Abstract
Background
Obesity is a growing epidemic in the United States, and little is known about the characteristics of the morbidly obese population (body mass index [BMI] <40 kg/m) undergoing stress myocardial perfusion imaging (MPI).
Methods and Results
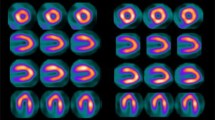
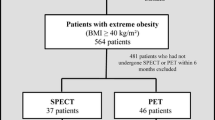
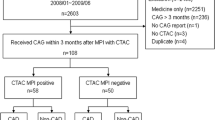
We retrospectively reviewed all consecutive morbidly obese patients without known coronary artery disease presenting for a clinically indicated technetium 99m (Tc-99m) gated stress single photon emission computed tomography imaging study over a 42-month period. Studies were analyzed for image quality, for the contribution of attenuation correction to image interpretation, and for the hemodynamic response to pharmacologic stress. In patients who subsequently had cardiac catheterization, the results were compared with those from the initial MPI study, and the Social Security Death Index and hospital medical records were searched to the assess survival rate in the entire cohort. A total of 433 patients were identified with a mean BMI of 47.3 ± 8 kg/m2 and a mean Tc-99m stress dose of 35.6 ± 5.4 mCi. Image quality was good in 61% of the patients, adequate in 37%, and poor in 2%. It was found to be dependent on the Stressor used (better with exercise) but did not correlate with increasing weight or BMI. Attenuation correction was used in 95% of the studies reviewed and was helpful for image interpretation in 60%. The heart rate response to dipyridamole and adenosine was more pronounced and the blood pressure response to dipyridamole was less pronounced in morbidly obese patients compared with nonobese control patients. In the 43 patients who underwent catheterization, stress MPI had a sensitivity of 95% and negative predictive value of 80%. Kaplan-Meier survival analysis at 1 year showed a significant difference in survival rate of 98.3% for normal MPI studies and 94.0% for abnormal MPI studies (P = .02).
Conclusion
Diagnostic-quality single photon emission computed tomography imaging is feasible in the majority (98%) of morbidly obese patients with the use of a dual-head camera, attenuation correction, and high stress Tc-99m tracer doses. Exercise stress was associated with better image quality. The prognostic value of a normal MPI study in this population appears to be less favorable than in non-morbidly obese patients.
Similar content being viewed by others
References
Overweight and obesity threaten U.S. health gains: communities can help address the problem, Surgeon General says [press release] Washington, DC: US Department of Health and Human Services; 2001.
Grundy SM. Obesity, metabolic syndrome, and cardiovascular disease. J Clin Endocrinol Metab 2004;89:2595–600.
Eckel RH, Krauss RM. American Heart Association call to action: obesity as a major risk factor for coronary heart disease. AHA Nutrition Committee. Circulation 1998;97:2099–100.
Kim KS, Owen WL, Williams D, Adams-Campbell LL. A comparison between BMI and Conicity index on predicting coronary heart disease: the Framingham Heart Study. Ann Epidemiol 2000;10:424–31.
Rimm EB, Stampfer MJ, Giovannucci E, Ascherio A, Spiegelman D, Colditz GA, et al. Body size and fat distribution as predictors of coronary heart disease among middle-aged and older US men. Am J Epidemiol 1995;141:1117–27.
Clinical guidelines on the identification, evaluation and treatment of overweight and obesity in adults: the evidence report. Bethesda (MD): National Institutes of Health; 1998.
Wang TJ, Parise H, Levy D, D’Agostino RB Sr, Wolf PA, Vasan RS, et al. Obesity and the risk of new-onset atrial fibrillation. JAMA 2004;292:2471–7.
Sowers JR. Obesity as a cardiovascular risk factor. Am J Med 2003;115(Suppl 8A):37S-41S.
Haffner S, Taegtmeyer H. Epidemic obesity and the metabolic syndrome. Circulation 2003;108:1541–5.
Bahadori B, Neuer E, Schumacher M, Fruhwald F, Eber B, Klein W, et al. Prevalence of coronary artery disease in obese versus lean men with angina pectoris and positive exercise stress test. Am J Cardiol 1996;77:1000-l.
McNulty PH, Ettinger SM, Field JM, Gilchrist IC, Kozak M, Chambers CE, et al. Cardiac catheterization in morbidly obese patients. Catheter Cardiovasc Interv 2002;56:174–7.
