Abstract
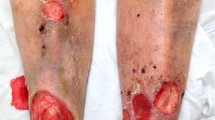
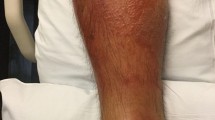
Coagulase-negative staphylococcus organisms may be normal flora of human skin, however these bacteria can also be pathogens in skin and soft tissue infections. A summary of skin and soft tissue infections caused by coagulase-negative staphylococcus species is provided in this review. We conducted a search of the PubMed database using the following terms: abscess, auricularis, biofilm, capitis, cellulitis, coagulase, contaminant, cyst, draining, epidermidis, felon, folliculitis, furuncle, haemolyticus, hominis, indolent, infection, lugdunensis, mecA, microbiome, negative, osteomyelitis, paronychia, saprophyticus, skin, simulans, sinus, soft, staphylococcus, systemic, tissue, virulence, virulent, and vulvar. The relevant papers, and their references, generated by the search were reviewed. Skin and soft tissue infections have been observed to be caused by many coagulase-negative staphylococcus organisms: Staphylococcus auricularis, Staphylococcus capitis, Staphylococcus epidermidis, Staphylococcus haemolyticus, Staphylococcus hominis, Staphylococcus lugdunensis, Staphylococcus saprophyticus, and Staphylococcus simulans. Coagulase-negative staphylococcus skin infections predominantly present as abscesses and paronychia. They are most common in elderly patients or those individuals who are immunosuppressed, and tend to be broadly susceptible to antibiotic treatment. In conclusion, albeit less common, coagulase-negative staphylococcus organisms can result in skin and soft tissue infections, particularly in older and/or immunocompromised individuals. A review of the literature found that coagulase-negative staphylococcus organisms are most commonly grown in cultures of abscesses and paronychia. Therefore, coagulase-negative staphylococcal organisms should not always be considered as contaminants or normal flora, but rather as causative pathogens. They are usually susceptible to antibiotics used to treat methicillin-sensitive Staphylococcus aureus.


Similar content being viewed by others
References
Piette A, Verschraegen G. Role of coagulase-negative staphylococci in human disease. Vet Microbiol. 2009;134:45–54. https://doi.org/10.1016/j.vetmic.2008.09.009.
Yu W, Kim HK, Rauch S, Schneewind O, Missiakas D. Pathogenic conversion of coagulase-negative staphylococci. Microbes Infect. 2017;19:101–9. https://doi.org/10.1016/j.micinf.2016.12.002.
Rogers K, Fey P, Rupp M. Coagulase-negative staphylococcal infections. Infect Dis Clin N Am. 2009;23:73–98. https://doi.org/10.1016/j.idc.2008.10.001.
Akiyama H, Kanzaki H, Tada J, Arata J. Coagulase-negative staphylococci isolated from various skin lesions. J Dermatol. 1998;25:563–8. https://doi.org/10.1111/j.1346-8138.1998.tb02459.x.
Fukuda S, Wada K, Yasuda K, Iwasa J, Yamaguchi S. Acute osteomyelitis of the acetabulum induced by Staphylococcus capitis in a young athlete. Pediatr Rep. 2010;2:e2. https://doi.org/10.4081/pr.2010.e2.
Lai Y, Di Nardo A, Nakatsuji T, Leichtle A, Yang Y, Cogen AL, et al. Commensal bacteria regulate Toll-like receptor 3-dependent inflammation after skin injury. Nat Med. 2009;15:1377–82. https://doi.org/10.1038/nm.2062.
Nguyen TH, Park MD, Otto M. Host response to Staphylococcus epidermidis colonization and infections. Front Cell Infect Microbiol. 2017;7:90. https://doi.org/10.3389/fcimb.2017.00090.
Spiliopoulou AI, Kolonitsiou F, Krevvata MI, Leontsinidis M, Wilkinson TS, Mack D, et al. Bacterial adhesion, intracellular survival and cytokine induction upon stimulation of mononuclear cells with planktonic or biofilm phase Staphylococcus epidermidis. FEMS Microbiol Lett. 2012;330:56–65. https://doi.org/10.1111/j.1574-6968.2012.02533.x.
