Abstract
Purpose
To compare the efficacy of tramadol and morphine for intra-and postoperative analgesia in patients undergoing laparoscopic cholecystectomy.
Methods
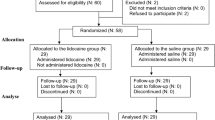
In a prospective, randomized, double-blind study 100 patients were allocated randomly into two groups. Ten minutes before induction of anaesthesia, patients in group I received 100 mg tramadol and those in group 2 received 10 mg morphineiv. Anaesthesia was induced with 5 mg·kg−1 thiopental and was maintained with O2, N2O plus isoflurane with additional doses of tramadol or morphine as decided by the attending anaesthetist. Postoperatively, patients in group I and group 2 received tramadol and morphine, respectively, from a patient-controlled analgesia (PCA) device. Pain, analgesic consumption, vital signs and side effects were recorded postoperatively for 24 hr.
Results
Intraoperative consumption of tramadol and morphine were 137 ± 37 and 12.2 ± 3 mg, respectively. Compared with morphine, patients receiving tramadol had higher blood pressures and required greater mean ETiso to control haemodynamic variables (P < 0.05). Postoperatively, there were no differences in observer pain score or visual analogue pain score during the first 24 hr between groups except at 30, 45, and 90 min where patients in the tramadol group reported higher pain scores (P < 0.05). The cumulative, 24 hr PCA consumption was III ± 93 and 7.5 ± 6.6 mg of tramadol and morphine, respectively.
Conclusions
There was no difference between the use of tramadol and morphine to treat pain after laparoscopic cholecystectomy from 90 min after the end of surgery. Morphine was more effective than tramadol as an intraoperative analgesic.
Résumé
Objectif
Comparer l’efficacité du tramadol et de la morphine pour l’analgésie peropératoire et postopératoire de patients devant subir une cholécystectomie laparoscopique.
Méthode
Lors d’une étude prospective, randomisée et en double aveugle, 100 patients ont été répartis au hasard en deux groupes. Dix minutes avant l’induction de l’anesthésie, les patients du groupe I ont reçu 100 mg de tramadol et ceux du groupe 2, 10 mg de morphineiv. Lanesthésie a été induite avec 5 mg·kg−1 de thiopental et a été maintenue avec un mélange d’O2 et de N2O plus de l’isoflurane et des doses supplémentaires de tramadol ou de morphine selon la décision de l’anesthésiste traitant. Après l’intervention, les patients des groupes 1 et 2 ont reçu respectivement du tramadol et de la morphine à l’aide d’un dispositif d’analgésie contrôlée par le patient (ACP). En période postopératoire également, on a enregistré pendant 24 heures la douleur, la consommation d’analgésiques, les signes vitaux et les effets secondaires.
Résultats
La consommation peropératoire de tramadol et de morphine a été de 137 ± 37 et de 12,2 ± 3 mg, respectivement. Comparativement, les patients qui ont reçu du tramadol ont présenté une tension artérielle plus élevée et ont eu besoin d’isofluraneTE (télé-expiratoire) de moyenne plus élevée pour contrôler les variables hémo-dynamiquesP < 0,05). Il n’y a pas eu de différence de douleur postopératoire entre les groupes d’après les niveaux enregistrés par un observateur ou par l’échelle visuelle analogique, pendant les 24 premières heures, sauf à 30, 45 et 90 min alors que les patients du groupe ayant reçu du tramadol ont éprouvé des douleurs plus intenses (P < 0,05). La consommation totale des 24 h d’ACP a été de 111 ±93 et de 7,5 ± 6,6 mg de tramadol et de morphine, respectivement.
Conclusion
À partir de 90 min après la chirurgie, il n’y a pas de différence entre l’usage de tramadol ou de morphine pour traiter la douleur consécutive à la cholécystectomie laparoscopique. La morphine a été plus efficace que le tramadol en tant qu’analgésique peropératoire.
Article PDF
Similar content being viewed by others
References
Ruffa RB, Friderichs E, Reimann W, Shank RP, Codd EE, Vaught JL. Opioid and non-opioid components independently contribute to the mechanism of action of tramadol, an ‘atypical’ opioid analgesic. J Pharmacol Exp Ther 1992; 260: 275–85.
Hennies H-H, Friderichs E, Schneider J. Receptor binding, analgesic and antitussive potency of tramadol and other selected opioids. Arzneimittelforschung 1988; 38; 877–80.
