Abstract
Background
There are conflicting data regarding the role of KRAS mutation on the risk of venous thromboembolism (VTE) in colorectal cancer (CRC) patients. Moreover, the role of other biomarkers such as NRAS or BRAF has not been studied.
Purpose
To analyze the incidence of VTE in a cohort of patients with CRC based on KRAS, NRAS, and BRAF status.
Methods
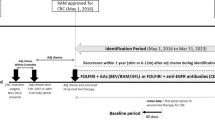
We performed a retrospective review of patients with unresectable locally advanced and metastatic CRC (mCRC) and known KRAS/NRAS/BRAF status, attended in the Medical Oncology Department of the Hospital General Universitario Gregorio Marañón (Madrid, Spain). The primary outcome was VTE defined as any venous thromboembolic event that occurred either 6 months before or at any time after the diagnosis of CRC. The biomarker status (KRAS, NRAS, and BRAF) and other predictors of thrombosis were collected.
Results
One hundred and ninety-four patients were identified and included in the analysis. Forty-one patients (21.1%) experienced VTE. The incidence was 19.1% in RAS-mutated patients, 28.6% in BRAF-mutated patients and 21% in triple wild-type patients (p = NS). In multivariate analysis, ECOG ≥ 2 was the only independent predictor of VTE (OR 8.73; CI 95% 1.32–57.82; p = 0.025).
Conclusions
In our study, biomarkers have not been associated with an increased risk of VTE in CRC patients. A high incidence of VTE in BRAF-mutated patients has been observed and should be explored in further studies.
Similar content being viewed by others
References
Sørensen HT, Mellemkjaer L, Olsen JH, Baron JA. Prognosis of cancers associated with venous thromboembolism. N Engl J Med. 2000;343(25):1846–50.
Mandalà M, Falanga A, Roila F. Management of venous thromboembolism (VTE) in cancer patients: ESMO Clinical Practice Guidelines. Ann Oncol. 2011;22(Suppl 6):vi85–92.
Kearon C, Akl EA, Comerota AJ, et al. Antithrombotic therapy for VTE disease: Antithrombotic therapy and prevention of thrombosis, 9th ed: American Collegue of Chest Physicians Evidence-Based Clinical Practice Guideline. Chest. 2012;141(2 Suppl):e419S–496S.
Muñoz Martín AJ, Font Puig C, Navarro Martín LM, Borrega García P, Martín JM. Clinical guide SEOM on venous thromboembolism in cancer patients. Clin Transl Oncol. 2014;16(12):1079–90.
Key NS, Khorana AA, Kuderer NM, et al. Venous thromboembolism prophylaxis and treatment in patients with cancer: ASCO Clinical Practice Guideline update. J Clin Oncol. 2019. https://doi.org/10.1200/JCO.19.01461.
Farge D, Frere C, Connors JM, et al. 2019 international clinical practice guidelines for the treatment and prophylaxis of venous thromboembolism in patients with cancer. Lancet Oncol. 2019;20(10):e566–e581581.
Khorana AA, Kuderer NM, Culakova E, et al. Development and validation of a predictive model for chemotherapy-associated thrombosis. Blood. 2008;111:4902–7.
Ay C, Dunkler D, Marosi C, et al. Prediction of venous thromboembolism in cancer patients. Blood. 2010;116:5377–82.
Verso M, Agnelli G, Barni S, et al. A modified Khorana risk assessment score for venous thromboembolism in cancer patients receiving chemotherapy: the Protecht score. Intern Emerg Med. 2012;7:291–2.
Pelzer U, Sinn M, Stieler J, et al. Primary pharmacological prevention of thromboembolic events in ambulatory patients with advanced pancreatic cancer treated with chemotherapy? Dtsch Med Wochenschr. 2013;138:2084–8.
Cella CA, Di Minno G, Carlomagno C, et al. Preventing venous thromboembolism in ambulatory cancer patients: the ONKOTEV study. Oncologist. 2017;22:601–8.
Gerotziafas GT, Taher A, Abdel-Razeq H, et al. A predictive score for thrombosis associated with breast, colorectal, lung, or ovarian cancer: the prospective COMPASS-cancer-associated thrombosis study. Oncologist. 2017;22:1222–311.
Muñoz Martin AJ, Ortega I, Font C, et al. Multivariable clinical-genetic risk model for predicting venous thromboembolic events in patients with cancer. Br J Cancer. 2018;118:1056–61.
Pabinger I, van Es N, Heinze G, et al. A clinical prediction model for cancer-associated venous thromboembolism: a development and validation study in two independent prospective cohorts. Lancet Haematol. 2018;5:e289–e298298.
Zugazagoitia J, Biosca M, Oliveira J, et al. Incidence, predictors and prognostic significance of thromboembolic disease in patients with advanced ALK-rearranged non-small cell lung cancer. Eur Respir J. 2018;51(5):1702431.
Muñoz Unceta N, Zugazagoitia J, Manzano A, et al. Incidencia de enfermedad tromboembólica venosa en pacientes con adenocarcinoma de pulmón y traslocación ROS-1. Proceedings of National Congress of Spanish Society of Medical Oncology, Pamplona, Spain, 22–25 October 2019.
Boccaccio C, Comoglio PM. Genetic link between cancer and thrombosis. J Clin Oncol. 2009;27(29):4827–33.
Lee MKC, Loree JM. Current and emerging biomarkers in metastatic colorectal cancer. Curr Oncol. 2019;26(S1):S7–S15.
