Abstract
Objective
An increased prevalence of vertebral fractures (VFs) has been reported in previous studies. The aim of this study was to evaluate the association between bone mineral density (BMD), bone turnover markers, serum sclerostin levels, and vertebral fractures (VFs) in acromegaly patients. We also evaluated the effects of gonadal status, disease activity, treatment modality, age, sex, and body mass index (BMI) on skeletal endpoints.
Design
Case–control study.
Patients and measurements
Seventy acromegaly patients (M/F:36/34, mean age 45.5 ± 11.9 years) and 70 controls (M/F:31/39; mean age 45.66 ± 11.9 years) were included. VFs, BMD, calcium metabolism, markers of bone turnover, and sclerostin levels were evaluated. BMD was measured by dual-energy X-ray absorptiometry (Hologic QDR 4500). Conventional lateral radiography of the spine was performed and the Genant method was used for the assessment of fractures of T4–L5 vertebrae.
Results
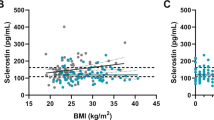
The prevalence of vertebral fractures was higher in acromegalic patients as compared with the control group (72.9 vs. 20%; p < 0.001). Serum phosphate (P) levels (3.46 ± 0.59 mg/dl vs. 3.11 ± 0.44 mg/dl; p < 0.001) and b-cross laps (CTx) levels (0.47 µg/l, range 0.04–2.38 vs. 0.28 µg/l, range 0.11–0.80; p < 0.001) were significantly higher in acromegaly patients than control subjects. Serum sclerostin levels were similar between either acromegaly patients and control subjects or acromegaly patients with VF and without VF. In the means of treatment modality, VFs were more frequent in patients treated with adjuvant gamma knife radiosurgery (GKS) (p = 0.07). In the binary logistic regression analysis, the age of the acromegaly patients, the presence of hypogonadism, and GKS treatment were the factors significantly correlated with the occurrence of spinal fractures.
Conclusions
The prevalence of VFs in patients with acromegaly is higher than in control subjects. Since advanced age, the presence of hypogonadism and GKS treatment were the factors predicting VFs in acromegaly; radiological evaluations should be considered as an emerging tool especially in those patients. Although markers of bone turnover elevated in acromegaly, they were not useful for the prediction of fractures. Serum sclerostin levels showed no discrepancy between the two groups and further studies are required for assessment of sclerostin role in this form of secondary osteoporosis.

Similar content being viewed by others
References
A. Colao, L.F.S. Grasso, A. Giustina, S. Melmed, P. Chanson, A.M. Pereira et al. Acromegaly. Nat. Rev. Dis. Prim. 5(1), 20 (2019)
M. Cellini, E. Biamonte, M. Mazza, N. Trenti, P. Ragucci, D. Milani et al. Vertebral fractures associated with spinal sagittal imbalance and quality of life in acromegaly: a radiographic study with Eos 2d/3d technology. Neuroendocrinology (2020)
G. Mazziotti, A.G.A. Lania, E. Canalis, Management of endocrine disease: bone disorders associated with acromegaly: mechanisms and treatment. Eur. J. Endocrinol. 181(2), R45–R56 (2019)
A. Giustina, G. Mazziotti, E. Canalis, Growth hormone, insulin-like growth factors, and the skeleton. Endocr. Rev. 29(5), 535–59 (2008)
S. Bonadonna, G. Mazziotti, M. Nuzzo, A. Bianchi, A. Fusco, L. De Marinis et al. Increased prevalence of radiological spinal deformities in active acromegaly: a cross-sectional study in postmenopausal women. J. Bone Min. Res. 20(10), 1837–44 (2005)
G. Mazziotti, E. Biagioli, F. Maffezzoni, M. Spinello, V. Serra, R. Maroldi et al. Bone turnover, bone mineral density, and fracture risk in acromegaly: a meta-analysis. J. Clin. Endocrinol. Metab. 100(2), 384–94 (2015)
