Abstract
Purpose
This study assessed the effect of oxygen affinity and molecular weight (MW) of o-raffinose cross-linked hemoglobin based oxygen carriers (HBOCs) on cerebral oxygen delivery and mean arterial blood pressure (MAP) following hemorrhage and resuscitation in rats.
Methods
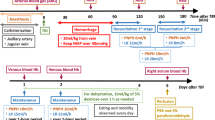
Isoflurane anesthetized rats (n = 6-7 per group) underwent 30% hemorrhage and resuscitation with an equivalent volume of one of three different HBOCs: 1) High P50 Poly o-raffinose hemoglobin (Poly OR-Hb, P50 = 70 mmHg); 2) High P50 > 128 Poly OR-Hb (MW > 128 kDa, P50 = 70 mmHg) and 3) Low P50 > 128 Poly OR-Hb (MW > 128 kDa, P50 = 11 mmHg). Hippocampal cerebral tissue oxygen tension, regional cerebral blood flow (rCBF), MAP, total hemoglobin concentration and arterial blood gases were measured. Data analysis by two-way ANOVA and post hoc Tukey tests determined significance (P < 0.05, mean ± SD).
Results
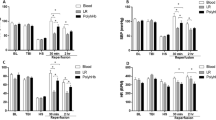
Hippocampal tissue oxygen tension increased in all HBOC groups following resuscitation. The rCBF remained unchanged after HBOC resuscitation in all groups. Following resuscitation, the peak MAP was higher in the High P50 Poly OR-Hb group ( 152 ± 13 mmHg) when compared to either the Low or High P50 large MW, (> 128 kDa) HBOC group (119 ± 15 mmHg or 127 ± 18 respectively, P < 0.05 for both).
Conclusions
O-raffinose polymerized HBOC, with or without lower MW components, maintained cerebral tissue oxygen delivery following hemorrhage and resuscitation in rats. The higher MW HBOCs showed a decrease in peak MAP, which did not alter oxygen delivery. No significant effect of oxygen affinity on cerebral tissue oxygen tension or blood flow was observed.
Résumé
Objectif
Évaluer l’effet de l’affinité pour l’oxygène et du poids moléculaire (PM) des transporteurs d’oxygène à base d’hémoglobine (TOBH) avec o-raffinose sur l’apport d’oxygène cérébral et la tension artérielle moyenne (TAM) après une hémorragie et une réanimation chez des rats.
Méthode
Des rats anesthésiés à l’isoflurane (n = 6-7 par groupe) ont subi une hémorragie à 30% et une réanimation avec un volume équivalent de l’un des trois différents TOBH suivants : 1) de l’hémoglobine Poly o-raffinose à P50 élevé (Poly OR-Hb, P50 = 70 mmHg) ; 2) 128 Poly OR-Hb à P50 élevé (PM > 128 kDa, P50 = 70 mmHg) et 3) 128 Poly OR-Hb à faible P50 (PM > 128 kDa, P50 = 1 1 mmHg). La tension en oxygène du tissu cérébral hippocampique, le débit sanguin cérébral régional (DSCr), la TAM, la concentration d’hémoglobine totale et la gazométrie du sang artériel ont été mesurés. L’analyse de données, par double ANOVA et tests de Tukey ultérieur, ont permis de déterminer la valeur significative (P < 0,05, moyenne ± SD).
Résultats
La tension en oxygène du tissu hippocampique s’est accrue dans tous les groupes de TOBH après la réanimation. Le DSCr est resté le même dans tous les groupes après la réanimation avec les TOBH. Après la réanimation, la TAM était plus élevée dans le groupe Poly OR-Hb à P50 élevé (152 ± 13 mmHg) comparé au groupe de TOBH de P50 élevé et de grand PM, (> 128 kDa) (119 ± 15 mmHg ou 127 ± 18 respectivement, P < 0,05 pour les deux).
Conclusion
Les TOBH polymérisés avec o-raffinose, avec ou sans composants de faible PM, ont maintenu l’apport d’oxygène au tissu cérébral après une hémorragie et une réanimation chez des rats. Les TOBH de PM élevé ont montré une baisse de la TAM qui n’a pas nui à l’apport d’oxygène. Aucun effet significatif de l’affinité pour l’oxygène sur la tension en oxygène du tissu cérébral ou sur le débit sanguin n’a été observé.
Article PDF
Similar content being viewed by others
References
Carson JL, Poses RM, Spence RK, Bonavita G. Severity of anaemia and operative mortality and morbidity. Lancet 1988; 1:727–9.
Dunne JR, Malone D, Tracy JK, Gannon C, Napolitano LM. Perioperative anemia: an independent risk factor for infection, mortality, and resource utilization in surgery. J Surg Res 2002; 102:237–44.
Jonas RA, Wypij D, Roth SJ, et al. The influence of hemodilution on outcome after hypothermic cardiopulmonary bypass: results of a randomized trial in infants. J Thorac Cardiovasc Surg 2003; 126:1765–74.
