Abstract
Purpose
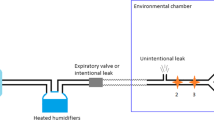
To determine the effect of heat and moisture exchange (HME) on the tracheobronchial tree (TBT) using a unidirectional anesthesic circuit with or without CO2 absorber and high or low fresh gas flow (FGF), in dogs.
Methods
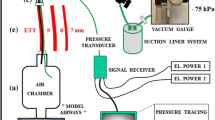
Thirty-two dogs were randomly allocated to four groups: G1 (n = 8) valvular circuit without CO2 absorber and high FGF (5 L· min−1); G2 (n=8) as G1 with HME; G3 (n=8) circuit with CO2 absorber with a low FGF (1 L· min−1); G4 (n=8) as G3 with HME. Anesthesia was induced and maintained with pentobarbital. Tympanic temperature (TT), inhaled gas temperature (IGT), relative (RH) and absolute humidity (AH) of inhaled gas were measured at 15 (control), 60, 120 and 180 min of controlled ventilation. Dogs were euthanized and biopsies in the areas of TBT were performed by scanning electron microscopy.
Results
The G2 and G4 groups showed the highest AH (> 20 mgH2O· L−1) and G1 the lowest (< 10 mgH2O· L−1) and G3 was intermediate (< 20 mgH2O· L−1) (P < 0.01), There was no difference of TT and IGT among groups. Alterations of the mucociliary system were greatest in G1, least in G2 and G4, and intermediate in G3.
Conclusion
In dogs, introduction of HME to a unidirectional anesthetic circuit with/without CO2 absorber and high or low FGF preserved humidity of inspired gases. HME attenuated but did not prevent alterations of the mucociliary system of the TBT.
Objectif
Déterminer, chez des chiens, l’effet de l’échange de chaleur et d’humidité (ECH) sur l’arbre trachéobronchique (ATB) en utilisant un circuit anesthésique unidirectionnel avec ou sans absorption de CO2 et un haut ou bas débit de gaz frais (DGF).
Méthode
Trente-deux chiens ont été répartis au hasard en quatre groupes: G1 (n=8), un circuit à valve sans absorption de CO2 et avec un haut DGF (5 L· min−1); G2 (n=8), comme G1 avec ECH; G3 (n = 8), un circuit avec absorption de CO2 et un bas DGF (1 L· min−1); G4 (n = 8), comme G3 avec ECH. L’anesthésie a été induite et maintenue avec du pentobarbital. La température tympanique (TT), la température des gaz inhalés (TGI), l’humidité relative (HR) et absolue (HA) des gaz inhalés ont été mesurées après 15 (témoin), 60, 120 et 180 min de ventilation contrôlée. Les chiens ont été sacrifiés et des biopsies de l’ATB ont été réalisées par microscopie électronique à balayage.
Résultats
Les groupes G2 et G4 ont affiché les plus hauts taux d’HA (> 20 mgH2O· L−1), G1 avait le plus bas taux (< 10 mgH2O· L−1) et G3 était intermédiaire (< 20 mgH2O· L−1) (P < 0,01). Il n’y a pas eu de différence intergroupe concernant la TT et la TGI. Les modifications du système mucociliaire ont été plus importantes dans le G1, moindres dans les G2 et G4 et intermédiaires dans le G3.
Conclusion
L’introduction, chez des chiens, d’un ECH à un circuit anesthésique avec ou sans absorption de CO2 et avec un haut ou bas DGF a préservé l’humidité des gaz inhalés. L’ECH a diminué, mais n’a pas empêché, les modifications du système mucociliaire de l’ATB.
Article PDF
Similar content being viewed by others
References
McFadden ER, Pichurko BM, Bowman HF, et al. Thermal mapping of the airways in humans. J Appl Physiol 1985; 58: 564–70.
Noguchi H, Takumi Y, Aochi O. A study of humidification in tracheostomized dogs. Br J Anaesth 1973; 45: 844–8.
van Oostdam JC, Walker DC, Knudson K, Dirks P, Dahlby RW, Hogg JC. Effect of breathing dry air on structure and function of airways. J Appl Physiol 1986; 61: 312–7.
Shelly MP, Lloyd GM, Park GR. A review of the mechanisms and methods of humidification of inspired gases. Intensive Care Med 1988; 14: 1–9.
