Abstract
Purpose: To determine whether remifentanil, combined with propofol, could induce controlled hypotension, reduce middle ear blood flow (MEBF) measured by laser-Doppler flowmetry, provide a “dry” operative field, and could be compared with nitroprusside or esmolol combined with alfentanil and propofol.
Methods: Thirty patients undergoing tympanoplasty and anesthetized with 2.5 mg·kg−1 propofoliv followed by a constant infusion of 120µg·kg−1·min−1, were randomly assigned in three groups to receive either 1µg·kg−1 remifentaniliv followed by a continuous infusion of 0.25 to 0.50µg·kg−1, or nitroprussideiv, or esmololiv combined for the latter two groups with alfentaniliv.
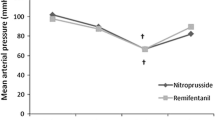
Results: Controlled hypotension was achieved at the target pressure of 80 mmHg within 107±16, 69±4.4, 53.3±4.4 sec for remifentanil, nitroprusside and esmolol respectively. MEBF decreased by 24±0.3, 22±3.3, 37±3% and preceded the decrease in SABP, within 30±6.1, 11.2±3.1, 15±2.8 sec for remifentanil, nitroprusside and esmolol respectively. Remifentanil, and nitroprusside decreased MEBF autoregulation less than esmolol (0.36±0.1, 0.19±0.2, −0.5±0.2). Controlled hypotension was sustained in all three groups throughout surgery, and the surgical field rating decreased in a range of 80% in all three groups. Nitroprusside decreased pH and increased PaCO2. There were no postoperative complications in any of the groups.
Conclusions: Remifentanil combined with propofol enabled controlled hypotension, reduced middle ear blood flow and provided good surgical conditions for tympanoplasty with no need for additional use of a potent hypotensive agent.
Résumé
Objectif: Déterminer si le rémifentanil, associé au propofol, peut induire une hypotension contrôlée, réduire le débit sanguin de l’oreille moyenne (DSOM) mesuré par laser-Doppler, assurer un champ opératoire exsangue et être comparé au nitroprussiate et à l’esmolol associés à l’alfentanil et au propofol.
Méthode: Trente patients subissant une tympanoplastie, et anesthésiés par 2,5 mg·kg−1 de propofoliv suivis d’une perfusion de 120µg·kg−1·min−1, ont été répartis après randomisation en 3 groupes recevant soit 1µg·kg−1 de rémifentaniliv suivis d’une perfusion de 0,25 à 0,50µg·kg−1·min−1, soit du nitroprussiate, soit de l’esmololiv, associé pour les 2 derniers à de l’alfentanil.
Résultats: Tout d’abord, l’hypotension contrôlée a été obtenue au niveau souhaité de 80 mmHg en 107±16; 69±4,4; 53,3±4,4 sec pour le rémifentanil, le nitroprussiate et l’esmolol. Le DSOM a diminué de 24±0,3; 22±3,3; 37±3% et a précédé la chute de pression de 30±6,1; 11,2±3,1; 15±2,8 sec pour le rémifentanil, le nitroprussiate et l’esmolol. Le rémifentanil et le nitroprussiate ont moins réduit l’autorégulation que l’esmolol (0,36±0,1; 0,19±0,2; −0,5±0,2). Ensuite, l’hypotension contrôlée a été maintenue dans les 3 groupes tout au long de l’opération, et le saignement opératoire a été diminué de 80% dans les 3 groupes. Le nitroprussiate a diminué le pH et augmenté la PaCO2. Il n’y a eu aucune complication postopératoire dans chacun des groupes.
Conclusion: Le rémifentanil associé au propofol a permis de réaliser une hypotension contrôlée, de réduire le débit sanguin de l’oreille moyenne et d’assurer de bonnes conditions opératoires pour la tympanoplastie sans recours à un agent hypotenseur puissant.
Article PDF
Similar content being viewed by others
References
Smith C Haemostasis in ear surgery. Proc R Soc Med 1971; 64: 1225–6.
Kerr AR. Anaesthesia with profound hypotension for middle ear surgery. Br J Anaesth 1977; 49: 447–52.
Saarnivaara L, Brander P. Comparison of three hypotensive anaesthetic methods for middle ear microsurgery. Acta Anaesthesiol Scand 1984; 28: 435–42.
Degoute CS, Dubreuil C, Ray MJ, et al. Effects of posture, hypotension and locally applied vasoconstriction on the middle ear microcirculation in anaesthetized humans. Eur J Appl Physiol 1994; 69: 414–20.
Newton MC, Chadd GD, O’Donoghue B, Sapsed-Byrne SM, Hall GM. Metabolic and hormonal responses to induced hypotension for middle ear surgery. Br J Anaesth 1996; 76: 352–7.
Dietrich GV, Heesen M, Boldt J, Hempelmann G. Platelet function and adrenoceptors during and after induced hypotension using nitroprusside. Anesthesiology 1996; 85: 1334–40.
Pilli G, Güzeldemir ME, Bayhan N. Esmolol for hypotensive anesthesia in middle ear surgery. Acta Anaesthesiol Belg 1996; 47: 85–91.
Saarnivaara L, Klemola U-M, Lindgren L. Labetalol as a hypotensive agent for middle ear microsurgery. Acta Anaesthesiol Scand 1987; 31: 196–201.
