Abstract
Objective
Histopathological analysis of the relationship between penile elastography and erectile dysfunction.
Material and method
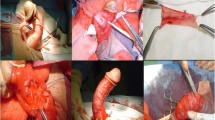
12 patients who applied to our clinic for erectile dysfunction in the last 1 year and accepted this study were included. Preoperative two-dimensional shear wave elastography imaging was performed in 12 patients and recorded in the Pascal (kPa) unit. Approximately 0.5 × 0.5 × 0.5 cm tissue samples were taken from the right and left cavernous tissue during penile prosthesis implantation operation. Tissue samples were sent to the pathology department. The percentage of the area covered by muscle fibers and elastic fibers in the corpus cavernosum was noted semi-quantitatively (ratio of muscle fibers and cavernous body elastic fiber score). All data obtained were compared with each other.
Results
Cavernous body elastic fiber score data(Grouped Score 1, 2 and 3) and percentage of cavernous body muscle fibers data (Grouped %10, %20, %30… %100) were compared with Shear wave elastography data (kPa). The results were not statistically significant according to the Kruskal Wallis Test. Cavernous body elastic fiber score and the percentage of cavernous body muscle fibers were also compared, it was not statistically significant according to the Kruskal Wallis test and Spearman’s correlation test.
Conclusions
Penile shear wave elastography can be used clinically to quantitatively assess the amount of smooth muscle cells and elastic fibers in the penis, but it deserves to be studied with a larger number of patients and a more specific interpretation of the pathology preparation.




Similar content being viewed by others
References
Gratzke C, Angulo J, Chitaley K et al (2010) Anatomy, physiology, and pathophysiology of erectile dysfunction. J Sex Med 7(1 Pt 2):445–475. https://doi.org/10.1111/j.1743-6109.2009.01624.x
NIH Consensus Conference. Impotence. NIH Consensus Development Panel on Impotence. JAMA. 1993;270(1):83–90.
Çayan S, Kendirci M, Yaman Ö et al (2017) Prevalence of erectile dysfunction in men over 40 years of age in Turkey: results from the Turkish Society of Andrology Male Sexual Health Study Group. Turk J Urol 43(2):122–129. https://doi.org/10.5152/tud.2017.24886
Akkus E, Kadioglu A, Esen A, Turkish Erectile Dysfunction Prevalence Study Group, et al. Prevalence and correlates of erectile dysfunction in Turkey: a population-based study. Eur Urol. 2002;41(3):298–304. https://doi.org/10.1016/s0302-2838(02)00027-1.
Nicolosi A, Moreira ED, Shirai M, Bin-Mohd-Tambi MI, Glasser DB (2003) Epidemiology of erectile dysfunction in four countries: cross-national study of the prevalence and correlates of erectile dysfunction. Urology 61(1):201–206. https://doi.org/10.1016/s0090-4295(02)02102-7
Feldman HA, Goldstein I, Hatzichristou DG, Krane RJ, McKinlay JB (1994) Impotence and its medical and psychosocial correlates: results of the Massachusetts Male Aging Study. J Urol 151(1):54–61. https://doi.org/10.1016/s0022-5347(17)34871-1
Azadzoi KM (2006) Vasculogenic erectile dysfunction: beyond the haemodynamic changes. BJU Int 97(1):11–16. https://doi.org/10.1111/j.1464-410X.2006.05778.x
Falke G, Yoo JJ, Kwon TG, Moreland R, Atala A (2003) Formation of corporal tissue architecture in vivo using human cavernosal muscle and endothelial cells seeded on collagen matrices. Tissue Eng 9(5):871–879. https://doi.org/10.1089/107632703322495529
Sarvazyan AP, Rudenko OV, Swanson SD, Fowlkes JB, Emelianov SY (1998) Shear wave elasticity imaging: a new ultrasonic technology of medical diagnostics. Ultrasound Med Biol 24(9):1419–1435. https://doi.org/10.1016/s0301-5629(98)00110-0
Nightingale K, McAleavey S, Trahey G (2003) Shear-wave generation using acoustic radiation force: in vivo and ex vivo results. Ultrasound Med Biol 29(12):1715–1723. https://doi.org/10.1016/j.ultrasmedbio.2003.08.008
Gennisson JL, Deffieux T, Fink M, Tanter M (2013) Ultrasound elastography: principles and techniques. Diagn Interv Imaging 94(5):487–495. https://doi.org/10.1016/j.diii.2013.01.022
