Abstract
Background
Despite the burden of atrial fibrillation/flutter (AF/AFL) in the USA, an assessment of contemporary mortality trends is scarce in the literature. This study aimed to assess the temporal trends in AF/AFL deaths among US adults by age, sex, race/ethnicity, and census region from 1999 to 2020.
Methods
National mortality data was abstracted from the National Center for Health Statistics to identify decedents whose underlying cause of death was cardiovascular disease and multiple cause of death, AF/AFL. Joinpoint regression assessed mortality trends, and we calculated the average percentage changes (APC) and average annual percentage changes in mortality rates. Results were presented as effect estimates and 95% confidence intervals (95% CI).
Results
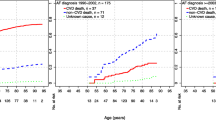
Between 1999 and 2020, 657,126 adults died from AF/AFL in the USA. Contemporary trends have worsened overall except among individuals from the Northeast region for whom the rates have remained stationary since 2015 (APC = 0.1; 95% CI, − 1.0, 1.1). Regional and demographic disparities were observed, with higher rates noted among younger persons below 65 years of age, women (APC = 2.1; 95% CI, 1.7, 2.5), and non-Hispanic Blacks (APC = 4.5; 95% CI, 3.9, 5.2).
Conclusions
The temporal trends in AF/AFL mortality in the USA have exhibited a worsening pattern in recent years, with regional and demographic disparities. Further investigations are warranted to explore the determinants of AF/AFL mortality in the US population and identify factors that may explain the observed differences. Understanding these factors will facilitate efforts to promote improved and equitable health outcomes for the population.



Similar content being viewed by others
Data Availability
The data that support the findings of this study are openly available in the Centers for Disease Control and Prevention’s Wide-ranging Online Data for Epidemiologic Research database.
References
DeLago AJ, Essa M, Ghajar A, Hammond-Haley M, Parvez A, Nawaz I, Philips B. Incidence and mortality trends of atrial fibrillation/atrial flutter in the United States 1990 to 2017. The American journal of cardiology. 2021;148:78–83.
Miyasaka Y, Barnes ME, Gersh BJ, Cha SS, Bailey KR, Abhayaratna WP. Tsang TS (2006) Secular trends in incidence of atrial fibrillation in Olmsted County, Minnesota, 1980 to 2000, and implications on the projections for future prevalence. Circulation. 2006;114(2):119–25.
Schnabel RB, Yin X, Gona P, Larson MG, Beiser AS, McManus DD, Levy D. 50 year trends in atrial fibrillation prevalence, incidence, risk factors, and mortality in the Framingham Heart Study: a cohort study. The Lancet. 2015;386(9989):154–62.
Deshmukh A, Iglesias M, Khanna R, Beaulieu T. Healthcare utilization and costs associated with a diagnosis of incident atrial fibrillation. Heart Rhythm O2. 2022;3(5):577–86. https://doi.org/10.1016/j.hroo.2022.07.010.
Tanaka Y, Shah NS, Passman R, Greenland P, Lloyd-Jones DM, Khan SS. Trends in cardiovascular mortality related to atrial fibrillation in the United States, 2011 to 2018. J Am Heart Assoc. 2021;10(15):e020163.
Piccini JP, Hammill BG, Sinner MF, Jensen PN, Hernandez AF, Heckbert SR, ... & Curtis LH. Incidence and prevalence of atrial fibrillation and associated mortality among Medicare beneficiaries: 1993–2007. Circulation: Cardiov Qual Outcomes 2012; 5(1), 85–93.
Williams BA, Honushefsky AM, Berger PB. Temporal trends in the incidence, prevalence, and survival of patients with atrial fibrillation from 2004 to 2016. Am J Cardiol. 2017;120(11):1961–5.
Centers for Disease Control and Prevention. CDC WONDER. 2023. Retrieved from https://wonder.cdc.gov/ucd-icd10.html
Lloyd-Jones DM, Martin DO, Larson MG, Levy D. Accuracy of death certificates for coding coronary heart disease as the cause of death. Ann Intern Med. 1998;129(12):1020–6.
Kim HJ, Fay MP, Feuer EJ, Midthune DN. Permutation tests for Joinpoint regression with applications to cancer rates. Stat Med. 2000;19(3):335–51.
Ghajar A, Essa M, DeLago A, et al. Atrial fibrillation/atrial flutter related mortality trends in the US population 2010–2020: Regional, racial, sex variations. Pacing Clin Electrophysiol. 2023;46(6):519–25. https://doi.org/10.1111/pace.14643.
Andersson C, Vasan RS. Epidemiology of cardiovascular disease in young individuals. Nat Rev Cardiol. 2018;15(4):230–40. https://doi.org/10.1038/nrcardio.2017.154.
Andes LJ, Cheng YJ, Rolka DB, Gregg EW, Imperatore G. Prevalence of prediabetes among adolescents and young adults in the United States, 2005–2016. JAMA Pediatr. 2020;174(2):e194498. https://doi.org/10.1001/jamapediatrics.2019.4498.
Ogden CL, Carroll MD, Lawman HG, et al. Trends in obesity prevalence among children and adolescents in the United States, 1988–1994 Through 2013–2014. JAMA. 2016;315(21):2292–9. https://doi.org/10.1001/jama.2016.6361.
Baczek VL, Chen WT, Kluger J, Coleman CI. Predictors of warfarin use in atrial fibrillation in the United States: a systematic review and meta-analysis. BMC Fam Pract. 2012;13:1–14.