Malone DL, Dunne J, Tracy JK, Putnam AT, Scalea TM, Napolitano LM. Blood transfusion, independent of shock severity, is associated with worse outcome in trauma. J Trauma 2003; 54:898–905.
Gould SA, Moore EE, Hoyt DB, et al. The first randomized trial of human polymerized hemoglobin as a blood substitute in acute trauma and emergent surgery. J Am Coll Surg 1998; 187:113–20.
Levy JH, Goodnough LT, Greilich PE, et al. Polymerized bovine hemoglobin solution as a replacement for allogeneic red blood cell transfusion after cardiac surgery: results of a randomized, double-blind trial. J Thorac Cardiovasc Surg 2002; 124:35–42.
Cheng DC, Mazer CD, Martineau R, et al. A phase II dose-response study of hemoglobin raffimer (Hemolink) in elective coronary artery bypass surgery. J Thorac Cardiovasc Surg 2004; 127:79–86.
Greenburg AG, Kim HW. Use of an oxygen therapeutic as an adjunct to intraoperative autologous donation to reduce transfusion requirements in patients undergoing coronary artery bypass graft surgery. J Am Coll Surg 2004; 198:373–83.
Sloan EP, Koenigsberg M, Gens D, et al. Diaspirin cross-linked hemoglobin (DCLHb) in the treatment of severe traumatic hemorrhagic shock: a randomized controlled efficacy trial. JAMA 1999; 282:1857–64.
GulatiA, Singh R, Chung SM, Sen AP. Role of endothelin-converting enzyme in the systemic hemodynamics and regional circulatory effects of proendothelin-1 (1-38) and diaspirin cross-linked hemoglobin in rats. J Lab Clin Med 1995; 126:559–70.
Saxena R, Wijnhoud AD, Man in ’t Veld AJ, et al. Effect of diaspirin cross-linked hemoglobin on endo- thelin-1 and blood pressure in acute ischemic stroke in man. J Hypertens 1998; 16:1459–65.
Gulati A, Rebello Sen AP. Role of adrenergic mechanisms in the pressor effect of diaspirin cross-linked hemoglobin. J Lab Clin Med 1994; 124:125–33.
Asano Y, Koehler RC, Ulatowski JA, Traystman RJ, Bucci E. Effect of cross-linked hemoglobin transfusion on endothelial-dependent dilation in cat pial arterioles. Am J Physiol 1998; 275:H1313–21.
von Dobschuetz E, Hutter J, Hoffmann T, Messmer K. Recombinant human hemoglobin with reduced nitric oxide-scavenging capacity restores effectively pancreatic microcirculatory disorders in hemorrhagic shock. Anesthesiology 2004; 100:1484–90.
Winslow RM, Gonzales A, Gonzales ML, et al. Vascular resistance and the efficacy of red cell substitutes in a rat hemorrhage model. J Appl Physiol 1998; 85:993- 1003.
Lieberthal W, Fuhro R, Freedman JE, Toolan G, Loscalzo J, Valeri CR. O-raffinose cross-linking markedly reduces systemic and renal vasoconstrictor effects of unmodified human hemoglobin. J Pharmacol Exp Ther 1999; 288:1278–87.
Conover CD, Linberg R, Shum KL, Shorr RG. The ability of polyethylene glycol conjugated bovine hemoglobin (PEG-Hb) to adequately deliver oxygen in both exchange transfusion and top-loaded rat models. Artif Cells Blood Substit Immobil Biotechnol 1999; 27:93–107.
Vaslef SN, Kaminski BJ, Talarico TL. Oxygen transport dynamics of acellular hemoglobin solutions in an iso- volemic hemodilution model in swine. J Trauma 2001; 51:1153–60.
Sakai H, Tsai AG, Rohlfs RJ, et al. Microvascular responses to hemodilution with Hb vesicles as red blood cell substitutes: influence of O2 affinity. Am J Physiol 1999; 276:H553–62.
Cabrales P, Sakai H, Tsai AG, Takeoka S, Tsuchida E, Intaglietta M. Oxygen transport by low and normal P50 hemoglobin-vessicles in extreme hemodilution. Am J Physiol 2004; 288:H1885–92.
Richardson RS, Tagore K, Haseler LJ, Jordan M, Wagner PD. Increased VO2 max with right-shifted Hb-O2 dissociation curve at a constant O2 delivery in dog muscle in situ. J Appl Physiol 1998; 84:995- 1002.
Carmichael FJ, Ali AC, Campbell J A, et al. A phase I study of oxidized raffinose cross-linked human hemoglobin. Crit Care Med 2000; 28:2283–92.
Hare GMT, Hum KM, Kim SY, Barr A, Baker AJ, Mazer CD. Increased cerebral tissue oxygen tension after extensive hemodilution with a hemoglobin-based oxygen carrier. Anesth Analg 2004; 99:528–35.
