Abstract
Purpose
The aim of this updated systematic review and meta-analysis was the association between hyperglycemia and periodontitis.
Methods
We searched PubMed/MEDLINE, Web of Science, and Scopus until March 2021. The key search words were based on "periodontitis" and "hyperglycemia." We included cohort, case–control, and cross-sectional studies, restricted to publications in English. The quality assessment of included studies and data extraction were done by two independent reviewers. Meta-analysis was performed for cross-sectional studies using the random-effects model.
Results
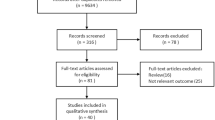
The literature search yielded 340 studies, and finally, 19 and 11 studies were included in systematic review and meta-analysis, respectively. The total sample size of the eligible studies in the meta-analysis was 38,896 participants, of whom 33% were male with a mean age of 51.20 ± 14.0 years. According to a random-effect meta-analysis in cross-sectional studies, the pooled odds ratio (OR) for the association between hyperglycemia and periodontal indices was statistically significant (OR: 1.50, 95%CI: 1.11, 1.90). There was evidence of publication bias (coefficient: − 3.53, p-value = 0.014) which, after imputing missing studies, the pooled OR of the association between hyperglycemia and periodontitis change to 1.55 (95%CI: 1.20, 1.90).
Conclusion
Results of the present study show that hyperglycemia was positively associated with periodontitis. However, more cohort and prospective longitudinal studies should be conducted to find the exact association. Overall, it seems the management of hyperglycemia could be considered as a preventive strategy for periodontitis.



Similar content being viewed by others
References
Slots J. Periodontitis: facts, fallacies and the future. Periodontology 2000. 2017;75(1):7–23.
Eke PI, Borgnakke WS, Genco RJ. Recent epidemiologic trends in periodontitis in the USA. Periodontology 2000. 2020;82(1):257–67.
Frencken JE, et al. Global epidemiology of dental caries and severe periodontitis–a comprehensive review. J Clin Periodontol. 2017;44:S94–105.
Löe H. Periodontal disease. The sixth complication of diabetes mellitus. Diabetes Care. 1993;16(1):329–34.
Bullon P, et al. Metabolic syndrome and periodontitis: is oxidative stress a common link? J Dent Res. 2009;88:503–18.
Dandona P, Aljada A, Bandyopadhyay A. Inflammation: the link between insulin resistance, obesity and diabetes. Trends Immunol. 2004;25:4–7.
Deshpande K, et al. Diabetes and periodontitis. J Indian Soc Periodontol. 2010;14:207.
Wu Y-Y, Xiao E, Graves DT. Diabetes mellitus related bone metabolism and periodontal disease. I J Oral Sci. 2015;7:63–72.
Moher D, et al. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Int J Surg. 2010;8(5):336–41.
Stang A. Critical evaluation of the Newcastle-Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur J Epidemiol. 2010;25(9):603–5.
Higgins JPT, et al. Measuring inconsistency in meta-analyses. BMJ. 2003;327(7414):557–60.
Kushiyama M, Shimazaki Y, Yamashita Y. Relationship between metabolic syndrome and periodontal disease in Japanese adults. J Periodontol. 2009;80(10):1610–5.
Morita T, et al. Association between periodontal disease and metabolic syndrome. J Public Health Dent. 2009;69(4):248–53.
Morita T, et al. A cohort study on the association between periodontal disease and the development of metabolic syndrome. J Periodontol. 2010;81(4):512–9.
Kwon YE, et al. The relationship between periodontitis and metabolic syndrome among a Korean nationally representative sample of adults. J Clin Periodontol. 2011;38:781–6.
Katz J. Elevated blood glucose levels in patients with severe periodontal disease. J Clin Periodontol. 2001;28(7):710–2.
Chuang S-F, et al. Oral and dental manifestations in diabetic and nondiabetic uremic patients receiving hemodialysis. Oral Surg Oral Med Oral Pathol Oral Radiol Endodontol. 2005;99(6):689–95.
D’Aiuto F, et al. Association of the metabolic syndrome with severe periodontitis in a large US population-based survey. J Clin Endocrinol Metabol. 2008;93(10):3989–94.
Benguigui C, et al. Metabolic syndrome, insulin resistance, and periodontitis: a cross-sectional study in a middle-aged French population. J Clin Periodontol. 2010;37(7):601–8.
Thanakun S, et al. Association of untreated metabolic syndrome with moderate to severe periodontitis in Thai population. J Periodontol. 2014;85(11):1502–14.
LaMonte MJ, et al. Association between metabolic syndrome and periodontal disease measures in postmenopausal women: the Buffalo OsteoPerio study. J Periodontol. 2014;85(11):1489–501.
