Abstract
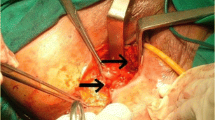
Transanal rectal advancement flap (TRAF) is a surgical option in the management of rectovaginal and other complicated fistulas involving the anorectum. Most reported series have a short follow-up. PURPOSE: This study was undertaken to determine the long-term success, safely, applicability, and factors affecting recurrence in patients managed with TRAF, including patients with Crohn's disease. METHODS/MATERIALS: Retrospective analysis of all patients undergoing endorectal advancement flaps at a single institution between 1988 and 1993 was performed. One hundred one patients were identified (70 percent female; 30 percent male). Included were 52 patients with rectovaginal, 46 with anal perineal, and 3 with rectourethral fistulas. Causes were obstetric injury in 13 patients, Crohn's disease in 47, cryptoglandular in 19, mucosal ulcerative colitis in 7, and surgical trauma or undefined causes in 15 patients. RESULTS: No mortality occurred. Median follow-up was 31 (range, 1–79 months). Immediate failure (within one week of the repair) was seen in 6 percent of patients. Statistically (tP <0.001) higher recurrence rates were observed in patients who had undergone previous repairs. Mean hospital stay was four days. Overall recurrence was seen in 29 patients (29 percent). Seventy-five percent of all recurrences occurred within the first 15 months; however, recurrence was noted for up to 55 months after repair. Etiology of fistula, use of constipating medications, antibiotic use, and most importantly associated Crohn's disease did not statistically affect recurrence rates. Failure rate was only influenced by previous number of repairs. CONCLUSION: TRAF is a safe technique for managing complicated anorectal and rectovaginal fistulas, including patients with Crohn's disease. Long-term follow-up is essential to accurately report recurrence rates.
Similar content being viewed by others
References
Ramanujam PS. The role of seton in fistulotomy of the anus. Surg Gynecol Obstet 1983;157:419–22.
Culp CE. Use of Penrose drains to treat certain anal fistulas: a primary operative seton. Mayo Clin Proc 1989;59:613–7.
Kuypers HC. Use of the seton in the treatment of extra sphincter anal fistula. Dis Colon Rectum 1984;27:109–10.
Mann CV, Clifton MA. Re-routing of the track for the treatment of high anal and anorectal fistulas. Br J Surg 1985;72:139–71.
Kupferberg A, Zer M, Rabinson S. The use of PMMA beads in recurrent high anal fistula: a preliminary report. World J Surg 1989;8:970–9.
Parks AG. Pathogenesis and treatment of fistula-in-ano. BMJ 1961;1:463–9.
Khubchandani M. Comparison of results of treatment of fistula-in-ano. J R Soc Med 1989;77:369–71.
Elting AW. The treatment of fistula-in-ano. Ann Surg 1912;56:779–82.
Gallagher DM, Scarborough RA. Repair of low rectovaginal fistula. Dis Colon Rectum 1962;5:193–5.
Aguilar PS, Plasencia G, Hardy TG Jr, Hartmann RF, Stewart RC. Mucosal advancement in the treatment of anal fistula. Dis Colon Rectum 1985;28:496–8.
Kodner IJ, Mazor A, Shemesh EI. Endorectal advancement flap repair of rectovaginal and other complicated anorectal fistulas. Surgery 1993;114:682–9.
Fazio VW. Complex anal fistula. Gastroenterol Clin North Am 1987;16:93–114.
Stone JM, Goldberg SM. The endorectal advancement flap procedure. Int J Colorectal Dis 1990;5:232–5.
Farkas AM, Gingold BS. Repair of rectovaginal fistula in Crohn's disease by rectal mucosal advancement flap. Mt Sinai J Med 1983;50:420–3.
Radcliffe AG, Ritchie JK, Hawley PR, Lennard-Jones JE, Northover JM. Anovaginal and rectovaginal fistulas in Crohn's disease. Dis Colon Rectum 1988;31:94–9.
Morrison JG, Gathright JB Jr, Ray JF, Ferrari BT, Hicks TC, Timmcke AE. Results of operation for rectovaginal fistula in Crohn's disease. Dis Colon Rectum 1989;32:497–9.
Jones IT, Fazio VW, Jagelman DG. The use of transanal rectal advancement flaps in the management of fistulas involving the anorectum. Dis Colon Rectum 1987;30:919–23.
Rothenberger DA, Christenson CE, Balcos EG,et al. Endorectal advancement flap for treatment of simple rectovaginal fistulas. Dis Colon Rectum 1982;25:297–300.
Hilsabeck JR. Transanal advancement of the anterior rectal wall for vaginal fistulas involving the lower rectum. Dis Colon Rectum 1980;123:236–41.
Noble GH. A new operation for complete laceration of the perineum designed for the purpose of eliminating danger of infection from the rectum. Trans Am Gynecol Soc 1902;27:357–63.
Oh C. Management of high recurrent anal fistula. Surgery 1983;93:330–2.
Mengert WF, Fish SA. Anterior rectal wall advancement technique for repair of complete perineal laceration and rectovaginal fistula. Obstet Gynecol 1955;5:262–7.
Fazio VW, Jones IT, Jagelman DG, Weakley FL. Rectourethral fistulas in Crohn's disease. Surg Gynecol Obstet 1987;169:148–50.
Laird DR. Procedures used in treatment of complicated fistulas. Am J Surg 1948;76:701–8.
Jackman RJ. Rectovaginal and anovaginal fistulas: a surgical procedure for treatment of certain types. J Iowa M Soc 1952;42:435–40.
Parks AG, Motson RW. Perianal repair of rectoprostatic fistula. Br J Surg 1983;70:725–6.
Greenwald JC, Hoexter B. Repair of rectovaginal fistula. Surg Gynecol Obstet 1978;146:443–5.
Buchmann P, Keighley MR, Allan RN, Thompson H, Alexander-Williams J. Natural history of perianal Crohn's disease. Am J Surg 1980;190:642–4.
Lowry AC, Thorson AG, Rothenberger DA, Goldberg SM. Repair of simple rectovaginal fistulas: influence of previous repairs. Dis Colon Rectum 1988;31:676–8.
Author information
Authors and Affiliations
Additional information
Read at the meeting of The American Society of Colon and Rectal Surgeons, Montreal, Quebec, Canada, May 7 to 12, 1995.
About this article
Cite this article
Ozuner, G., Hull, T.L., Cartmill, J. et al. Long-term analysis of the use of transanal rectal advancement flaps for complicated anorectal/vaginal fistulas. Dis Colon Rectum 39, 10–14 (1996). https://doi.org/10.1007/BF02048261
Issue Date:
DOI: https://doi.org/10.1007/BF02048261