Abstract
Background
Abnormal activation of the coagulation system is associated with malignant tumor progression. Although neoadjuvant treatment (NAT) for resectable esophageal squamous cell carcinoma (ESCC) is the standard of care, the correlation between coagulation status and prognosis of patients undergoing preoperative treatment is insufficiently understood.
Methods
Patients (n = 200) who underwent radical subtotal esophagectomy after preoperative treatment for ESCC between January 2012 and December 2021were included in the analysis. Plasma D-dimer and fibrinogen levels and their combined indices (non-hypercoagulation; D-dimer and fibrinogen levels within the upper normal limit, or hypercoagulation; D-dimer or fibrinogen levels above the upper normal limit) were determined before and after NAT and correlated to clinicopathological factors and prognosis.
Results
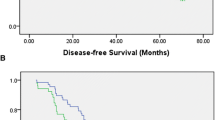
The nonhypercoagulation group achieved superior overall survival (OS) than the hypercoagulation group (5-year OS rates = 89% vs. 55%; hazard ratio 3.62, P = 0.0008) when determined according to coagulation status after NAT. Multivariate analysis showed that hypercoagulation after NAT served as an independent factor for poor postoperative OS (hazard ratio 3.20; P = 0.0028). The nonhypercoagulation group achieved significantly better disease-free survival (76% vs. 54%; P = 0.0065) than the hypercoagulation group that experienced a significantly higher rate of hematogenous metastasis as an initial recurrence (P = 0.0337).
Conclusions
Hypercoagulation state after NAT served as a valid indicator correlating with postoperative outcomes of patients with ESCC who underwent NAT followed by radical subtotal esophagectomy.



Similar content being viewed by others
References
Ando N, Kato H, Igaki H, et al. A randomized trial comparing postoperative adjuvant chemotherapy with cisplatin and 5-fluorouracil versus preoperative chemotherapy for localized advanced squamous cell carcinoma of the thoracic esophagus (JCOG9907). Ann Surg Oncol. 2012;19(1):68–74.
Watanabe M, Toh Y, Ishihara R, et al. Comprehensive registry of esophageal cancer in Japan, 2015. Esophagus. 2023;20(1):1–28.
Kanda M, Koike M, Shimizu D, et al. Characteristics associated with nodal and distant recurrence after radical esophagectomy for squamous cell carcinoma of the thoracic esophagus. Ann Surg Oncol. 2020;27(9):3195–205.
Zhang D, Zhou X, Bao W, et al. Plasma fibrinogen levels are correlated with postoperative distant metastasis and prognosis in esophageal squamous cell carcinoma. Oncotarget. 2015;6(35):38410–20.
Diao D, Zhu K, Wang Z, et al. Prognostic value of the D-dimer test in oesophageal cancer during the perioperative period. J Surg Oncol. 2013;108(1):34–41.
Zhang Han-Ze, Jin Guang-Fu, Shen Hong-Bing. Epidemiologic differences in esophageal cancer between Asian and Western populations. Chin J Cancer. 2012;31(6):281–6.
Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2018;68(6):394–424.
Uhlenhopp DJ, Then EO, Sunkara T, Gaduputi V. Epidemiology of esophageal cancer: update in global trends, etiology and risk factors. Clin J Gastroenterol. 2020;13(6):1010–21.
Matz M, Valkov M, Sekerija M, et al. Worldwide trends in esophageal cancer survival, by sub-site, morphology, and sex: an analysis of 696,974 adults diagnosed in 60 countries during 2000–2014(CONCORD-3). Cancer Commun (Lond). 2023;43(9):963–80.
Weiss JA, Jain S. Neoadjuvant and adjuvant therapy in esophageal cancer. J Gastrointest Oncol. 2023;14(4):1927–32.
Falanga A, Marchetti M, Vignoli A. Coagulation and cancer: biological and clinical aspects. J Thromb Haemost. 2013;11(2):223–33.
