Abstract
Background
Placebo-controlled studies have reported the efficacy of apremilast in the management of palmoplantar psoriasis but studies comparing efficacy with a conventional agent are lacking.
Objective
The objective of this article was to compare the efficacy and safety of apremilast and methotrexate in patients with palmoplantar psoriasis.
Methods
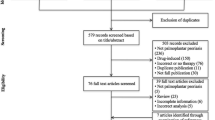
In this prospective, randomized, active-controlled, observer-blinded clinical trial, conducted at a psoriasis clinic of a tertiary care institute in India from 1 July, 2019 to 1 June, 2020, 84 patients with palmoplantar psoriasis were randomized (1:1) to receive either methotrexate (0.4 mg/kg/week orally) or apremilast (30 mg twice daily). The treatment protocol was continued for 16 weeks or until achieving a ≥ 75% improvement in the Modified Palmoplantar Psoriasis Area and Severity Index (m-PPPASI 75), whichever was earlier. Changes in m-PPPASI and Dermatology Life Quality Index scores from baseline, the proportion of patients achieving m-PPPASI 75, and adverse events were assessed.
Results
Eighty-four patients were included (76 palmoplantar psoriasis and 8 palmoplantar pustulosis). The mean age (standard deviation) was 44.5 (12.9) years and 53 (63%) were women. The m-PPPASI score [median (interquartile range)] after 16 weeks of treatment showed a significant improvement from baseline in both apremilast [− 6.3 (10.9), p < 0.001] and methotrexate groups [− 8.5 (9.9), p < 0.001]. The estimated median difference between the groups was − 1.2 (p = 0.39, 95% confidence interval − 4.2 to 2.1). At 16 weeks, m-PPPASI 75 was achieved by 14/42 (33%) and 17/42 (41%) patients in the apremilast and methotrexate groups, respectively (p = 0.49). A significant reduction in the Dermatology Life Quality Index score [median (interquartile range)] was observed in both groups [apremilast: − 3.0 (6.0), p < 0.001; methotrexate: − 3.0 (6.3), p < 0.001] with an estimated median difference of 0.0 (p = 0.99, 95% confidence interval − 1.0 to 2.0). The proportion of patients experiencing adverse events was comparable (p = 0.49).
Conclusions
Apremilast showed a comparable efficacy and safety profile to methotrexate in the management of palmoplantar psoriasis.
Clinical Trial Registration
CTRI/2019/06/019830, date of registration: 24 June, 2019; trial registered prospectively.


Similar content being viewed by others
References
Chung J, Callis Duffin K, Takeshita J, Shin DB, Krueger GG, Robertson AD, et al. Palmoplantar psoriasis is associated with greater impairment of health-related quality of life compared with moderate to severe plaque psoriasis. J Am Acad Dermatol. 2014;71(4):623–32. https://doi.org/10.1016/j.jaad.2014.04.063.
Merola JF, Qureshi A, Husni ME. Underdiagnosed and undertreated psoriasis: nuances of treating psoriasis affecting the scalp, face, intertriginous areas, genitals, hands, feet, and nails. Dermatol Ther. 2018;31(3):e12589. https://doi.org/10.1111/dth.12589.
Raposo I, Torres T. Palmoplantar psoriasis and palmoplantar pustulosis: current treatment and future prospects. Am J Clin Dermatol. 2016;17(4):349–58. https://doi.org/10.1007/s40257-016-0191-7.
Wald JM, Klufas DM, Strober BE. The use of methotrexate, alone or in combination with other therapies, for the treatment of palmoplantar psoriasis. J Drugs Dermatol. 2015;14(8):888–92.
Gupta SK, Singh KK, Lalit M. Comparative therapeutic evaluation of different topicals and narrow band ultraviolet B therapy combined with systemic methotrexate in the treatment of palmoplantar psoriasis. Indian J Dermatol. 2011;56(2):165–70. https://doi.org/10.4103/0019-5154.80410.
