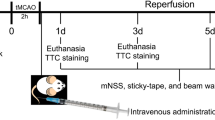
Abstract
Stroke is the leading cause of severe long-term disability. Cell therapy has recently emerged as an approach to facilitate functional recovery in stroke. Although administration of peripheral blood mononuclear cells preconditioned by oxygen–glucose deprivation (OGD-PBMCs) has been shown to be a therapeutic strategy for ischemic stroke, the recovery mechanisms remain largely unknown. We hypothesised that cell–cell communications within PBMCs and between PBMCs and resident cells are necessary for a polarising protective phenotype. Here, we investigated the therapeutic mechanisms underlying the effects of OGD-PBMCs through the secretome. We compared levels of transcriptomes, cytokines, and exosomal microRNA in human PBMCs by RNA sequences, Luminex assay, flow cytometric analysis, and western blotting under normoxic and OGD conditions. We also performed microscopic analyses to assess the identification of remodelling factor-positive cells and evaluate angiogenesis, axonal outgrowth, and functional recovery by blinded examination by administration of OGD-PBMCs after ischemic stroke in Sprague–Dawley rats. We found that the therapeutic potential of OGD-PBMCs was mediated by a polarised protective state through decreased levels of exosomal miR-155-5p, and upregulation of vascular endothelial growth factor and a pluripotent stem cell marker stage-specific embryonic antigen-3 through the hypoxia-inducible factor-1α axis. After administration of OGD-PBMCs, microenvironment changes in resident microglia by the secretome promoted angiogenesis and axonal outgrowth, resulting in functional recovery after cerebral ischemia. Our findings revealed the mechanisms underlying the refinement of the neurovascular unit by secretome-mediated cell–cell communications through reduction of miR-155-5p from OGD-PBMCs, highlighting the therapeutic potential carrier of this approach against ischemic stroke.








Similar content being viewed by others
Availability of Data and Materials
All miRNA microarray data were deposited in the Gene Expression Omnibus (GEO) (https://www.ncbi.nlm.nih.gov/geo/) database (accession number: miRNA data, GSE190407). All other relevant data and materials are available within the article file or Supplementary Information or are available from the authors on reasonable request.
Abbreviations
- ANOVA:
-
Analysis of variance
- CD:
-
Cluster of differentiation
- CNS:
-
Central nervous system
- DAPI:
-
4′,6′-Diamidino-2-phenylindole
- GAP43:
-
Growth associated protein 43
- GO:
-
Gene ontology
- HIF-1α:
-
Hypoxia-inducible factor-1alpha
- IL:
-
Interleukin
- KEGG:
-
Kyoto Encyclopaedia of Genes and Genomes
- MAP2:
-
Microtubule-associated protein 2
- miRNA:
-
MicroRNA
- NF-kB:
-
Nuclear factor-kappa B
- OGD:
-
Oxygen–glucose deprivation
- OGD-PBMC:
-
Peripheral blood mononuclear cell preconditioned by oxygen–glucose deprivation
- PBMC:
-
Peripheral blood mononuclear cell
- pNF-kB:
-
Phospho-NF-kB
- RNAseq:
-
RNA sequencing
- ROI:
-
Regions of interest
- rRNA:
-
Ribosomal RNA
- PPARγ:
-
Proliferator-activated receptor gamma
- SD:
-
Standard deviation
- SSEA-3:
-
Stage-specific embryonic antigen 3
- TGF-β:
-
Transforming growth factor-beta
- TNF-α:
-
Tumour necrosis factor-alpha
- TMEM119:
-
Transmembrane protein 119
- VEGF:
-
Vascular endothelial growth factor
- vWF:
-
Von Willebrand factor
References
Gorelick PB. The global burden of stroke: persistent and disabling. Lancet Neurol. 2019;18(5):417–8. https://doi.org/10.1016/S1474-4422(19)30030-4.
