Abstract
Purpose
No conclusive information is available about the association between hypothyroidism or hyperthyroidism and risk of colorectal cancer (CRC). We therefore aimed to summarize the findings of observational studies on the relation between hypothyroidism or hyperthyroidism and risk of CRC.
Methods
A literature search was conducted using relevant keywords in online databases for appropriate publications through July 2023. Random effects model was used to calculate combined effect sizes (ESs) and 95% confidence intervals (CIs) to investigate relationship between hypothyroidism or hyperthyroidism and CRC risk.
Results
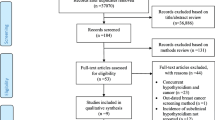
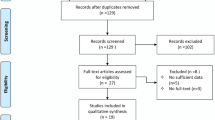
Totally, we included 13 studies in the current systematic review and meta-analysis, with a total sample size of 33,557,450 individuals and 25,363 cases of CRC. Pooling 13 effect sizes revealed no significant association between hypothyroidism and risk of CRC (combined effect size: 1.13, 95% CI 0.87–1.48, P = 0.343). There was also no significant association between hyperthyroidism and risk of CRC (combined effect size: 1.09, 95% CI 0.75–1.57, P = 0.638). Additionally, there were significant associations between hypothyroidism and risk of CRC in the Far Eastern studies, between hyperthyroidism and risk of CRC in the Middle East, along with small sample size studies.
Conclusions
This meta-analysis did not reveal any association between hypothyroidism or hyperthyroidism and risk of CRC.
Trial Registration
PROSPERO CRD42022331089.





Similar content being viewed by others
Availability of Data and Materials
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- CRC:
-
Colorectal cancer
- ESs:
-
Effect sizes
- CIs:
-
Confidence intervals
- THs:
-
Thyroid hormones
- TSH:
-
Thyroid stimulating hormone
- T4:
-
Tetraiodothyronine
- T3:
-
Triiodothyronine
- TRα:
-
Thyroid hormone receptors alpha
- TRβ:
-
Thyroid hormone receptors beta
- TREs:
-
Thyroid hormone response elements
- PRISMA:
-
Preferred Reporting Items for Systematic Review and Meta-Analysis
- RR:
-
Relative risk
- HR:
-
Hazard ratio
- OR:
-
Odds ratio
- NOS:
-
Newcastle-Ottawa Scale
- PI3K:
-
Phosphatidyl inositol 3-kinase
- HIF1α:
-
Hypoxia-inducible factor-1α
- DIO3:
-
Deiodinase type III
- DIO2:
-
Deiodinase type II
- rT3:
-
Reverse T3
- NTIS:
-
Non-thyroidal illness syndrome
References
Ortiga-Carvalho TM, Chiamolera MI, Pazos-Moura CC, Wondisford FE. Hypothalamus-pituitary-thyroid axis. Compr Physiol. 2011;6(3):1387–428.
Piekiełko-Witkowska A, Nauman A. Iodothyronine deiodinases and cancer. J Endocrinol Invest. 2011;34(9):716–28.
Davis PJ, Goglia F, Leonard JL. Nongenomic actions of thyroid hormone. Nat Rev Endocrinol. 2016;12(2):111–21.
Taylor PN, Albrecht D, Scholz A, Gutierrez-Buey G, Lazarus JH, Dayan CM, Okosieme OE. Global epidemiology of hyperthyroidism and hypothyroidism. Nat Rev Endocrinol. 2018;14(5):301–16.
Huang CH, Wei JC, Chien TC, Kuo CW, Lin SH, Su YC, Hsu CY, Chiou JY, Yeh MH. Risk of breast cancer in females with hypothyroidism: a nationwide, population-based, cohort study. Endocr Pract. 2021;27(4):298–305.
Kirkegård J, Farkas DK, Jørgensen JOL, Cronin-Fenton D. Hyper- and hypothyroidism and gastrointestinal cancer risk: a Danish nationwide cohort study. Endocr Connect. 2018;7(11):1129–35.
Søgaard M, Farkas DK, Ehrenstein V, Jørgensen JO, Dekkers OM, Sørensen HT. Hypothyroidism and hyperthyroidism and breast cancer risk: a nationwide cohort study. Eur J Endocrinol. 2016;174(4):409–14.
Yeh NC, Chou CW, Weng SF, Yang CY, Yen FC, Lee SY, Wang JJ, Tien KJ. Hyperthyroidism and thyroid cancer risk: a population-based cohort study. Exp Clin Endocrinol Diabetes. 2013;121(7):402–6.
L’Heureux A, Wieland DR, Weng C-H, Chen Y-H, Lin C-H, Lin T-H, Weng C-H. Association between thyroid disorders and colorectal cancer risk in adult patients in Taiwan. JAMA Netw Open. 2019;2(5):e193755–e193755.
Wolf AM, Fontham ET, Church TR, Flowers CR, Guerra CE, LaMonte SJ, Etzioni R, McKenna MT, Oeffinger KC, Shih YCT. Colorectal cancer screening for average‐risk adults: 2018 guideline update from the American Cancer Society. CA: Cancer J Clin. 2018;68(4):250–281.
