Key summary points
Investigate the relationship between cognitive function and phase angle, a measure of muscle quality.
AbstractSection FindingsPhase angle consistently decreased with worsening general cognition in individuals with Alzheimer's dementia or amnesic mild cognitive impairment in men.
AbstractSection MessageOur study strengthened the findings of the very few previous studies indicating that low muscle quality is associated with poor cognitive function.
Abstract
Purpose
The purpose of this study was to investigate the relationship between cognitive function and phase angle (PhA), an indicator of muscle quality.
Methods
This cross-sectional study enrolled outpatients who visited a memory clinic at the Nagoya University hospital from January 2016 to June 2022. We enrolled 153 participants with body composition measurements. Inclusion criteria were a Mini-Mental State Examination score of 20–30 and a clinical diagnosis of Alzheimer’s dementia (AD) or amnesic mild cognitive impairment (aMCI). The background characteristics of the participants were compared according to AD and aMCI. Next, linear regression analysis was performed with PhA as the objective variable. In addition, logistic regression analysis was performed for AD diagnosis.
Results
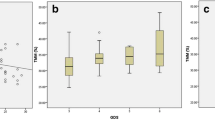
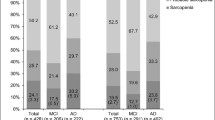
PhA was lower in the AD group (P = 0.009). In linear regression analysis, PhA consistently decreased with worsening ADAS score. In logistic regression analysis, high PhA was associated with absence of AD. Gender-specific analyses showed these associations existed only in men.
Conclusions
Our study of patients with AD and aMCI found that PhA decreased with worsening of cognitive function. Compared with aMCI, AD was associated with significantly lower PhA. Our results strengthen the limited evidence in the literature showing that low muscle quality is associated with poor cognitive function.

Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Delmonico MJ et al (2009) Longitudinal study of muscle strength, quality, and adipose tissue infiltration. Am J Clin Nutr 90(6):1579–1585
Cesari M et al (2009) Skeletal muscle and mortality results from the InCHIANTI study. J Gerontol A Biol Sci Med Sci 64(3):377–384
Newman AB et al (2006) Strength, but not muscle mass, is associated with mortality in the health, aging and body composition study cohort. J Gerontol A Biol Sci Med Sci 61(1):72–77
Avesani CM et al (2023) Muscle fat infiltration in chronic kidney disease: a marker related to muscle quality, muscle strength and sarcopenia. J Nephrol 36(3):895–910
Lim JY, Frontera WR (2022) Single skeletal muscle fiber mechanical properties: a muscle quality biomarker of human aging. Eur J Appl Physiol 122(6):1383–1395
Yamada M et al (2017) Differential characteristics of skeletal muscle in community-dwelling older adults. J Am Med Dir Assoc 18(9):807.e9-807.e16
Sergi G et al (2016) Imaging of sarcopenia. Eur J Radiol 85(8):1519–1524
Mirón Mombiela R et al (2020) Ultrasound biomarkers for sarcopenia: what can we tell so far? Semin Musculoskelet Radiol 24(2):181–193
Norman K et al (2012) Bioelectrical phase angle and impedance vector analysis–clinical relevance and applicability of impedance parameters. Clin Nutr 31(6):854–861
Bosy-Westphal A et al (2006) Phase angle from bioelectrical impedance analysis: population reference values by age, sex, and body mass index. JPEN J Parenter Enteral Nutr 30(4):309–316
Akamatsu Y et al (2022) Phase angle from bioelectrical impedance analysis is a useful indicator of muscle quality. J Cachexia Sarcopenia Muscle 13(1):180–189
Barbosa-Silva MC et al (2005) Bioelectrical impedance analysis: population reference values for phase angle by age and sex. Am J Clin Nutr 82(1):49–52
Uemura K et al (2020) Predictivity of bioimpedance phase angle for incident disability in older adults. J Cachexia Sarcopenia Muscle 11(1):46–54
Di Vincenzo O et al (2021) Bioelectrical impedance analysis (BIA) -derived phase angle in sarcopenia: a systematic review. Clin Nutr 40(5):3052–3061
Lukaski HC, Kyle UG, Kondrup J (2017) Assessment of adult malnutrition and prognosis with bioelectrical impedance analysis: phase angle and impedance ratio. Curr Opin Clin Nutr Metab Care 20(5):330–339
Fujisawa C et al (2017) Physical function differences between the stages from normal cognition to moderate Alzheimer disease. J Am Med Dir Assoc 18(4):368.e9-368.e15
Sui SX et al (2020) Skeletal muscle health and cognitive function: a narrative review. Int J Mol Sci. https://doi.org/10.3390/ijms22010255
van Dam R et al (2018) Lower cognitive function in older patients with lower muscle strength and muscle mass. Dement Geriatr Cogn Disord 45(3–4):243–250
Buchman AS et al (2013) Association of brain pathology with the progression of frailty in older adults. Neurology 80(22):2055–2061
