Abstract
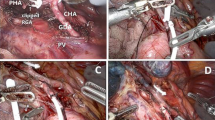
Hepatocellular carcinoma (HCC) is a life-threatening complication of hemophilia. Reports of patients with hemophilia undergoing hepatectomy for HCC are scarce. We report the cases of patients with hemophilia A and B who underwent laparoscopic hepatectomy for HCC. Perioperative hemophilia management was supervised by the hematology team. The patients received coagulation factor bolus injections immediately preoperatively, then continuous intravenous infusions intra- and postoperatively. A laparoscopic segment II partial hepatectomy was performed in case 1. Due to severe adhesions, intermittent pedicle clamping could not be used during parenchymal transection. The surgical duration was 235 min, and the estimated blood loss was 13 mL. The patient was discharged 11 days postoperatively without any complications. In case 2, laparoscopic partial hepatectomy for segments V/VI was performed. An intermittent pedicle clamp (Pringle method) was used during parenchymal transection. The surgical duration and estimated blood loss were 219 min and 18 mL, respectively. The patient was discharged 8 days postoperatively without complications. In both cases, intraoperative bleeding was minimal, and the patients were discharged without postoperative hemorrhage with appropriate perioperative coagulation factor management. Laparoscopic hepatectomy can be safely performed and appears to be a feasible treatment option for HCC in patients with hemophilia.




Similar content being viewed by others
References
Srivastava A, Brewer AK, Mauser-Bunschoten EP, et al. Guidelines for the management of hemophilia. Haemophilia. 2013;19:e1-47.
Darby SC, Ewart DW, Giangrande PL, et al. Mortality from liver cancer and liver disease in haemophilic men and boys in UK given blood products contaminated with hepatitis C. UK Haemophilia Centre Directors’ Organisation. Lancet. 1997;350:1425–31.
Goedert JJ, Eyster ME, Lederman MM, et al. End-stage liver disease in persons with hemophilia and transfusion-associated infections. Blood. 2002;100:1584–9.
Inokawa Y, Sugimoto H, Kanda M, et al. Hepatectomy for hepatocellular carcinoma in patients with hemophilia. J Hepato-Bil Pancreat Sci. 2014;21:824–8.
Kobayashi K, Kokudo T, Yamaguchi T, et al. Hepatectomy in patients with inherited blood coagulation disorders can be safely performed with adequate coagulation factor replacement. Haemophilia. 2019;25:463–7.
Araki K, Harimoto N, Ishii N, et al. Optimal indications for an intercostal port for the superior segments in laparoscopic partial liver resection. Asian J Endosc Surg. 2020;13:382–9.
Jones RM, Moulton CE, Hardy KJ. Central venous pressure and its effect on blood loss during liver resection. Br J Surg. 1998;85:1058–60.
Iguchi T, Ikegami T, Fujiyoshi T, et al. Low positive airway pressure without positive end-expiratory pressure decreases blood loss during hepatectomy in living liver donors. Dig Surg. 2017;34:192–6.
Kobayashi S, Honda G, Kurata M, et al. An experimental study on the relationship among airway pressure, pneumoperitoneum pressure, and central venous pressure in pure laparoscopic hepatectomy. Ann Surg. 2016;263:1159–63.
Shetty S, Sharma N, Ghosh K. Epidemiology of hepatocellular carcinoma (HCC) in hemophilia. Crit Rev Oncol Hematol. 2016;99:129–33.
Shen SC, Harada A, Kurokawa T, et al. Partial hepatectomy for hepatocellular carcinoma in a patient with hemophilia: a case report. Hepatogastroenterology. 1994;41:283–6.
Narushima Y, Ishiyama S, Kawashima K, et al. Operated hepatocellular carcinoma in two HIV− and HCV-positive hemophilic patients. J Hepato-Bil Pancreat Surg. 2004;11:207–10.
Jones AE, Roy A, Armstrong T, et al. Successful liver surgery in a haemophilia patient with high titre factor VIII inhibitor. Haemophilia. 2009;15:1332–3.
Hasegawa K, Takemura N, Yamashita T, et al. Clinical practice guidelines for hepatocellular carcinoma: The Japan Society of Hepatology 2021 version (5th JSH‐HCC guidelines). Hepatol Res. 2023;53:383–90.
Ng KKC, Chok KSH, Chan ACY, et al. Randomized clinical trial of hepatic resection versus radiofrequency ablation for early-stage hepatocellular carcinoma. Br J Surg. 2017;104:1775–84.
Takayama T, Hasegawa K, Izumi N, et al. Surgery versus radiofrequency ablation for small hepatocellular carcinoma: a randomized controlled trial (SURF trial). Liver Cancer. 2021;29:209–18.
Goka R, Morimoto N, Miura K, et al. Successful treatment of hepatocellular carcinoma by laparoscopic radiofrequency ablation in a patient with hemophilia A. Clin J Gastroenterol. 2020;13:907–13.
Yoshimoto-Haramura T, Hidaka M, Hasegawa K, et al. National survey of hepatobiliary and pancreatic surgery in hemophilia patients in Japan. J Hepato-Bil Pancreat Sci. 2022;29:385–93.
Matsuda T, Umeda Y, Yoshida K, et al. Laparoscopic Hepatectomy for the patient with hemophilia a with high titer factor VIII inhibitor. Acta Med Okayama. 2021;75:199–204.
Yin Z, Fan X, Ye H, et al. Short- and long-term outcomes after laparoscopic and open hepatectomy for hepatocellular carcinoma: a global systematic review and meta-analysis. Ann Surg Oncol. 2013;20:1203–15.
Takahara T, Wakabayashi G, Beppu T, et al. Long-term and perioperative outcomes of laparoscopic versus open liver resection for hepatocellular carcinoma with propensity score matching: a multi-institutional Japanese study. J Hepato-Bil Pancreat Sci. 2015;22:721–7.
White GC 2nd, Rosendaal F, Aledort LM, et al. Definitions in hemophilia. Recommendation of the scientific subcommittee on factor VIII and factor IX of the scientific and standardization committee of the International Society on Thrombosis and Haemostasis. Thromb Haemost. 2001;85:560.
Takatsuki M, Natsuda K, Hidaka M, et al. The treatment choices and outcome of hepatocellular carcinoma in hemophilic patients with human immunodeficiency virus/hepatitis C virus (HIV/HCV) coinfection due to contaminated blood products in Japan. J Gastrointest Oncol. 2021;12:2952–9.
Author information
Authors and Affiliations
Contributions
All the authors declare that they contributed to this article and have read and approved the final manuscript. MT reported this case and wrote the manuscript. MT, NH, KA, NI, KH, KH, and KS performed the surgery and perioperative management of the patients and helped draft the manuscript. KY, YO, and HH supervised the perioperative management of the hemophilia. KS participated in the critical revision of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there is no conflict of interest.
Human/animal rights
All procedures were performed in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and the Helsinki Declaration of 1975, as revised in 2008(5).
Informed consent
Written informed consent was obtained from both patients to publish this case report and any accompanying images.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Tsukagoshi, M., Harimoto, N., Araki, K. et al. Laparoscopic hepatectomy for hepatocellular carcinoma in patients with hemophilia A and B: a report of two cases. Clin J Gastroenterol 16, 884–890 (2023). https://doi.org/10.1007/s12328-023-01854-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12328-023-01854-2