GBD 2016 Lifetime Risk of Stroke Collaborators, Feigin VL, Nguyen G, Cercy K, Johnson CO, Alam T, Parmar PG, et al. Global, regional, and country-specific lifetime risks of stroke, 1990 and 2016. N Engl J Med. 2018;379(25):2429–2437. https://doi.org/10.1056/NEJMoa1804492.
Otsu Y, Namekawa M, Toriyabe M, et al. Strategies to prevent hemorrhagic transformation after reperfusion therapies for acute ischemic stroke: a literature review. J Neurol Sci. 2020;419:117217. doi: https://doi.org/10.1016/j.jns.2020.117217.
RESCUE BT Trial Investigators, Qiu Z, Li F, Sang H, et al. Effect of intravenous tirofiban vs placebo before endovascular thrombectomy on functional outcomes in large vessel occlusion stroke: the RESCUE BT randomized clinical trial. JAMA. 2022;328(6):543–553. doi: https://doi.org/10.1001/jama.2022.12584.
MacKenzie IER, Moeini-Naghani I, Sigounas D. Trends in endovascular mechanical thrombectomy in treatment of acute ischemic stroke in the United States. World Neurosurg. 2020;138:e839–46. https://doi.org/10.1016/j.wneu.2020.03.105.
Liu X, Ye R, Yan T, et al. Cell based therapies for ischemic stroke: from basic science to bedside. Prog Neurobiol. 2014;115:92–115. https://doi.org/10.1016/j.pneurobio.2013.11.007.
Park YJ, Niizuma K, Mokin M, Dezawa M, Borlongan CV. Cell-based therapy for stroke: musing with muse cells. Stroke. 2020;51(9):2854–62. https://doi.org/10.1161/STROKEAHA.120.030618.
Kanazawa M, Miura M, Toriyabe M, et al. Microglia preconditioned by oxygen-glucose deprivation promote functional recovery in ischemic rats. Sci Rep. 2017;7(1):42582. https://doi.org/10.1038/srep42582.
Hatakeyama M, Kanazawa M, Ninomiya I, et al. A novel therapeutic approach using peripheral blood mononuclear cells preconditioned by oxygen-glucose deprivation. Sci Rep. 2019;9(1):16819. https://doi.org/10.1038/s41598-019-53418-5.
Jiang C, Wang J, Yu L, et al. Comparison of the therapeutic effects of bone marrow mononuclear cells and microglia for permanent cerebral ischemia. Behav Brain Res. 2013;250:222–9. https://doi.org/10.1016/j.bbr.2013.05.011.
Ukai R, Honmou O, Harada K, et al. Mesenchymal stem cells derived from peripheral blood protects against ischemia. J Neurotrauma. 2007;24(3):508–20. https://doi.org/10.1089/neu.2006.0161.
Kanazawa M, Takahashi T, Ishikawa M, et al. Angiogenesis in the ischemic core: a potential treatment target? J Cereb Blood Flow Metab. 2019;39(5):753–69. https://doi.org/10.1177/0271678X19834158.
Roberts AB, Sporn MB, Assoian RK, et al. Transforming growth factor type beta: rapid induction of fibrosis and angiogenesis in vivo and stimulation of collagen formation in vitro. Proc Natl Acad Sci USA. 1986;83(12):4167–71. https://doi.org/10.1073/pnas.83.12.4167.
Jin K, Mao XO, Greenberg DA. Vascular endothelial growth factor stimulates neurite outgrowth from cerebral cortical neurons via Rho kinase signaling. J Neurobiol. 2006;66(3):236–42. https://doi.org/10.1002/neu.20215.
Yi JJ, Barnes AP, Hand R, Polleux F, Ehlers MD. TGF-beta signaling specifies axons during brain development. Cell. 2010;142(1):144–57. https://doi.org/10.1016/j.cell.2010.06.010.
Hatakeyama M, Ninomiya I, Kanazawa M. Angiogenesis and neuronal remodeling after ischemic stroke. Neural Regen Res. 2020;15(1):16–9. https://doi.org/10.4103/1673-5374.264442.
