Abstract
MicroRNAs (miRNAs) and long non-coding RNAs (lncRNAs) are two important types of non-coding RNAs that are not translated into protein. These molecules can regulate various biological processes, including stem cell differentiation and self-renewal. One of the first known miRNAs in mammals is miR-21. Cancer-related studies have shown that this miRNA has proto-oncogene activity and is elevated in cancers. However, it is confirmed that miR-21 inhibits stem cell pluripotency and self-renewal and induces differentiation by targeting various genes. Regenerative medicine is a field of medical science that tries to regenerate and repair damaged tissues. Various studies have shown that miR-21 plays an essential role in regenerative medicine by affecting stem cell proliferation and differentiation. In this review, we will discuss the function of miR-21 in regenerative medicine of the liver, nerve, spinal cord, wound, bone, and dental tissues. In addition, the function of natural compounds and lncRNAs will be analyzed as potential regulators of miR-21 expression in regenerative medicine.
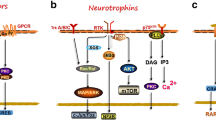
Graphical Abstract





Similar content being viewed by others
Data Availability
Available upon request.
Code Availability (software application or custom code)
Not applicable.
References
Kalhori, M. R., Soleimani, M., Arefian, E., Alizadeh, A. M., Mansouri, K., et al. (2022). The potential role of miR-1290 in cancer progression, diagnosis, prognosis, and treatment: an oncomiR or onco-suppressor microRNA? Journal of Cellular Biochemistry, 123(3), 506–531. https://doi.org/10.1002/jcb.30191
Kalhori, M. R., Soleimani, M., Yari, K., Moradi, M., & Kalhori, A. A. (2022). MiR-1290: a potential therapeutic target for regenerative medicine or diagnosis and treatment of non-malignant diseases. Clinical and Experimental Medicine. https://doi.org/10.1007/s10238-022-00854-9
Jacques, E., & Suuronen, E. J. (2020). The progression of regenerative medicine and its impact on therapy translation. Clinical and Translational Science, 13(3), 440–450. https://doi.org/10.1111/cts.12736
Mao, A. S., & Mooney, D. J. (2015). Regenerative medicine: current therapies and future directions. Proceedings of the National Academy of Sciences of the United States of America, 112(47), 14452–14459. https://doi.org/10.1073/pnas.1508520112
Hayes, M., Curley, G., Ansari, B., & Laffey, J. G. (2012). Clinical review: stem cell therapies for acute lung injury/acute respiratory distress syndrome - hope or hype? Critical Care, 16(2), 205. https://doi.org/10.1186/cc10570
Bacakova, L., Zarubova, J., Travnickova, M., Musilkova, J., Pajorova, J., et al. (2018). Stem cells: their source, potency and use in regenerative therapies with focus on adipose-derived stem cells - a review. Biotechnology Advances, 36(4), 1111–1126. https://doi.org/10.1016/j.biotechadv.2018.03.011
Yu, Z., Li, Y., Fan, H., Liu, Z., & Pestell, R. G. (2012). miRNAs regulate stem cell self-renewal and differentiation. Frontiers in Genetics, 3, 191. https://doi.org/10.3389/fgene.2012.00191
Lakshmipathy, U., Love, B., Goff, L. A., Jörnsten, R., Graichen, R., et al. (2007). MicroRNA expression pattern of undifferentiated and differentiated human embryonic stem cells. Stem Cells and Development, 16(6), 1003–1016. https://doi.org/10.1089/scd.2007.0026
Houbaviy, H. B., Murray, M. F., & Sharp, P. A. (2003). Embryonic stem cell-specific MicroRNAs. Developmental Cell, 5(2), 351–358. https://doi.org/10.1016/s1534-5807(03)00227-2
Jenike, A. E., & Halushka, M. K. (2021). miR-21: a non-specific biomarker of all maladies. Biomarker Research, 9(1), 18. https://doi.org/10.1186/s40364-021-00272-1
Lam, D. K., & Schmidt, B. L. (2012). Molecular biology of head and neck cancer: therapeutic implications. Current Therapy in Oral and Maxillofacial Surgery (pp. 92–101). Elsevier Inc.
