Abstract
Gestational diabetes mellitus (GDM) is a metabolic disorder, characterized by underlying glucose intolerance, diabetes onset or first diagnosis during pregnancy. Galactooligosaccharide (GOS) is essential for consumer protection as food supplementation. However, there is limited understanding of the effects of GOS on GDM. We successfully established a GDM rat model to explore GOS whether participated in PPARs/PI3K/Akt pathway and gut microbiota metabolites to treat for GDM. In this study, compared with the GDM group, GOS administration lowered the levels of TG, LDL-C, and HDL-C in rat serum, as well as improved the pathological changes pancreatic, liver, and kidney tissues. Compared with the GDM group, the protein expressions of PPARα, PPARγ, and PPARβ/δ markedly enhanced in GOS-treated groups (P < 0.01). Moreover, GOS administration upregulated the protein expressions of PPARα, PPARβ, PPARγ, PI3K, Akt, GLUT4, Bax, and Bcl2. GOS administration altered gut microbiota metabolites, including both SCFAs and BAs. Correlation analysis revealed close relationships between gut microbiota and experimental indicators. This study indicated that GOS effectively improved GDM in rats through the modulation of PPARs/PI3K/Akt pathway and gut microbiota. Thus, the GOS could be recommended as a candidate for novel therapy of GDM.
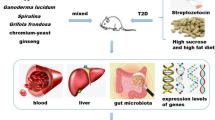
Graphical Abstract










Similar content being viewed by others
Data Availability
All data generated or analyzed during this study are available from the corresponding author on reasonable request.
References
Metzger BE, Lowe LP, Dyer AR, Trimble ER, Chaovarindr U, Coustan DR, Hadden DR, McCance DR, Hod M, McIntyre HD et al (2008) Hyperglycemia and adverse pregnancy outcomes. N Engl J Med 358:1991–2002. https://doi.org/10.1056/NEJMoa0707943
Yew TW, Chi C, Chan SY, van Dam RM, Whitton C, Lim CS, Foong PS, Fransisca W, Teoh CL, Chen J et al (2021) A randomized controlled trial to evaluate the effects of a smartphone application-based lifestyle coaching program on gestational weight gain, glycemic control, and maternal and neonatal outcomes in women with gestational diabetes mellitus: The SMART-GDM Study. Diabetes Care 44:456–463. https://doi.org/10.2337/dc20-1216
Song XL, Shu J, Zhang SM, Chen LT, Diao J, Li JQ, Li YH, Wei JH, Liu YP, Sun MT et al (2022) Pre-pregnancy body mass index and risk of macrosomia and large for gestational age births with gestational diabetes mellitus as a mediator: A prospective cohort study in central China. Nutrients 14. https://doi.org/10.3390/nu14051072
Yong HY, Mohd Shariff Z, Mohd Yusof BN, Rejali Z, Tee YYS, Bindels J, van der Beek EM (2020) Independent and combined effects of age, body mass index and gestational weight gain on the risk of gestational diabetes mellitus. Sci Rep 10:8486. https://doi.org/10.1038/s41598-020-65251-2
Song C, Lyu Y, Li C, Liu P, Li J, Ma RC, Yang X (2018) Long-term risk of diabetes in women at varying durations after gestational diabetes: a systematic review and meta-analysis with more than 2 million women. Obes Rev 19:421–429. https://doi.org/10.1111/obr.12645
Vounzoulaki E, Khunti K, Abner SC, Tan BK, Davies MJ, Gillies CL (2020) Progression to type 2 diabetes in women with a known history of gestational diabetes: systematic review and meta-analysis. BMJ (Clin Res Ed) 369:m1361. https://doi.org/10.1136/bmj.m1361