Hori E, Hayakawa Y, Hayashi T, et al. Mobilization of pluripotent multilineage-differentiating stress-enduring cells in ischemic stroke. J Stroke Cerebrovasc Dis. 2016;25(6):1473–81. https://doi.org/10.1016/j.jstrokecerebrovasdis.2015.12.033.
Kanazawa M, Ninomiya I, Hatakeyama M, Takahashi T, Shimohata T. Microglia and monocytes/macrophages polarization reveal novel therapeutic mechanism against stroke. Int J Mol Sci. 2017;18(10):2135. https://doi.org/10.3390/ijms18102135.
Hatakeyama M, Ninomiya I, Otsu Y, et al. Cell therapies under clinical trials and polarized cell therapies in pre-clinical studies to treat ischemic stroke and neurological diseases: a literature review. Int J Mol Sci. 2020;21(17):6194. https://doi.org/10.3390/ijms21176194.
Lo EH, Ning M. Mechanisms and challenges in translational stroke research. J Investig Med. 2016;64(4):827–9. https://doi.org/10.1136/jim-2016-000104.
Zhang L, Wei W, Ai X, et al. Extracellular vesicles from hypoxia-preconditioned microglia promote angiogenesis and repress apoptosis in stroke mice via the TGF-β/Smad2/3 pathway. Cell Death Dis. 2021;12(11):1068. https://doi.org/10.1038/s41419-021-04363-7.
Zhang ZG, Buller B, Chopp M. Exosomes - beyond stem cells for restorative therapy in stroke and neurological injury. Nat Rev Neurol. 2019;15(4):193–203. https://doi.org/10.1038/s41582-018-0126-4.
Dabrowska S, Andrzejewska A, Strzemecki D, et al. Human bone marrow mesenchymal stem cell-derived extracellular vesicles attenuate neuroinflammation evoked by focal brain injury in rats. J Neuroinflammation. 2019;16(1):216. https://doi.org/10.1186/s12974-019-1602-5.
Dong P, Li Q, Han H. HIF-1α in cerebralischemia (review). Mol Med Rep. 2022;25(2):41. https://doi.org/10.3892/mmr.2021.12557.
Caballero-Garrido E, Pena-Philippides JC, Lordkipanidze T, et al. In vivo inhibition of miR-155 promotes recovery after experimental mouse stroke. J Neurosci. 2015;35(36):12446–64. https://doi.org/10.1523/JNEUROSCI.1641-15.2015.
Ginouvès A, Ilc K, Macías N, et al. PHDs overactivation during chronic hypoxia “desensitizes” HIFalpha and protects cells from necrosis. Proc Natl Acad Sci U S A. 2008;105(12):4745–50. https://doi.org/10.1073/pnas.0705680105.
Song S, Park JT, Na JY, et al. Early expressions of hypoxia-inducible factor 1alpha and vascular endothelial growth factor increase the neuronal plasticity of activated endogenous neural stem cells after focal cerebral ischemia. Neural Regen Res. 2014;9(9):912–8. https://doi.org/10.4103/1673-5374.133136.
Percie du Sert N, Hurst V, Ahluwalia A, et al. The ARRIVE guidelines 2.0: updated guidelines for reporting animal research. J Cereb Blood Flow Metab. 2020;40(9):1769–1777. https://doi.org/10.1177/0271678X20943823.
Milner R, Hung S, Wang X, et al. Responses of endothelial cell and astrocyte matrix-integrin receptors to ischemia mimic those observed in the neurovascular unit. Stroke. 2008;39(1):191–7. https://doi.org/10.1161/STROKEAHA.107.486134.
Kanazawa M, Kawamura K, Takahashi T, Miura M, Tanaka Y, Koyama M, et al. Multiple therapeutic effects of progranulin on experimental acute ischaemic stroke. Brain. 2015;138(Pt 7):1932–48. https://doi.org/10.1093/brain/awv079.
Dobin A, Davis CA, Schlesinger F, et al. STAR: ultrafast universal RNA-seq aligner. Bioinformatics. 2013;29(1):15–21. https://doi.org/10.1093/bioinformatics/bts635.