Williams R, Rankin N, Smith T, Galler D, Seakins P. Relationship between the humidity and temperature of inspired gas and function of the airway mucosa. Crit Care Med 1996; 24: 1920–9.
Tsuda T, Noguchi H, Takumi T, Aochi O. Optimum humidification of air administred to a tracheostomy in dogs. Scanning electron microscopy and surfactant studies. Br J Anaesth 1977; 49: 965–77.
Chalon J, Loew DAY, Malebranche J. Effects of dry anesthetic gases on tracheobronchial ciliated epithelium. Anesthesiology 1972; 37: 338–43.
Hirsch JA, Tokayer JL, Robinson MJ, Sackner MA. Effects of dry air and subsequent humidification on tracheal mucous velocity in dogs. J Appl Physiol 1975; 39: 242–6.
Kleemann PP. Humidity of anaesthetic gases with respect to low flow anaesthesia. Anaesth Intensive Care 1994; 22: 396–408.
Henriksson B-A, Sundling J, Hellman A. The effect of a heat and moisture exchanger on humidity in a low-flow anaesthesia system. Anaesthesia 1997; 52: 144–9.
Déry R. The evolution of heat and moisture in the respiratory tract during anaesthesia with a nonrebreathing system. Can Anaesth Soc J 1973; 20: 296–309.
Tubelis A, Do Nascimento FJL. Umidade do ar.In: Metereologia Descritiva: Fundamentos e Aplicações Brasileiras. São Paulo: Editora Distribuidora Brasil 1980: 94–127.
Chazalet J-J, Eurin B. Utilisation des filtres et des échangeurs de chaleur et d’humidité en anesthésiologie. Encycl Méd Chir, Anesth Réanim, 36180 A40, 1991: 1–4.
Bickler PE, Sessler DI. Efficiency of airway heat and moisture exchangers in anesthetized humans. Anesth Analg 1990; 71: 415–8.
Eckerbom B, Lindholm C-E, Mannting F. Mucociliary transport with and without the use of a heat and moisture exchanger. An animal study. Acta Anaesthesiol Scand 1991; 35: 297–301.
Deriaz H, Fiez N, Lienhart A. Comparative effects of a hygrophobic filter and a heated humidifier on intraoperative hypothermia. (French) Ann Fr Anesth Réanim 1992; 11: 145–9.
Haslam KR, Nielsen CH. Do passive heat and moisture exchangers keep the patient warm? Anesthesiology 1986; 64: 379–81.
Lloyd G, Howells J, Liddle C, Klineberg PL. Barriers to hepatitis C transmission within breathing systems: efficacy of a pleated hydrophobic filter. Anaesth Intensive Care 1997; 25: 235–8.
Chalon J, Markham JP, Ali MM, Ramanathtan S, Turndorf H. The pall ultipor breathing circuit filter —an efficient heat and moisture exchanger. Anesth Analg 1984; 63: 566–70.
Turtle MJ, Ilsley AH, Rutten AJ, Runciman WB. An evaluation of six disposable heat and moisture exchangers. Anaesth Intensive Care 1987; 15: 317–22.
Cornaggia G, Chidini G, Stella I, Clinical evaluation on four HMEs during general anaesthesia. (Italian) Minerva Anestesiol 1994; 60: 649–55.
Aldrete JA, Cubillos P, Sherrill D. Humidity and temperature changes during low flow and closed system anaesthesia. Acta Anaesthesiol Scand 1981; 25: 312–4.
Chalon J, Ali M, Ramanathan S, Turndorf H. The humidification of anaesthetic gases. Its importance and control. Can Anaesth Soc J 1979; 26: 361–6.
Mebius C. A comparative evaluation of disposable humidifiers. Acta Anaesthesiol Scand 1983; 27: 403–9.
Martins RHG, Braz JRC, Defaveri J, Curi PR. Study of humidification and heating of inspired gases during mechanical ventilation in dogs. (Portuguese) Rev Bras Otorrinolaringol 1996; 62: 206–18.
Savarese JJ, Miller RD, Lien CA, Caldwell JE. Pharmacology of muscle relaxants and their antagonists.In: Miller ED. (Ed.). Anesthesia, 4th ed, New York: Churchill Livingstone Inc., 1994: 417–87.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bisinotto, F.M.B., Braz, J.R.C., Martins, R.H.G. et al. Tracheobronchial consequences of the use of heat and moisture exchangers in dogs. Can J Anesth 46, 897–903 (1999). https://doi.org/10.1007/BF03012983
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03012983