Amaranath L, Kellermeyer WF Jr. Tachyphylaxis to sodium nitroprusside. Anesthesiology 1976; 44: 345–8.
Tinker JH, Michenfelder JD. Sodium nitroprusside: pharmacology, toxicology and therapeutics. Anesthesiology 1976; 45: 340–54.
Blau WS, Kafer ER, Anderson JA. Esmolol is more effective than sodium nitroprusside in reducing blood loss during orthognathic surgery. Anesth Analg 1992; 75: 172–8.
Guy J, Hindman BJ, Baker KZ, et al. Comparison of remifentanil and fentanyl in patients undergoing craniotomy for supratentorial space-occupying lesions. Anesthesiology 1997; 86: 514–24.
Philip BK, Scuderi PE, Chung F, et al. Remifentanil compared with alfentanil for ambulatory surgery using total intravenous anesthesia. Anesth Analg 1997; 84: 515–21.
Davis PJ, Lerman J, Suresh S, et al. A randomized multicenter study of remifentanil compared with alfentanil, isoflurane, or propofol in anesthetized pediatric patients undergoing elective strabismus surgery. Anesth Analg 1997; 84: 982–9.
Schüttler J, Albrecht S, Breivik H, et al. A comparison of remifentanil and alfentanil in patients undergoing major abdominal surgery. Anaesthesia 1997; 52: 307–17.
Baker KZ, Ostapkovich N, Sisti MB, Warner DS, Young WL. Intact cerebral blood flow reactivity during remifentanil/nitrous oxyde anesthesia. J Neurosurg Anesthesiol 1997; 9: 134–40.
Hogue CW Jr,Bowdle TA, OrsLeary C, et al. A multicenter evaluation of total intravenous anesthesia with remifentanil and propofol for elective inpatient surgery. Anesth Analg 1996; 83: 279–85.
Strebel S, Lam AM, Matta B, Mayberg TS, Aaslid R, Newell DW. Dynamic and static cerebral autoregulation during isoflurane, desflurane, and propofol anesthesia. Anesthesiology 1995; 83: 66–76.
Fromme GA, Mackenzie RA, Gould AB Jr,Lund BA, Offord KP. Controlled hypotension for orthognathic surgery. Anesth Analg 1986; 65: 683–6.
Ornstein E, Matteo RS, Weinstein JA, Schwartz AE. A controlled trial of esmolol for the induction of deliberate hypotension. J Clin Anesth 1988; 1: 31–5.
Ornstein E, Young WL, Ostapkovich N, Matteo RS, Diaz J. Deliberate hypotension in patients with intracranial arteriovenous malformations: esmolol compared with isoflurane and sodium nitroprusside. Anesth Analg 1991; 72: 639–44.
Boezaart AP, Van der Merwe J, Coetzee A. Comparison of sodium nitroprusside- and esmolol-induced controlled hypotension for functional endoscopic sinus surgery. Can J Anaesth 1995; 42: 373–6.
Pinaud M, Souron R, Lelausque J-N, Gazeau M-F, Lajat Y, Dixneuf B. Cerebral blood flow and cerebral oxygen consumption during nitroprussid-induced hypotension to less than 50 mmHg. Anesthesiology 1989; 70: 255–60.
Taylor TH, Styles M, Lamming AJ. Sodium nitroprusside as a hypotensive agent in general anaesthesia. Br J Anaesth 1970; 42: 859–64.
Degoute C-S, Saumet J-L, Banssillon V, Dittmar A. Skin blood flow measured by thermal clearance method in anesthesia. Anesth Analg 1985; 64: 179–82.
Saumet JL, Degoute CS, Dittmar A, Banssillon V. Changes in skin thermal clearance during anaesthesia. Anaesthesia 1986; 41: 386–9.
Saumet JL, Leftheriotis G, Dittmar A, Delhomme G, Degoute CS. Skin blood flow changes in anaesthetized humans: comparison between skin thermal clearance and finger pulse amplitude measurement. Eur J Appl Physiol 1986; 54: 574–7.
Hultcrantz E, Linder J, Angelborg C. Sympathetic effects on cochlear blood flow at different blood pressure levels. Portmann M, Aran JM (Eds,). INSERM, 1977; 68: 271–8.
Degoute C-S, Preckel M-P, Dubreuil C, Banssillon V, Duclaux R. Sympathetic nerve regulation of cochlear blood flow during increases in blood pressure in humans. Eur J Appl Physiol 1997; 75: 326–32.
Ebert TJ, Muzi M, Berens R, Goff D, Kampine JP. Sympathetic responses to induction of anesthesia in humans with propofol or etomidate. Anesthesiology 1992; 76: 725–33.
McPherson RW, Krempasanka E, Eimerl D, Traystman RJ. Effects of alfentanil on cerebral vascular reactivity in dogs. Br J Anaesth 1985; 57: 1232–8.
Author information
Authors and Affiliations
Corresponding author
Additional information
This work was supported in part by grants from Institut National de la Santé et de la Recherche Médicale, and Région Rhône-Alpes, and Hospices Civils de Lyon.
Rights and permissions
About this article
Cite this article
Degoute, CS., Ray, MJ., Manchon, M. et al. Remifentanil and controlled hypotension; comparison with nitroprusside or esmolol during tympanoplasty. Can J Anaesth 48, 20–27 (2001). https://doi.org/10.1007/BF03019809
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03019809