Abstract
Purpose
To determine if early recovery from severe postoperative anemia is accelerated byiv iron therapy alone or in combination with recombinant erythropoietin (EPO).
Methods
In this double-blinded, placebo-controlled randomized study, consenting adult patients without preoperative anemia whose hemoglobin concentration (Hb) was 70 to 90 g·L-1 on the first day after cardiac or orthopedic surgery (POD 1) were assigned to one of three groups: control,iv iron alone (200 mg of iron sucrose on POD 1, 2, and 3) or in combination with EPO (600 U·kg-1 on POD 1 and 3). The primary outcome was increase in Hb (adjusted for red blood cell transfusions) from POD 1 to 7. Analysis was by intention-to-treat in patients for whom the primary outcome was available. Group effect was analyzed by the ANOVA test, and between-group differences were specified with a Duncan multiple-range test.
Results
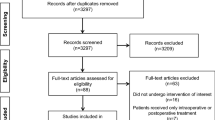
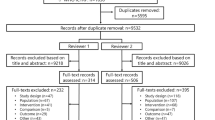
The primary outcome was available in 31 of 38 randomized patients. The average POD 1 Hb was 84 ± 4 g·L-1. There were no between-group differences in outcomes except for higher reticulocyte counts on POD-7 in the combination group. The average adjusted one-week increases in Hb were 7 ± 8 g·L-1 in the control group (n = 10), 9 ± 9 g·L-1 in theiv iron group (n = 11), and 10 ± 14 g·L-1 in the combination group (n = 10). The average adjusted six-week increases in Hb were 37 ± 14 g·L-1 in the control group, 40 ± 7 g·L-1 in theiv iron group, and 45 ± 12 g·L-1 in the combination group.
Conclusion
Early postoperative treatment withiv iron alone or in combination with EPO does not appear to accelerate early recovery from postoperative anemia.
Résumé
Objectif
Vérifier si la récupération précoce ďune sévère anémie postopératoire est accélérée par le fer iv seul ou en combinaison avec de ľérythropoÏétine recombinante (EPO).
Méthode
Pour ľétude à double insu, randomisée et contrôlée contre placebo, des adultes sans anémie préopératoire, chez qui la concentration ďhémoglobine (Hb) était de 70 à 90 g·L-1 au premier jour post-opération cardiaque ou orthopédique (JPO 1), ont été assignés à ľun des trois groupes: témoin, fer iv seul (200 mg de sucrose ferreux aux JPO 1, 2 et 3) ou en combinaison avec de ľEPO (600 U·kg-1 aux JPO POD 1 et 3). Le résultat principal était une hausse de ľHb (ajustée pour les transfusions de culots globulaires) des JPO 1 à 7. Ľévaluation, pour les patients ayant atteint ce résultat, utilisait ľanalyse par intention de traiter. Ľeffet de groupe a été analysé par le test ANOVA test et les différences intergroupes ont été précisées avec le test à gamme multiple de Duncan.
Résultats
Le résultat principal était atteint chez 31 des 38 patients randomisés. La moyenne de ľHb au JPO 1 a été de 84 ± 4 g·L-1. Il n’y a pas eu de différence de résultat intergroupe sauf pour une numération plus élevée des réticulocytes au JPO 7 dans le groupe ďEPO. Les hausses moyennes ďHb ajustées sur une semaine ont été de 7 ± 8 g·L-1dans le groupe témoin (n = 10), 9 ± 9 g·L-1 avec le fer iv (n = 11) et 10 ± 14 g·L-1 avec ľEPO (n = 10). Les hausses moyennes ďHb ajustées sur six semaines ont été de 37 ± 14 g·L-1 chez les témoins, 40 ± 7 g·L-1 avec le fer iv et 45 ± 12 g·L-1 avec ľEPO.
Conclusion
Le traitement postopératoire précoce avec du fer iv seul ou en combinaison avec ľEPO ne semble pas hâter la récupération de ľanémie postopératoire.
Article PDF
Similar content being viewed by others
References
British Society for Haematology. Guidelines for the clinical use of red cell transfusions. Br J Haematol 2001; 113: 24–31.
Hebert PC, Wells G, Blajchman MA, et al. A multicenter, randomized, controlled clinical trial of transfusion requirements in critical care. Transfusion requirements in Critical Care Investigators, Canadian Care Trials Group. N Engl J Med 1999; 340: 409–17.
Woodson RD, Wills RE, Lenfant C. Effect of acute and established anemia on O2 transport at rest, submaximal and maximal work. J Appl Physiol 1978; 44: 36–43.
Winslow RM. A physiological basis for the transfusion trigger.In: Spiess BD, Counts RB, Gould SA (Eds). Perioperative Transfusion Medicine. Baltimore: Williams & Wilkins; 1997: 27–43.
Cella D. Factors influencing quality of life in cancer patients: anemia and fatigue. Semin Oncol 1998; 25: 43–6.
Hillman RS, Finch CA. Red Cell Manual, 7 ed. Philadelphia: F.A. Davis Company; 1996.
van Iperen CE, Kraaijenhagen RJ, Biesma DH, Beguin Y, Marx JJ, van de Wiel A. Iron metabolism and erythropoiesis after surgery. Br J Surg 1998; 85: 41–5.