Del Campo N et al (2016) Relationship of regional brain β-amyloid to gait speed. Neurology 86(1):36–43
Liu C et al (2023) Does the regulation of skeletal muscle influence cognitive function? A scoping review of pre-clinical evidence. J Orthop Translat 38:76–83
Binder DK, Scharfman HE (2004) Brain-derived neurotrophic factor. Growth Factors 22(3):123–131
Park H, Poo MM (2013) Neurotrophin regulation of neural circuit development and function. Nat Rev Neurosci 14(1):7–23
Valenzuela PL et al (2020) Obesity-associated poor muscle quality: prevalence and association with age, sex, and body mass index. BMC Musculoskelet Disord 21(1):200
Shaw FE (2002) Falls in cognitive impairment and dementia. Clin Geriatr Med 18(2):159–173
Vassallo M et al (2004) The effect of changing practice on fall prevention in a rehabilitative hospital: the Hospital Injury Prevention Study. J Am Geriatr Soc 52(3):335–339
Folstein MF, Folstein SE, McHugh PR (1975) “Mini-mental state”. A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res 12(3):189–98
Mohs RC, Cohen L (1988) Alzheimer’s disease assessment scale (ADAS). Psychopharmacol Bull 24(4):627–628
Yesavage JA et al (1982) Development and validation of a geriatric depression screening scale: a preliminary report. J Psychiatr Res 17(1):37–49
McKhann GM et al (2011) The diagnosis of dementia due to Alzheimer’s disease: recommendations from the National Institute on Aging-Alzheimer’s Association workgroups on diagnostic guidelines for Alzheimer’s disease. Alzheimers Dement 7(3):263–269
Petersen RC et al (2001) Current concepts in mild cognitive impairment. Arch Neurol 58(12):1985–1992
Sale A et al (2023) Long-term beneficial impact of the randomised trial ‘Train the Brain’, a motor/cognitive intervention in mild cognitive impairment people: effects at the 14-month follow-up. Age Ageing. https://doi.org/10.1093/ageing/afad067
Mahoney FI, Barthel DW (1965) Functional evaluation: the barthel index. Md State Med J 14:61–65
Rubenstein LZ et al (2001) Screening for undernutrition in geriatric practice: developing the short-form mini-nutritional assessment (MNA-SF). J Gerontol A Biol Sci Med Sci 56(6):M366–M372
Canon ME, Crimmins EM (2011) Sex differences in the association between muscle quality, inflammatory markers, and cognitive decline. J Nutr Health Aging 15(8):695–698
Zhu X et al (2023) Screening efficacy of PhA and MNA-SF in different stages of sarcopenia in the older adults in community. BMC Geriatr 23(1):13
Mattiello R et al (2020) Reference values for the phase angle of the electrical bioimpedance: systematic review and meta-analysis involving more than 250,000 subjects. Clin Nutr 39(5):1411–1417
Kajiyama S et al (2023) The impact of nutritional markers and dietary habits on the bioimpedance phase angle in older individuals. Nutrients. https://doi.org/10.3390/nu15163599
Campa F et al (2023) New bioelectrical impedance vector references and phase angle centile curves in 4,367 adults: the need for an urgent update after 30 years. Clin Nutr 42(9):1749–1758
Bettcher BM, Kramer JH (2014) Longitudinal inflammation, cognitive decline, and Alzheimer’s disease: a mini-review. Clin Pharmacol Ther 96(4):464–469
Heringa SM et al (2014) Markers of low-grade inflammation and endothelial dysfunction are related to reduced information processing speed and executive functioning in an older population—the Hoorn Study. Psychoneuroendocrinology 40:108–118
Teunissen CE et al (2003) Inflammation markers in relation to cognition in a healthy aging population. J Neuroimmunol 134(1–2):142–150
Weaver JD et al (2002) Interleukin-6 and risk of cognitive decline: MacArthur studies of successful aging. Neurology 59(3):371–378
Schram MT et al (2007) Systemic markers of inflammation and cognitive decline in old age. J Am Geriatr Soc 55(5):708–716
Ershler WB, Keller ET (2000) Age-associated increased interleukin-6 gene expression, late-life diseases, and frailty. Annu Rev Med 51:245–270
Funding
The study was partly supported by the Organized Registration for the Assessment of Dementia of the Nationwide General Consortium toward Effective Treatment in Japan.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no direct conflicts of interest regarding the content of this manuscript.
Ethical approval
The study protocol was thoroughly reviewed before being approved by the Ethics Committee of Nagoya University Graduate School of Medicine.
Informed consent
All participants provided written informed consent prior to their participation.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yamada, Y., Watanabe, K., Fujisawa, C. et al. Relationship between cognitive function and phase angle measured with a bioelectrical impedance system. Eur Geriatr Med 15, 201–208 (2024). https://doi.org/10.1007/s41999-023-00894-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s41999-023-00894-8