Cooray SD, Boyle JA, Soldatos G, Allotey J, Wang H, Fernandez-Felix BM, Zamora J, Thangaratinam S, Teede HJ (2022) Development, validation and clinical utility of a risk prediction model for adverse pregnancy outcomes in women with gestational diabetes: The PeRSonal GDM model. EClinicalMedicine 52:101637. https://doi.org/10.1016/j.eclinm.2022.101637
McIntyre HD, Catalano P, Zhang C, Desoye G, Mathiesen ER, Damm P (2019) Gestational diabetes mellitus. Nat Rev Dis Primers 5:47. https://doi.org/10.1038/s41572-019-0098-8
Most J, Broskey NT, Altazan AD, Beyl RA, St Amant M, Hsia DS, Ravussin E, Redman LM (2019) Is energy balance in pregnancy involved in the etiology of gestational diabetes in women with obesity? Cell Metab 29:231–233. https://doi.org/10.1016/j.cmet.2018.12.002
Ghomian N, Vahed SHM, Firouz S, Yaghoubi MA, Mohebbi M, Sahebkar A (2019) The efficacy of metformin compared with insulin in regulating blood glucose levels during gestational diabetes mellitus: A randomized clinical trial. J Cell Physiol 234:4695–4701. https://doi.org/10.1002/jcp.27238
Crusell MKW, Hansen TH, Nielsen T, Allin KH, Rühlemann MC, Damm P, Vestergaard H, Rørbye C, Jørgensen NR, Christiansen OB et al (2018) Gestational diabetes is associated with change in the gut microbiota composition in third trimester of pregnancy and postpartum. Microbiome 6:89. https://doi.org/10.1186/s40168-018-0472-x
Liu J, Yang H, Yin Z, Jiang X, Zhong H, Qiu D, Zhu F, Li R (2017) Remodeling of the gut microbiota and structural shifts in Preeclampsia patients in South China. Eur J Clin Microbiol Infect Dis 36:713–719. https://doi.org/10.1007/s10096-016-2853-z
Tsai HJ, Hung WC, Hung WW, Lee YJ, Chen YC, Lee CY, Tsai YC, Dai CY (2023) Circulating short-chain fatty acids and non-alcoholic fatty liver disease severity in patients with type 2 diabetes mellitus. Nutrients 15. https://doi.org/10.3390/nu15071712
Liu H, Pan LL, Lv S, Yang Q, Zhang H, Chen W, Lv Z, Sun J (2019) Alterations of gut microbiota and blood lipidome in gestational diabetes mellitus with hyperlipidemia. Front Physiol 10:1015. https://doi.org/10.3389/fphys.2019.01015
Ahmad TR, Haeusler RA (2019) Bile acids in glucose metabolism and insulin signalling - mechanisms and research needs. Nat Rev Endocrinol 15:701–712. https://doi.org/10.1038/s41574-019-0266-7
Song XY, Wang HJ, Su C, Wang ZH, Du WW, Huang FF, Zhang JG, Jia XF, Jiang HR, Ouyang YF et al (2021) Trajectories of energy intake distribution and risk of dyslipidemia: Findings from the China health and nutrition survey (1991–2018). Nutrients 13. https://doi.org/10.3390/nu13103488
Fan HM, Mitchell AL, Williamson C (2021) Endocrinology in pregnancy: Metabolic impact of bile acids in gestation. Eur J Endocrinol 184:R69–r83. https://doi.org/10.1530/eje-20-1101
Liu H, Wang J, He T, Becker S, Zhang GL, Li DF, Ma X (2018) Butyrate: A double-edged sword for health? Adv Nutr 9:21–29. https://doi.org/10.1093/advances/nmx009
Zhu JX, Wu MR, Zhou H, Cheng LZ, Wei XL, Wang YF (2021) Liubao brick tea activates the PI3K-Akt signaling pathway to lower blood glucose, metabolic disorders and insulin resistance via altering the intestinal flora. Food Res Int 148:110594. https://doi.org/10.1016/j.foodres.2021.110594
Wu QQ, Deng W, Xiao Y, Chen JJ, Liu C, Wang J, Guo Y, Duan M, Cai Z, Xie S et al (2019) The 5-lipoxygenase inhibitor zileuton protects pressure overload-induced cardiac remodeling via activating PPARα. Oxid Med Cell Longev 2019:7536803. https://doi.org/10.1155/2019/7536803
Mao Y, Han CY, Hao L, Bang IH, Bae EJ, Park BH (2021) p21-activated kinase 4 phosphorylates peroxisome proliferator-activated receptor Υ and suppresses skeletal muscle regeneration. J Cachexia Sarcopenia Muscle 12:1776–1788. https://doi.org/10.1002/jcsm.12774