Trapnell C, Roberts A, Goff L, et al. Differential gene and transcript expression analysis of RNA-seq experiments with TopHat and Cufflinks. Nat Protoc. 2012;7(3):562–78. https://doi.org/10.1038/nprot.2012.016.
Falcon S, Gentleman R. Using GOstats to test gene lists for GO term association. Bioinformatics. 2007;23(2):257–8. https://doi.org/10.1093/bioinformatics/btl567.
Ritchie ME, Phipson B, Wu D, et al. limma powers differential expression analyses for RNA-sequencing and microarray studies. Nucleic Acids Res. 2015;43(7):e47. https://doi.org/10.1093/nar/gkv007.
Oosterhof N, Holtman IR, Kuil LE, et al. Identification of a conserved and acute neurodegeneration-specific microglial transcriptome in the zebrafish. Glia. 2017;65(1):138–49. https://doi.org/10.1002/glia.23083.
Matsuura Y, Wada H, Eguchi H, et al. Exosomal miR-155 derived from hepatocellular carcinoma cells under hypoxia promotes angiogenesis in endothelial cells. Dig Dis Sci. 2019;64(3):792–802. https://doi.org/10.1007/s10620-018-5380-1.
Nakai W, Yoshida T, Diez D, et al. A novel affinity-based method for the isolation of highly purified extracellular vesicles. Sci Rep. 2016;6:33935. https://doi.org/10.1038/srep33935.
Kanazawa M, Kakita A, Igarashi H, et al. Biochemical and histopathological alterations in TAR DNA-binding protein-43 after acute ischemic stroke in rats. J Neurochem. 2011;116(6):957–65. https://doi.org/10.1111/j.1471-4159.2010.06860.x.
Kanazawa M, Igarashi H, Kawamura K, et al. Inhibition of VEGF signaling pathway attenuates hemorrhage after tPA treatment. J Cereb Blood Flow Metab. 2011;31(6):1461–74. https://doi.org/10.1038/jcbfm.2011.9.
Balkaya M, Kröber J, Gertz K, Peruzzaro S, Endres M. Characterization of long-term functional outcome in a murine model of mild brain ischemia. J Neurosci Methods. 2013;213(2):179–87. https://doi.org/10.1016/j.jneumeth.2012.12.021.
Wang R, Liu Y, Ye Q, et al. RNA sequencing reveals novel macrophage transcriptome favoring neurovascular plasticity after ischemic stroke. J Cereb Blood Flow Metab. 2020;40(4):720–38. https://doi.org/10.1177/0271678X19888630.
Freytes DO, Kang JW, Marcos-Campos I, Vunjak-Novakovic G. Macrophages modulate the viability and growth of human mesenchymal stem cells. J Cell Biochem. 2013;114(1):220–9. https://doi.org/10.1002/jcb.24357.
Bennett ML, Bennett FC, Liddelow SA, et al. New tools for studying microglia in the mouse and human CNS. Proc Natl Acad Sci USA. 2016;113(12):E1738-1746. https://doi.org/10.1073/pnas.1525528113.
Clevers H. Wnt/beta-catenin signaling in development and disease. Cell. 2006;127(3):469–80. https://doi.org/10.1016/j.cell.2006.10.018.
Jain AK, Barton MC. p53: emerging roles in stem cells, development and beyond. Development. 2018;145(8):dev158360. doi: https://doi.org/10.1242/dev.158360.
Wu C, Chen J, Chen C, et al. Wnt/β-catenin coupled with HIF-1α/VEGF signaling pathways involved in galangin neurovascular unit protection from focal cerebral ischemia. Sci Rep. 2015;5:16151. https://doi.org/10.1038/srep16151.
Reya T, Duncan AW, Ailles L, et al. A role for Wnt signalling in self-renewal of haematopoietic stem cells. Nature. 2003;423(6938):409–14. https://doi.org/10.1038/nature01593.
Ransohoff RM. A polarizing question: do M1 and M2 microglia exist? Nat Neurosci. 2016;19(8):987–91. https://doi.org/10.1038/nn.4338.
