Abstract
Purpose
To study the analgesic and sedative effects of remifentanil in critically-ill patients.
Methods
Remifentanil infusion was started at 0.02 μg·kg−1·min−1 in ten mechanically ventilated critically-ill patients, and the infusion rate was increased to 0.05, 0.10, 0.15, 0.20, and 0.25 μg·kg−1·min−1 every 30 min. Basally and 25 min after each increase we measured: the Ramsey sedation score (RSS) and the respiratory response subscore of comfort scale (CSRR); the bispectral index (BIS) before and after lightly touching tracheal mucosa; heart rate and systemic arterial pressure; respiratory variables; plasma epinephrine and norepinephrine levels.
Results
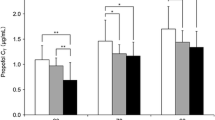
Infusion rates up to 0.05 μg·kg−1·min−1 were effective against agitation and achieved a good degree of adaption to the respirator in all patients (RSS 2 or more and CSRR 3 or less); BIS decreased significantly; respiratory and circulatory variables were unaffected; mean plasma epinephrine levels decreased. At infusion rates higher than 0.05 μg·kg−1·min−1 RSS but not BIS decreased further and patient arousability caused by noxious stimuli was not prevented; respiratory drive suppression occurred at the infusion rates higher than 0.05 μg·kg−1·min−1 in four patients; bradycardia and arterial hypotension was observed in three patients; plasma epinephrine levels decreased significantly, while norepinephrine was unaffected; severe itching was experienced by one patient.
Conclusions
Low doses of remifentanil (upto 0.05 μg·kg−1·min−1) can be useful in critically-ill patients in order to achieve calm and sedation. Higher doses can inhibit respiratory drive and require controlled mechanical ventilation.
Zusammenfassung
Objectif
Étudier les effets analgésiques et sédatifs du rémifentanil chez de grands malades.
Méthode
Une perfusion de rémifentanil a été amorcée à 0,02 μg·kg−1·min−1 chez dix grands malades ventilés mécaniquement. La vitesse de perfusion a été augmentée à 0,05, 0,10, 0,15, 0,20 et 0,25 μg·kg−1·min−1 toutes les 30 min. Au début, et 25 min après chaque augmentation, nous avons mesuré : les scores de sédation de Ramsey (SSR) et le score auxiliaire de réponse respiratoire de l’échelle de confort (RREC); l’index bispectral (BIS) avant et après avoir légèrement stimulé la muqueuse trachéale; la fréquence cardiaque et la tension artérielle générale; les variables respiratoires; les niveaux plasmatiques d’adrénaline et de noradrénaline.
Résultats
Les vitesses de perfusion allant jusqu’à 0,05 μg·kg−1·min−1 ont été efficaces contre l’agitation et ont permis une bonne adaptation au respirateur chez tous les patients (2 ou moins à SSR et 3 ou moins à RREC); le BIS a diminué de manière significative; les variables respiratoires et circulatoires n’ont pas été affectées; il y a eu une baisse des niveaux plasmatiques d’adrénaline et de noradrénaline. Sous des vitesses de perfusion plus élevées que 0,05 μg·kg−1·min−1, le SSR, mais non le BIS, a baissé davantage et la réaction des patients aux stimuli nuisibles n’a pu être empêchée; la suppression de la commande respiratoire s’est produite avec des perfusion audessus de 0,05 μg·kg−1·min−1 chez quatre patients; on a observé de la bradycardie et de l’hypotension chez trois patients; les niveaux plasmatiques d’adrénaline ont baissé significativement, mais ceux de la noradrénaline n’ont pas changé; un prurit sévère a été noté chez un patient.
Conclusion
Des doses faibles de rémifentanil (jusqu’à 0,05 μg·kg−1·min−1) peuvent apporter calme et sédation chez de grands malades. Des doses plus élevées peuvent inhiber la commande respiratoire et exiger une ventilation mécanique contrôlée.
Article PDF
Similar content being viewed by others
References
Reves JG. Educational considerations for the clinical introduction and use of remifentanil. Anesth Analg 1999; 89(4 Suppl): S4–6.
Glass PS, Gan TJ, Howell S. A review of the pharmacokinetics and pharmacodynamics of remifentanil. Anesth Analg 1999; 89(4 Suppl): S7–14.
Cohen J, Royston D. Remifentanil. Curr Opin Crit Care 2001; 7: 227–31.
Bowdle TA, Camporesi EM, Maysick L, et al. A multicenter evaluation of remifentanil for early postoperative analgesia. Anesth Analg 1996; 83: 1292–7.
Wilhelm W, Dorscheid E, Schlaich N, Niederprum P, Deller D. The use of remifentanil in critically ill patients. Clinical findings and early experience (German). Anaesthesist 1990; 48: 625–9.
