Abstract
Objective
To evaluate the effect of tracheal gas insufflation (TGI) in spontaneously breathing, intubated patients with chronic obstructive pulmonary disease (COPD) undergoing weaning from the mechanical ventilation.
Design
A prospective study in humans.
Setting
Polyvalent intensive care unit (14-bed ICU) in a 700-bed general university hospital.
Patients
Twelve patients with chronic obstructive pulmonary disease (COPD) who required intubation and mechanical ventilation were studied. All patients met standard criteria for weaning from mechanical ventilation. Seven patients (group 1) had been transorally intubated during episodes of acute respiratory failure. Five patients, all men (group 2), had previously undergone tracheostomy and had a transtracheal tube in place.
Interventions
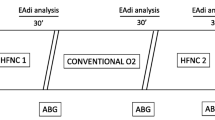
Intratracheal, humidified, O2-mixture insufflation (TGI) was given via a catheter placed in distal or proximal position. Gas delivered through the intratracheal catheter was blended to match the fractional of inspired gas through the endotracheal tube. Continuous flows of 3 and 6 l/min in randomized order were used in each catheter position. Prior to data collection at each stage, an equilibration period of at least 30 min was observed, and thereafter blood gases were analyzed every 5 min. A new steady state was assumed to have been established when values of bothP aCO2 and\(\dot V\) CO2 changed by less than 5% between adjacent measurements. The last values of blood gases were taken as representative. The new steady state was confirmed within 35–50 min. Baseline measurements with zero\(\dot V_{cath} \) were made at the beginning and end of the experiment.
Results
This study shows that VT, MV,P aCO2, and VD/VT are reduced in a flow-dependent manner when gas is delivered through an oral-tracheal tube (group 1). The distal catheter position was more effective than the proximal one. In contrast, when gas was delivered through tracheostomy (group 2), TGI was ineffective in the proximal position and less effective than in group 1 in distal position.
Conclusion
Under the experimental conditions, tracheal gas insufflation decreased dead space, increased alveolar ventilation and possibly reduced work of breathing. From the preliminary data reported here, we believe that TGI may help patients experiencing difficulty during weaning.
Article PDF
Similar content being viewed by others
References
Heffner J, Miller K, Sahn S (1986) Tracheostomy in the intensive care unit. I. Indications, technique, management. Chest 90: 169
Heffner J (1989) Medical indications for tracheostomy. Chest 96: 186
Heimlich H (1982) Respiratory rehabilitation with a transtracheal oxygen system. Ann Otol Rhinol Laryngol 91: 643–647
Heimlich H, Carr G (1985) Transtracheal catheter technique for pulmonary rehabilitation. Ann Otol Rhinol Laryngol 94: 502–504
Hoffman L, Dauber J, Ferson P, Openbrier D, Zullo T (1987) Patients' response to transtracheal oxygen delivery. Am Rev Respir Dis 135: 153–156
Wesmiller S, Hoffman L, Bauber J, Ferson P, Johnson J, Donaheo M (1988) Twelve-minute walk distance during nasal cannula and transtracheal oxygen delivery. Am Rev Respir Dis A 137: 156
Christopher K, Spofford B, Petrun M, McCarty D, Goodman J, Petty T (1987) A program for transtracheal oxygen delivery. Ann Intern Med 107: 802–808
Couser J, Make B (1989) Transtracheal oxygen decreases inspired minute ventilation. An Rev Respir Dis 139: 627–631
Scott G, Hinson J, Scott R, Quigley P, Christopher K, Metzler M (1993) The effects of transtracheal gas delivery on central inspiratory neuromuscular drive. Chest 104: 1199–1202
Ravenscraft S, Burke C, Nahum A, Adams A, Nakos G, Marcy T, Marini J (1993) Tracheal gas insufflation augments CO2 clearance during mechanical ventilation. Am Rev Respir Dis 148: 345–351
Burke C, Nahum A, Ravenscraft S, Nakos G, Adams A, Marcy T, Marini J (1983) Modes of tracheal gas insufflation: comparison of continuous and phase-specific gas injection in normal dogs. Am Rev Respid Dis 148: 562–568
Nahum A, Ravenscraft S, Nakos G, Burke W, Adams A, Marcy T, Marini J (1992) Tracheal gas insufflation during pressure-control ventilation: effect of catheter position, diameter and flow rate. Am Rev Respir Dis 146: 1411–1418
Sahn S, Lakshminarayan Y (1973) Bedside criteria for discontinuation of mechanical ventilation. Chest 63: 1002–1005
American Thoracic Society (1987) Standards for diagnosis and care of patients with chronic obstructive disease and asthma. Am Rev Respir Dis 136: 225–244
Sznajder JI, Becker CJ, Crawford GP, Wood LDH (1989) Combination of constant-flow and continuous positive-pressure ventilation in canine pulmonary edema. J Appl Physiol 67: 817–832
Bye P, Esau S, Levy R et al (1985) Ventilatory muscle function during exercise in air and oxygen in patients with chronic air-flow limitation. Am Rev Respir Dis 132: 236–240
Nunn J (1988) Control of breathing. In: Nunn J (ed) Applied respiratory physiology. Butterworths, London, pp 72–99
Coleridge H, Coleridge J (1985) Reflexes evoked from tracheobronchial tree and lungs. In: Cherniak N, Widdicombe J (ed) Handbook of physiology. The respiratory system. Control of breathing. American Physiology Society, Bethesda, Md., pp 395–429
Cullen J (1983) An evaluation of tracheostomy in pulmonary emphysema. Ann Intern Med 58: 953–960
Bergofsky E, Hurewitz A (1989) Airway insufflation: physiologic effects on acute and chronic gas exchange in humans. Am Rev Respir Dis 140: 885–890
Hurewitz A, Bergofsky E, Vomero E (1991) Air insufflation: increased flow rates progressively reduce dead space in respiratory failure. Am Rev Respir Dis 144: 1229–1233
Nakos G, Zakinthinos S, Kotanidou A, Tsagaris H, Roussos C (1994) Tracheal gas insufflation reduces the tidal volume while PaCO2 is maintained constant. Intensive Care Med 20: 407–413
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Nakos, G., Lachana, A., Prekates, A. et al. Respiratory effects of tracheal gas insufflation in spontaneously breathing COPD patients. Intensive Care Med 21, 904–912 (1995). https://doi.org/10.1007/BF01712331
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF01712331