelson J.S., Smith K.R. Jr. Histiocytosis X in the optic chiasm of an adult with hypopituitarism: case report. J. Neurosurg. 1968, 24: 290–295.
Rami B., Schneider U., Wandl-Vergesslich K., Frisch H., Schober E. Primary hypothyroidism, central diabetes insipidus and growth hormone deficiency in multisystem Langerhans cell histiocytosis: a case report. Acta Paediatr. 1998, 87: 112–114.
Kitahama S., Iitaka M., Shimizu T., Serizawa N., Fukasawa N., Miura S., Kawasaki S., Yamanaka K., Kawakami Y., Murakami S., Ishii J., Katayama S. Thyroid involvement by malignant histiocytosis of Langerhans’ cell type. Clin. Endocrinol. (Oxf.) 1996, 45: 357–363.
Bernert G., Broadbent V., Czech T., D’angio G., Egeler M., Favara B.E., Grois N. Report of the histiocyte society workshop on “central nervous system (CNS) disease in Langerhans cell histiocytosis (LCH)”. Med. Pediatr. Oncol. 1997, 29: 73–78.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Modan-Moses, D., Weintraub, M., Meyerovitch, J. et al. Hypopituitarism in Langerhans cell histiocytosis: Seven cases and literature review. J Endocrinol Invest 24, 612–617 (2001). https://doi.org/10.1007/BF03343902
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/BF03343902