Abstract
Background
Cardiac point-of-care ultrasound (cPOCUS) can aid in the diagnosis and treatment of cardiac disorders. Such disorders can arise as complications of acute brain injury, but most neurologic intensive care unit (NICU) providers do not receive formal training in cPOCUS. Caption artificial intelligence (AI) uses a novel deep learning (DL) algorithm to guide novice cPOCUS users in obtaining diagnostic-quality cardiac images. The primary objective of this study was to determine how often NICU providers with minimal cPOCUS experience capture quality images using DL-guided cPOCUS as well as the association between DL-guided cPOCUS and change in management and time to formal echocardiograms in the NICU.
Methods
From September 2020 to November 2021, neurology-trained physician assistants, residents, and fellows used DL software to perform clinically indicated cPOCUS scans in an academic tertiary NICU. Certified echocardiographers evaluated each scan independently to assess the quality of images and global interpretability of left ventricular function, right ventricular function, inferior vena cava size, and presence of pericardial effusion. Descriptive statistics with exact confidence intervals were used to calculate proportions of obtained images that were of adequate quality and that changed management. Time to first adequate cardiac images (either cPOCUS or formal echocardiography) was compared using a similar population from 2018.
Results
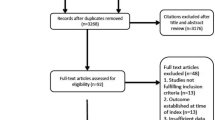
In 153 patients, 184 scans were performed for a total of 943 image views. Three certified echocardiographers deemed 63.4% of scans as interpretable for a qualitative assessment of left ventricular size and function, 52.6% of scans as interpretable for right ventricular size and function, 34.8% of scans as interpretable for inferior vena cava size and variability, and 47.2% of scans as interpretable for the presence of pericardial effusion. Thirty-seven percent of screening scans changed management, most commonly adjusting fluid goals (81.2%). Time to first adequate cardiac images decreased significantly from 3.1 to 1.7 days (p < 0.001).
Conclusions
With DL guidance, neurology providers with minimal to no cPOCUS training were often able to obtain diagnostic-quality cardiac images, which informed management changes and significantly decreased time to cardiac imaging.



Similar content being viewed by others
Data Availability
Deidentified data will be made available upon reasonable request. Requests for data sharing can be sent to jhc9010@med.cornell.edu.
References
Kuohn LR, Leasure AC, Acosta JN, Vanent K, Murthy SB, Kamel H, et al. Cause of death in spontaneous intracerebral hemorrhage survivors: multistate longitudinal study. Neurology. 2020;95(20):e2736–45.
Morris NA, Chatterjee A, Adejumo OL, Chen M, Merkler AE, Murthy SB, et al. The risk of Takotsubo cardiomyopathy in acute neurological disease. Neurocrit Care. 2019;30(1):171–6.
Gopinath R, Ayya SS. Neurogenic stress cardiomyopathy: what do we need to know. Ann Card Anaesth. 2018;21(3):228–34.
Prosser J, MacGregor L, Lees KR, Diener HC, Hacke W, Davis S, VISTA Investigators. Predictors of early cardiac morbidity and mortality after ischemic stroke. Stroke. 2007;38(8):2295–302.
Rauh R, Fischereder M, Spengel FA. Transesophageal echocardiography in patients with focal cerebral ischemia of unknown cause. Stroke. 1996;27(4):691–4.
Belcour D, Jabot J, Grard B, Roussiaux A, Ferdynus C, Vandroux D, et al. Prevalence and risk factors of stress cardiomyopathy after convulsive status epilepticus in ICU patients. Crit Care Med. 2015;43(10):2164–70.
Pathan N, Hemingway CA, Alizadeh AA, Stephens AC, Boldrick JC, Oragui EE, et al. Role of interleukin 6 in myocardial dysfunction of meningococcal septic shock. Lancet. 2004;363(9404):203–9.
Cheng CY, Hsu CY, Wang TC, Jeng YC, Yang WH. Evaluation of cardiac complications following hemorrhagic stroke using 5-year Centers for Disease Control and Prevention (CDC) database. J Clin Med. 2018;7(12):519.
Tigaran S, Mølgaard H, McClelland R, Dam M, Jaffe AS. Evidence of cardiac ischemia during seizures in drug refractory epilepsy patients. Neurology. 2003;60(3):492–5.
Cheema BS, Walter J, Narang A, Thomas JD. Artificial intelligence-enabled POCUS in the COVID-19 ICU: a new spin on cardiac ultrasound. JACC Case Rep. 2021;3(2):258–63.