Greenberg R, Goldsmith T, Zeltser D, Shapira I, Berliner S, Rogowski O, et al. Comorbidities in patients with palmoplantar plaque psoriasis. J Am Acad Dermatol. 2021;84(3):639–43. https://doi.org/10.1016/j.jaad.2020.03.112.
Brunasso AM, Puntoni M, Aberer W, Delfino C, Fancelli L, Massone C. Clinical and epidemiological comparison of patients affected by palmoplantar plaque psoriasis and palmoplantar pustulosis: a case series study. Br J Dermatol. 2013;168(6):1243–51. https://doi.org/10.1111/bjd.12223.
Mease PJ. Apremilast: a phosphodiesterase 4 inhibitor for the treatment of psoriatic arthritis. Rheumatol Ther. 2014;1(1):1–20. https://doi.org/10.1007/s40744-014-0005-4.
Cutolo M, Myerson GE, Fleischmann RM, Lioté F, Díaz-González F, Van den Bosch F, et al. A phase III, randomized, controlled trial of apremilast in patients with psoriatic arthritis: results of the PALACE 2 trial. J Rheumatol. 2016;43(9):1724–34. https://doi.org/10.3899/jrheum.151376.
Edwards CJ, Blanco FJ, Crowley J, Birbara CA, Jaworski J, Aelion J, et al. Apremilast, an oral phosphodiesterase 4 inhibitor, in patients with psoriatic arthritis and current skin involvement: a phase III, randomised, controlled trial (PALACE 3). Ann Rheum Dis. 2016;75(6):1065–73. https://doi.org/10.1136/annrheumdis-2015-207963.
Papp K, Reich K, Leonardi CL, Kircik L, Chimenti S, Langley RG, et al. Apremilast, an oral phosphodiesterase 4 (PDE4) inhibitor, in patients with moderate to severe plaque psoriasis: results of a phase III, randomized, controlled trial (Efficacy and Safety Trial Evaluating the Effects of Apremilast in Psoriasis [ESTEEM] 1). J Am Acad Dermatol. 2015;73(1):37–49. https://doi.org/10.1016/j.jaad.2015.03.049.
Paul C, Cather J, Gooderham M, Poulin Y, Mrowietz U, Ferrandiz C, et al. Efficacy and safety of apremilast, an oral phosphodiesterase 4 inhibitor, in patients with moderate-to-severe plaque psoriasis over 52 weeks: a phase III, randomized controlled trial (ESTEEM 2). Br J Dermatol. 2015;173(6):1387–99. https://doi.org/10.1111/bjd.14164.
Bissonnette R, Pariser DM, Wasel NR, Goncalves J, Day RM, Chen R, et al. Apremilast, an oral phosphodiesterase-4 inhibitor, in the treatment of palmoplantar psoriasis: results of a pooled analysis from phase II PSOR-005 and phase III Efficacy and Safety Trial Evaluating the Effects of Apremilast in Psoriasis (ESTEEM) clinical trials in patients with moderate to severe psoriasis. J Am Acad Dermatol. 2016;75(1):99–105. https://doi.org/10.1016/j.jaad.2016.02.1164.
Bissonnette R, Haydey R, Rosoph LA, Lynde CW, Bukhalo M, Fowler JF, et al. Apremilast for the treatment of moderate-to-severe palmoplantar psoriasis: results from a double-blind, placebo-controlled, randomized study. J Eur Acad Dermatol Venereol. 2018;32(3):403–10. https://doi.org/10.1111/jdv.14647.
Brunasso AM, Salvini C, Massone C. Efalizumab for severe palmo-plantar psoriasis: an open-label pilot trial in five patients. J Eur Acad Dermatol Venereol. 2009;23(4):415–9. https://doi.org/10.1111/j.1468-3083.2008.03062.x.
