Abstract
Purpose
Autoimmune Thyroiditis (AIT) is the most common thyroid disease; however, there were no measures to prevent the progression of the disease. The present study attempts to identify that Notch signaling regulates the differentiation of T helper 17 (Th17) cells by activating downstream Phosphatidylinositol-3 kinase/protein kinase/mechanistic target of rapamycin complex 1 (PI3K/AKT/mTORC1) pathway participating in the thyroid injury of the experimental autoimmune thyroiditis (EAT).
Methods
In vivo experiments, mice were randomly divided into 4 groups: a control group, an EAT group, and two groups with LY294002 treatment (pTg plus 25 mg/kg or 50 mg/kg LY294002, respectively). The degrees of thyroiditis were evaluated, and the percentage of Th17 cells, expression of interleukin-17A (IL-17A), and the main components of the Notch–PI3K signaling pathway were detected in different groups. In vitro experiments, two different dosages of LY294002 (25 and 50 μM) were used to intervene splenic mononuclear cells (SMCs) from EAT mice to further evaluate the regulatory effect of Notch–PI3K pathway on Th17 cells.
Results
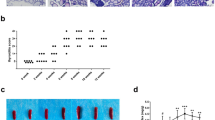
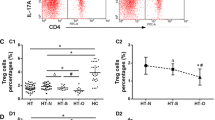
Our data demonstrate that the infiltration of Th17 cells and the expressions of IL-17A, Notch, hairy and split 1 (Hes1), p‑AKT (Ser473), p‑AKT (Thr308), p‑mTOR (Ser2448), S6K1, and S6K2 increased remarkably in EAT mice. After PI3K pathway was blocked, the degrees of thyroiditis were significantly alleviated, and the proportion of Th17 cells, the expression of IL-17A, and the above Notch–PI3K pathway-related molecules decreased in a dose-dependent manner. Additionally, the proportion of Th17 cells was positively correlated with the concentration of serum thyroglobulin antibody (TgAb), IL-17A, and Notch–PI3K pathway-related molecules mRNA levels.
Conclusions
Notch signal promotes the secretion of IL-17A from Th17 cells by regulating the downstream PI3K/AKT/mTORC1 pathway through Hes-Phosphatase and tensin homolog (PTEN) and participates in thyroid autoimmune damage, and the PI3K pathway inhibitor may play important effects on AIT by affecting Th17 cells differentiation.













Similar content being viewed by others
Data availability
The data used to support the findings of this study are available from the corresponding authors upon request.
References
Dayan CM, Daniels GH (1996) Chronic autoimmune thyroiditis. N Engl J Med 335(2):99–107. https://doi.org/10.1056/NEJM199607113350206
Wang B, Shao X, Song R, Xu D, Zhang JA (2017) The emerging role of epigenetics in autoimmune thyroid diseases. Front Immunol 8:396. https://doi.org/10.3389/fimmu.2017.00396
Ralli M, Angeletti D, Fiore M, D’Aguanno V, Lambiase A, Artico M et al (2020) Hashimoto’s thyroiditis: an update on pathogenic mechanisms, diagnostic protocols, therapeutic strategies, and potential malignant transformation. Autoimmun Rev 19(10):102649. https://doi.org/10.1016/j.autrev.2020.102649
Lee GR (2018) The balance of Th17 versus treg cells in autoimmunity. Int J Mol Sci. https://doi.org/10.3390/ijms19030730
Dolff S, Witzke O, Wilde B (2019) Th17 cells in renal inflammation and autoimmunity. Autoimmun Rev 18(2):129–136. https://doi.org/10.1016/j.autrev.2018.08.006
Yasuda K, Takeuchi Y, Hirota K (2019) The pathogenicity of Th17 cells in autoimmune diseases. Semin Immunopathol 41(3):283–297. https://doi.org/10.1007/s00281-019-00733-8