Minagawa K, et al. Relationship between metabolic syndrome and periodontitis in 80-year-old Japanese subjects. J Periodontal Res. 2015;50(2):173–9.
Teeuw WJ, et al. Periodontitis as a possible early sign of diabetes mellitus. BMJ Open Diab Res Care. 2017;5(1):e000326.
Timonen P, et al. Metabolic syndrome, periodontal infection, and dental caries. J Dent Res. 2010;89(10):1068–73.
Shimazaki Y, et al. Relationship of metabolic syndrome to periodontal disease in Japanese women: the Hisayama Study. J Dent Res. 2007;86(3):271–5.
Chen L, et al. Association of periodontal parameters with metabolic level and systemic inflammatory markers in patients with type 2 diabetes. J Periodontol. 2010;81(3):364–71.
Susanto H, et al. Periodontal inflamed surface area and C-reactive protein as predictors of HbA1c: a study in Indonesia. Clin Oral Invest. 2012;16(4):1237–42.
Iwasaki M, et al. Longitudinal relationship between metabolic syndrome and periodontal disease among Japanese adults aged≥ 70 years: the Niigata Study. J Periodontol. 2015;86(4):491–8.
Tanwir F, Tariq A. Effect of glycemic conrol on periodontal status. J Coll Physicians Surg Pak. 2012;22(6):371–4.
Khader Y, et al. Periodontal status of patients with metabolic syndrome compared to those without metabolic syndrome. J Periodontol. 2008;79(11):2048–53.
Rocchietta I, Nisand D. A review assessing the quality of reporting of risk factor research in implant dentistry using smoking, diabetes and periodontitis and implant loss as an outcome: critical aspects in design and outcome assessment. J Clin Periodontol. 2012;39:114–21.
Nascimento GG, et al. Does diabetes increase the risk of periodontitis? A systematic review and meta-regression analysis of longitudinal prospective studies. Acta Diabetol. 2018;55(7):653–67.
Mealey BL, Oates TW. Diabetes mellitus and periodontal diseases. J Periodontol. 2006;77(8):1289–303.
Corbella S, et al. Effect of periodontal treatment on glycemic control of patients with diabetes: A systematic review and meta-analysis. J Diabetes Invest. 2013;4(5):502–9.
Graves DT, et al. Diabetes-enhanced inflammation and apoptosis–impact on periodontal pathology. J Dent Res. 2006;85(1):15–21.
Pradhan S, Goel K. Interrelationship between diabetes and periodontitis: a review. JNMA. 2011;51(183):144–53.
Hardo PG, et al. Helicobacter pylori infection and dental care. Gut. 1995;37(1):44–6.
Zarić S, et al. Periodontal therapy improves gastric Helicobacter pylori eradication. J Dent Res. 2009;88(10):946–50.
Bascones-Martinez A, Gonzalez-Febles J, Sanz-Esporrin J. Diabetes and periodontal disease. Review of the literature. Am J Dent. 2014;27(2):63–7.
Stanko P, Holla LI. Bidirectional association between diabetes mellitus and inflammatory periodontal disease. A review. Biomed Pap Med Fac Univ Palacky Olomouc Czech Repub. 2014;158(1):35–8.
Acknowledgements
Research reported in this publication was supported by Elite Researcher Grant Committee under award number [971188] from the National Institute for Medical Research Development (NIMAD), Tehran, Iran.
Funding
Not applicable.
Author information
Authors and Affiliations
Contributions
AM: contributed to the conception, design, interpretation, did a search strategy, analyzed data, drafted the manuscript, and critically revised the manuscript; SD: contributed to the conception, investigated quality assessment of studies, and drafted the manuscript. ES: contributed to the conception, extracted, and extracted and analyzed data; ED: contributed to the conception, assessed the studies, and critically revised the manuscript; JH: contributed to the conception, assessed the studies, investigated quality assessment; AM-G: contributed to the conception, assessed the studies, and investigated quality assessment; RH, contributed to the conception, assessed the studies, drafted the manuscript, and critically revised the manuscript; MQ, contributed to conception, design, interpretation, assessed and investigated studies, extracted data, drafted the manuscript critically, and revised the manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
Not applicable.
Ethical approval
The protocol study and the proposal approved by the ethical committee of Alborz University of Medical Sciences. All of the included studies would be cited in all reports and all future publications.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Mirzaei, A., Shahrestanaki, E., Daneshzad, E. et al. Association of hyperglycaemia and periodontitis: an updated systematic review and meta-analysis. J Diabetes Metab Disord 20, 1327–1336 (2021). https://doi.org/10.1007/s40200-021-00861-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40200-021-00861-9