Abstract
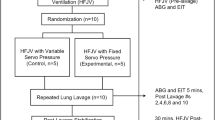
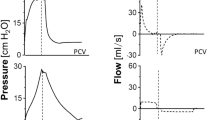
In 19 anesthetized piglets 3 ventilatory modes were studied after inducing pulmonary insufficiency by bronchoalveolar lavage by the method of Lachmann. The lavage model was considered suitable for reproduction of severe respiratory distress. This model was reproducible and stable with respect to alveolar collapse, decrease in static chest-lung compliance and increase in extravascular lung water. The ventilatory modes studied were volume-controlled intermittent positive-pressure ventilation (IPPV), pressure-controlled inverse ratio ventilation (IRV), and pressure-controlled high-frequency positive-pressure ventilation (HFPPV). The 3 ventilatory modes were used in random sequence for at least 30 min to produce a ventilatory steady state. Ventilation with no PEEP, permitting alveolar collapse, was interposed between each experimental mode. The ability to open collapsed alveoli, i.e. alveolar recruitment, was different. The recruitment rate for IPPV was 74%, but for IRV and HFPPV it was 95%, respectively. Although IRV provided the best PaO2, this was at the expense of high airway pressures with circulatory interference and reduced oxygen transport. In contrast to this, HFPPV provided lower airway pressures, less circulatory interference and improved oxygen transport. In the clinical setting there might be negative effects on vital organs and functions unless the ventilatory modes are continuously and cautiously adapted to the individual requirements in different phases of severe respiratory distress. Therefore, one ventilatory strategy could be to “open the airways” with IRV, but then switch to HFPPV in an attempt to maintain the airways open with lesser risk of barotrauma and with improved oxygen transport.
Article PDF
Similar content being viewed by others
References
Matthay MA (1989) New modes of mechanical ventilation for ARDS — how should they be evaluated? Chest 95:1175–1177
Lachmann B, Danzmann E, Haendly B, Jonson B (1982) Ventilator settings and gas exchange in respiratory distress syndrome. In: Prakash O (ed) Applied physiology in clinical respiratory care. Nijhoff, The Hague, pp 141–176
Albert RK (1985) Least PEEP: primum non nocere. Chest 87:2–4
Reynolds EOR (1971) Effect of alterations in mechanical ventilator setting on pulmonary gas exchange in hyaline membrane disease. Arch Dis Child 46:152–159
Sjöstrand U (1980) High-frequency positive-pressure ventilation (HFPPV): a review. Crit Care Med 8:345–364
Sjöstrand UH (1989) In what respect does high frequency positive pressure ventilation differ from conventional ventilation? Acta Anaesthesiol Scand 33 [Suppl 90]:5–12
Jonzon A, Öberg PÅ, Sedin G, Sjöstrand U (1971) High-frequency positive-pressure ventilation by endotracheal insufflation. Acta Anaesthesiol Scand 15 [Suppl 43]:1–43
Lachmann B, Robertson B, Vogel J (1980) In vivo lung lavage as an experimental model of the respiratory distress syndrome. Acta Anaesthesiol Scand 24:231–236
Lachmann B, Jonson B, Lindroth M, Robertson B (1982) Modes of artificial ventilation in severe distress syndrome. Lung function and morphology in rabbits after wash-out of alveolar surfactant. Crit Care Med 10:724–732
Menkes H, Traystman R, Terry P (1979) Collateral ventilation. Fed Proc 38:22–26
Kuriyama T, Latham LP, Horwitz LD, Reeves JT, Wagner WW Jr (1984) Role of collateral ventilation in ventilation-perfusion balance. J Appl Physiol 56:1500–1506
Sjöstrand UH, Edgren E, Nielsen JB (1990) Pressure-controlled HFPPV with PEEP in the pig — An efficient mode of ventilation in severe respiratory distress. In: Aochi O, Amaha K, Takeshita H (eds) Intensive and critical care medicine. Excerpta Medica International Congress Series 885, pp 766–768
Sjöstrand UH (1989) High frequency positive pressure ventilation. In: Branson RD, Hurst JM, Davis K Jr (eds) Alternative modes of ventilatory support. Probl Respir Care 2:1–15
Sjöstrand U (1977) Review of the physiological rationale for an development of high-frequency positive-pressure ventilation — HFPPV. Acta Anaesthesiol Scand 21 [Suppl 64]:7–27
Pfeiffer UJ, Aschenbrenner G, Kolb E, Blümel G, Pfeiffer HG (1986) Die Messung des intrathoracalen Volumens als sensitiver Parameter zur Steuerung der Volumensubstitution. Chir Forum 86:203–207