Marco ML, Sanders ME, Gänzle M, Arrieta MC, Cotter PD, De Vuyst L, Hill C, Holzapfel W, Lebeer S, Merenstein D et al (2021) The International Scientific Association for Probiotics and Prebiotics (ISAPP) consensus statement on fermented foods. Nat Rev Gastroenterol Hepatol 18:196–208. https://doi.org/10.1038/s41575-020-00390-5
Ghosh SS, Wang J, Yannie PJ, Sandhu YK, Korzun WJ, Ghosh S (2020) Dietary supplementation with galactooligosaccharides attenuates high-fat, high-cholesterol diet-induced glucose intolerance and disruption of colonic mucin layer in C57BL/6 mice and reduces atherosclerosis in Ldlr-/- mice. J Nutr 150:285–293. https://doi.org/10.1093/jn/nxz233
Chen QC, Liu M, Zhang PY, Fan SJ, Huang JL, Yu SY, Zhang CH, Li HJ (2019) Fucoidan and galactooligosaccharides ameliorate high-fat diet-induced dyslipidemia in rats by modulating the gut microbiota and bile acid metabolism. Nutrition 65:50–59. https://doi.org/10.1016/j.nut.2019.03.001
Sergeev IN, Aljutaily T, Walton G, Huarte E (2020) Effects of synbiotic supplement on human gut microbiota, body composition and weight loss in obesity. Nutrients 12. https://doi.org/10.3390/nu12010222
Taylor AM, Holscher HD (2020) A review of dietary and microbial connections to depression, anxiety, and stress. Nutr Neurosci 23:237–250. https://doi.org/10.1080/1028415x.2018.1493808
Chen C, Wang LL, Lu YQ, Yu HY, Tian HX (2019) Comparative transcriptional analysis of lactobacillus plantarum and Its ccpA-knockout mutant under galactooligosaccharides and glucose conditions. Front Microbiol 10:1584. https://doi.org/10.3389/fmicb.2019.01584
Ai J, Bao B, Battino M, Giampieri F, Chen C, You LJ, Cespedes-Acuña CL, Ognyanov M, Tian LM, Bai WB (2021) Recent advances on bioactive polysaccharides from mulberry. Food Funct 12:5219–5235. https://doi.org/10.1039/d1fo00682g
Bhargava P, Smith MD, Mische L, Harrington E, Fitzgerald KC, Martin K, Kim S, Reyes AA, Gonzalez-Cardona J, Volsko C et al (2020) Bile acid metabolism is altered in multiple sclerosis and supplementation ameliorates neuroinflammation. J Clin Invest 130:3467–3482. https://doi.org/10.1172/jci129401
Yuan YF, Kong F, Xu HW, Zhu AQ, Yan N, Yan CY (2022) Cryo-EM structure of human glucose transporter GLUT4. Nat Commun 13:2671. https://doi.org/10.1038/s41467-022-30235-5
Tufiño C, Vanegas M, Velázquez Nevárez R, Villanueva López C, Bobadilla Lugo RA (2021) Divergent impact of gestational diabetes mellitus between the thoracic and abdominal rat aorta: Influence of endothelium and angiotensin II receptors. Eur J Pharmacol 899:173981. https://doi.org/10.1016/j.ejphar.2021.173981
Krumbeck JA, Rasmussen HE, Hutkins RW, Clarke J, Shawron K, Keshavarzian A, Walter J (2018) Probiotic Bifidobacterium strains and galactooligosaccharides improve intestinal barrier function in obese adults but show no synergism when used together as synbiotics. Microbiome 6:121. https://doi.org/10.1186/s40168-018-0494-4
Alshahrani S, Anwer T, Alam MF, Ahmed RA, Khan G, Sivakumar SM, Shoaib A, Alam P, Azam F (2021) Effect of thymoquinone on high fat diet and STZ-induced experimental type 2 diabetes: A mechanistic insight by in vivo and in silico studies. J Food Biochem. https://doi.org/10.1111/jfbc.13807:e13807.10.1111/jfbc.13807
Arck P, Toth B, Pestka A, Jeschke U (2010) Nuclear receptors of the peroxisome proliferator-activated receptor (PPAR) family in gestational diabetes: from animal models to clinical trials. Biol Reprod 83:168–176. https://doi.org/10.1095/biolreprod.110.083550
