Abstract
Purpose
This study investigated trends in chronic glucocorticoid (GC) use in South Korea, and determined the association between chronic GC use and 5-year all-cause mortality.
Methods
A sample cohort was extracted from the South Korean National Health Insurance database. Patients prescribed a continuous dose of GC for ≥30 days were defined as chronic GC users. Time-dependent Cox regression was used for statistical analysis, and chronic GC exposure was considered a time-varying variable.
Results
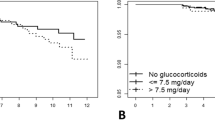
The prevalence of chronic GC use gradually increased from 0.16% in 2002 to 0.54% in 2015. In the 2010 cohort (n = 822,097), chronic GC users had a significantly 1.41-fold higher 5-year all-cause mortality compared with controls [hazard ratio: 1.41, 95% confidence interval (CI): 1.28–1.55, P < 0.001]. On sensitivity analysis, chronic high-dose GC users showed 1.52-fold (HR: 1.52, 95% CI: 1.32–1.76; P < 0.001) and low-dose GC users showed 1.34-fold (HR: 1.34, 95% CI: 1.18–1.51; P < 0·001) higher 5-year all-cause mortality, compared with controls; the disease-specific 5-year mortality risk in chronic GC users was highest due to musculoskeletal disease (HR: 9.50), followed by infectious and parasitic diseases (HR: 2.43), and respiratory disease (HR: 2.18).
Conclusions
Numbers of chronic GC users gradually increased during 2002–2015; chronic GC use increased risks of 5-year all-cause mortality in the general adult South Korean population. This association was more evident among high-dose GC users (>5 mg/day of prednisolone). The risk of disease-specific mortality among chronic GC users was increased in those with musculoskeletal, infectious and parasitic, and respiratory diseases.


Similar content being viewed by others
Data availability
The datasets generated and analyzed during the current study are available from the corresponding author on reasonable request.
References
R.A. Overman, J.Y. Yeh, C.L. Deal, Prevalence of oral glucocorticoid usage in the United States: a general population perspective. Arthritis Care Res. (Hoboken) 65(2), 294–298 (2013). https://doi.org/10.1002/acr.21796
T.P. van Staa, H.G. Leufkens, L. Abenhaim, B. Begaud, B. Zhang, C. Cooper, Use of oral corticosteroids in the United Kingdom. QJM 93(2), 105–111 (2000)
D.T. Boumpas, G.P. Chrousos, R.L. Wilder, T.R. Cupps, J.E. Balow, Glucocorticoid therapy for immune-mediated diseases: basic and clinical correlates. Ann. Intern. Med. 119(12), 1198–1208 (1993)
M. Goppelt-Struebe, D. Wolter, K. Resch, Glucocorticoids inhibit prostaglandin synthesis not only at the level of phospholipase A2 but also at the level of cyclo-oxygenase/PGE isomerase. Br. J. Pharm. 98(4), 1287–1295 (1989)
V.M. Keatings, A. Jatakanon, Y.M. Worsdell, P.J. Barnes, Effects of inhaled and oral glucocorticoids on inflammatory indices in asthma and COPD. Am. J. Respir. Crit. Care Med. 155(2), 542–548 (1997). https://doi.org/10.1164/ajrccm.155.2.9032192
A.S. Tait, C.L. Butts, E.M. Sternberg, The role of glucocorticoids and progestins in inflammatory, autoimmune, and infectious disease. J. Leukoc. Biol. 84(4), 924–931 (2008). https://doi.org/10.1189/jlb.0208104
J.M. Berthelot, Comments about the article by Mouterde et al. entitled “Indications of glucocorticoids in early arthritis and rheumatoid arthritis: Recommendations for clinical practice based on data from the literature and expert opinions”. Jt. Bone Spine 77, 597–603 (2010). Low-dose prednisone and biologics: allies rather than competitors? Joint Bone Spine 79(1), 103-104; author reply 104-106 (2012). https://doi.org/10.1016/j.jbspin.2011.09.005
