Abstract
Background
Predicting spontaneous preterm birth (SPTB) during mid-trimester would be very useful. We used a multimodality screening approach mainly focusing on urogenital infections among unselected obstetric population between 18 and 24 weeks in a tertiary center.
Method
Diagnosis of lower genital tract infection (LGTI) was attempted among 228 pregnant women using several factors—symptom of vaginal discharge, characteristic appearance of discharge on speculum, point of care tests using Amsel’s criteria and gram staining of vaginal swab. Nugent’s scoring was taken as gold standard. Urine microscopy/culture was obtained. Serum inflammatory markers were done. Total leukocyte count, neutrophil/lymphocyte ratio and C-reactive protein were obtained. Data on cervical length were obtained from mid-trimester scan.
Results
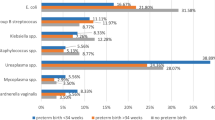
Thirty patients complained of vaginal discharge. Speculum examination revealed discharge in 221 (96.92%), appearing pathological in 192 (86.87%). Amsel’s criteria showed poor sensitivity to detect full (57%) and partial (24%) bacterial vaginosis (BV). On gram staining, 104 (45.61%) showed evidence of LGTI; 14 full BV (6.1%); 45 partial BV (19.5%); 40 candidiasis (17.5%); and two each of trichomoniasis and aerobic vaginitis. Appearance of vaginal discharge and microscopic diagnosis of LGTI were poorly correlated. Forty women (17.5%) had SPTB, 24 following membrane rupture and 16 following spontaneous labor. The presence of BV (specifically partial) increased the likelihood of SPTB with OR of 3.347 (CI 1.642, 6.823). Three of seven women with short cervix delivered preterm. No other screening modality was associated with SPTB.
Conclusion
Active screening for LGTI between 18 and 24 weeks shows high prevalence of BV in Indian setting. There is a strong link between partial BV and SPTB.

Similar content being viewed by others
References
Georgiou HM, Di Quinzio MKW, Permezel M, Brennecke SP. Predicting preterm labour: current status and future prospects. Dis Markers. 2015. https://doi.org/10.1155/2015/435014.
Blencowe H, Cousens S, Oestergaard MZ, Chou D, Moller AB, Narwal R, Adler A, Vera Garcia C, Rohde S, Say L, Lawn JE. National, regional, and worldwide estimates of preterm birth rates in the year 2010 with time trends since 1990 for selected countries: a systematic analysis and implications. Lancet. 2012;379:2162–72.
Lamont RF. Antibiotics to prevent preterm birth. In: Keelan JA, Newnham JP, editors. Advances in the prevention and treatment of inflammation-associated preterm birth, Frontiers Media SA; 2016. p. 79–87.
Nwankwo TO, Aniebue UU, Umeh UA. Syndromic diagnosis in evaluation of women with symptoms of vaginitis. Curr Infect Dis Rep. 2017. https://doi.org/10.1007/s11908-017-0558-9.
Kim M-A, Lee YS, Seo K, Kallapur SG. Assessment of predictive markers for placental inflammatory response in preterm births. PLoS ONE. 2014;9(10):e107880.
Mengistie Z, Woldeamanuel Y, Asrat D, Adera A. Prevalence of bacterial vaginosis among pregnant women attending antenatal care in Tikur Anbessa University Hospital, Addis Ababa, Ethiopia. BMC Res Notes. 2014;20(7):822. https://doi.org/10.1186/1756-0500-7-822.
Mohammadzadeh F, Dolatian M, Jorjani M, Majd HA. Diagnostic value of Amsel’s clinical criteria for diagnosis of bacterial vaginosis. Glob J Health Sci. 2015;7(3):8–14.
Mengistie Z, Woldeamanuel Y, Asrat D, Yigeremu M. Comparison of clinical and gram stain diagnosis methods of bacterial vaginosis among pregnant women in Ethiopia. J Clin Diagn Res. 2013;7(12):2701–3.
Witkin SS. Limitations of treating pregnant women based solely on vaginal pH. British J Obstet Gynecol. 2018;125(12):1610. https://doi.org/10.1111/1471-0528.15281.
Hoffman MK, Bellad MB, Charantimath US, et al. A comparison of colorimetric assessment of vaginal ph with Nugent score for the detection of bacterial vaginosis. Infect Dis Obstet Gynecol. 2017. https://doi.org/10.1155/2017/1040984.
Zemouri C, Wi TE, Kiarie J, Seuc A, Mogasale V, Latif A, Broutet N. The performance of the vaginal discharge syndromic management in treating vaginal and cervical infection: a systematic review and meta-analysis. PLoS ONE. 2016;11(10):e0163365.
Lima TM, Teles LR, de Oliveira A, Campos FC, Barbosa RD, Pinheiro AK, et al. Vaginal discharge in pregnant women: comparison between syndromic approach and examination of clinical nurs- ing practice. Rev Esc Enferm USP. 2013;47(6):1265–71. https://doi.org/10.1590/S0080-623420130000600002.
Gupta A, Garg P, Nigam S. Bacterial vaginosis in pregnancy (< 28 weeks) and its effect on pregnancy outcome: a study from a western up city. Indian J Clin Pract. 2013;23(11):740–4.
Tellapragada C, Vandana KE, Bhat PV, Rao C, Kamath A, Nayak S, Shashidhar V, Acharya S, Mukhopadhyay C. Lower genital tract infections during pregnancy and adverse pregnancy outcomes: a hospital-based observational cohort study. BMC Infect Dis. 2014;14(Suppl 3):E35.