Capobianco E, Martínez N, Fornes D, Higa R, Di Marco I, Basualdo MN, Faingold MC, Jawerbaum A (2013) PPAR activation as a regulator of lipid metabolism, nitric oxide production and lipid peroxidation in the placenta from type 2 diabetic patients. Mol Cell Endocrinol 377:7–15. https://doi.org/10.1016/j.mce.2013.06.027
Lee MY, Lee YJ, Kim YH, Lee SH, Park JH, Kim MO, Suh HN, Ryu JM, Yun SP, Jang MW et al (2009) Role of peroxisome proliferator-activated receptor (PPAR)δ in embryonic stem cell proliferation. Int J Stem Cells 2:28–34. https://doi.org/10.15283/ijsc.2009.2.1.28
Aye IL, Rosario FJ, Powell TL, Jansson T (2015) Adiponectin supplementation in pregnant mice prevents the adverse effects of maternal obesity on placental function and fetal growth. Proc Natl Acad Sci USA 112:12858–12863. https://doi.org/10.1073/pnas.1515484112
Roberti SL, Higa R, White V, Powell TL, Jansson T, Jawerbaum A (2018) Critical role of mTOR, PPARγ and PPARδ signaling in regulating early pregnancy decidual function, embryo viability and feto-placental growth. Mol Hum Reprod 24:327–340. https://doi.org/10.1093/molehr/gay013
Zhou J, Zhe RL, Guo XH, Chen YY, Zou Y, Zhou L, Wang ZJ (2020) The role of PPARδ agosnist GW501516 in rats with gestational diabetes mellitus. Diabetes Metab Syndr Obes 13:2307–2316. https://doi.org/10.2147/dmso.s251491
Doktorova M, Zwarts I, Zutphen TV, Dijk THV, Bloks VW, Harkema L, Bruin A, Downes M, Evans RM, Verkade HJ et al (2017) Intestinal PPARδ protects against diet-induced obesity, insulin resistance and dyslipidemia. Sci Rep 7:846. https://doi.org/10.1038/s41598-017-00889-z
Lee EK, Lee MJ, Abdelmohsen K, Kim W, Kim MM, Srikantan S, Martindale JL, Hutchison ER, Kim HH, Marasa BS et al (2011) miR-130 suppresses adipogenesis by inhibiting peroxisome proliferator-activated receptor gamma expression. Mol Cell Biol 31:626–638. https://doi.org/10.1128/mcb.00894-10
Choi JH, Banks AS, Kamenecka TM, Busby SA, Chalmers MJ, Kumar N, Kuruvilla DS, Shin Y, He Y, Bruning JB et al (2011) Antidiabetic actions of a non-agonist PPARγ ligand blocking Cdk5-mediated phosphorylation. Nature 477:477–481. https://doi.org/10.1038/nature10383
Gorowska-Wojtowicz E, Duliban M, Kotula-Balak M, Bilinska B (2022) Modulatory effects of estradiol and its mixtures with ligands of GPER and PPAR on MAPK and PI3K/Akt signaling pathways and tumorigenic factors in mouse testis explants and mouse tumor leydig cells. Biomedicines 10. https://doi.org/10.3390/biomedicines10061390
Lee CC, Huang CC, Hsu KS (2011) Insulin promotes dendritic spine and synapse formation by the PI3K/Akt/mTOR and Rac1 signaling pathways. Neuropharmacology 61:867–879. https://doi.org/10.1016/j.neuropharm.2011.06.003
Liu TY, Shi CX, Gao R, Sun HJ, Xiong XQ, Ding L, Chen Q, Li YH, Wang JJ, Kang YM et al (2015) Irisin inhibits hepatic gluconeogenesis and increases glycogen synthesis via the PI3K/Akt pathway in type 2 diabetic mice and hepatocytes. Clin Sci (Lond) 129:839–850. https://doi.org/10.1042/cs20150009
Zhou YZ, Zhang QQ, Kong YY, Guo XH, Zhang HY, Fan HQ, Liu LX (2020) Insulin-like growth factor binding protein-related protein 1 activates primary hepatic stellate cells via autophagy regulated by the PI3K/Akt/mTOR signaling pathway. Dig Dis Sci 65:509–523. https://doi.org/10.1007/s10620-019-05798-x
Gregnani MF, Hungaro TG, Martins-Silva L, Bader M, Araujo RC (2020) Bradykinin B2 receptor signaling increases glucose uptake and oxidation: Evidence and open questions. Front Pharmacol 11:1162. https://doi.org/10.3389/fphar.2020.01162