Kip KE, Marroquin OC, Kelley DE, Johnson BD, Kelsey SF, Shaw LJ, et al. Clinical importance of obesity versus the metabolic syndrome in cardiovascular risk in women: a report from the Women’s Ischemia Syndrome Evaluation (WISE) study. Circulation 2004;109:706–13.
Madu EC. Transesophageal dobutamine stress echocardiography in the evaluation of myocardial ischemia in morbidly obese subjects. Chest 2000;117:657–61.
Hendel RC, Wackers FJ, Berman DS, Ficaro E, Depuey EG, Klein L, et al. American Society of Nuclear Cardiology consensus statement: reporting of radionuclide myocardial perfusion imaging studies. J Nucl Cardiol 2003;10:705–8.
Thompson RC, Heller GV, Johnson LL, Case JA, Cullom SJ, Garcia EV, et al. Value of attenuation correction on ECG-gated SPECT myocardial perfusion imaging related to body mass index. J Nucl Cardiol 2005;12:195–202.
Hachamovitch R, Berman DS, Shaw LJ, Kiat H, Cohen I, Cabico JA, et al. Incremental prognostic value of myocardial perfusion single photon emission computed tomography for the prediction of cardiac death: differential stratification for risk of cardiac death and myocardial infarction. Circulation 1998;97:535–43.
Berman DS, Kang X, Hayes SW, Friedman JD, Cohen I, Abidov A, et al. Adenosine myocardial perfusion single-photon emission computed tomography in women compared with men. Impact of diabetes mellitus on incremental prognostic value and effect on patient management. J Am Coll Cardiol 2003;41:1125–33.
Hachamovitch R, Berman DS, Kiat H, Cohen I, Friedman JD, Shaw LJ. Value of stress myocardial perfusion single photon emission computed tomography in patients with normal resting electrocardiograms: an evaluation of incremental prognostic value and cost-effectiveness. Circulation 2002; 105:823–9.
Hachamovitch R, Berman DS, Kiat H, Cohen I, Lewin H, Amanullah A, et al. Incremental prognostic value of adenosine stress myocardial perfusion single-photon emission computed tomography and impact on subsequent management in patients with or suspected of having myocardial ischemia. Am J Cardiol 1997;80:426–33.
Giri S, Shaw LJ, Murthy DR, Travin MI, Miller DD, Hachamovitch R, et al. Impact of diabetes on the risk stratification using stress single-photon emission computed tomography myocardial perfusion imaging in patients with symptoms suggestive of coronary artery disease. Circulation 2002; 105:32–40.
Gibbons RJ, Hodge DO, Berman DS, Akinboboye OO, Heo J, Hachamovitch R, et al. Long-term outcome of patients with intermediate-risk exercise electrocardiograms who do not have myocardial perfusion defects on radionuclide imaging. Circulation 1999;100:2140–5.
Abidov A, Bax JJ, Hayes SW, Hachamovitch R, Cohen I, Gerlach J, et al. Transient ischemic dilation ratio of the left ventricle is a significant predictor of future cardiac events in patients with otherwise normal myocardial perfusion SPECT. J Am Coll Cardiol 2003;42:1818–25.
Schisterman EF, Whitcomb BW. Use of the Social Security Administration Death Master File for ascertainment of mortality status. Popul Health Metr 2004;2:2.
Cowper DC, Kubal JD, Maynard C, Hynes DM. A primer and comparative review of major US mortality databases. Ann Epidemiol 2002;12:462–8.
Hill ME, Rosenwaike I. The Social Security Administration’s Death Master File: the completeness of death reporting at older ages. Soc Secur Bull 2001;64:45–51.
Sesso HD, Paffenbarger RS, Lee IM. Comparison of National Death Index and World Wide Web death searches. Am J Epidemiol 2000;152:107-ll.
Lash TL, Silliman RA. A comparison of the National Death Index and Social Security Administration databases to ascertain vital status. Epidemiology 2001;12:259–61.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Duvall, W.L., Croft, L.B., Corriel, J.S. et al. SPECT myocardial perfusion imaging in morbidly obese patients: Image quality, hemodynamic response to pharmacologic stress, and diagnostic and prognostic value. J Nucl Cardiol 13, 202–209 (2006). https://doi.org/10.1007/BF02971244
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF02971244