Yang Y, Xu H, Zhou L, et al. Platelet to lymphocyte ratio is a predictive marker of prognosis and therapeutic effect of postoperative chemotherapy in non-metastatic esophageal squamous cell carcinoma. Clin Chim Acta. 2018;479:160–5.
Kato T, Oshikiri T, Goto H, et al. Impact of the platelet-to-lymphocyte ratio as a biomarker for esophageal squamous cell carcinoma. Anticancer Res. 2022;42(5):2775–82.
Li J, Zheng Z, Fang M. Impact of pretreatment plasma D-dimer levels and its perioperative change on prognosis in operable esophageal squamous cell carcinoma. Oncotarget. 2017;8(45):79537–45.
Ma M, Cao R, Wang W, et al. The D-dimer level predicts the prognosis in patients with lung cancer: a systematic review and meta-analysis. J Cardiothorac Surg. 2021;16(1):243.
Zhao LY, Zhao YL, Wang JJ, et al. Is preoperative fibrinogen associated with the survival prognosis of gastric cancer patients? A multi-centered, propensity score-matched retrospective study. World J Surg. 2020;44(1):213–22.
Matsuda S, Takeuchi H, Fukuda K, et al. Clinical significance of plasma fibrinogen level as a predictive marker for postoperative recurrence of esophageal squamous cell carcinoma in patients receiving neoadjuvant treatment. Dis Esophagus. 2014;27(7):654–61.
Liu DQ, Li FF, Jia WH. Cumulative scores based on plasma D-dimer and serum albumin levels predict survival in esophageal squamous cell carcinoma patients treated with transthoracic esophagectomy. Chin J Cancer. 2016;35:11.
Zhang F, Chen Z, Wang P, et al. Combination of platelet count and mean platelet volume (COP-MPV) predicts postoperative prognosis in both resectable early and advanced stage esophageal squamous cell cancer patients. Tumour Biol. 2016;37(7):9323–31.
Feng JF, Huang Y, Chen QX. Preoperative platelet lymphocyte ratio (PLR) is superior to neutrophil lymphocyte ratio (NLR) as a predictive factor in patients with esophageal squamous cell carcinoma. World J Surg Oncol. 2014;12:58.
Zhang D, Zheng Y, Wang Z, et al. Comparison of the 7th and proposed 8th editions of the AJCC/UICC TNM staging system for esophageal squamous cell carcinoma underwent radical surgery. Eur J Surg Oncol. 2017;43(10):1949–55.
Kanda M, Koike M, Iwata N, et al. An open-label single-arm phase II study of treatment with neoadjuvant S-1 plus cisplatin for clinical stage III squamous cell carcinoma of the esophagus. Oncologist. 2020;25(11):e1650–4.
Nakamura K, Kato K, Igaki H, et al. Three-arm phase III trial comparing cisplatin plus 5-FU (CF) versus docetaxel, cisplatin plus 5-FU (DCF) versus radiotherapy with CF (CF-RT) as preoperative therapy for locally advanced esophageal cancer (JCOG1109, NExT study). Jpn J Clin Oncol. 2013;43(7):752–5.
Ken K, Kei M, Nobutoshi A, et al. A phase II study of nedaplatin and 5-fluorouracil in metastatic squamous cell carcinoma of the esophagus: The Japan Clinical Oncology Group (JCOG) Trial (JCOG 9905-DI). Esophagus. 2014;11(3):183–8.
Miyata H, Sugimura K, Motoori M, et al. Clinical Implications of Conversion Surgery After Induction Therapy for T4b Thoracic Esophageal Squamous Cell Carcinoma. Ann Surg Oncol. 2019;26(13):4737–43.
Kanda M, Shimizu D, Sawaki K, et al. Therapeutic monoclonal antibody targeting of neuronal pentraxin receptor to control metastasis in gastric cancer. Mol Cancer. 2020;19(1):131.
Kanda M, Kasahara Y, Shimizu D, et al. Amido-bridged nucleic acid-modified antisense oligonucleotides targeting SYT13 to treat peritoneal metastasis of gastric cancer. Mol Ther Nucleic Acids. 2020;22:791–802.