Jiang R, Wang MY, Shi L, Zhou JY, Ma R, Feng K, Chen XN, Xu XH, Li XY, Li T et al (2019) Panax ginseng total protein facilitates recovery from dexamethasone-induced muscle atrophy through the activation of glucose consumption in C2C12 myotubes. Biomed Res Int 2019:3719643. https://doi.org/10.1155/2019/3719643
Li S, Zhang Y, Sun YW, Zhang GZ, Bai J, Guo JF, Su XD, Du HQ, Cao X, Yang JK et al (2019) Naringenin improves insulin sensitivity in gestational diabetes mellitus mice through AMPK. Nutr Diabetes 9:28. https://doi.org/10.1038/s41387-019-0095-8
Yan R, Wang KC, Wang QQ, Jiang HY, Lu YF, Chen XX, Zhang H, Su XL, Du YL, Chen LF et al (2022) Probiotic Lactobacillus casei Shirota prevents acute liver injury by reshaping the gut microbiota to alleviate excessive inflammation and metabolic disorders. Microb Biotechnol 15:247–261. https://doi.org/10.1111/1751-7915.13750
Ferrocino I, Ponzo V, Gambino R, Zarovska A, Leone F, Monzeglio C, Goitre I, Rosato R, Romano A, Grassi G et al (2018) Changes in the gut microbiota composition during pregnancy in patients with gestational diabetes mellitus (GDM). Sci Rep 8:12216. https://doi.org/10.1038/s41598-018-30735-9
Koren O, Goodrich JK, Cullender TC, Spor A, Laitinen K, Bäckhed HK, Gonzalez A, Werner JJ, Angenent LT, Knight R et al (2012) Host remodeling of the gut microbiome and metabolic changes during pregnancy. Cell 150:470–480. https://doi.org/10.1016/j.cell.2012.07.008
Wang JF, Zheng JY, Shi WY, Du N, Xu XM, Zhang YM, Ji PF, Zhang FY, Jia Z, Wang YP et al (2018) Dysbiosis of maternal and neonatal microbiota associated with gestational diabetes mellitus. Gut 67:1614–1625. https://doi.org/10.1136/gutjnl-2018-315988
Cortez RV, Taddei CR, Sparvoli LG, Ângelo AGS, Padilha M, Mattar R, Daher S (2019) Microbiome and its relation to gestational diabetes. Endocrine 64:254–264. https://doi.org/10.1007/s12020-018-1813-z
Huang L, Thonusin C, Chattipakorn N, Chattipakorn SC (2021) Impacts of gut microbiota on gestational diabetes mellitus: a comprehensive review. Eur J Nutr 60:2343–2360. https://doi.org/10.1007/s00394-021-02483-6
Hasain Z, Mokhtar NM, Kamaruddin NA, Mohamed Ismail NA, Razalli NH, Gnanou JV, Raja Ali RA (2020) Gut microbiota and gestational diabetes mellitus: a review of host-gut microbiota interactions and their therapeutic potential. Front Cell Infect Microbiol 10:188. https://doi.org/10.3389/fcimb.2020.00188
Martineau MG, Raker C, Dixon PH, Chambers J, Machirori M, King NM, Hooks ML, Manoharan R, Chen K, Powrie R et al (2015) The metabolic profile of intrahepatic cholestasis of pregnancy is associated with impaired glucose tolerance, dyslipidemia, and increased fetal growth. Diabetes Care 38:243–248. https://doi.org/10.2337/dc14-2143
Funding
This work was supported by the National Key R & D Projects of China (Grant No. 2018YFC1704204).
Author information
Authors and Affiliations
Contributions
JW and JZ conceived and drafted the manuscript, prepared figures. JW, JZ, and YH conceived and designed the experiments. JW and JZ performed the animal experiments and analyzed the data. YH, HZ, and JZ (Jieqiong Zeng) reviewed and modified the manuscript. All authors have read and approved the final manuscript.
Corresponding authors
Ethics declarations
Competing Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wan, J., Zhu, J., Zeng, J. et al. Effect of Galactooligosaccharide on PPARs/PI3K/Akt Pathway and Gut Microbiota in High-Fat and High-Sugar Diet Combined with STZ-Induced GDM Rat Model. Probiotics & Antimicro. Prot. (2023). https://doi.org/10.1007/s12602-023-10186-z
Accepted:
Published:
DOI: https://doi.org/10.1007/s12602-023-10186-z