Finlay AY, Khan GK. Dermatology Life Quality Index (DLQI): a simple practical measure for routine clinical use. Clin Exp Dermatol. 1994;19(3):210–6. https://doi.org/10.1111/j.1365-2230.1994.tb01167.x.
Singhal R, Diwan NG, Nair PA. Impact of palmoplantar dermatoses on quality of life. Indian Dermatol Online J. 2018;9(5):309–13. https://doi.org/10.4103/idoj.IDOJ_347_17.
Misiak-Galazka M, Wolska H, Rudnicka L. What do we know about palmoplantar pustulosis? J Eur Acad Dermatol Venereol. 2017;31(1):38–44. https://doi.org/10.1111/jdv.13846.
Reich K, Bomas S, Korge B, Manasterski M, Schwichtenberg U, Mentz H, et al. Physician- and patient-reported outcomes with apremilast for patients with plaque psoriasis during routine dermatology care in Germany: a second interim analysis. J Am Acad Dermatol. 2018;79(3):AB221. https://doi.org/10.1016/j.jaad.2018.05.884.
Janagond AB, Kanwar AJ, Handa S. Efficacy and safety of systemic methotrexate vs acitretin in psoriasis patients with significant palmoplantar involvement: a prospective, randomized study. J Eur Acad Dermatol Venereol. 2013;27(3):e384–9. https://doi.org/10.1111/jdv.12004.
Ara S, Mowla MR, Alam M, Khan I. Efficacy of oral methotrexate (MTX) monotherapy vs oral MTX plus narrowband ultraviolet light B phototherapy in palmoplantar psoriasis. Dermatol Ther. 2020;33(4):e13486. https://doi.org/10.1111/dth.13486.
Afra TP, Razmi TM, Dogra S. Apremilast in psoriasis and beyond: big hopes on a small molecule. Indian Dermatol Online J. 2019;10(1):1–12. https://doi.org/10.4103/idoj.IDOJ_437_18.
Kt S, Thakur V, Dogra S, Handa S, Narang T. Photosensitivity during apremilast treatment in patients with palmoplantar psoriasis. Int J Dermatol. 2020;59(12):e442–4. https://doi.org/10.1111/ijd.15051.
Del Alcázar E, Suárez-Pérez JA, Armesto S, Rivera R, Herrera-Acosta E, Herranz P, et al. Real-world effectiveness and safety of apremilast in psoriasis at 52 weeks: a retrospective, observational, multicentre study by the Spanish Psoriasis Group. J Eur Acad Dermatol Venereol. 2020;34(12):2821–9. https://doi.org/10.1111/jdv.16439.
West J, Ogston S, Foerster J. Safety and efficacy of methotrexate in psoriasis: a meta-analysis of published trials. PLoS ONE. 2016;11(5):e0153740. https://doi.org/10.1371/journal.pone.0153740.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No sources of funding were received for the conduct of this study or the preparation of this article.
Conflict of Interest
Soufila KT, Vishal Thakur, Tarun Narang,Sunil Dogra, and Sanjeev Handa have no conflicts of interest that are directly relevant to the content of this article.
Ethics Approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the institutional ethics committee.
Consent to Participate
Informed consent was obtained from all individual participants included in the study.
Availability of Data and Material
The datasets generated and analyzed during the current study are available from the corresponding author on reasonable request.
Author Contributions
Study concept and design: SKT, VT, TN, SD, SH. Analysis and interpretation of data: SKT, VT, TN, SD. Drafting of the manuscript: SKT, VT, TN. Critical revision of the manuscript for important intellectual content: TN, SD, SH. Statistical analysis: SKT, VT. Study supervision: TN, SD, SH.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
KT, S., Thakur, V., Narang, T. et al. Comparison of the Efficacy and Safety of Apremilast and Methotrexate in Patients with Palmoplantar Psoriasis: A Randomized Controlled Trial. Am J Clin Dermatol 22, 415–423 (2021). https://doi.org/10.1007/s40257-021-00596-6
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40257-021-00596-6