Neumann R, Worek FS, Blümel G, Zimmerann GJ, Fehm HL, Pfeiffer UJ (1989) Cortisol deficiency in etomidate anesthetized bacteremic pigs: results in circulatory failure — beneficial effects of cortisol substitution. Acta Anaesthesiol Scand 33:379–384
Worek FS, Blümel G, Zeravik J, Zimmermann GJ, Pfeiffer UJ (1988) Comparison of ketamine and pentobarbital anesthesia with the conscious state in a porcine model ofPseudomonas aeruginosa septicemia. Acta Anaesthesiol Scand 32:509–515
Lewis FR, Elings VB (1978) Microprocessor determination of lung water using thermal-green dye double indicator dilution. Surg Forum 29:182–184
Newmann EV, Merell MM, Genecin A (1951) The dye dilution method for describing the central circulation. An analysis of factors shaping the time-concentration curves. Circulation 4:735–746
Lewis FR, Elings VB, Hill SL et al (1982) The measurement of extravascular lung water by thermal-green dye indicator dilution. Ann NY Acad Sci 384:394–410
Peiffer U, Birk M, Aschenbrenner H, Blümel G (1982) The system for quantitating thermal-dye extravascular lung water. In: Prakash O (ed) Computers in critical care and pulmenary medicine. Vol 2. Plenum Publishing Corporation, London, pp 123–125
Pfeiffer U, Zimmermann G (1984) Fehlermoglichkeiten und Grenzen der Lungenwasserbestimmung mit der Thermo-Dye-Technik. Anaesthesiol Intensivmed 6:81–104
Wickerts CJ, Jakobsson J, Frostell C, Hedenstierna G (1990) Measurement of extravascular lung water by thermal-dye dilution technique: mechanisms of cardiac output dependence. Intensive Care Med 16:115–120
Fuhrman BP, Smith-Wright DL, Venkataram S, Orr RA, Howland DF (1989) Proximal mean airway pressure: a good estimator of mean alveolar pressure during continuous positive-pressure breathing. Crit Care Med 17:666–670
Svensson BA, Westman J, Rastad J (1985) Light and electron microscopic study of neurons in the feline lateral cervical nucleus with a descending projection. Brain Res 361:114–124
Gattinoni L, Pesenti A, Mascheroni D, Marcolin R, Fumagalli R, Rossi F, Iapichino G, Romagnoli G, Uziel L, Agostoni A (1986) Low frequency positive-pressure ventilation with extracorporeal CO2 removal in severe acute respiratory failure. JAMA 256: 881–886
Kirby RR, Downs JB, Civetta JM, Modell JH, Dannemiller FJ, Klein EF, Hodges M (1975) High level positive end-expiratory pressure (PEEP) in acute respiratory insufficiency. Chest 67:156–163
Nelson LD, Civetta JM, Hudson-Civetta J (1987) Titrating positive end-expiratory pressure in patients with early moderate arterial hypoxemia. Crit Care Med 15:14–19
Brigham KL, Woolverton WC, Blake LH, Staub NC (1974) Increased sheep lung vascular permeability caused by pseudomonas bacteremia. J Clin Invest 54:792–804
Brown PP, Coalson JJ, Elkins RC, Hinshaw LB, Greenfield LJ (1973) Hemodynamic and respiratory responses of conscious swine toE. coli endotoxin. Surg Forum 24:67–68
Dehring DJ, Crocker SH, Wismar BL, Steinberg SM, Lowery BD, Cloutier CT (1983) Comparison of live bacteria infusion in a porcine model of acute respiratory failure. J Surg Res 34:151–158
Borg T, Modig J (1987) Intermittent and continuous positive-pressure ventilation in the prophylaxis of endotoxin-induced lung insufficiency. A study in pigs. Acta Anaesthesiol Scand 31:67–72
Borg T, Alvfors A, Gerdin B, Modig J (1985) A porcine model of early adulty respiratory distress syndrome induced by endotoxinaemia. Acta Anaesthesiol Scand 29:814–830
Hickling KG (1990) Ventilatory management of ARDS: can it affect outcome? Intensive Care Med 16:219–226
Hickling KG, Henderson SJ, Jackson R (1990) Low mortality associated with low volume pressure limited ventilation with permissive hypercapnia in severe adult respiratory distress syndrome. Intensive Care Med 16:372–377
Author information
Authors and Affiliations
Additional information
This study was supported by the Swedish Medical Research Council (projects 4252 and 2710), Sweden
Rights and permissions
About this article
Cite this article
Nielsen, J.B., Sjöstrand, U.H., Edgren, E.L. et al. An experimental study of different ventilatory modes in piglets in severe respiratory distress induced by surfactant depletion. Intensive Care Med 17, 225–233 (1991). https://doi.org/10.1007/BF01709882
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF01709882