Tipps LB, Coplin WM, Murry KR, Rhoney DH. Safety and feasibility of continuous infusion of remifentanil in the neurosurgical intensive care unit. Neurosurgery 2000; 46: 596–601.
Ramsay MA, Savege TM, Simpson BR, Goodwin R. Controlled sedation with alphaxalone-alphadolone. Br Med J 1974; 2: 656–9.
Ambuel B, Hamlett KW, Marx CM, Blumer JL. Assessing distress in pediatric intensive care environments: the COMFORT scale. J Pediatr Psychol 1992; 17: 95–109.
Banner MJ, Kirby RR, Blanch PB, Layon AJ. Decreasing imposed work of the breathing apparatus to zero using pressure-support ventilation. Crit Care Med 1993; 21: 1333–8.
Kirton OC, Banner MJ, Axelrad A, Drugas G. Detection of unsuspected imposed work of breathing: case reports. Crit Care Med 1993; 21: 790–5.
Petros AJ, Lamond CT, Bennett D. The Bicore pulmonary monitor. A device to assess the work of breathing while weaning from mechanical ventilation. Anaesthesia 1993; 48: 985–8.
Perrigault PF, Pouzeratte TH, Jaber S, et al. Changes in occlusion pressure (P0.1) and breathing pattern during pressure support ventilation. Thorax 1999; 54: 119–23.
Whitelaw WA, Derenne JP, Milic-Emili J. Occlusion pressure as a measure of respiratory center output in conscious man. Respir Physiol 1975; 23: 181–99.
Rosa G, Conti G, Orsi P, et al. Effects of low-dose propofol administration on central respiratory drive, gas exchanges and respiratory pattern. Acta Anaesthesiol Scand 1992; 36: 128–31.
Conti G, De Blast R, Pelaia P, et al. Early prediction of successful weaning during pressure support ventilation in chronic obstructive pulmonary disease patients. Crit Care Med. 1992; 20: 366–71.
Conti G, Cinnella G, Barboni E, Lemaire F, Harf A, Brochard L. Estimation of occlusion pressure during assisted ventilation in patients with intrinsic PEEP. Am J Respir Crit Care Med 1996; 154: 907–12.
Hussain SN, Pardy RL, Dempsey JA. Mechanical impedance as determinant of inspiratory neural drive during exercise in humans. J Appl Physiol 1985; 59: 365–75.
Rosow CE. An overview of remifentanil. Anesth Analg 1999; 89(4 Suppl): S1–3.
Guignard B, Menigaux C, Dupont X, Fletcher D, Chauvin M. The effect of remifentanil on the bispectral index change and hemodynamic responses after orotracheal intubation. Anesth Analg 2000; 90: 161–7.
Lysakowski C, Dumont L, Pellegrini M, Clergue F, Tassonyi E. Effects of fentanyl, alfentanil, remifentanil and sufentanil on loss of consciousness and bispectral index during propofol induction of anaesthesia. Br J Anaesth 2001;86: 523–7.
Bowdle TA. Adverse effects of opioid agonists and agonist-antagonists in anaesthesia. Drug Saf 1998; 19: 173–89.
Grassi G, Esler M. How to assess sympathetic activity in humans. J Hypertens 1999; 17: 719–34.
Maling TJ, Dollery CT, Hamilton CA. Clonidine and sympathetic activity during sleep. Clin Sci (Lond) 1979; 57: 509–14.
Hall RI, MacLaren C, Smith MS, et al. Light versus heavy sedation after cardiac surgery: myocardial ischemia and the stress response. Maritime Heart Centre and Dalhousie University. Anesth Analg 1997; 85: 971–8.
Plunkett JJ, Reeves JD, Ngo L, et al. Urine and plasma catecholamine and cortisol concentrations after myocardial revascularization. Modulation by continuous sedation. Multicenter Study of Perioperative Ischemia (McSPI) Research Group, and the Ischemia Research and Education Foundation (IREF). Anesthesiology 1997; 86: 785–96.
Robertson D, Johnson GA, Robertson RM, Nies AS, Shand DG, Oates JA. Comparative assessment of stimuli that release neuronal and adrenomedullary catecholamines in man. Circulation 1979; 59: 637–43.
Kjellberg F, Tramer MR. Pharmacological control of opioid-induced pruritus: a quantitative systematic review of randomized trials. Eur J Anaesthesiol 2001; 18: 346–57.
Avramov MN, Smith I, White PF. Interactions between midazolam and remifentanil during monitored anesthesia care. Anesthesiology 1996; 85: 1283–9.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Cavaliere, F., Antonelli, M., Arcangeli, A. et al. A low-dose remifentanil infusion is well tolerated for sedation in mechanically ventilated, critically-ill patients. Can J Anesth 49, 1088–1094 (2002). https://doi.org/10.1007/BF03017909
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03017909