Abstract
Background and Objective
Immune checkpoint inhibitors (ICIs)—cytotoxic T-lymphocyte antigen-4 (CTLA-4) and programmed death receptor-1 (PD-1) monoclonal antibodies (mAbs)—either as single agents or in combination have become the standard of care for an increasing number of indications. Understanding both the ICI-associated adverse events (AEs) and the possible rank-order of these drugs in terms of susceptibility is essential if we are to improve the curative effect and reduce toxicity.
Methods
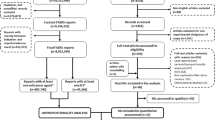
We detected signals of the AEs of ICIs by data mining using the US Food and Drug Administration (FDA) AEs Reporting System (FAERS) database. The definition relied on the preferred terms (PTs) and the standardized MedDRA Queries (SMQs) provided by the Medical Dictionary for Regulatory Activities (MedDRA). Disproportionality analysis was performed by calculating the reporting odds ratios (ROR) with 95% confidence intervals (CIs).
Results
Adverse effects of CTLA-4 and PD-1 mAbs were most commonly observed in the skin, gastrointestinal tract, endocrine systems, liver, and lung, and they included rash, diarrhea, colitis, and thyroid dysfunction. Thyroid dysfunction, type 1 diabetes mellitus, and pneumonitis were more closely associated with the use of anti-PD-1, whereas colitis, diarrhea, hypophysitis, and adrenal insufficiency were more closely associated with anti-CTLA-4; rash and hepatitis occurred similarly in both. Disproportionality signals for less common AEs in other organ systems, including the renal, neurological, cardiac, ocular, musculoskeletal, and hematologic systems, were also detected. Nivolumab and pembrolizumab have very similar safety profiles, but the signal strength of AEs increased when combined with ipilimumab.
Conclusions
The results of this study are in agreement with clinical observations, suggesting the usefulness of pharmacovigilance in “real-world” safety monitoring.
Similar content being viewed by others
References
Haanen JBAG, Carbonnel F, Robert C, et al. Management of toxicities from immunotherapy: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up. Ann Oncol. 2017;28(4):119–42.
Sibaud V, Meyer N, Lamant L, et al. Dermatologic complications of anti-PD-1/PD-L1 immune checkpoint antibodies. Curr Opin Oncol. 2016;28(4):254–63.
Gupta A, De Felice KM, Loftus EV Jr, et al. Systematic review: colitis associated with anti-CTLA-4 therapy. Aliment Pharmacol Ther. 2015;42(4):406–17.
Wei W, Luo Z. Risk of gastrointestinal toxicities with PD-1 inhibitors in cancer patients: a meta-analysis of randomized clinical trials. Medicine (Baltimore). 2017;96(48):e8931.
Wang W, Lie P, Guo M, et al. Risk of hepatotoxicity in cancer patients treated with immune checkpoint inhibitors: a systematic review and meta-analysis of published data. Int J Cancer. 2017;141(5):1018–28.
Le Min. Immune-related endocrine disorders in novel immune checkpoint inhibition therapy. Genes Dis. 2016;3(4):252–6.
Sznol M, Postow MA, Davies MJ, et al. Endocrine-related adverse events associated with immune checkpoint blockade and expert insights on their management. Cancer Treat Rev. 2017;58:70–6.
Harpaz R, DuMouchel W, LePendu P, et al. Performance of pharmacovigilance signal-detection algorithms for the FDA adverse event reporting system. Clin Pharmacol Ther. 2013;93(6):539–46.
Poluzzi E, Raschi E, Piccinni C, et al. Data mining techniques in pharmacovigilance: analysis of the publicly accessible FDA adverse event reporting system (AERS). In: Karahoca A, et al., editors. Data mining applications in engineering and medicine. Croatia: InTech; 2012. p. 265–302.
van Puijenbroek EP, Bate A, Leufkens HG, et al. A comparison of measures of disproportionality for signal detection in spontaneous reporting systems for adverse drug reactions. Pharmacoepidemiol Drug Saf. 2002;11(1):3–10.
Bate A, Evans SJ. Quantitative signal detection using spontaneous ADR reporting. Pharmacoepidemiol Drug Saf. 2009;18(6):427–36.
Barroso-Sousa R, Barry WT, Garrido-Castro AC, et al. Incidence of endocrine dysfunction following the use of different immune checkpoint inhibitor regimens: a systematic review and meta-analysis. JAMA Oncol. 2018;4(2):173–82.
Osorio JC, Ni A, Chaft JE, et al. Antibody-mediated thyroid dysfunction during T-cell checkpoint blockade in patients with non-small-cell lung cancer. Ann Oncol. 2017;28(3):583–9.
Morganstein DL, Lai Z, Spain L, et al. Thyroid abnormalities following the use of cytotoxic T-lymphocyte antigen-4 and programmed death receptor protein-1 inhibitors in the treatment of melanoma. Clin Endocrinol (Oxf). 2017;86(4):614–20.
Corsello SM, Barnabei A, Marchetti P, et al. Endocrine side effects induced by immune checkpoint inhibitors. J Clin Endocrinol Metab. 2013;98(4):1361–75.
