Abstract
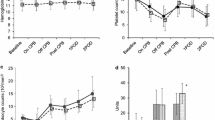
Objective: The usefulness of heparin-bonded circuits under normothermic cardiopulmonary bypass has not been elucidated. We studied platelet activation and aggregation differences between heparin-bonded and nonheparin-bonded circuits in patients undergoing surgery involving normothermic cardiopulmonary bypass.Methods: Eight patients underwent coronary artery bypass grafting with non heparin-bonded circuits (controls) and 7 the same with heparin-bonded circuits (heparin group). Heparin bonding was applied to the blood contact surface of our system, including the oxygenator and connecting tubes. Patient body temperature was kept between 36 and 37°C. Beta-thromboglobulin and platelet factor 4 were measured before, during, and after cardiopulmonary bypass, and platelet aggregation was evaluated by laser-light scattering.Results: Changes in beta-thromboglobulin and platelet factor 4 during and after cardiopulmonary bypass were similar in both groups. Small particle formation was the primary aggregate induced during and after cardiopulmonary bypass in both groups, and serial changes in particle formation up to 24 hours after cardiopulmonary bypass were similar in both groups.Conclusions: Our results indicate that in 2–3 hours of normothermic cardiopulmonary bypass, heparin-bonded circuits are similar to nonheparin-bonded ones in platelet compatibility.
Similar content being viewed by others
References
Baufreton C, Moczar M, Intrator L, et al. Inflammatory response to cardiopulmonary bypass using two different types of heparin-coated extracorporeal circuits. Perfusion 1998; 13: 419–27.
te Velthuis H, Baufreton C, Jansen PGM, Thijs CM, Hack CE, Sturk A, et al. Heparin coating of extracorporeal circuits inhibits contact activation during cardiac operations. J Thorac Cardiovasc Surg 1997; 114: 117–22.
Ashraf S, Tian Y, Cowan D, Entress A, Martin PG, Watterson KG. Release of proinflammatory cytokines during pediatric cardiopulmonary bypass: heparinbonded versus nonbonded oxygenators. Ann Thorac Surg 1997; 64: 1790–4.
Gu YJ, van Oeveren W, Akkerman C, Boonstra PW, Huyzen RJ, Wildevuur CRH. Heparin-coated circuits reduce the inflammatory response to cardiopulmonary bypass. Ann Thorac Surg 1993; 55: 917–22.
Videm V, Svennevig JL, Fosse E, Semb G, Osterud A, Mollnes TE. Reduced compliment activation with heparin-coated oxygenator and tubings in coronary artery bypass operations. J Thorac Cardiovasc Surg 1992; 103: 806–13.
Videm V, Mollness TE, Bergh K, Fosse E, Mohr B, Hagve TA, et al. Heparin-coated cardiopulmonary bypass equipment. II. Mechanisms for reduced compliment activation in vivo. J Thorac Cardiovasc Surg 1999; 117: 803–9.
te Velthuis H, Jansen PGM, Hack CE, Eijsman L, Wildevuur CRH. Specific compliment inhibition with heparin-coated extracorporeal circuits. Ann Thorac Surg 1996; 61: 1153–7.
Kawahito K, Mohara J, Misawa Y, Kato M, Fuse K. Assessment of the myocardial protective effect of antegrade warm blood cardioplegia by measuring the release of biochemical markers. Jpn J Surg 1999; 29: 322–6.
Ozaki Y, Satoh K, Yatomi Y, Yamamoto T, Shirasawa Y, Kume S. Detection of platelet aggregates with a particle counting method using light scattering. Anal Biochem 1994; 218: 284–94.
Yamamoto T, Egawa Y, Shirasawa Y, et al. A laser light scattering in situ system for counting aggregates in blood platelet aggregation. Meas Sci Technol 1995; 6: 174–80.
Tohgi H, Takahashi H, Watanabe K, Kuki H, Shirasawa Y. Development of large platelet aggregates from small aggregates as determined by laser-light scattering: effects of aggregant concentration and antiplatelet medication. Thromb Haemost 1996; 75: 838–43.
Kawahito K, Kobayashi E, Iwasa H, Misawa Y, Fuse K. Platelet aggregation during cardiopulmonary bypass evaluated by a laser light-scattering method. Ann Thorac Surg 1999; 67: 79–84.
Wendel HP, Heller W, Gallimore MJ, Hoffmeister HE. Heparin-coated oxygenators significantly reduce contact system activation in an in vivo cardiopulmonary bypass model. Blood Coag and Fibrinol; 1994; 5: 673–8.
Nakajima T, Osawa S, Ogawa M, Sasaki T, Izumoto H, Yagi Y, et al. Clinical study of platelet function and coagulation/fibrinolysis with Duraflo II heparin coated cardiopulmonary bypass equipment. ASAIO J 1996; 42: 301–5.
Wagner WR, Johnson PC, Thompson KA, Marrone GC. Heparin-coated cardiopulmonary bypass circuits: hepmostatic alterations and postoperative blood loss. Ann Thorac Surg 1994; 58: 734–41.
Jansen PGM, te Velthuis H, Huybregts RAJM, Paulus R, Bulder ER, van der Spoel HI, et al. Reduced compliment activation and improved postoperative performance after cardiopulmonary bypass with heparincoated circuits. J Thorac Cardiovasc Surg 1995; 110: 829–34.
Hennein HA, Ebba H, Rodriguez JL, et al. Relationship of the proinflammatory cytokines to myocardial ischemia and dysfunction after uncomplicated coronary revascularization. J Thorac Cardiovasc Surg 1994; 108: 626–35.
Korn RL, Fisher CA, Livingston ER, Stenach N, Fishman SJ, Jeevanandam V, et al. The effects of Cameda bioactive surface on human blood components during simulated extracorporeal circulation. J Thorac Cardiovasc Surg 1996; 111: 1073–84.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Misawa, Y., Konishi, H., Kawahito, K. et al. Platelet activation and aggregation during normothermic cardiopulmonary bypass. Jpn J Thorac Cardiovasc Surg 49, 21–28 (2001). https://doi.org/10.1007/BF02913119
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF02913119