Hsu JC, Maddox TM, Kennedy KF, Katz DF, Marzec LN, Lubitz SA, Marcus GM. Oral anticoagulant therapy prescription in patients with atrial fibrillation across the spectrum of stroke risk: insights from the NCDR PINNACLE registry. JAMA cardiology. 2016;1(1):55–62.
Penado S, Cano M, Acha O, Hernández JL, Riancho JA. Atrial fibrillation as a risk factor for stroke recurrence. Am J Med. 2003;114(3):206–10.
Rodriguez F, Stefanick ML, Greenland P, Soliman EZ, Manson JE, Parikh N, Perez MV. Racial and ethnic differences in atrial fibrillation risk factors and predictors in women: findings from the Women’s Health Initiative. American Heart Journal. 2016;176:70–7.
Ugowe FE, Jackson LR II, Thomas KL. Racial and ethnic differences in the prevalence, management, and outcomes in patients with atrial fibrillation: a systematic review. Heart Rhythm. 2018;15(9):1337–45.
Essien UR, Chiswell K, Kaltenbach LA, et al. Association of race and ethnicity with oral anticoagulation and associated outcomes in patients with atrial fibrillation: findings from the get with the guidelines–Atrial Fibrillation Registry. JAMA Cardiol. 2022;7(12):1207–17. https://doi.org/10.1001/jamacardio.2022.3704.
Cheranda N, Luo S, Sanfilippo KM, Eisen SA, Schoen MW. Survival in Black and non-Black patients with metastatic prostate cancer. J Clin Oncol. 2023;41(6_suppl):101–101. https://doi.org/10.1200/JCO.2023.41.6_suppl.101.
Montes de Oca MK, Chen Q, Howell E, Wilson LE, Meernik C, Previs RA, ... & Akinyemiju T. Health-care access dimensions and ovarian cancer survival: SEER-Medicare analysis of the ORCHiD study. JNCI Cancer Spectrum 2023; 7(2): pkad011.
Mufarreh A, Shah AJ, Vaccarino V, Kulshreshtha A. Trends in provision of medications and lifestyle counseling in ambulatory settings by gender and race for patients with atherosclerotic cardiovascular disease, 2006–2016. JAMA Netw Open. 2023;6(1):e2251156. https://doi.org/10.1001/jamanetworkopen.2022.51156.
Gillespie CD, Wigington C, Hong Y. Centers for Disease Control and Prevention (CDC). Coronary heart disease and stroke deaths - United States, 2009. MMWR Suppl. 2013;62(3):157–60.
Andrilla CHA, Patterson DG, Garberson LA, Coulthard C, Larson EH. Geographic variation in the supply of selected behavioral health providers. Am J Prev Med. 2018;54(6):S199–207.
Levine DA, Kiefe CI, Howard G, Howard VJ, Williams OD, Allison JJ. Reduced medication access: a marker for vulnerability in US stroke survivors. Stroke. 2007;38(5):1557–64.
Onega T, Duell EJ, Shi X, Wang D, Demidenko E, Goodman D. Geographic access to cancer care in the US. Cancer. 2008;112(4):909–18.
Rossouw JE. Hormones, genetic factors, and gender differences in cardiovascular disease. Cardiovascular Research. 2002;53(3):550–7. https://doi.org/10.1016/S0008-6363(01)00478-3.
Emdin CA, Wong CX, Hsiao AJ, Altman DG, Peters SA, Woodward M, Odutayo AA. Atrial fibrillation as risk factor for cardiovascular disease and death in women compared with men: systematic review and meta-analysis of cohort studies. BMJ. 2016;532:h7013. https://doi.org/10.1136/bmj.h7013.
Volgman AS, Benjamin EJ, Curtis AB, Fang MC, Lindley KJ, Naccarelli GV, ... & American College of Cardiology Committee on Cardiovascular Disease in Women. Women and atrial fibrillation. J Cardiovasc Electrophysiol 2021; 32(10), 2793–2807.
Deshmukh A, Pothineni NV, Patel N, Badheka A, Mulpuru SK, Paydak H, Noseworthy PA. Trends in hospitalizations of young patients with atrial fibrillation: a cause for concern? Int J Cardiol. 2016;203:164–5.
Naderi S, Wang Y, Miller AL, Rodriguez F, Chung MK, Radford MJ, Foody JM. The impact of age on the epidemiology of atrial fibrillation hospitalizations. Am J Med. 2014;127(2):158-e1.
Arias E, Eschbach K, Schauman WS, Backlund EL, Sorlie PD. The Hispanic mortality advantage and ethnic misclassification on US death certificates. Am J Public Health. 2010;100(S1):S171–7.
Mitrani LR, Tumasian RA 3rd, Vilches S, De Los SJ, Gonzalez-Lopez E, Caponetti AG, Saturi G, Mirelis JG, Longhi S, Gagliardi C, Goldsmith J, Rapezzi C, García-Pavía P, Maurer MS. Racial differences in atrial fibrillation management between white patients and black patients in transthyretin cardiac amyloid. Am J Cardiol. 2023;15(187):164–70. https://doi.org/10.1016/j.amjcard.2022.10.039.
Author information
Authors and Affiliations
Contributions
All authors had access to the data and a role in writing the manuscript.
Corresponding author
Ethics declarations
Ethics Approval
No ethical approval required.
Consent to Participate
N/A
Consent for Publication
N/A
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Okoli, U., Ogunsola, A.S., Adeniyi, Z. et al. Regional and Demographic Disparities in Atrial Fibrillation Mortality in the USA. J. Racial and Ethnic Health Disparities (2024). https://doi.org/10.1007/s40615-024-01917-1
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s40615-024-01917-1