Masuda T, Sankowski R, Staszewski O, et al. Spatial and temporal heterogeneity of mouse and human microglia at single-cell resolution. Nature. 2019;566(7744):388–92. https://doi.org/10.1038/s41586-019-0924-x.
Arderiu G, Peña E, Aledo R, et al. MicroRNA-145 regulates the differentiation of adipose stem cells toward microvascular endothelial cells and promotes angiogenesis. Circ Res. 2019;125(1):74–89. https://doi.org/10.1161/CIRCRESAHA.118.314290.
Kurtzwald-Josefson E, Zeevi-Levin N, Rubchevsky V, et al. Cardiac fibroblast-induced pluripotent stem cell-derived exosomes as a potential therapeutic mean for heart failure. Int J Mol Sci. 2020;21(19):7215. https://doi.org/10.3390/ijms21197215.
Hong Y, He H, Jiang G, et al. miR-155–5p inhibition rejuvenates aged mesenchymal stem cells and enhances cardioprotection following infarction. Aging Cell. 2020;19(4):e13128. https://doi.org/10.1111/acel.13128.
O’Connell RM, Rao DS, Chaudhuri AA, et al. Sustained expression of microRNA-155 in hematopoietic stem cells causes a myeloproliferative disorder. J Exp Med. 2008;205(3):585–94. https://doi.org/10.1084/jem.20072108.
Hornick NI, Doron B, Abdelhamed S, et al. AML suppresses hematopoiesis by releasing exosomes that contain microRNAs targeting c-MYB. Sci Signal. 2016;9(444):ra88. https://doi.org/10.1126/scisignal.aaf2797.
Bruning U, Cerone L, Neufeld Z, et al. MicroRNA-155 promotes resolution of hypoxia-inducible factor 1alpha activity during prolonged hypoxia. Mol Cell Biol. 2011;31(19):4087–96. https://doi.org/10.1128/MCB.01276-10.
Wang J, Zou Y, Du B, et al. SNP-mediated lncRNA-ENTPD3-AS1 upregulation suppresses renal cell carcinoma via miR-155/HIF-1α signaling. Cell Death Dis. 2021;12(7):672. https://doi.org/10.1038/s41419-021-03958-4.
Bacigaluppi M, Pluchino S, Peruzzotti-Jametti L, et al. Delayed post-ischaemic neuroprotection following systemic neural stem cell transplantation involves multiple mechanisms. Brain. 2009;132(Pt 8):2239–51. https://doi.org/10.1093/brain/awp174.
van Velthoven CT, Kavelaars A, van Bel F, Heijnen CJ. Mesenchymal stem cell transplantation changes the gene expression profile of the neonatal ischemic brain. Brain Behav Immun. 2011;25(7):1342–8. https://doi.org/10.1016/j.bbi.2011.03.021.
Froger N, Matonti F, Roubeix C, et al. VEGF is an autocrine/paracrine neuroprotective factor for injured retinal ganglion neurons. Sci Rep. 2020;10(1):12409. https://doi.org/10.1038/s41598-020-68488-z.
Ogunshola OO, Antic A, Donoghue MJ, et al. Paracrine and autocrine functions of neuronal vascular endothelial growth factor (VEGF) in the central nervous system. J Biol Chem. 2002;277(13):11410–5. https://doi.org/10.1074/jbc.M111085200.
Uchida H, Niizuma K, Kushida Y, et al. Human muse cells reconstruct neuronal circuitry in subacute lacunar stroke model. Stroke. 2017;48(2):428–35. https://doi.org/10.1161/STROKEAHA.116.014950.
Närvä E, Pursiheimo JP, Laiho A, et al. Continuous hypoxic culturing of human embryonic stem cells enhances SSEA-3 and MYC levels. PLoS One. 2013;8(11):e78847. https://doi.org/10.1371/journal.pone.0078847.