Licciardello JT, Moake JL, Rudy CK, Karp DD, Hong WK. Elevated plasma von Willebrand factor levels and arterial occlusive complications associated with cisplatin-based chemotherapy. Oncology. 1985;42(5):296–300.
Fernandes CJ, Morinaga LTK, Alves JLJ, et al. Cancer-associated thrombosis: the when, how and why. Eur Respir Rev. 2019; 28(151).
Varki A. Trousseau’s syndrome: multiple definitions and multiple mechanisms. Blood. 2007;110(6):1723–9.
Mukai M, Oka T. Mechanism and management of cancer-associated thrombosis. J Cardiol. 2018;72(2):89–93.
Liu P, Zhu Y, Liu L. Elevated pretreatment plasma D-dimer levels and platelet counts predict poor prognosis in pancreatic adenocarcinoma. Oncol Targets Ther. 2015;8:1335–40.
Palumbo JS, Talmage KE, Massari JV, et al. Platelets and fibrin(ogen) increase metastatic potential by impeding natural killer cell-mediated elimination of tumor cells. Blood. 2005;105(1):178–85.
Gay LJ, Felding-Habermann B. Contribution of platelets to tumour metastasis. Nat Rev Cancer. 2011;11(2):123–34.
Kelly RJ, Ajani JA, Kuzdzal J, et al. Adjuvant Nivolumab in Resected Esophageal or Gastroesophageal Junction Cancer. N Engl J Med. 2021;384(13):1191–203.
Rothwell PM, Wilson M, Price JF, Belch JF, Meade TW, Mehta Z. Effect of daily aspirin on risk of cancer metastasis: a study of incident cancers during randomized controlled trials. Lancet. 2012;379(9826):1591–601.
Mahmud S, Franco E, Aprikian A. Prostate cancer and use of nonsteroidal anti-inflammatory drugs: systematic review and meta-analysis. Br J Cancer. 2004;90(1):93–9.
Khuder SA, Mutgi AB. Breast cancer and NSAID use: a meta-analysis. Br J Cancer. 2001;84(9):1188–92.
Jiang Y, Su Z, Li C, et al. Association between the use of aspirin and risk of lung cancer: results from pooled cohorts and Mendelian randomization analyses. J Cancer Res Clin Oncol. 2021;147(1):139–51.
Corley DA, Kerlikowske K, Verma R, Buffler P. Protective association of aspirin/NSAIDs and esophageal cancer: a systematic review and meta-analysis. Gastroenterology. 2003;124(1):47–56.
Thun MJ. Beyond willow bark: aspirin in the prevention of chronic disease. Epidemiology. 2000;11(4):371–4.
Liu JF, Jamieson GG, Wu TC, Zhu GJ, Drew PA. A preliminary study on the postoperative survival of patients given aspirin after resection for squamous cell carcinoma of the esophagus or adenocarcinoma of the cardia. Ann Surg Oncol. 2009;16(5):1397–402.
Coyle C, Cafferty FH, Rowley S, et al. ADD-ASPIRIN: A phase III, double blind, placebo controlled, randomised trial assessing the effects of aspirin on disease recurrence and survival after primary therapy in common non-metastatic solid tumours. Contemp Clin Trials. 2016;51:56–64.
van Hagen P, Hulshof MCCM, van Lanschot JJB, et al. Preoperative chemoradiotherapy for esophageal or junctional cancer. 2012;366(22):2074–84.
Acknowledgments
The authors thank Edanz (https://jp.edanz.com/ac) for editing a draft of this manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosure
The authors declare that they have no competing interests. No financial support was received.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sugiyama, F., Kanda, M., Shimizu, D. et al. Absence of Hypercoagulation Status after Neoadjuvant Treatment is Associated with Favorable Prognosis in Patients Undergoing Subtotal Esophagectomy for Esophageal Squamous Cell Carcinoma. Ann Surg Oncol 31, 3417–3425 (2024). https://doi.org/10.1245/s10434-024-14938-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-024-14938-1