S. Dimeloe, A. Nanzer, K. Ryanna, C. Hawrylowicz, Regulatory T cells, inflammation and the allergic response-The role of glucocorticoids and Vitamin D. J. Steroid. Biochem. Mol. Biol. 120(2-3), 86–95 (2010). https://doi.org/10.1016/j.jsbmb.2010.02.029
M. Bloechliger, D. Reinau, J. Spoendlin, S.C. Chang, K. Kuhlbusch, L.G. Heaney, S.S. Jick, C.R. Meier, Adverse events profile of oral corticosteroids among asthma patients in the UK: cohort study with a nested case-control analysis. Respir. Res 19(1), 75 (2018). https://doi.org/10.1186/s12931-018-0742-y
T. Volmer, T. Effenberger, C. Trautner, R. Buhl, Consequences of long-term oral corticosteroid therapy and its side-effects in severe asthma in adults: a focused review of the impact data in the literature. Eur. Respir. J. 52(4), (2018). https://doi.org/10.1183/13993003.00703-2018
S.T. Sharma, L.K. Nieman, R.A. Feelders, Cushing’s syndrome: epidemiology and developments in disease management. Clin. Epidemiol. 7, 281–293 (2015). https://doi.org/10.2147/CLEP.S44336
J. Newell-Price, X. Bertagna, A.B. Grossman, L.K. Nieman, Cushing’s syndrome. Lancet 367(9522), 1605–1617 (2006)
T.F. Mebrahtu, A.W. Morgan, A. Keeley, P.D. Baxter, P.M. Stewart, M. Pujades-Rodriguez, Dose dependency of iatrogenic glucocorticoid excess and adrenal insufficiency and mortality: a cohort study in England. J. Clin. Endocrinol. Metab. (2019). https://doi.org/10.1210/jc.2019-00153
M. Sherlock, R.C. Reulen, A.A. Alonso, J. Ayuk, R.N. Clayton, M.C. Sheppard, M.M. Hawkins, A.S. Bates, P.M. Stewart, ACTH deficiency, higher doses of hydrocortisone replacement, and radiotherapy are independent predictors of mortality in patients with acromegaly. J. Clin. Endocrinol. Metab. 94(11), 4216–4223 (2009). https://doi.org/10.1210/jc.2009-1097
H. Lee, J. Ryu, E. Nam, S. J. Chung, Y. Yeo, D.W. Park, T.S. Park, J.Y. Moon, T.H. Kim, J.W. Sohn, H.J. Yoon, S.H. Kim, Increased Mortality in Patients with Corticosteroid-dependent Asthma: A Nationwide Population-based Study. Eur. Respir J. (2019). https://doi.org/10.1183/13993003.00804-2019
A.M. Schols, G. Wesseling, A.D. Kester, G. de Vries, R. Mostert, J. Slangen, E.F. Wouters, Dose dependent increased mortality risk in COPD patients treated with oral glucocorticoids. Eur. Respir. J. 17(3), 337–342 (2001). https://doi.org/10.1183/09031936.01.17303370
M. Movahedi, R. Costello, M. Lunt, S.R. Pye, J.C. Sergeant, W.G. Dixon, Oral glucocorticoid therapy and all-cause and cause-specific mortality in patients with rheumatoid arthritis: a retrospective cohort study. Eur. J. Epidemiol. 31(10), 1045–1055 (2016). https://doi.org/10.1007/s10654-016-0167-1
J.D. Lewis, F.I. Scott, C.M. Brensinger, J.A. Roy, M.T. Osterman, R. Mamtani, M. Bewtra, L. Chen, H. Yun, F. Xie, J.R. Curtis, Increased Mortality Rates With Prolonged Corticosteroid Therapy When Compared With Antitumor Necrosis Factor-alpha-Directed Therapy for Inflammatory Bowel Disease. Am. J. Gastroenterol. 113(3), 405–417 (2018). https://doi.org/10.1038/ajg.2017.479
J.P. Vandenbroucke, E. von Elm, D.G. Altman, P.C. Gotzsche, C.D. Mulrow, S.J. Pocock, C. Poole, J.J. Schlesselman, M. Egger, S. Initiative, Strengthening the Reporting of Observational Studies in Epidemiology (STROBE): explanation and elaboration. PLoS Med. 4(10), e297 (2007). https://doi.org/10.1371/journal.pmed.0040297
R.L. Morgan, P. Whaley, K.A. Thayer, H.J. Schunemann, Identifying the PECO: A framework for formulating good questions to explore the association of environmental and other exposures with health outcomes. Environ. Int. 121(Pt 1), 1027–1031 (2018). https://doi.org/10.1016/j.envint.2018.07.015
