Abstract
Purpose
To compare the post-operative analgesic effect of 100 mgvs 200 mg epidural tramadol and saline in patients undergoing elective Cesarean section.
Methods
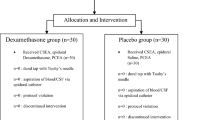
Sixty healthy women undergoing Cesarean delivery with epidural anesthesia were randomly allocated into three groups (n = 20 in each). Patients received, at skin closure via the epidural catheter, 100 mg tramadol (Group I), 200 mg tramadol (Group II) or 10 ml saline (Control group). Pain scores and side effects were evaluated at 1, 2, 4, 8, 12 and 24 hr after surgery. Mean times to the first analgesic administration, as well as the cumulative doses of analgesic requirements over 24 hr postoperatively were compared.
Results
The mean time to first analgesic administration was longer in patients who received 100 mg tramadol (4.5 ±3.1 hr) and the 200 mg tramadol (6.6 ±3.4 hr) than in those who received placebo (2.8 ± 2 hr). The mean cumulative doses of meperidine over 24 hr were less in the 100 mg tramadol group (0.3 ± 0.3 mg·kg−1) and the 200 mg tramadol group (0.3 ± 0.3 mg·kg−1) than in the control group (0.7 ± 0.4 mg·kg−1). Also, the mean doses of diclofenac over 24 hr were less in the 100 mg tramadol group (156 ± 59 mg) and the 200 mg tramadol group (142 ± 62 mg) than in the control group (214 ± 70 mg). However, no difference was obtained between patients receiving 100 mg and 200 mg tramadol concerning all parameters studied.
Conclusion
Epidural tramadol 100 mg can provide adequate postoperative analgesia without respiratory depression in patients after Cesarean delivery.
Résumé
Objectif
Comparer l’effet analgésique postopératoire de 100 mg vs 200 mg de tramadol épidural ou d’une solution salée chez des patientes qui doivent subir une césarienne.
Méthode
Soixante femmes en santé admises pour une césarienne sous anesthésie épidurale ont été réparties au hasard en trois groupes (n = 20 chacun). Elles ont reçu, lors de la fermeture cutanée et au moyen d’un cathéter épidural, 100 mg (groupe I) ou 200 mg (groupe II) de tramadol ou 10 ml de solution salée (groupe témoin). Les scores de douleur et les effets secondaires ont été évalués à 1, 2, 4, 8, 12 et 24 h après l’intervention. On a comparé les temps moyens de la première administration d’analgésique et quelles en étaient les doses cumulatives postopératoires demandées pendant 24 h.
Résultats
Le temps moyen pour la première analgésie a été plus long chez les patientes qui ont reçu 100 mg (4,5 ±3,1 h) ou 200 mg (6,6 ± 3,4 h) de tramadol que chez celles qui n’ont reçu que le placebo (2,8 ± 2 h). Pendant 24 h après la césarienne, les doses moyennes cumulatives de mépéridine ont été moindres dans les groupes I et II (0,3 ± 0,3 mg·kg−1; 0,3 ± 0,3 mg·kg−1) que dans le groupe témoin (0,7 ± 0,4 mg·kg−1) et les doses moyennes de diclofénac ont été plus faibles dans les groupes I et II (156 ± 59 mg; 142 ± 62 mg) que dans le groupe témoin (214 ± 70 mg). Cependant, aucune différence n’a été notée entre les patientes des groupes I et II, et ce, pour tous les paramètres étudiés.
Conclusion
Ladministration épidurale de 100 mg de tramadol peut fournir une analgésie postopératoire adéquate sans dépression respiratoire chez des patientes qui ont subi une césarienne.
Article PDF
Similar content being viewed by others
References
Uchiyama A, Ueyama H, Nakano S, Nishimura M, Tashiro C. Low dose intrathecal morphine and pain relief following cesarean section. Int J Obst Anesth 1994; 3: 87–91.
Abouleish E, Rawal N, Fallon K, Hernandez D. Combined intrathecal morphine and bupivacaine for cesarean section. Anesth Analg 1988; 67: 370–4.
Chadwick HS, Ready LB. Intrathecal and epidural morphine sulfate for postcesarean analgesia — a clinical comparison. Anesthesiology 1988; 68: 925–9.
Abboud TK, Dror A, Mosaad P, et al. Mini-dose intracheal morphine for the relief of post-cesarean section pain: safety, efficacy and ventilatory responses to carbon dioxide. Anesth Analg 1988; 67: 137–43.
Rosen MA, Hugbes SC, Shnider SM, et al. Epidural morphine for the relief of postoperative pain after cesarean delivery. Anesth Analg 1983; 62: 666–72.
