Abstract
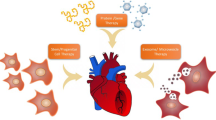
Noninvasive injection of pro-angiogenic compounds such as vascular endothelial growth factor (VEGF) has shown promising results in regenerating cardiac microvasculature. However, these results have failed to translate into successful clinical trials in part due to the short half-life of VEGF in circulation. Increasing the dose of VEGF may increase its availability to the target tissue, but harmful side-effects remain a concern. Encapsulating and selectively targeting VEGF to the MI border zone may circumvent these problems. Anti-P-selectin conjugated immunoliposomes containing VEGF were developed to target the infarct border zone in a rat MI model. Targeted VEGF therapy significantly improves vascularization and cardiac function after an infarction.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Scott RC, Wang B, Nallamothu R et al (2007) Targeted delivery of antibody conjugated liposomal drug carriers to rat myocardial infarction. Biotechnol Bioeng 96:795–802
Misao Y, Takemura G, Arai M et al (2006) Importance of recruitment of bone marrow-derived CXCR4+ cells in post-infarct cardiac repair mediated by G-CSF. Cardiovasc Res 71:455–465
Scott RC, Crabbe D, Krynska B et al (2008) Aiming for the heart: targeted delivery of drugs to diseased cardiac tissue. Expert Opin Drug Deliv 5:459–470
Wang B, Ansari R, Sun Y et al (2005) The scar neovasculature after myocardial infarction in rats. Am J Physiol Heart Circ Physiol 289:H108–H113
Sun Y, Weber KT (1996) Angiotensin converting enzyme and myofibroblasts during tissue repair in the rat heart. J Mol Cell Cardiol 28:851–858
Scott RC, Rosano JM, Ivanov Z et al (2009) Targeting VEGF-encapsulated immunoliposomes to MI heart improves vascularity and cardiac function. FASEB J 23:3361–3367
Pattillo CB, Sari-Sarraf F, Nallamothu R et al (2005) Targeting of the antivascular drug combretastatin to irradiated tumors results in tumor growth delay. Pharm Res 22:1117–1120
Burch EE, Shinde PV, Camphausen RT et al (2002) The N-terminal peptide of PSGL-1 can mediate adhesion to trauma-activated endothelium via P-selectin in vivo. Blood 100:531–538
Wang B, Scott RC, Pattillo CB et al (2007) Microvascular transport model predicts oxygenation changes in the infarcted heart after treatment. Am J Physiol Heart Circ Physiol 293:H3732–H3739
Wang B, Scott RC, Pattillo CB et al (2008) Modeling oxygenation and selective delivery of drug carriers post-myocardial infarction. Adv Exp Med Biol 614:333–343
Lopez JJ, Laham RJ, Stamler A et al (1998) VEGF administration in chronic myocardial ischemia in pigs. Cardiovasc Res 40:272–281
Freedman SB, Isner JM (2001) Therapeutic angiogenesis for ischemic cardiovascular disease. J Mol Cell Cardiol 33:379–393
Rudge JS, Holash J, Hylton D et al (2007) VEGF Trap complex formation measures production rates of VEGF, providing a biomarker for predicting efficacious angiogenic blockade. Proc Natl Acad Sci U S A 104:18363–18370
Acknowledgments
This work was supported by grants from The American Heart Association, and The National Heart, Lung and Blood Institute. The human VEGF165A was generously provided by Genentech, Inc., San Francisco, CA.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2013 Springer Science+Business Media New York
About this paper
Cite this paper
Wang, B., Cheheltani, R., Rosano, J., Crabbe, D.L., Kiani, M.F. (2013). Targeted Delivery of VEGF to Treat Myocardial Infarction. In: Welch, W.J., Palm, F., Bruley, D.F., Harrison, D.K. (eds) Oxygen Transport to Tissue XXXIV. Advances in Experimental Medicine and Biology, vol 765. Springer, New York, NY. https://doi.org/10.1007/978-1-4614-4989-8_43
Download citation
DOI: https://doi.org/10.1007/978-1-4614-4989-8_43
Published:
Publisher Name: Springer, New York, NY
Print ISBN: 978-1-4614-4771-9
Online ISBN: 978-1-4614-4989-8
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)