Mustafa O, Althakafi S, Kattan S, Kattan M, AlHathal N. Scrotal abscess precipitating late infection of a malleable penile prosthesis: the risk never evanesces. Case Rep Urol. 2016;3280418. 10.1155/2016/3280418
Hessam S, Sand M, Georgas D, Anders A, Bechara FG. Microbial profile and antimicrobial susceptibility of bacteria found in inflammatory hidradenitis suppurativa lesions. Skin Pharmacol Physiol. 2016;29:161–7. https://doi.org/10.1159/000446812.
Gautam V, Sethuraman N, Kaur R, Sachdev S, Marwaha N, Ray P. Changing epidemiology of coagulase-negative staphylococci in normal flora of skin. Indian J Med Microbiol. 2017;35:277–8. https://doi.org/10.4103/ijmm.IJMM_16_282.
Caccavale S, La Montagna M. Uncommon superficial angiomyxoma of the vulva complicated with condyloma acuminatum and Staphylococcus hominis infection: a mere example of gynecological immunocompromised district. Int J Dermatol. 2015;54:505–6. https://doi.org/10.1111/ijd.12931.
Kutsyk RV, Kurovets LM. Species composition and antibiotic sensitivity of staphylococci isolated from patients with furunculosis. Mikrobiol Z. 2002;64:59–62.
Heldt Manica LA, Cohen PR. Staphylococcus lugdunensis infections of the skin and soft tissue: a case series and review. Dermatol Ther. 2017;7:555–62. https://doi.org/10.1007/s13555-017-0202-5.
Heldt Manica LA, Cohen PR. Cutaneous Staphylococcus lugdunensis infection: an emerging bacterial pathogen. Dermatol Online J. 2018;24(3). pii: 13030/qt4sv3z6gk.
Mehmood M, Khasawneh FA. Staphylococcus lugdunensis gluteal abscess in a patient with end stage renal disease on hemodialysis. Clin Pract. 2018;5:706. https://doi.org/10.4081/cp.2015.706.
Papapetropoulos N, Papapetropoulou M, Vantarakis A. Abscesses and wound infections due to staphylococcus lugdunensis: report of 16 cases. Infection. 2013;41:525–8. https://doi.org/10.1007/s15010-012-0381-z.
Bellamy R, Barkham T. Staphylococcus lugdunensis infection sites: predominance of abscesses in the pelvic girdle region. Clin Infect Dis. 2002;35:E32–4. https://doi.org/10.1086/341304.
Males BM, Bartholomew WR, Amsterdam D. Staphylococcus simulans septicemia in a patient with chronic osteomyelitis and pyarthrosis. J Clin Microbiol. 1985;21:255–7.
Shields BE, Tschetter AJ, Wanat KA. Staphylococcus simulans: an emerging cutaneous pathogen. JAAD Case Rep. 2016;2:428–9. https://doi.org/10.1016/j.jdcr.2016.08.0157.2.
Argemi X, Hansmann Y, Riegel P, Prévost G. Is Staphylococcus lugdunensis significant in clinical samples? J Clin Microbiol. 2017;55:3167–74. https://doi.org/10.1128/JCM.00846-17.
Huda S, Azmiza SJ, Tengku J, Rosni I. A review of Staphylococcal cassette chromosome mec (SCCmec) types in coagulase-negative staphylococci (CoNS) species. Malays J Med Sci. 2017;24:7–18. https://doi.org/10.21315/mjms2017.24.5.2.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Funding
No funding was received for the preparation of this manuscript.
Conflicts of interest
NE Natsis and PR Cohen have no conflicts of interest to declare.
Rights and permissions
About this article
Cite this article
Natsis, N.E., Cohen, P.R. Coagulase-Negative Staphylococcus Skin and Soft Tissue Infections. Am J Clin Dermatol 19, 671–677 (2018). https://doi.org/10.1007/s40257-018-0362-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40257-018-0362-9