Raffa RB, Friderichs E, Reimann W, Shank RP, Codd EE, Vaught JL. Opioid and nonopioid components independently contribute to the mechanism of action of tramadol, an ‘atypical’ opioid analgesic. J Pharmacol Exp Ther 1992; 260: 275–85.
Houmes R-JM, Voets MA, Verkaaik A, Erdmann W, Lachmann B. Efficacy and safety of tramadol versus morphine for moderate and severe postoperative pain with special regard to respiratory depression. Anesth Analg 1992; 74: 510–4.
Vickers MD, O’Flaherty D, Szekely SM, Read M, Yoshizumi J. Tramadol: pain relief by an opioid without depression of respiration. Anaesthesia 1992; 47: 291–6.
Eggers KA, Power I. Tramadol (Editorial). Br J Anaesth 1995; 74: 247–9
Sunshine A, Olson NZ, Zighelboim I, DeCastro A, Minn FL. Analgesic oral efficacy of tramadol hydrochloride in postoperative pain. Clin Pharmacol Ther 1992; 51: 740–6.
Carlsson K-H, Jurna I. Effects of tramadol on motor and sensory responses of the spinal nociceptive system in the rat. Eur J Pharmacol 1987; 139: 1–10.
Baraka A, Jabbour S, Ghabash M, Nader A, Khoury G, Sibai A. A comparison of epidural tramadol and epidural morphine for postoperative analgesia. Can J Anaesth 1993; 40: 308–13.
Delilkan AE, Vijayan R. Epidural tramadol for postoperative pain relief. Anaesthesia 1993; 48: 328–31.
Wolfe MJ, Nicholas ADG. Selective epidural analgesia (Letter). Lancet 1979; 2: 150–1.
Kotelko DM, Dailey PA, Shnider SM, Rosen MA, Hughes SC, Brizgys RV. Epidural morphine analgesia after Cesarean delivery. Obstet Gynecol 1984; 63: 409–13.
Etches RC, Sandier AN, Daley MD. Respiratory depression and spinal opioids. Can J Anaesth 1989; 36: 165–85.
Cousins MJ, Mather LE. Intrathecal and epidural administration of opioids. Anesthesiology 1984; 61: 276–310.
Bromage PR. The price of intraspinal narcotic analgesia: basic constraints (Editorial). Anesth Analg 1981; 60: 461–3.
Rawal N, Wattwil M. Respiratory depression after epidural morphine — an experimental and clinical study. Anesth Analg 1984; 63: 8–14.
Hennies HH, Friderichs E, Schneider J. Receptor binding, analgesic and antitussive potency of tramadol and other selected opioids. Azzneimittel-Forshung/Drug Research 1988; 38: 877–80.
Dhasmana KM, Banerjee AK, Rating W, Erdmann W. Analgesic effect of tramadol in the rat. Chung Kuo Yao Li Hsueh Pao — Acta Pharmacologica Sinica 1989; 10: 289–93.
Kayser V, Besson J-M, Guildbaud G. Effects of the analgesic agent tramadol in normal and arthritic rats; comparison with the effects of different opioids, including tolerance and cross-tolerance ot morphine. Eur J Pharmacol 1991; 195: 37–45.
Baraka A, Noueihid R, Hajj S. Intrathecal injection of morphine for obstetric analgesia. Anesthesiology 1981, 54: 136–40.
Lee CR, McTavish D, Sorkin EM. Tramadol. A preliminary review of its pharmacodynamic and pharmacokinetic properties, and therapeutic potential in acute and chronic pain states. Drugs 1993; 46: 313–40.
Dennis AR, Leeson-Payne CG, Hobbs GJ. Analgesia after Caesarean section. Anaesthesia 1995; 50: 297–9.
Cardoso MMSC, Carvalho JCA, Amaro AR, Prado AA, Cappelli EL. Small doses of intrathecal morphine combined with systemic diclofenac for postoperative pain control after cesarean delivery. Anesth Analg 1998; 86: 538–41.
Power I, Chambers WA, Greer IA, Ramage D, Simon E. Platelet function after intramuscular diclofenac. Anaesthesia 1990; 45: 916–9.
Andersson K-E, Forman A, Ulmsten U. Pharmacology of labor. Clin Obstet Gynecol 1983; 26: 56–77.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Siddik-Sayyid, S., Aouad-Maroun, M., Sleiman, D. et al. Epidural tramadol for postoperative pain after Cesarean section. Can J Anesth 46, 731–735 (1999). https://doi.org/10.1007/BF03013907
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03013907