Gulati A, Sen AP, Sharma AC, Singh G. Role of ET and NO in resuscitative effect of diaspirin cross-linked hemoglobin after hemorrhage in rat. Am J Physiol 1997; 273:H827–36.
Freas W, Llave R, Jing M, Hart J, McQuillan P, Muldoon S. Contractile effects of diaspirin cross-linked hemoglobin (DCLHb) on isolated porcine blood vessels. J Lab Clin Med 1995; 125:762–7.
Drobin D, Kjellstrom BT, Malm E, et al. Hemodynamic response and oxygen transport in pigs resuscitated with maleimide-polyethylene glycol-modified hemoglobin (MP4). J Appl Physiol 2004; 96:1843–53.
Hare GM, Mazer CD, Liu E, Qu R, Sikich N, Baker AJ. Resuscitation with albumin improves cerebral oxygenation following hemorrhage in rats. J Neuro trauma 2004; 9:1280.
Kavdia M, Pittman RN, Popel AS. Theoretical analysis of effects of blood substitute affinity and cooperativity on organ oxygen transport. J Appl Physiol 2002; 93:2122–8.
Conover CD, Malatesta P, Lejeune L, Chang CL, Shorr RG. The effects of hemodilution with polyethylene glycol bovine hemoglobin (PEG-Hb) in a conscious porcine model. J Invest Med 1996; 44:238–46.
Rosen AL, Gould S, Sehgal LR, et al. Cardiac output response to extreme hemodilution with hemoglobin solutions of various P50 values. Crit Care Med 1979; 7:380–4.
Pittman RN, Miller KB, Tait PH. Effect of hemoglobin solutions as hemodiluents on capillary oxygen tension. Adv Exp Med Biol 2003; 510:83–8.
Driessen B, Jahr JS, Lurie F, Golkaryeh MS, Gunther RA. Arterial oxygenation and oxygen delivery after hemoglobin-based oxygen carrier infusion in canine hypovolemic shock: a dose-response study. Crit Care Med 2003; 31:1771–9.
von Dobschuetz E, Hoffmann T, Messmer K. Diaspirin cross-linked hemoglobin effectively restores pancreatic microcirculatory failure in hemorrhagic shock. Anesthesiology 1999; 91:1754–62.
Chappell JE, McBride WJ, Shackford SR. Diaspirin cross-linked hemoglobin resuscitation improves cerebral perfusion after head injury and shock. J Trauma 1996; 41:781–8.
Wettstein R, Tsai AG, Erni D, Winslow RM, Intaglietta M. Resuscitation with polyethylene glycol-modified human hemoglobin improves microcirculatory blood flow and tissue oxygenation after hemorrhagic shock in awake hamsters. Crit Care Med 2003; 31:1824–30.
Kerger H, Tsai AG, Saltzman DJ, Winslow RM, Intaglietta M. Fluid resuscitation with O2 vs. non-O2 carriers after 2 h of hemorrhagic shock in conscious hamsters. Am J Physiol 1997; 272:H525–37.
Katz LM, Manning JE, McCurdy S, et al. HBOC-201 improves survival in a swine model of hemorrhagic shock and liver injury. Resuscitation 2002; 54:77–87.
Maxwell RA, Gibson JB, Fabian TC, Proctor KG. Resuscitation of severe chest trauma with four different hemoglobin-based oxygen-carrying solutions. J Trauma 2000; 49:200–9.
Manley GT, Hemphill JC, Morabito D, et al. Small-volume resuscitation with the hemoglobin substitute HBOC-201: effect on brain tissue oxygenation. Advanc Exp Med Biol 2003; 530:311–7.
Saxena R, Wijnhoud AD, Carton H, et al. Controlled safety study of a hemoglobin-based oxygen carrier, DCLHb, in acute ischemic stroke. Stroke 1999; 30:993–6.
Cabrales P, Intaglietta M, Tsai AG. Increase plasma viscosity sustains microcirculation after resuscitation from hemorrhagic shock and continuous bleeding. Shock 2005; 23:549–55.
Shen H, Greene AS, Stein EA, Hudetz AG. Functional cerebral hyperemia is unaffected by isovolemic hemodi-lution. Anesthesiology 2002; 96:142–7.
Author information
Authors and Affiliations
Corresponding author
Additional information
Supported by the Anemia Institute for Research and Education, Canadian Anesthesiologists’ Society, Physicians Services Incorporated Foundation, Hemosol LP, St. Michael’s Hospital. Dr. Hare is a recipient of the Bristol-Myers Squibb-CAS Career Scientist Award. Hemoglobin based oxygen carriers (HBOCs) were generously provided by Hemosol LP. Mississauga, ON, Canada.
Rights and permissions
About this article
Cite this article
Hare, G.M.T., Harrington, A., Liu, E. et al. Effect of oxygen affinity and molecular weight of HBOCs on cerebral oxygenation and blood pressure in rats. Can J Anesth 53, 1030–1038 (2006). https://doi.org/10.1007/BF03022533
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03022533