Hanley TL, Yiu ZZ (2017) Role of IL-17 in plaque psoriasis: therapeutic potential of ixekizumab. Ther Clin Risk Manag 13:315–323. https://doi.org/10.2147/TCRM.S111107
Xue H, Yu X, Ma L, Song S, Li Y, Zhang L et al (2015) The possible role of CD4(+)CD25(high)Foxp3(+)/CD4(+)IL-17A(+) cell imbalance in the autoimmunity of patients with Hashimoto thyroiditis. Endocrine 50(3):665–673. https://doi.org/10.1007/s12020-015-0569-y
Xue H, Yang Y, Zhang Y, Song S, Zhang L, Ma L et al (2015) Macrophage migration inhibitory factor interacting with Th17 cells may be involved in the pathogenesis of autoimmune damage in Hashimoto’s thyroiditis. Mediators Inflamm 2015:621072. https://doi.org/10.1155/2015/621072
Brandstadter JD, Maillard I (2019) Notch signalling in T cell homeostasis and differentiation. Open Biol 9(11):190187. https://doi.org/10.1098/rsob.190187
Liu H, Li Y, Zhu Y, Ma L, Xue H (2023) Notch signaling pathway promotes Th17 cell differentiation and participates in thyroid autoimmune injury in experimental autoimmune thyroiditis mice. Mediators Inflamm 2023:1195149. https://doi.org/10.1155/2023/1195149
Wang P, Zhang Q, Tan L, Xu Y, Xie X, Zhao Y (2020) The regulatory effects of mTOR complexes in the differentiation and function of CD4(+) T cell subsets. J Immunol Res 2020:3406032. https://doi.org/10.1155/2020/3406032
Peng X, Zhou J, Li B, Zhang T, Zuo Y, Gu X (2020) Notch1 and PI3K/Akt signaling blockers DAPT and LY294002 coordinately inhibit metastasis of gastric cancer through mutual enhancement. Cancer Chemother Pharmacol 85(2):309–320. https://doi.org/10.1007/s00280-019-03990-4
Jiang H, Fan D, Zhou G, Li X, Deng H (2010) Phosphatidylinositol 3-kinase inhibitor(LY294002) induces apoptosis of human nasopharyngeal carcinoma in vitro and in vivo. J Exp Clin Cancer Res. https://doi.org/10.1186/1756-9966-29-34
Bondar VM, Sweeney-Gotsch B, Andreeff M et al (2002) Induces apoptosis in pancreatic carcinoma cells in vitro and inhibition of the phosphatidylinositol 3′-kinase-AKT pathway in vivo. Mol Cancer Ther 1:989–997
Raphael I, Joern RR, Forsthuber TG (2020) Memory CD4(+) T cells in immunity and autoimmune diseases. Cells. https://doi.org/10.3390/cells9030531
Stadhouders R, Lubberts E, Hendriks RW (2018) A cellular and molecular view of T helper 17 cell plasticity in autoimmunity. J Autoimmun 87:1–15. https://doi.org/10.1016/j.jaut.2017.12.007
Wu B, Wan Y (2020) Molecular control of pathogenic Th17 cells in autoimmune diseases. Int Immunopharmacol 80:106187. https://doi.org/10.1016/j.intimp.2020.106187
Shao S, He F, Yang Y, Yuan G, Zhang M, Yu X (2012) Th17 cells in type 1 diabetes. Cell Immunol 280(1):16–21. https://doi.org/10.1016/j.cellimm.2012.11.001
Ivanov II, McKenzie BS, Zhou L, Tadokoro CE, Lepelley A, Lafaille JJ et al (2006) The orphan nuclear receptor RORgammat directs the differentiation program of proinflammatory IL-17+ T helper cells. Cell 126(6):1121–1133. https://doi.org/10.1016/j.cell.2006.07.035
Ghoreschi K, Laurence A, Yang XP, Tato CM, McGeachy MJ, Konkel JE et al (2010) Generation of pathogenic T(H)17 cells in the absence of TGF-beta signalling. Nature 467(7318):967–971. https://doi.org/10.1038/nature09447
Cerboni S, Gehrmann U, Preite S, Mitra S (2021) Cytokine-regulated Th17 plasticity in human health and diseases. Immunology 163(1):3–18. https://doi.org/10.1111/imm.13280