Shiina T, Nightingale KR, Palmeri ML et al (2015) WFUMB guidelines and recommendations for clinical use of ultrasound elastography: part 1: basic principles and terminology. Ultrasound Med Biol 41(5):1126–1147. https://doi.org/10.1016/j.ultrasmedbio.2015.03.009
Nowicki A, Dobruch-Sobczak K (2016) Introduction to ultrasound elastography. J Ultrason 16(65):113–124. https://doi.org/10.15557/JoU.2016.0013
Srinivasa-Babu A, Wells ML, Teytelboym OM et al (2016) Elastography in chronic liver disease: modalities, techniques, limitations, and future directions. Radiographics 36(7):1987–2006. https://doi.org/10.1148/rg.2016160042
Nehra A, Goldstein I, Pabby A et al (1996) Mechanisms of venous leakage: a prospective clinicopathological correlation of corporeal function and structure. J Urol 156(4):1320–1329. https://doi.org/10.1016/s0022-5347(01)65578-2
Saenz-de-Tejada I, Moroukian P, Tessier J, Kim JJ, Goldstein I, Frohrib D (1991) Trabecular smooth muscle modulates the capacitor function of the penis. Studies on a rabbit model. Am J Physiol 260(5 Pt 2):H1590–H1595. https://doi.org/10.1152/ajpheart.1991.260.5.H1590
Wespes E, Goes PM, Schiffmann S, Depierreux M, Vanderhaeghen JJ, Schulman CC (1991) Computerized analysis of smooth muscle fibers in potent and impotent patients. J Urol 146(4):1015–1017. https://doi.org/10.1016/s0022-5347(17)37990-9
Corona G, Maggi M (2010) The role of testosterone in erectile dysfunction. Nat Rev Urol 7(1):46–56. https://doi.org/10.1038/nrurol.2009.235
Bastos AL, Sampaio FJ, Cardoso LE (2005) Compositional changes of collagen and glycosaminoglycans in the tunica albuginea and corpus cavernosum from the human penis during the fetal and postnatal periods. J Urol 173(3):1039–1043. https://doi.org/10.1097/01.ju.0000145592.32180.24
Zhang J-J, Qiao X-H, Gao F, Bai M, Li F, Du L-F, Xing J-F (2015) Smooth muscle cells of penis in the rat: noninvasive quantification with shear wave elastography. BioMed Res Int 2015:5. https://doi.org/10.1155/2015/595742
Halls J, Bydawell G, Patel U (2009) Erectile dysfunction: the role of penile Doppler ultrasound in diagnosis. Abdom Imaging 34(6):712–725. https://doi.org/10.1007/s00261-008-9463-x
Zhang JJ, Qiao XH, Gao F et al (2015) Smooth muscle cells of penis in the rat: noninvasive quantification with shear wave elastography. Biomed Res Int 2015:595742. https://doi.org/10.1155/2015/595742 (Epub 2015 Oct 15)
Dean RC, Lue TF (2005) Physiology of penile erection and pathophysiology of erectile dysfunction. Urol Clin North Am 32(4):379–395. https://doi.org/10.1016/j.ucl.2005.08.007
Illiano E, Trama F, Ruffo A et al (2021) Shear wave elastography as a new, non-invasive diagnostic modality for the diagnosis of penile elasticity: a prospective multicenter study. Ther Adv Urol 19(13):17562872211007978
Qiao XH, Zhang JJ, Gao F et al (2017) An experimental study: evaluating the tissue structure of penis with 2D-ShearWave™ Elastography. Int J Impot Res 29(1):12–16. https://doi.org/10.1038/ijir.2016.37
Mariappan YK, Glaser KJ, Ehman RL (2010) Magnetic resonance elastography: a review. Clin Anatomy (New York, NY) 23(5):497–511. https://doi.org/10.1002/ca.21006
Yoon JH, Lee JM, Joo I, Lee ES, Sohn JY, Jang SK, Lee KB, Han JK, Choi BI (2014) Hepatic fibrosis: prospective comparison of MR elastography and US shear-wave elastography for evaluation. Radiology 273(3):772–782. https://doi.org/10.1148/radiol.14132000
Acknowledgements
None declared.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Financial disclosure
None.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Consent to publish
The authors affirm that human research participants provided informed consent for publication of the images in Fig. 1 and Fig. 2
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Bozkurt, Y.E., Gümüş, B.H., Düzgün, F. et al. Comparison of preoperative penile elastographic ultrasound findings and pathological tissue results of patients implemented with penile prosthesis. J Ultrasound 26, 99–105 (2023). https://doi.org/10.1007/s40477-022-00705-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40477-022-00705-z