Narang A, Bae R, Hong H, Thomas Y, Surette S, Cadieu C, et al. Utility of a deep-learning algorithm to guide novices to acquire echocardiograms for limited diagnostic use. JAMA Cardiol. 2021;6(6):624–32.
Asch FM, Poilvert N, Abraham T, Jankowski M, Cleve J, Adams M, et al. Automated echocardiographic quantification of left ventricular ejection fraction without volume measurements using a machine learning algorithm mimicking a human expert. Circ Cardiovasc Imaging. 2019;12(9): e009303.
Asch FM, Mor-Avi V, Rubenson D, Goldstein S, Saric M, Mikati I, et al. Deep learning-based automated echocardiographic quantification of left ventricular ejection fraction: a point-of-care solution. Circ Cardiovasc Imaging. 2021;14(6): e012293.
Liu RB, Blaivas M, Moore C, Sivitz AB, Flannigan M, Tirado A, et al. Emergency ultrasound standard reporting guidelines. 2018. https://www.acep.org/globalassets/uploads/uploaded-files/acep/clinical-and-practice-management/policy-statements/information-papers/emergency-ultrasound-standard-reporting-guidelines-2018.pdf. Accessed 30 May 2022.
Ahmed I, Sasikumar N. Echocardiography imaging techniques. In: StatPearls. December 26, 2021. https://www.ncbi.nlm.nih.gov/books/NBK572130/. Accessed 12 July 2022.
StataCorp. Stata Statistical Software: Release 15. StataCorp; 2017.
Vieillard-Baron A, Millington SJ, Sanfilippo F, Chew M, Diaz-Gomez J, McLean A, et al. A decade of progress in critical care echocardiography: a narrative review. Intensive Care Med. 2019;45(6):770–8. Erratum in: Intensive Care Med. 2019;45(6):911.
Papolos A, Narula J, Bavishi C, Chaudhry FA, Sengupta PP. U.S. hospital use of echocardiography: insights from the nationwide inpatient sample. J Am Coll Cardiol. 2016;67(5):502–11.
Raina S, Sengupta PP. AI-powered navigation system for steering POCUS in the COVID-ICU. JACC Case Rep. 2021;3(2):264–6.
Scholtz LC, Rosenberg J, Robbins MS, Wong T, Mints G, Kaplan A, et al. Ultrasonography in neurology: a comprehensive analysis and review. J Neuroimaging. 2023;33(4):511–20.
Funding
None.
Author information
Authors and Affiliations
Contributions
Authorship requirements have been met and the final manuscript was approved by all authors. Jennifer Mears contributed to the design, data collection, data analysis, and manuscript preparation. Safa Kaleem, contributed to data collection, data analysis, and manuscript preparation. Rohan Panchamia contributed to design and manuscript preparation. Hooman Kamel contributed to the design, data analysis, and manuscript preparation. Chris Tam contributed to design and manuscript preparation. Richard Thalappillil contributed to design and manuscript preparation. Santosh Murthy contributed to design, data analysis, and manuscript preparation. Alexander E. Merkler contributed to design, data analysis, and manuscript preparation. Cenai Zhang contributed to data analysis and manuscript preparation. Judy H. Ch’ang contributed to design, data collection, data analysis, and manuscript preparation.
Corresponding author
Ethics declarations
Conflicts of interest
Mears: none. Kaleem: none. Panchamia: none. Kamel: Dr. Kamel serves as a principal investigator for the National Institutes of Health–funded AtRial Cardiopathy and Antithrombotic Drugs In Prevention After Cryptogenic Stroke (ARCADIA) trial (National Institute of Neurological Disorders and Stroke grant U01NS095869), which receives in-kind study drug from the BMS-Pfizer Alliance for Eliquis and ancillary study support from Roche Diagnostics; serves as Deputy Editor for JAMA Neurology; serves on clinical trial steering/executive committees for Medtronic, Janssen, and Javelin Medical; serves on end point adjudication committees for AstraZeneca, Novo Nordisk, and Boehringer Ingelheim; and has an ownership interest in TETMedical, Inc. Tam: none. Thalappillil: none. Murthy: none. Merkler: Dr. Merkler serves as an expert witness for medicolegal cases. Zhang: none. Ch'ang: none.
Ethical Approval/Informed Consent
The Weill Cornell Medicine Institutional Review Board approved this ambidirectional analysis of data collected as part of the quality initiative.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Mears, J., Kaleem, S., Panchamia, R. et al. Leveraging the Capabilities of AI: Novice Neurology-Trained Operators Performing Cardiac POCUS in Patients with Acute Brain Injury. Neurocrit Care (2024). https://doi.org/10.1007/s12028-024-01953-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12028-024-01953-z