Tellapragada C, Eshwara VK, Bhat P, Kamath A, Aletty S, Mukhopadhyay C. Screening of vulvovaginal infections during pregnancy in resource constrained settings: implications on preterm delivery. J Infect Public Health. 2017;10(4):431–7. https://doi.org/10.1016/j.jiph.2016.06.003.
Abdelaziz ZA, Ibrahim ME, Bilal NE, Hamid ME. Vaginal infections among pregnant women at Omdurman Maternity Hospital in Khartoum. Sudan. J Infect Dev Ctries. 2014;8(4):490–7. https://doi.org/10.3855/jidc.3197.
Krauss-Silva L, Almada-Horta A, Alves MB, Camacho KG, Moreira ME, Braga A. Basic vaginal pH, bacterial vaginosis and aerobic vaginitis: prevalence in early pregnancy and risk of spontaneous preterm delivery, a prospective study in a low socioeconomic and multiethnic South American population. BMC Pregnancy Childbirth. 2014;14:107. https://doi.org/10.1186/1471-2393-14-107.
Christine CA, Eva KP, Elizabeth C, Ruth AQ, Julie P, Kimberly O. Prevalence and risk factors for infections in a pregnant adolescent population. J Pediatr Adolesc Gynecol. 2017;30(1):71–5.
Farr A, Kiss H, Holzer I, Husslein P, Hagmann M, Petricevic L. Effect of asymptomatic vaginal colonization with Candida albicans on pregnancy outcome. Acta Obstet Gynecol Scand. 2015;94(9):989–96. https://doi.org/10.1111/aogs.12697.
Bretelle F, Rozenberg P, Pascal A, Favre R, Bohec C, Loundou A, et al. High Atopobium vaginae and Gardnerella vaginalis vaginal loads are associated with preterm birth. Clin Infect Dis. 2015;60(6):860–7. https://doi.org/10.1093/cid/ciu966.
Farr A, Kiss H, Hagmann M, Marschalek J, Husslein P, Petricevic L. Routine use of an antenatal infection screen-and-treat program to prevent preterm birth: long-term experience at a tertiary referral center. Birth. 2015;42(2):173–80. https://doi.org/10.1111/birt.12154.
Roberts CL, Algert CS, Rickard KL, Morris JM. Treatment of vaginal candidiasis for the prevention of preterm birth: a systematic review and meta-analysis. Syst Rev. 2015;4:31. https://doi.org/10.1186/s13643-015-0018-2.
Folger AT. Maternal Chlamydia trachomatis infections and preterm birth: the impact of early detection and eradication during pregnancy. Matern Child Health J. 2014;18(8):1795–802. https://doi.org/10.1007/s10995-013-1423-6.
Sangkomkamhang US, Lumbiganon P, Prasertcharoensuk W, Laopaiboon M. Antenatal lower genital tract infection screening and treatment programs for preventing preterm delivery. Cochrane Database Syst Rev. 2015;1(2):CD006178. https://doi.org/10.1002/14651858.cd006178.pub3.
Brabant G. Bacterial vaginosis and spontaneous preterm birth. J Gynecol Obstet Biol Reprod (Paris). 2016;45(10):1247–60. https://doi.org/10.1016/j.jgyn.2016.09.014.
Haahr T, Ersboll AS, Karlsen MA, Svare J, Sneider K, Hee L, Weile LK, et al. Treatment of bacterial vaginosis in pregnancy in order to reduce the risk of spontaneous preterm delivery—a clinical recommendation. Acta Obstet Gynecol Scand. 2016;95(8):850–60. https://doi.org/10.1111/aogs.12933.
Laura MJ. Bacterial Vaginosis and Preterm Birth. J Midwifery womens health. 2011;15(6):575–83. https://doi.org/10.1111/j.1542-2011.2011.00086.x.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Vidyashree Ganesh Poojari, Samantha Dawson, Akhila Vasudeva, Nivedita Hegde, Geetha Kaipa, Vandana Eshwara, Chaitanya Tellapragada, and Pratap Kumar declare that they have no conflict of interest.
Ethical Statement
Kasturba Medical College and Kasturba Hospital, Manipal—Institutional ethics committee clearance obtained (IEC Number–403/2015)
Informed Consent
An informed consent was obtained from all patients for being included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Vidyashree Ganesh Poojari is an Associate Professor in Department of Obstetrics and Gynecology at Kasturba Medical College, MAHE, Manipal, Karnataka, India. Samantha Dawson is an Junior Resident in Department of Obstetrics and Gynecology at Kasturba Medical College, MAHE, Manipal, Karnataka, India. Akhila Vasudeva is an Professor in Department of Obstetrics and Gynecology at Kasturba Medical College, MAHE, Manipal, Karnataka, India. Nivedita Hegde is an Assistant Professor in Department of Obstetrics and Gynecology at Kasturba Medical College, MAHE, Manipal, Karnataka, India. Geetha Kaipa is an Junior Resident in Department of Microbiology at Kasturba Medical College, MAHE, Manipal, Karnataka, India. Vandana Eshwara is an Professor in Department of Microbiology at Kasturba Medical College, MAHE, Manipal, Karnataka, India. Chaitanya Tellapragada is an Post Doctorate, Department of Laboratory, Medicine, Karolinska institute, Sweden. Pratap Kumar is an Professor in Department of Obstetrics and Gynecology at Kasturba Medical College, MAHE, Manipal, Karnataka, India.
Rights and permissions
About this article
Cite this article
Poojari, V.G., Dawson, S., Vasudeva, A. et al. Multimodality Screening for Lower Genital Tract Infections Between 18 and 24 Weeks of Pregnancy and its Efficacy in Predicting Spontaneous Preterm Delivery. J Obstet Gynecol India 70, 36–43 (2020). https://doi.org/10.1007/s13224-019-01287-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13224-019-01287-3