Wang W, Sun R, Zeng L, Chen Y, Zhang N, Cao S et al (2021) GALNT2 promotes cell proliferation, migration, and invasion by activating the Notch/Hes1-PTEN-PI3K/Akt signaling pathway in lung adenocarcinoma. Life Sci 276:119439. https://doi.org/10.1016/j.lfs.2021.119439
Artero R, Sachan N, Mishra AK, Mutsuddi M, Mukherjee A (2013) The drosophila importin-α3 is required for nuclear import of notch in vivo and it displays synergistic effects with notch receptor on cell proliferation. PLoS ONE. https://doi.org/10.1371/journal.pone.0068247
Henrique D, Schweisguth F (2019) Mechanisms of notch signaling: a simple logic deployed in time and space. Development. https://doi.org/10.1242/dev.172148
Siebel C, Lendahl U (2017) Notch signaling in development, tissue homeostasis, and disease. Physiol Rev 97(4):1235–1294. https://doi.org/10.1152/physrev.00005.2017
Kovall RA, Gebelein B, Sprinzak D, Kopan R (2017) The canonical notch signaling pathway: structural and biochemical insights into shape, sugar, and force. Dev Cell 41(3):228–241. https://doi.org/10.1016/j.devcel.2017.04.001
Chen S, Paveley R, Kraal L, Sritharan L, Stevens E, Dedi N et al (2020) Selective targeting of PI3Kdelta suppresses human IL-17-producing T cells and innate-like lymphocytes and may be therapeutic for IL-17-mediated diseases. J Autoimmun 111:102435. https://doi.org/10.1016/j.jaut.2020.102435
Yu L, Wei J, Liu P (2022) Attacking the PI3K/Akt/mTOR signaling pathway for targeted therapeutic treatment in human cancer. Semin Cancer Biol 85:69–94. https://doi.org/10.1016/j.semcancer.2021.06.019
Vanhaesebroeck B, Guillermet-Guibert J, Graupera M, Bilanges B (2010) The emerging mechanisms of isoform-specific PI3K signalling. Nat Rev Mol Cell Biol 11(5):329–341. https://doi.org/10.1038/nrm2882
Kurebayashi Y, Nagai S, Ikejiri A, Ohtani M, Ichiyama K, Baba Y et al (2012) PI3K-Akt-mTORC1-S6K1/2 axis controls Th17 differentiation by regulating Gfi1 expression and nuclear translocation of RORgamma. Cell Rep 1(4):360–373. https://doi.org/10.1016/j.celrep.2012.02.007
Sarbassov DD, Guertin DA, Ali SM, Sabatini DM (2005) Phosphorylation and regulation of Akt/PKB by the rictor-mTOR complex. Science 307(5712):1098–1101. https://doi.org/10.1126/science.1106148
Alessi DR, James SR, Downes CP, Holmes AB, Gaffney PR, Reese CB et al (1997) Characterization of a 3-phosphoinositide-dependent protein kinase which phosphorylates and activates protein kinase Balpha. Curr Biol 7(4):261–269. https://doi.org/10.1016/s0960-9822(06)00122-9
Chen CY, Chen J, He L, Stiles BL (2018) PTEN: tumor suppressor and metabolic regulator. Front Endocrinol (Lausanne) 9:338. https://doi.org/10.3389/fendo.2018.00338
Manning BD, Toker A (2017) AKT/PKB Signaling: navigating the network. Cell 169(3):381–405. https://doi.org/10.1016/j.cell.2017.04.001
Hua H, Kong Q, Zhang H, Wang J, Luo T, Jiang Y (2019) Targeting mTOR for cancer therapy. J Hematol Oncol. https://doi.org/10.1186/s13045-019-0754-1
Ren W, Yin J, Duan J, Liu G, Tan B, Yang G et al (2016) mTORC1 signaling and IL-17 expression: defining pathways and possible therapeutic targets. Eur J Immunol 46(2):291–299. https://doi.org/10.1002/eji.201545886
Chan SM, Weng AP, Tibshirani R, Aster JC, Utz PJ (2007) Notch signals positively regulate activity of the mTOR pathway in T-cell acute lymphoblastic leukemia. Blood 110(1):278–286. https://doi.org/10.1182/blood-2006-08-039883