Houmes R-JM, Voets MA, Verkaaik A, Erdmann W, Lachmann B. Efficacy and safety of tramadol versus morphine for moderate and severe postoperative pain with special regard to respiratory depression. Anesth Analg 1992; 74: 510–4.
Lehmann KA, Kratzenberg U, Schroeder-Bark B, Horrichs-Haermeyer G. Postoperative patient-controlled analgesia with tramadol: analgesic efficacy and minimum effective concentrations. Clin J Pain 1990; 6: 212–20.
Kupers R, Callebaut V, Debois V, et al. Efficacy and safety of oral tramadol and pentazocine for postoperative pain following prolapsed intervertebral disc repair. Acta Anæsthesiol Belg 1995; 46: 31–7.
James MFM, Heijke SAM, Gordon PC. Intravenous tramadol versus epidural morphine for postthoracotomy pain relief: a placebo-controlled double-blind study. Anesth Analg 1996; 83: 87–91.
Ng KFJ, Tsui SL, Yang JCS, Ho ETF. Comparison of tramadol and tramadol/droperidol mixture for patient-controlled analgesia. Can J Anaesth 1997; 44: 810–5.
Lehmann KA, Horrichs G, Hoeckle W. Tramadol as an intraoperative analgesic. A randomised double-blind study with placebo. Anaesthesist 1985; 34: 11–9.
Coetzee JF, Maritz JS, Du Toit JC. Effect of tramadol on depth of anaesthesia. Br J Anaesth 1996; 76: 415–8.
Lauretti GR, Mattos AL, Lima IC. Tramadol and beta-cyclodextrin piroxicam. Effective multimodal balanced analgesia for the intra-and postoperative period. Reg Anesth 1997; 22: 243–8.
Desmeules JA, Piguet V, Collart L, Dayer P. Contribution of monoaminergic modulation to the analgesic effect of tramadol. Br J Clin Pharmacol 1996; 41: 7–12.
Joris JL, Noirot DP, Legrand MJ, Jacquet NJ, Lamy ML. Hemodynamic changes during laparoscopic chole-cystectomy. Anesth Analg 1993; 76: 1067–71.
Rademaker BM, Ringers J, Odoom JA, de Wit LT, Kalkman CJ, Oosting J. Pulmonary function and stress response after laparoscopic cholecystectomy: comparison with subcostal incision and influence of thoracic epidural analgesia. Anesth Analg 1992; 75: 381–5.
Holohan TV. Laparoscopic cholecystectomy. Lancet 1991; 338: 801–3.
Rose DK, Cohen MM, Soutter DI. Laparoscopic chole-cystectomy: the anaesthetist’s point of view. Can J Anaesth 1992; 39: 809–15.
Joris J, Thiry E, Paris P, Weerts J, Lamy M. Pain after laparoscopic cholecystectomy: characteristics and effect of intraperitoneal bupivacaine. Anesth Analg 1995; 81: 379–84.
Scheinin B, Kellokumpu I, Lindgren L, Haglund C, Rosenberg PH. Effect of intraperitoneal bupivacaine on pain after laparoscopic cholecystectomy. Acta Anaesthesiol Scand 1995; 39: 195–8.
Fredman B, Jedeikin R, Olsfanger D, Flor P, Gruzman A. Residual pneumoperitoneum: a cause of postoperative pain after laparoscopic cholecystectomy. Anesth Analg 1994; 79: 152–4.
Alexander JI. Pain after laparoscopy. Br J Anaesth 1997; 79: 369–78.
Vickers MD, Pamvicini D. Comparison of tramadol with morphine for post-operative pain following abdominal surgery. Eur J Anaesthesiol 1995; 12: 265–71.
Baraka A, Jabbour S, Ghabash M, Nader A, Khoury G, Sibai A. A comparison of epidural tramadol and epidural morphine for postoperative analgesia. Can J Anaesth 1993; 40: 308–13.
Vickers MD, O’Flaherty D, Szekely SM, Read M, Yoshizumi J. Tramadol: pain relief by an opioid without depression of respiration. Anaesthesia 1992; 47: 291–6.
Naguib M, El Bakry AK, Khoshim MHB, et al. Prophylactic antiemetic therapy with ondansetron, tropisetron, granisetron and metoclopramide in patients undergoing laparoscopic cholecystectomy: a randomized, double-blind comparison with placebo. Can J Anaesth 1996; 43: 226–31.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Naguib, M., Seraj, M., Attia, M. et al. Perioperative antinociceptive effects of tramadol. A prospective, randomized, double-blind comparison with morphine. Can J Anaesth 45, 1168–1175 (1998). https://doi.org/10.1007/BF03012458
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03012458