Arnold M, Sierra MS, Laversanne M, Soerjomataram I, Jemal A, Bray F. Global patterns and trends in colorectal cancer incidence and mortality. Gut. 2017;66(4):683–91.
Rennert G, Rennert HS, Pinchev M, Gruber SB. A case-control study of levothyroxine and the risk of colorectal cancer. J Natl Cancer Inst. 2010;102(8):568–72.
Chen YK, Lin CL, Cheng FT, Sung FC, Kao CH. Cancer risk in patients with Hashimoto’s thyroiditis: a nationwide cohort study. Br J Cancer. 2013;109(9):2496–501.
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, Shamseer L, Tetzlaff JM, Akl EA, Brennan SE, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. Syst Rev. 2021;10(1):89.
Stang A. Critical evaluation of the Newcastle-Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur J Epidemiol. 2010;25(9):603–5.
DerSimonian R, Laird N. Meta-analysis in clinical trials revisited. Contemp Clin Trials. 2015;45(Pt A):139–45.
Chandler J, Cumpston M, Li T. Cochrane handbook for systematic reviews of interventions.
van Enst WA, Ochodo E, Scholten RJ, Hooft L, Leeflang MM. Investigation of publication bias in meta-analyses of diagnostic test accuracy: a meta-epidemiological study. BMC Med Res Methodol. 2014;14(1):1–11.
Mansoor E, Chouhan V, Abou Saleh M, Sheriff ZM, Cooper GS. 330 increased risk of colorectal cancer in individuals with hypothyroidism and hyperthyroidism: results from a population-based national study. Offic J Am Coll Gastroenterol | ACG. 2019;114:S194.
Kirkegård J, Farkas DK, Jørgensen JOL, Cronin-Fenton DP. Hyperthyroidism or hypothyroidism and gastrointestinal cancer risk: a Danish nationwide cohort study. Endocr Connect. 2018;7(11):1129–35.
Chan YX, Knuiman MW, Divitini ML, Brown SJ, Walsh J, Yeap BB. Lower TSH and higher free thyroxine predict incidence of prostate but not breast, colorectal or lung cancer. Eur J Endocrinol. 2017;177(4):297–308.
Chan YX, Alfonso H, Chubb SAP, Fegan PG, Hankey GJ, Golledge J, Flicker L, Yeap BB. Higher thyrotropin concentration is associated with increased incidence of colorectal cancer in older men. Clin Endocrinol. 2017;86(2):278–85.
Mu G, Mu X, Xing H, Xu R, Sun G, Dong C, Pan Q, Xu C. Subclinical hypothyroidism as an independent risk factor for colorectal neoplasm. Clin Res Hepatol Gastroenterol. 2015;39(2):261–6.
Boursi B, Haynes K, Mamtani R, Yang Y-X. Thyroid dysfunction, thyroid hormone replacement and colorectal cancer risk. J Natl Cancer Inst. 2015;107(6):djv084.
Chen Y-K, Lin C-L, Chang Y-J. Cheng FT-F, Peng C-L, Sung F-C, Cheng Y-H, Kao C-H. Cancer risk in patients with Graves’ disease: a nationwide cohort study. Thyroid. 2013;23(7):879–84.
Hellevik AI, Åsvold BO, Bjøro T, Romundstad PR, Nilsen TIL, Vatten LJ. Thyroid function and cancer risk: a prospective population study. Cancer Epidemiology and Prevention Biomarkers. 2009;18(2):570–4.
Kuiper JG, Fenneman AC, van der Spek AH, Rampanelli E, Nieuwdorp M, van Herk-Sukel MP, Lemmens VE, Kuipers EJ, Herings RM, Fliers E. Levothyroxine use and the risk of colorectal cancer: a large population-based case–control study. Endocr Connect. 2022;11(1).
Wu CC, Islam MM, Nguyen PA, Poly TN, Wang CH, Iqbal U, Li YCJ, Yang HC. Risk of cancer in long-term levothyroxine users: retrospective population-based study. Cancer Sci. 2021;112(6):2533.
Rennert G, Rennert HS, Pinchev M, Gruber SB. A case–control study of levothyroxine and the risk of colorectal cancer. J Natl Cancer Inst. 2010;102(8):568–72.
Kuiper JG, Fenneman AC, van der Spek AH, Rampanelli E, Nieuwdorp M, van Herk-Sukel MPP, Lemmens V, Kuipers EJ, Herings RMC, Fliers E. Levothyroxine use and the risk of colorectal cancer: a large population-based case-control study. Endocr Connect. 2022;11(1).
Chen Y-K, Lin C-L, Chang Y-J. Cheng FT-F, Peng C-L, Sung F-C, Cheng Y-H, Kao C-H. Cancer risk in patients with Graves’ disease: a nationwide cohort study. Thyroid Offic J Am Thyroid Assoc. 2013;23(7):879–84.
Boursi B, Haynes K, Mamtani R, Yang YX. Thyroid dysfunction, thyroid hormone replacement and colorectal cancer risk. J Natl Cancer Inst. 2015;107(6).
