Abstract
Purpose
To examine the effect of halothane on the cytosolic Ca2+ concentration ([Ca2+]i)-tension relationship of rat aortic smooth muscle.
Methods
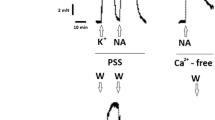
Rat aortic rings without endothelia were loaded with the fluorescent Ca2+ indicator, Fura PE3-AM, and then mounted in organ baths. The changes in isometric tension and [Ca2+]i were measured simultaneously. In one series ionomycin (10 nM–3 μM) was added to normal Krebs’ solution cumulatively in the absence and presence of halothane ( 1.5%, 3%). In the other series, CaCl2 (0.3–3 mM) was added to Ca2+-free Krebs’ solution including high KCl (50 mM), phenylephrine (100 nM) or prostaglandin F2α (PGF2α, 1–3 μM) in the absence and presence of halothane (1.5%, 3%). The linear part of [Ca2+]i-tension relationship was analyzed by a linear regression.
Results
Halothane, 1.5%, had no effect on the normal [Ca2+]i-tension relationship obtained with the calcium ionophore, ionomycin (10 nM–3 μM), but halothane 3% decreased the slope of the relationship (0.239 ± 0.037 for control and 0.110 ± 0.010 for halothane 3%,P < 0.05). Halothane, 1.5% and 3%, did not change the [Ca2+]i-tension relationship obtained with CaCl2 (0.3–3 mM) in the presence of high KCl (50 mM) or phenylephrine ( 100 nM). In contrast, halothane, 3%, inhibited the intercept of [Ca2+]i-tension relationship obtained with CaCl2 (0.3–3 mM) in the presence of prostaglandin F2α (PGF2α′, 1–3 μM) (45.708 ± 4.233 for control and 26.997 ± 2.522 for halothane 3%, P < 0.0l).
Conclusion
Halothane decreases the Ca2+ sensitivity and that in the presence of PGF2.
Résumé
Objectif
Étudier l’effet de l’halothane sur la relation tension isométrique-concentration calcique cytosolique ([Ca2+]i) sur le muscle lisse de l’aorte chez le rat.
Méthode
Des anneaux aortiques de rat, sans endothélium, ont été chargés avec un indicateur de fluorescence pour le Ca2+, le Fura PE3-AM, et montés ensuite dans des bains d’organes. Les changements de tension isométrique et de [Ca2+]i ont été mesurés simultanément. Dans une série, on a ajouté de l’ionomycine (10 nM–3 μM) à la solution Krebs normale, de façon cumulée en l’absence et en présence d’halothane (1,5 %, 3 %). Dans l’autre série, du CaCl2 (0,3–3 mM) a été ajouté à la solution Krebs libre de Ca2+ incluant une forte concentration de KCl (50 mM), de phényléphrine (100 nM) ou de prostaglandine F2 (PGF2, 1–3 μM) en l’absence et en présence d’halothane (1,5 %, 3 %). La portion linéaire de la relation [Ca2+]i-tension a été analysée par une régression linéaire.
Résultats
]L’halothane, 1,5%, n’a pas eu d’effet sur la relation [Ca2+]i-tension isométrique normale obtenue avec l’ionophore calcique (ionomycine 10 nM–3 μM), mais l’halothane 3% a fait baisser la pente de la relation (0,239 ± 0,037 pour les témoins et 0, 110 ± 0,010 pour l’halothane 3%, P < 0,05). Lhalothane, 1,5% et 3%, n’a pas changé la relation [Ca2+]i-tension obtenue avec le CaCl2 (0,3–3 mM) en présence d’une forte concentration de KCI (50 mM) ou de phényléphrine (100 nM). Par ailleurs, l’halothane 3% modifie à la baisse l’ordonnée à l’origine de la relation [Ca2+]i-tension obtenue avec le CaCI2 (0,3-3 mM) en présence de prostaglandine F2 (PGF2, 1–3 μM) (45,708 ± 4,233 pour les témoins et 26,997 ± 2,522 pour l’halothane 3 %,P < 0,01).
Conclusion
L’halothane diminue la sensibilité du Ca2+ et ce, en présence de la PGF2.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Sprague DH, Yang JC, Nagai SH. Effects of isoflurane and halothane on contractility and cyclic 3′,5′-adenosine monophosphate system in the rat aorta. Anesthesiology 1974; 40: 162–7.
Clark SC, MacCannell KL. Vascular responses to an aesthetic agents. Can Anaesth Soc J 1975; 22: 20–33.
Seyde WC, Longnecker DE. Anesthetic influences on regional hemodynamics in normal and hemorrhaged rats. Anesthesiology 1984; 61: 686–98.
Palahniuk RJ, Shnider SM. Maternal and fetal cardiovascular and acid-base changes during halothane and isoflurane anesthesia in the pregnant ewe. Anesthesiology 1974; 41: 462–72.
