Abstract
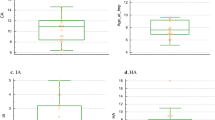
The goal of this study was to investigate the probable difference in auditory perception and speech intelligibility performance amongst cochlear implanted children who experienced hyperbilirubinemia or auditory neuropathy in comparison to the cochlear implanted children with unknown etiology for hearing loss. This case–control study was carried out on 106 cochlear implanted children with mean age of 32.36 ± 11.98 months who were purposively selected and allocated into four groups. Out of the total, 30 had no specific etiology for hearing loss, while the others had experienced auditory neuropathy or hyperbilirubinemia with/without blood exchange. The auditory perception and speech intelligibility performance of all the participants who had received auditory verbal therapy were assessed after 6 and 12 months of rehabilitation. Then, the data was analyzed, using the Statistical Package for Social Sciences-version 21(SPSS-21). Results indicated poor auditory perception and speech intelligibility performance of the cochlear implanted children with hyperbilirubinemia and blood exchange (P ≤ 0.05), while the participants in the control group with no specific etiology for hearing loss, the children with hyperbilirubinemia with no blood exchange, and those who suffered from auditory neuropathy performed better, respectively. Also, a significant correlation between auditory neuropathy and hyperbilirubinemia was observed. Despite lower improvement of auditory perception and speech intelligibility of the hearing impaired children who were experiencing moderate to severe degrees of hyperbilirubinemia or auditory neuropathy, cochlear implantation is highly recommended not only for children with unknown etiology for severe hearing loss but also for this group of hearing impaired children.


Similar content being viewed by others
References
Boo NY, Rohani AJ, Asma A (2008) Detection of sensorineural hearing loss using automated auditory brainstem-evoked response and transient-evoked otoacoustic emission in term neonates with severe hyperbilirubinaemia. Singap Med J 49(3):209–214 (PMID: 18363002)
Akinpelu OV, Waissbluth S, Daniel SJ (2013) Auditory risk of hyperbilirubinemia in term newborns: a systematic review. Int J Pediatr Otorhinolaryngol 77(6):898–905. https://doi.org/10.1016/j.ijporl.2013.03.029
Amin SB, Wang H (2015) Unbound unconjugated hyperbilirubinemia is associated with central apnea in premature infants. J Pediatr 166(3):571–575. https://doi.org/10.1016/j.jpeds.2014.12.003
Soorani-Lunsing I, Woltil HA, Hadders-Algra M (2001) Are moderate degrees of hyperbilirubinemia in healthy term neonates really safe for the brain? Pediatr Res 50(6):701–705. https://doi.org/10.1203/00006450-200112000-00012
Saluja S, Agarwal A, Kler N, Amin S (2010) Auditory neuropathy spectrum disorder in late preterm and term infants with severe jaundice. Int J Pediatr Otorhinolaryngol 74(11):1292–1297. https://doi.org/10.1016/j.ijporl.2010.08.007
Rhee CK, Park HM, Jang YJ (1999) Audiologic evaluation of neonates with severe hyperbilirubinemia using transiently evoked otoacoustic emissions and auditory brainstem responses. Laryngoscope 109(12):2005–2008. https://doi.org/10.1097/00005537-199912000-00021
Starr A, Picton TW, Sininger Y, Hood LJ, Berlin CI (1996) Auditory neuropathy. Brain 119(Pt 3):741–753. https://doi.org/10.1093/brain/119.3.741
Archbold S, Lutman ME, Nikolopoulos T (1998) Categories of auditory performance: inter-user reliability. Br J Audiol 32(1):7–12. https://doi.org/10.3109/03005364000000045
Allen MC, Nikolopoulos TP, O’Donoghue GM (1998) Speech intelligibility in children after cochlear implantation. Am J Otol 19(6):742–6
Xu J, Weng M, Li N, Wu X, Gao L, Yao H et al (2019) Relationship research between auditory neuropathy spectrum disorder and exchange transfusion in neonates with severe hyperbilirubinemia. Int J Pediatr Otorhinolaryngol 123:146–150. https://doi.org/10.1016/j.ijporl.2019.04.044
Rhee CK, Park HM, Jang YJ (2009) Audiologic evaluation of neonates with severe hyperbilirubinemia using transiently evoked otoacoustic emissions and auditory brainstem responses. Laryngoscope 109(12):2005–8. https://doi.org/10.1097/00005537-199912000-00021
Olds C, Oghalai JS (2015) Audiologic impairment associated with bilirubin-induced neurologic damage. Semin Fetal Neonatal Med 20(1):42–46. https://doi.org/10.1016/j.siny.2014.12.006
Paul R (2007) Language disorders from infancy through adolescence. Mosby, USA
Fagan MK, Pisoni DB (2010) Hearing experience and receptive vocabulary development in deaf children with cochlear implants. J Deaf Stud Deaf Educ 15(2):149–161. https://doi.org/10.1093/deafed/enq001
Shapiro SM, Nakamura H (2001) Bilirubin and the auditory system. J Perinatol 21:S52–S55. https://doi.org/10.1038/sj.jp.7210635 (discussion S9-62)
Matkin ND, Carhart R (1966) Auditory profiles associated with Rh incompatibility. Arch Otolaryngol (Chicago III: 1960) 84(5):502–13. https://doi.org/10.1001/archotol.1966.00760030504008
Amin SB, Ahlfors C, Orlando MS, Dalzell LE, Merle KS, Guillet R (2001) Bilirubin and serial auditory brainstem responses in premature infants. Pediatrics 107(4):664–670. https://doi.org/10.1542/peds.107.4.664
Acknowledgements
The authors would like to thank all the cochlear implant centers who collaborated in data collection. The authors wish to thank Mr. H. Argasi at the Research Consultation Center (RCC) of Shiraz University of Medical Sciences for his invaluable assistance in editing this manuscript too.
Funding
No funding was received for conducting this study.
Author information
Authors and Affiliations
Contributions
HSB and ML proposed the main concept and idea of the research, performed the research, interoperated the data and wrote the paper and made critical contribution to the concept and design of the research; RM did the statistical analysis and revision related to content of the manuscript. HF, RM, DA, FM, EH, contributed equally in the concept and design of the study and data collection, interpretation of data for the work, investigating and resolving the questions related to the work.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Ethical approval and Consent
All procedures performed in the present study were in accordance with the ethical standards of Shiraz University of Medical Sciences research committee and with the 1964 Helsinki declaration and its later amendments. The study protocol was reviewed and approved by the Ethics Committee of Shiraz University of Medical Sciences, Shiraz, Iran. (Ethic code: IR.SUMS.MED.REC.1399.043).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hashemi, S.B., Monshizadeh, L., Rahimi, M. et al. Hyperbilirobinemia and Its Effect on Auditory Perception and Speech Intelligibility in Cochlear Implanted Children (Cochlear Implantation Outcomes in Children Who Have Experienced Hyperbilirobinemia). Indian J Otolaryngol Head Neck Surg 74 (Suppl 3), 4144–4149 (2022). https://doi.org/10.1007/s12070-021-02877-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12070-021-02877-2