Biesma DH, van de Wiel A, Beguin Y, Kraaijenhagen RJ, Marx JJ. Post-operative erythropoiesis is limited by the inflammatory effect of surgery on iron metabolism. Eur J Clin Invest 1995; 25: 383–9.
van Iperen CE, Biesma DH, van de Wiel A, Marx JJ. Erythropoietic response to acute and chronic anaemia: focus on postoperative anaemia. Br J Anaesth 1998; 81(Suppl 1): 2–5.
Zauber NP, Zauber AG, Gordon FJ, et al. Iron supplementation after femoral head replacement for patients with normal iron stores. JAMA 1992; 267: 525–7.
Crosby L, Palarski VA, Cottington E, Cmolik B. Iron supplementation for acute blood loss anemia after coronary artery bypass surgery: a randomized, placebo-controlled study. Heart Lung 1994; 23: 493–9.
Mollison PL, Engelfriet CP, Contreras M. Blood transfusion in clinical medicine. 9 ed. Oxford: Blackwell Scientific Publications; 1993.
Karkouti K, McCluskey SA, Rampersaud R, et al. Postoperative anemia: incidence and transfusion needs. Can J Anesth 2001; 48: 30A (Abstract).
Madi-Jebara SN, Sleilaty GS, Achouh PE, et al. Postoperative intravenous iron used alone or in combination with low-dose erythropoietin is not effective for correction of anemia after cardiac surgery. J Cardiothorac Vasc Anesth 2004; 18: 59–63.
Mays T, Mays T. Intravenous iron-dextran therapy in the treatment of anemia occurring in surgical, gynecologic and obstetric patients. Surg Gynecol Obstet 1976; 143: 381–4.
Dudrick SJ, O’Donnell JJ, Matheny RG, Unkel SP, Raleigh DP. Stimulation of hematopoiesis as an alternative to transfusion. South Med J 1986; 79: 669–73.
Berniere J, Dehullu JP, Gall O, Murat I. Intravenous iron in the treatment of postoperative anemia in surgery of the spine in infants and adolescents (French). Rev Chir Orthop Reparatrice Appar Mot 1998; 84: 319–22.
Levine EA, Rosen AL, Sehgal LR, et al. Treatment of acute postoperative anemia with recombinant human erythropoietin. J Trauma 1989; 29: 1134–8.
Krieter H, Bruckner UB, Krumwieh D, Seiler FR, Messmer K. Erythropoietin accelerates the recovery from extreme hemodilution: a randomized, placebo-controlled study in dogs. Eur Surg Res 1990; 22: 121–7.
Hoynck van Papendrecht MA, Jeekel H, Busch OR, Marquet RL. Efficacy of recombinant erythropoietin for stimulating erythropoiesis after blood loss and surgery. An experimental study in rats. Eur J Surg 1992; 158: 83–7.
Rosen BS, Levine EA, Egrie JC, et al. Effects of recombinant human erythropoietin and interleukin-3 on erythropoietic recovery from acute anemia. Exp Hematol 1993; 21: 1487–91.
Koestner JA, Nelson LD, Morris JA Jr, Safcsak K. Use of recombinant human erythropoietin (r-HuEPO) in a Jehovah’s Witness refusing transfusion of blood products: case report. J Trauma 1990; 30: 1406–8.
Kraus P, Lipman J. Erythropoietin in patient following multiple trauma. Anaesthesia 1992; 47: 962–4.
Akingbola OA, Custer JR, Bunchman TE, Nedman AB. Management of severe anemia without transfusion in a pediatric Jehovah’s Witness patient. Crit Care Med 1994; 22: 524–8.
Collins SL, Timberlake GA. Severe anemia in the Jehovah’s Witness: case report and discussion. Am J Crit Care 1993; 2: 256–9.
von Bormann B, Weiler J, Aulich S. Acute treatment with recombinant erythropoietin in patients with preand postoperative anemia: a clinical report. Clin Invest 1994; 72: S31–5.
Wolff M, Fandrey J, Jelkmann W. Perioperative use of recombinant human erythropoietin in patients refusing blood transfusions. Pathophysiological considerations based on 5 cases. Eur J Haematol 1997; 58: 154–9.
Atabek U, Alvarez R, Pello MJ, Alexander JB, Camishion RC, Spence RK. Erythropoietin accelerates hematocrit recovery in post-surgical anemia. Am Surg 1995; 61: 74–7.
Feagan BG, Wong CJ, Kirkley A, et al. Erythropoietin with iron supplementation to prevent allogeneic blood transfusion in total hip joint arthroplasty. Ann Intern Med 2000; 133: 845–54.
Karkouti K, McCluskey SA, Evans L, Mahomed N, Ghannam M, Davey R. Erythropoietin is an effective modality for reducing RBC transfusion in joint surgery. Can J Anesth 2005; 52: 362–8.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Karkouti, K., McCluskey, S.A., Ghannam, M. et al. Intravenous iron and recombinant erythropoietin for the treatment of postoperative anemia. Can J Anesth 53, 11–19 (2006). https://doi.org/10.1007/BF03021522
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03021522