Ades S, Kumar S, Alam M, Goodwin A, Weckstein D, Dugan M, Ashikaga T, Evans M, Verschraegen C, Holmes CE. Tumor oncogene (KRAS) status and risk of venous thrombosis in patients with metastatic colorectal cancer. J Thromb Haemost. 2015;13:998–1003.
Menapace LA, Bena J, Morrison S, Khorana AA. KRAS mutational status in metastatic colorectal cancer and thrombotic risk. J Clin Oncol. 2017;35(15 suppl):15140–15140.
Alcalay A, Wun T, Khatri V, Chew HK, Harvey D, Zhou H, White RH. Venous thromboembolism in patients with colorrectal cancer: incidence and effect on survival. J Clin Oncol. 2006;24:1112–8.
Mandala M, Barni S, Floriani I, et al. Incidence and clinical implications of venous thromboembolism in advanced colorectal cancer patients: The ‘GISCAD-alternating schedule’ study findings. Eur J Cancer. 2009;45(1):65–73.
Koopman M, Antonini NF, Douma J, et al. Sequential versus combination chemotherapy with capecitabine, irinotecan, and oxaliplatin in advanced colorectal cancer (CAIRO): a phase III randomised controllled trial. Lancet. 2007;370(9582):135–42.
Yu JL, May L, Lhotak V, et al. Oncogenic events regulate tissue factor expression in colorectal cancer cells: implications for tumor progression and angiogenesis. Blood. 2005;105(4):1734–41.
Regina S, Rollin J, Bléchet C, et al. Tissue factor expression in non-small cell lung cancer: Relationship with vascular endothelial growth factor expression, microvascular density, and K-ras mutation. J Thorac Oncol. 2008;3:689–97.
Corrales-Rodriguez L, Soulières D, Weng X, et al. Mutations in NSCLC and their link with cancer-associated thrombosis: A case-control study. Thromb Res. 2014;133(1):48–51.
Dou F, Li H, Zhu M, et al. Association between oncogenic status and risk of venous thromboembolism in patients with non-small cell lung cancer. Respir Res. 2018;19(1):88.
Abdol Razak NB, Jones G, Bhandari M, Berndt MC, Metharom P. Cancer-associated thrombosis: An overview of mechanism, risk factors, and treatment. Cancers (Basel). 2018;10(10):380.
Petrelli F, Cabiddu M, Borgonovo K, et al. Risk of venous and arterial thromboembolic events associated with anti-EGFR agents: a metanalysis of randomized clinical trial. Ann Oncol. 2012;23(7):1672–730.
National Comprehensive Cancer Network. Colon cancer (version 1.2020). https://www.nccn.org/professionals/physician_gls/pdf/colon.pdf. Accessed February 3, 2020.
Funding
This study had no funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Laura Ortega Morán received speakers’ honoraria or honoraria for participation in Advisory Boards from Amgen and Sanofi; travel, accommodations and expenses from Amgen, Leo Pharma, Roche and Sanofi. Pilar García Alfonso received speakers’ honoraria or honoraria for participation in Advisory Boards from Roche, Amgen, Merck, Sanofi and Servier; travel, accommodations and expenses from Roche and Merck. Iker Aguilar Caballero received speakers’ honoraria from Kyowa Kirin; travel, accommodations and expenses from Astra-Zeneca, Roche, and Sanofi. Blanca Morón García received support for travel, accommodations, and expenses from MSD. Victoria Tirado Anula received support for travel, accommodations, and expenses from MSD. María de Toro Carmena received support for travel, accommodations, and expenses from Leo Pharma and MSD. Javier Soto Alsar has an immediate family member employed by Pfizer and Sanofi; travel, accommodations, and expenses from Angelini, MSD, Rovi, Sanofi, and Vifor Pharma. Marianela Bringas Beranek received support for travel, accommodations, and expenses from MSD, Rovi, Sanofi, and Vifor Pharma. Natalia Gutiérrez Alonso received support for travel, accommodations, and expenses from Angelini, MSD, Rovi, and Sanofi. Miguel Martín received speakers’ honoraria or honoraria for participation in Advisory Boards from Roche, Novartis, Pfizer, Lilly, Astra-Zeneca, Taiho Pharmaceutical, and PharmaMar; research funding from Novartis and Roche. Andrés J. Muñoz Martín received speakers’ honoraria or honoraria for participation in Advisory Boards from Astra-Zeneca, Bayer Halozyme, Celgene, Daiichi Sankyo Roche, Leo Pharma, Pfizer, Sanofi, Servier, Amgen, Lilly, and Rovi; research funding from Celgene, Leo Pharma, and Sanofi; patents: risk assessment model in venous thromboembolism in cancer patients; travel, accodomodations, and expenses from Amgen, Celgene, Merck Serono, Roche, and Sanofi.
Ethical approval
The study was approved by the Ethics Committee of Hospital General Universitario Gregorio Marañón, Madrid, Spain. The study has been approved by the appropriate institutional and/or national research ethics committee and has been performed in accordance with the ethical standards as laid down in the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards.
Informed consent
For this type of study formal consent is not required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ortega Morán, L., García Alfonso, P., Aguilar Caballero, I. et al. Incidence of venous thromboembolism in patients with colorectal cancer according to oncogenic status. Clin Transl Oncol 22, 2026–2031 (2020). https://doi.org/10.1007/s12094-020-02339-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12094-020-02339-1