Johnson D, Mayers I, To T. The effects of halothane in hypoxic pulmonary vasoconstriction. Anesthesiology 1990; 72: 125–33.
DeFeo TT, Morgan KG. Calcium-force relationships as detected with aequorin in two different vascular smooth muscles of the ferret. J Physiol (Lond) 1985; 369: 269–82.
Hori M, Sato K, Sakata K, et al. Receptor agonists induce myosin phosphorylarion-dependent and phosphorylation-independent contractions in vascular smooth muscle. J Pharmacol Exp Ther 1992; 261: 506–12.
Bruschi G, Bruschi ME, Regolisti G, Borghetti A. Myoplasmic Ca2+-force relationship studied with fura-2 during stimulation of rat aortic smooth muscle. Am J Physiol 1988; 254: H840–54.
Buljubasic N, Kusch NJ, Marijic J, Kampine JP, Bosnjak ZJ. Effects of halothane and isoflurane on calcium and potassium channel currents in canine coronary arterial cells. Anesthesiology 1992; 76: 990–8.
Su JY, Zhang CC. Intracellular mechanisms of halothane’s effect on isolated aortic strips of the rabbit. Anesthesiology 1989; 71: 409–17.
Akata T, Boyle WA III. Volatile anesthetic actions on contractile proteins in membrane-permeabilized small mesenteric arteries. Anesthesiology 1995; 82: 700–12.
Kakuyama M, Hatano Y, Nakamura K, et al. Halothane and enflurane constrict canine mesenteric arteries by releasing Ca2+ from intracellular Ca2+ stores. Anesthesiology 1994; 80: 1120–7.
Kitamura R, Kakuyama M, Nakamura K, Miyawaki I, Mori K. Thiobarbiturates suppress depolarizationinduced contraction of vascular smooth muscle without suppression of calcium influx. Br J Anaesth 1996; 77: 503–7.
Himpens B, Somlyo AP. Free-calcium and force transients during depolarization and pharmacomechanical coupling in guinea-pig smooth muscle. J Physiol (Lond) 1988; 395: 507–30.
Sato K, Ozaki H, Karaki H. Changes in cytosolic calcium level in vascular smooth muscle strip measured simultaneously with contraction using fluorescent calcium indicator fura 2. J Pharmacol Exp Ther 1988; 246: 294–300.
Kurata R, Takayanagi I, Hisayama T. Eicosanoidinduced Ca2+ release and sustained contraction in Ca2+-free media are mediated by different signal transduction pathways in rat aorta. Br J Pharmacol 1993; 110: 875–81.
Fukuizumi Y, Kobayashi S, Nishimura J, Kanaide H. Cytosolic calcium concentration-force relation during contractions in the rabbit femoral artery: time-dependency and stimulus specificity. Br J Pharmacol 1995; 114: 329–38.
Renzi F, Waud BE. Partition coefficients of volatile anesthetics in Krebs’ solution. Anesthesiology 1977; 47: 62–3.
White PF, Johnston RR, Eger EI II. Determination of anesthetics requirement in rats. Anesthesiology 1974; 40: 52–7.
Bylund DB, Eikenberg DC, Hieble JP, et al. International union of pharmacology nomenclature of adrenoceptors. Pharmacol Rev 1994; 46: 121–36.
Coleman RA, Smith WL, Narumiya S. International union of pharmacology classification of prostanoid receptors: properties distribution, and structure of the receptors and their subtypes. Pharmacol Rev 1994; 46: 205–29.
Hirakata H, Ushikubi F, Narumiya S, Hatano Y, Nakamura K, Mori K. The effect of inhaled anesthetics on the platelet aggregation and the ligand-binding affinity of the platelet thromboxane A2 receptor. Anesth Analg 1995; 81: 114–8.
Yamamoto M, Hatano Y, Kakuyama M, et al. Halothane and isoflurane preferentially inhibit prostanoid-induced vasoconstriction of rat aorta. Can J Anaesth 1994; 41: 991–5.
Olson DM, Lye SJ, Skinner K, Challis JRG. Prostanoid concentrations in maternal/fetal plasma and amniotic fluid and intrauterine tissue prostanoid output in relation to myometrial contractility during the onset of adrenocorticotropin-induced preterm labor in sheep. Endocrinology 1985; 116: 389–97.
Grbovi L, Jovanovi A, Tuli I. Indomethacin reduces contraction of isolated non-pregnant human uterine artery induced by prostaglandin F2α. Hum Reprod 1996; 11: 1998–2002.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kakuyama, M., Nakamura, K. & Mori, K. Halothane decreases calcium sensitivity of rat aortic smooth muscle. Can J Anesth 46, 1164–1171 (1999). https://doi.org/10.1007/BF03015527
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03015527