J. Lee, J.S. Lee, S.H. Park, S.A. Shin, K. Kim, Cohort Profile: The National Health Insurance Service-National Sample Cohort (NHIS-NSC), South Korea. Int J. Epidemiol. 46(2), e15 (2017). https://doi.org/10.1093/ije/dyv319
A.W. Meikle, F.H. Tyler, Potency and duration of action of glucocorticoids. Effects of hydrocortisone, prednisone and dexamethasone on human pituitary-adrenal function. Am. J. Med. 63(2), 200–207 (1977)
I. del Rincon, D.F. Battafarano, J.F. Restrepo, J.M. Erikson, A. Escalante, Glucocorticoid dose thresholds associated with all-cause and cardiovascular mortality in rheumatoid arthritis. Arthritis Rheumatol. 66(2), 264–272 (2014). https://doi.org/10.1002/art.38210
A.B. Pedersen, E.M. Mikkelsen, D. Cronin-Fenton, N.R. Kristensen, T.M. Pham, L. Pedersen, I. Petersen, Missing data and multiple imputation in clinical epidemiological research. Clin. Epidemiol. 9, 157–166 (2017). https://doi.org/10.2147/CLEP.S129785
L. Fardet, I. Petersen, I. Nazareth, Prevalence of long-term oral glucocorticoid prescriptions in the UK over the past 20 years. Rheumatol. (Oxf.) 50(11), 1982–1990 (2011). https://doi.org/10.1093/rheumatology/ker017
L. Buckley, M.B. Humphrey, N. Glucocorticoid-Induced Osteoporosis. J. Engl. Med. 379(26), 2547–2556 (2018). https://doi.org/10.1056/NEJMcp1800214
G. Ioannidis, A. Papaioannou, W.M. Hopman, N. Akhtar-Danesh, T. Anastassiades, L. Pickard, C.C. Kennedy, J.C. Prior, W.P. Olszynski, K.S. Davison, D. Goltzman, L. Thabane, A. Gafni, E.A. Papadimitropoulos, J.P. Brown, R.G. Josse, D.A. Hanley, J.D. Adachi, Relation between fractures and mortality: results from the Canadian Multicentre Osteoporosis Study. CMAJ 181(5), 265–271 (2009). https://doi.org/10.1503/cmaj.081720
J.R. Center, T.V. Nguyen, D. Schneider, P.N. Sambrook, J.A. Eisman, Mortality after all major types of osteoporotic fracture in men and women: an observational study. Lancet 353(9156), 878–882 (1999). https://doi.org/10.1016/S0140-6736(98)09075-8
S.S. Jick, E.S. Lieberman, M.U. Rahman, H.K. Choi, Glucocorticoid use, other associated factors, and the risk of tuberculosis. Arthritis Rheum. 55(1), 19–26 (2006). https://doi.org/10.1002/art.21705
K.S. Cho, Tuberculosis control in the Republic of Korea. Epidemiol. Health 40, e2018036 (2018). https://doi.org/10.4178/epih.e2018036
P. Brassard, A. Bitton, A. Suissa, L. Sinyavskaya, V. Patenaude, S. Suissa, Oral corticosteroids and the risk of serious infections in patients with elderly-onset inflammatory bowel diseases. Am. J. Gastroenterol. 109(11), 1795–1802 (2014). https://doi.org/10.1038/ajg.2014.313. quiz 1803
L. Fardet, I. Petersen, I. Nazareth, Common Infections in Patients Prescribed Systemic Glucocorticoids in Primary Care: A Population-Based Cohort Study. PLoS Med. 13(5), e1002024 (2016). https://doi.org/10.1371/journal.pmed.1002024
Author contributions
T.K.O. and I.A.S. contributed to the study design, methodology, analyzed the data, and drafted the first paper. All authors read and approved the final version of the paper.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The study protocol was approved by the Institutional Review Board of Seoul National University Bundang Hospital (X-1903-531-901) and the Health Insurance Review and Assessment Service (NHIS-2019-2-140). The requirement for informed consent was waived, because the study included anonymized data from the National Health Insurance Service (NHIS).
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Oh, T.K., Song, IA. Trends in long-term glucocorticoid use and risk of 5-year mortality: a historical cohort study in South Korea. Endocrine 69, 634–641 (2020). https://doi.org/10.1007/s12020-020-02382-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-020-02382-6