Cui P, Zhang P, Zhang Y, et al. HIF-1α/Actl6a/H3K9ac axis is critical for pluripotency and lineage differentiation of human induced pluripotent stem cells. FASEB J. 2020;34(4):5740–53. https://doi.org/10.1096/fj.201902829RR.
Takubo K, Goda N, Yamada W, et al. Regulation of the HIF-1alpha level is essential for hematopoietic stem cells. Cell Stem Cell. 2010;7(3):391–402. https://doi.org/10.1016/j.stem.2010.06.020.
Shyh-Chang N, Daley GQ, Cantley LC. Stem cell metabolism in tissue development and aging. Development. 2013;140(12):2535–47. https://doi.org/10.1242/dev.091777.
Weinberger L, Ayyash M, Novershtern N, Hanna JH. Dynamic stem cell states: naive to primed pluripotency in rodents and humans. Nat Rev Mol Cell Biol. 2016;17(3):155–69. https://doi.org/10.1038/nrm.2015.28.
Carmichael ST, Kathirvelu B, Schweppe CA, Nie EH. Molecular, cellular and functional events in axonal sprouting after stroke. Exp Neurol. 2017;287(Pt 3):384–94. https://doi.org/10.1016/j.expneurol.2016.02.007.
Jin K, Wang X, Xie L, et al. Evidence for stroke-induced neurogenesis in the human brain. Proc Natl Acad Sci USA. 2006;103(35):13198–202. https://doi.org/10.1073/pnas.0603512103.
Srivastava D, DeWitt N. In vivo cellular reprogramming: the next generation. Cell. 2016;166(6):1386–96. https://doi.org/10.1016/j.cell.2016.08.055.
Funding
This work was supported by a Grant-in-Aid for Scientific Research (Research Project Number: 18K07493, 21K19441, 22H03183), the Translational Research program, Strategic Promotion for practical application of Innovative Medical Technology (TR-SPRINT) supported by the Japan Agency for Medical Research and Development (AMED) under Grant Number JP19lm0203023, a grant from Takeda Science Foundation and SENSHIN Medical Research Foundation, and Moriyama Award of Japan Brain Foundation (Dr. Kanazawa). This work was also supported by a Grant-in-Aid for Scientific Research (Research Project Number: 20K16485) (Dr. Hatakeyama) and a grant from the Tsubaki Memorial Foundation (Dr. Otsu).
Author information
Authors and Affiliations
Contributions
Y.O. and M. H. performed the experiments, analysed the data, and drafted the manuscript. T.K., N. A., and I.N. performed the experiments and analysed the data. T.K. and O.O. advised experiments. K.O., M.F., and T.S. analysed the data and supervised all aspects of this project. M. K. performed the experiments, analysed the data, developed the concept, designed the experiments, wrote the manuscript, and supervised all aspects of this project. All authors have read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethical Approval and Consent to Participate
This study was conducted in strict accordance with the recommendations of the Guide for the Care and Use of Laboratory Animals of the National Institutes of Health (Bethesda, MD). The protocol (#SA00706) was approved by the Niigata University Administrative Panel on Laboratory Animal Care and the Ethical Committee of Niigata University. Ethical approval for the present study (#2019–0374) was provided by the Institutional Ethics Committee of Niigata University Medical and Dental Hospital. Informed consent was obtained healthy donors.
Consent for Publication
We have obtained consent to publish from the participant to report individual data.
Conflict of Interests
Prof. Shimohata is an academic advisor, Shimojani LLC. The authors declare no financial interests related to the materials in this manuscript. Drs. Otsu, Hatakeyama, Kanayama, Akiyama, Ninomiya, Omae, Kato, Onodera, Fukushima, and Kanazawa declare no competing interests.
Required Author Forms
Disclosure forms provided by the authors are available with the online version of this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Otsu, Y., Hatakeyama, M., Kanayama, T. et al. Oxygen–Glucose Deprived Peripheral Blood Mononuclear Cells Protect Against Ischemic Stroke. Neurotherapeutics 20, 1369–1387 (2023). https://doi.org/10.1007/s13311-023-01398-w
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13311-023-01398-w