L’Heureux A, Wieland DR, Weng CH, Chen YH, Lin CH, Lin TH, Weng CH. Association between thyroid disorders and colorectal cancer risk in adult patients in Taiwan. JAMA Netw Open. 2019;2(5).
Kirkegård J, Farkas DK, Jørgensen JOL, Fenton DPC. Hyperthyroidism or hypothyroidism and gastrointestinal cancer risk: a Danish nationwide cohort study. Endocr Connect. 2018;7(11):1129–35.
Alikhan M, Mansoor E, Panhwar MS, Abou Saleh M, Chouhan V, Sheriff MZ, Cooper GS. Increased risk of colorectal cancer in individuals with hypothyroidism and hyperthyroidism: results from a population-based national study. Gastroenterology. 2020;158(6):S499–500.
Krashin E, Piekiełko-Witkowska A, Ellis M, Ashur-Fabian O. Thyroid hormones and cancer: a comprehensive review of preclinical and clinical studies. Front Endocrinol. 2019;10:59.
Rawla P, Sunkara T, Barsouk A. Epidemiology of colorectal cancer: incidence, mortality, survival, and risk factors. Przeglad gastroenterologiczny. 2019;14(2):89–103.
Rostkowska O, Spychalski P, Dobrzycka M, Wilczyński M, Łachiński AJ, Obołończyk Ł, Sworczak K, Kobiela J. Effects of thyroid hormone imbalance on colorectal cancer carcinogenesis and risk - a systematic review. Endokrynol Pol. 2019;70(2):190–7.
Lars CM, Dagmar F. Thyroid hormone, thyroid hormone receptors, and cancer: a clinical perspective. Endocr Relat Cancer. 2013;20(2):R19–29.
Khan SR, Chaker L, Ruiter R, Aerts JGJV, Hofman A, Dehghan A, Franco OH, Stricker BHC, Peeters RP. Thyroid function and cancer risk: the Rotterdam study. J Clin Endocrinol Metab. 2016;101(12):5030–6.
Boursi B, Haynes K, Mamtani R, Yang Y-X. Thyroid dysfunction, thyroid hormone replacement and colorectal cancer risk. JNCI: J Natl Cancer Inst. 2015;107(6).
Liu Y-C, Yeh C-T, Lin K-H. Molecular functions of thyroid hormone signaling in regulation of cancer progression and anti-apoptosis. Int J Mol Sci. 2019;20(20):4986.
Zhu L, Tian G, Yang Q, De G, Zhang Z, Wang Y, Nie H, Zhang Y, Yang X, Li J. Thyroid hormone receptor β1 suppresses proliferation and migration by inhibiting PI3K/Akt signaling in human colorectal cancer cells. Oncol Rep. 2016;36(3):1419–26.
Brown AR, Simmen RCM, Simmen FA. The role of thyroid hormone signaling in the prevention of digestive system cancers. Int J Mol Sci. 2013;14(8):16240–57.
Dentice M, Luongo C, Ambrosio R, Sibilio A, Casillo A, Iaccarino A, Troncone G, Fenzi G, Larsen PR, Salvatore D. β-catenin regulates deiodinase levels and thyroid hormone signaling in colon cancer cells. Gastroenterology. 2012;143(4):1037–47.
Shimi G, Zand H, Pourvali K, Ghorbani A. Colorectal cancer causes alteration of thyroid hormone profile in newly diagnosed patients. Expert Rev Endocrinol Metab. 2021;16(5):259–62.
Deligiorgi MV, Trafalis DT. The intriguing thyroid hormones-lung cancer association as exemplification of the thyroid hormones-cancer association: three decades of evolving research. Int J Mol Sci. 2021;23(1):436.
Pasqualetti G, Schirripa M, Dochy E, Fassan M, Ziranu P, Puzzoni M, Scartozzi M, Alberti G, Lonardi S, Zagonel V, et al. Thyroid hormones ratio is a major prognostic marker in advanced metastatic colorectal cancer: results from the phase III randomised CORRECT trial. Eur J Cancer (Oxford, England : 1990). 2020;133:66–73.
Gómez-Izquierdo J, Filion KB, Boivin J-F, Azoulay L, Pollak M, Yu OHY. Subclinical hypothyroidism and the risk of cancer incidence and cancer mortality: a systematic review. BMC Endocr Disord. 2020;20(1):83.
Acknowledgements
Not applicable.
Funding
Not applicable.
Author information
Authors and Affiliations
Contributions
Conceptualization: O.A. and G.S; Methodology: O.A. and G.S; Formal analysis and investigation: O.A.; Writing original draft preparation: O.A. and G.S; Writing review and editing: K.P. and G.E.; Supervision: H.Z. and S.H.D. All authors have approved the submitted draft.
Corresponding author
Ethics declarations
Ethics Approval and Consent to Participate
Not applicable.
Consent for Publication
Not applicable.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Asbaghi, O., Shimi, G., Davoodi, S.H. et al. Thyroid Hormones Imbalances and Risk of Colorectal Cancer: a Meta-analysis. J Gastrointest Canc 55, 105–117 (2024). https://doi.org/10.1007/s12029-023-00979-4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12029-023-00979-4