G. Mazziotti, A. Bianchi, S. Bonadonna, V. Cimino, I. Patelli, A. Fusco et al. Prevalence of vertebral fractures in men with acromegaly. J. Clin. Endocrinol. Metab. 93(12), 4649–55 (2008)
M. Wassenaar, N. Biermasz, N. Hamdy, M. Zillikens, J. Van Meurs, F. Rivadeneira et al. High prevalence of vertebral fractures despite normal bone mineral density in patients with long-term controlled acromegaly. Eur. J. Endocrinol. 164(4), 475 (2011)
K. Claessen, H. Kroon, A. Pereira, N. Appelman-Dijkstra, M. Verstegen, M. Kloppenburg et al. Progression of vertebral fractures despite long-term biochemical control of acromegaly: a prospective follow-up study. J. Clin. Endocrinol. Metab. 98(12), 4808–15 (2013)
G. Mazziotti, A. Bianchi, T. Porcelli, M. Mormando, F. Maffezzoni, A. Cristiano et al. Vertebral fractures in patients with acromegaly: a 3-year prospective study. J. Clin. Endocrinol. Metab. 98(8), 3402–10 (2013)
A. Giustina, A. Barkan, A. Beckers, N. Biermasz, B.M.K. Biller, C. Boguszewski et al. A consensus on the diagnosis and treatment of acromegaly comorbidities: an update. J. Clin. Endocrinol. Metab. 105, 4 (2020)
J. Delgado-Calle, A.Y. Sato, T. Bellido, Role and mechanism of action of sclerostin in bone. Bone 96, 29–37 (2017)
A.R. Wijenayaka, M. Kogawa, H.P. Lim, L.F. Bonewald, D.M. Findlay, G.J. Atkins, Sclerostin stimulates osteocyte support of osteoclast activity by a RANKL-dependent pathway. PLoS ONE 6(10), e25900 (2011)
G. Holdsworth, S.J. Roberts, H.Z. Ke, Novel actions of sclerostin on bone. J. Mol. Endocrinol. 62(2), R167–R85 (2019)
M. McLung, A. Frauer, S. Boonen, Romosozumab in postmenopausal women with low bone mineral density. N. Engl. J. Med 370(5), 412–20 (2014)
K.A. Carpenter, R.D. Ross, Sclerostin antibody treatment increases bone mass and normalizes circulating phosphate levels in growing Hyp mice. J. Bone Miner. Res. 35(3), 596–607 (2020)
H.K. Genant, C.Y. Wu, C. Van Kuijk, M.C. Nevitt, Vertebral fracture assessment using a semiquantitative technique. J. Bone Miner. Res. 8(9), 1137–48 (1993)
M. Madeira, L.V. Neto, C.H. Torres, L.M.C. de Mendonça, M.R. Gadelha, M.L.F. de Farias, Vertebral fracture assessment in acromegaly. J. Clin. Densitom. 16(2), 238–43 (2013)
A. Giustina, A. Barkan, A. Beckers, N. Biermasz, B.M. Biller, C. Boguszewski et al. A consensus on the diagnosis and treatment of acromegaly comorbidities: an update. J. Clin. Endocrinol. Metab. 105(4), e937–e46 (2020)
Z. Pekkolay, F. Kılınç, N. Gozel, E. Önalan, A.K. Tuzcu, Increased serum sclerostin levels in patients with active acromegaly. J. Clin. Endocrinol. Metab. 105(3), 920–4 (2020)
J. Halupczok-Żyła, A. Jawiarczyk-Przybyłowska, A. Zembska, M. Bolanowski (eds) Sclerostin and fracture risk assessment in acromegaly. 21st European Congress of Endocrinology (BioScientifica, 2019)
B.M. Tang, G.D. Eslick, C. Nowson, C. Smith, A. Bensoussan, Use of calcium or calcium in combination with vitamin D supplementation to prevent fractures and bone loss in people aged 50 years and older: a meta-analysis. Lancet 370(9588), 657–66 (2007)
S. Chiloiro, A. Giampietro, S. Frara, C. Bima, F. Donfrancesco, C.M. Fleseriu et al. Effects of pegvisomant and pasireotide LAR on vertebral fractures in acromegaly resistant to first-generation SRLs. J. Clin. Endocrinol. Metab. 105(3), e100–e7 (2020)
M.M. Uygur, O. Deyneli, D.G. Yavuz, Long-term endocrinological outcomes of gamma knife radiosurgery in acromegaly patients. Growth Horm. IGF Res. 55, 101335 (2020)
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Uygur, M.M., Yazıcı, D.D., Buğdaycı, O. et al. Prevalence of vertebral fractures and serum sclerostin levels in acromegaly. Endocrine 73, 667–673 (2021). https://doi.org/10.1007/s12020-021-02751-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-021-02751-9