Mellati M, Eaton KD, Brooks-Worrell BM, et al. Anti-PD-1 and Anti-PDL-1 monoclonal antibodies causing type 1 diabetes. Diabetes Care. 2015;38(9):e137–8.
Wang DY, Ye F, Zhao S, et al. Incidence of immune checkpoint inhibitor-related colitis in solid tumor patients: a systematic review and meta-analysis. Oncoimmunology. 2017;6(10):e1344805.
Zhang X, Ran Y, Wang Y, et al. Incidence and risk of hepatic toxicities with PD-1 inhibitors in cancer patients: a meta-analysis. Drug Des Devel Ther. 2016;10:3153–61.
Chuzi S, Tavora F, Cruz M, et al. Clinical features, diagnostic challenges, and management strategies in checkpoint inhibitor-related pneumonitis. Cancer Manag Res. 2017;9:207–13.
Wu J, Hong D, Zhang X, et al. PD-1 inhibitors increase the incidence and risk of pneumonitis in cancer patients in a dose-independent manner: a meta-analysis. Sci Rep. 2017;7:44173.
Sibaud V. Dermatologic reactions to immune checkpoint inhibitors: skin toxicities and immunotherapy. Am J Clin Dermatol. 2018;19:345–61.
Belum VR, Benhuri B, Postow MA, et al. Characterisation and management of dermatologic adverse events to agents targeting the PD-1 receptor. Eur J Cancer. 2016;60:12–25.
Boutros C, Tarhini A, Routier E, et al. Safety profiles of anti-CTLA-4 and anti-PD-1 antibodies alone and in combination. Nat Rev Clin Oncol. 2016;13(8):473–86.
Hua C, Boussemart L, Mateus C, et al. Association of vitiligo with tumor response in patients with metastatic melanoma treated with pembrolizumab. JAMA Dermatol. 2016;152(1):45–51.
Murakami N, MotwaniL S, Riella V. Renal complications of immune checkpoint blockade. Curr Probl Cancer. 2017;41(2):100–10.
Johnson DB, Balko JM, Compton ML, et al. Fulminant myocarditis with combination immune checkpoint blockade. N Engl J Med. 2016;375(18):1749–55.
Abdel-Rahman O, Oweira H, Petrausch U, et al. Immune-related ocular toxicities in solid tumor patients treated with immune checkpoint inhibitors: a systematic review. Expert Rev Anticancer Ther. 2017;17(4):387–94.
Cappelli LC, Gutierrez AK, Bingham CO 3rd, et al. Rheumatic and musculoskeletal immune-related adverse events due to immune checkpoint inhibitors: a systematic review of the literature. Arthritis Care Res (Hoboken). 2017;69(11):1751–63.
Zimmer L, Goldinger SM, Hofmann L, et al. Neurological, respiratory, musculoskeletal, cardiac and ocular side-effects of anti-PD-1 therapy. Eur J Cancer. 2016;60:210–25.
Abdel-Rahman O, Eltobgy M, Oweira H, et al. Immune-related musculoskeletal toxicities among cancer patients treated with immune checkpoint inhibitors: a systematic review. Immunotherapy. 2017;9(14):1175–83.
Voskens CJ, Goldinger SM, Loquai C, et al. The price of tumor control: an analysis of rare side effects of anti-CTLA-4 therapy in metastatic melanoma from the ipilimumab network. PLoS One. 2013;8(1):e53745.
Spain L, Walls G, Julve M, et al. Neurotoxicity from immune-checkpoint inhibition in the treatment of melanoma: a single centre experience and review of the literature. Ann Oncol. 2017;28(2):377–85.
Cuzzubbo S, Javeri F, Tissier M, et al. Neurological adverse events associated with immune checkpoint inhibitors: review of the literature. Eur J Cancer. 2017;73:1–8.
Cortes J, Mauro M, Steegmann JL, et al. Cardiovascular and pulmonary adverse events in patients treated with BCR-ABL inhibitors: data from the FDA adverse event reporting system. Am J Hematol. 2015;90(4):E66–72.
Author information
Authors and Affiliations
Contributions
JHH and TXW planned this study’s content, extracted data, performed statistical analysis, and wrote the manuscript. JYT, SL and DZ participated in the design of the study and helped to write the manuscript. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Funding
This study was supported by the Health and Family Planning Commission of Chongqing grants (2016ZDXM017), Chongqing Science and Technology Commission grants (cstc2016shmszx130048).
Conflict of interest
Huan-huan JI, Xue-wen TANG, Zhi DONG, Lin SONG, and Yun-tao JIA declare that they have no conflict of interests.
Rights and permissions
About this article
Cite this article
Ji, Hh., Tang, Xw., Dong, Z. et al. Adverse Event Profiles of Anti-CTLA-4 and Anti-PD-1 Monoclonal Antibodies Alone or in Combination: Analysis of Spontaneous Reports Submitted to FAERS. Clin Drug Investig 39, 319–330 (2019). https://doi.org/10.1007/s40261-018-0735-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40261-018-0735-0