Lee K, Nam KT, Cho SH, Gudapati P, Hwang Y, Park DS et al (2012) Vital roles of mTOR complex 2 in Notch-driven thymocyte differentiation and leukemia. J Exp Med 209(4):713–728. https://doi.org/10.1084/jem.20111470
Wong GW, Knowles GC, Mak TW, Ferrando AA, Zuniga-Pflucker JC (2012) HES1 opposes a PTEN-dependent check on survival, differentiation, and proliferation of TCRbeta-selected mouse thymocytes. Blood 120(7):1439–1448. https://doi.org/10.1182/blood-2011-12-395319
Chen CJ, Sgritta M, Mays J, Zhou H, Lucero R, Park J et al (2019) Therapeutic inhibition of mTORC2 rescues the behavioral and neurophysiological abnormalities associated with Pten-deficiency. Nat Med 25(11):1684–1690. https://doi.org/10.1038/s41591-019-0608-y
Wang C, Zhang CJ, Martin BN, Bulek K, Kang Z, Zhao J et al (2017) IL-17 induced NOTCH1 activation in oligodendrocyte progenitor cells enhances proliferation and inflammatory gene expression. Nat Commun 8:15508. https://doi.org/10.1038/ncomms15508
Bedogni B, Warneke JA, Nickoloff BJ, Giaccia AJ, Powell MB (2008) Notch1 is an effector of Akt and hypoxia in melanoma development. J Clin Invest 118(11):3660–3670. https://doi.org/10.1172/JCI36157
Wang X, Chen H, Jiang R, Hong X, Peng J, Chen W et al (2021) Interleukin-17 activates and synergizes with the notch signaling pathway in the progression of pancreatic ductal adenocarcinoma. Cancer Lett 508:1–12. https://doi.org/10.1016/j.canlet.2021.03.003
Acknowledgements
The authors are gratefully for the contributions from Dr. Chen Li and Dr. Lijuan Yang from Medical Research Center of Binzhou Medical University Hospital for their assistance of experimental technology during all experiments.
Funding
This work was supported by grants from the Natural Science Foundation of Shandong Province (No. ZR2013HM049, ZR2022MH175), Key Technology Research and Development Program of Shandong (No. 2016GSF201021), Project of Shandong Province Higher Educational Science and Technology program (No. J16LL01), Reserve Leading Talents Project of Binzhou Medical University Hospital (No. JC2019-03), Scientific Research and Innovation Team Project of Binzhou Medical University Hospital (No. 202031), and Innovation Program of Post-graduate Education of Shandong Province (No. 20038612).
Author information
Authors and Affiliations
Contributions
HX and LM were responsible for the design of this study, and reviewed and edited this article. CH, YL, LG, YL, and BZ performed the experiments. CH participated in data analysis and wrote the first draft of the manuscript, especially for the development of the experimental models and the in vivo and in vitro experiments.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Research involving human participants and/or animals
Human participants were not involved in the present study, and the animal study was reviewed and approved (Approval No. 20220128-73) by the Laboratory Animal Ethics Committee of Binzhou Medical University Hospital (Binzhou, China).
Informed consent
No informed consent is required.
Consent for publication
All the authors have read the manuscript and agreed to submit the paper to the journal.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
He, C., Li, Y., Gan, L. et al. Notch signaling regulates Th17 cells differentiation through PI3K/AKT/mTORC1 pathway and involves in the thyroid injury of autoimmune thyroiditis. J Endocrinol Invest (2024). https://doi.org/10.1007/s40618-023-02293-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s40618-023-02293-z