Sachdeva, M., Zhu, S., & Mo, Y. Y. (2010). MicroRNA-21 as a novel therapeutic target. Current Cancer Therapy Reviews, 6(1), 41–50. https://doi.org/10.2174/157339410790596452
Liu, Y., Liu, J., Xia, T., Mi, B. B., Xiong, Y., et al. (2019). MiR-21 promotes fracture healing by activating the PI3K/Akt signaling pathway. European Review for Medical and Pharmacological Sciences, 23(7), 2727–2733. https://doi.org/10.26355/eurrev_201904_17544
Song, G., Sharma, A. D., Roll, G. R., Ng, R., Lee, A. Y., et al. (2010). MicroRNAs control hepatocyte proliferation during liver regeneration. Hepatology, 51(5), 1735–1743. https://doi.org/10.1002/hep.23547
Zhang, W. M., Zhang, Z. R., Yang, X. T., Zhang, Y. G., & Gao, Y. S. (2018). Overexpression of miR–21 promotes neural stem cell proliferation and neural differentiation via the Wnt/β–catenin signaling pathway in vitro. Molecular Medicine Reports, 17(1), 330–335. https://doi.org/10.3892/mmr.2017.7856
Ni, Y., Zhang, K., Liu, X., Yang, T., Wang, B., et al. (2014). miR-21 promotes the differentiation of hair follicle-derived neural crest stem cells into Schwann cells. Neural Regeneration Research, 9(8), 828–836. https://doi.org/10.4103/1673-5374.131599
Gao, X., Li, X., Qian, C., Li, F., Zhang, Y., et al. (2016). MiR-21 functions oppositely in proliferation and differentiation of neural stem/precursor cells via regulating AKT and GSK-3β. Cellular and Molecular Biology (Noisy-le-Grand, France), 62(12), 144–149. https://doi.org/10.14715/cmb/2016.62.12.24
Yang, L., Shen, X. M., Wang, Z. F., Li, K., & Wang, W. (2021). The notch signalling pathway and miRNA regulation play important roles in the differentiation of Schwann cells from adipose-derived stem cells. Laboratory Investigation. https://doi.org/10.1038/s41374-021-00687-2
Liu, Y., Zhang, X., Gao, C., Zhang, H., Zhang, H., et al. (2020). MicroRNA124 and microRNA21-5p regulate migration, proliferation and differentiation of rat bone marrow mesenchymal stem cells. Bioscience Reports, 40(10). https://doi.org/10.1042/bsr20193531
Chen, Z., Dai, T., Chen, X., Tan, L., & Shi, C. (2015). Activation and regulation of the granulation tissue derived cells with stemness-related properties. Stem Cell Research & Therapy, 6(1), 85. https://doi.org/10.1186/s13287-015-0070-9
Li, Q., Zhao, H., Chen, W., Huang, P., & Bi, J. (2019). Human keratinocyte-derived microvesicle miRNA-21 promotes skin wound healing in diabetic rats through facilitating fibroblast function and angiogenesis. International Journal of Biochemistry & Cell Biology, 114, 105570. https://doi.org/10.1016/j.biocel.2019.105570
Trohatou, O., Zagoura, D., Bitsika, V., Pappa, K. I., Antsaklis, A., et al. (2014). Sox2 suppression by miR-21 governs human mesenchymal stem cell properties. Stem Cells Translational Medicine, 3(1), 54–68. https://doi.org/10.5966/sctm.2013-0081
Sun, Y., Xu, L., Huang, S., Hou, Y., Liu, Y., et al. (2015). mir-21 overexpressing mesenchymal stem cells accelerate fracture healing in a rat closed femur fracture model. BioMed Research International, 2015, 412327. https://doi.org/10.1155/2015/412327
Meng, Y. B., Li, X., Li, Z. Y., Zhao, J., Yuan, X. B., Ren, Y., Cui, Z. D., Liu, Y. D., & Yang, X. J. (2015). MicroRNA-21 promotes osteogenic differentiation of mesenchymal stem cells by the PI3K/β-catenin pathway. Journal of Orthopaedic Research, 33(7), 957–964. https://doi.org/10.1002/jor.22884
Mei, Y., Bian, C., Li, J., Du, Z., Zhou, H., Yang, Z., & Zhao, R. C. (2013). MiR-21 modulates the ERK-MAPK signaling pathway by regulating SPRY2 expression during human mesenchymal stem cell differentiation. Journal of Cellular Biochemistry, 114(6), 1374–1384. https://doi.org/10.1002/jcb.24479
Zhang, D., Ran, J., Li, J., Yu, C., Cui, Z., Amevor, F. K., Wang, Y., Jiang, X., Qiu, M., Du, H., et al. (2021). MiR-21-5p regulates the proliferation and differentiation of skeletal muscle satellite cells by targeting KLF3 in chicken. Genes (Basel), 12(6). https://doi.org/10.3390/genes12060814
Bai, C., Li, X., Gao, Y., Wang, K., Fan, Y., Zhang, S., Ma, Y., & Guan, W. (2016). Role of microRNA-21 in the formation of insulin producing cells from pancreatic progenitor cells. Biochimica et Biophysica Acta, 1859(2), 280–293. https://doi.org/10.1016/j.bbagrm.2015.12.001
Surina, S., Fontanella, R. A., Scisciola, L., Marfella, R., Paolisso, G., & Barbieri, M. (2021). miR-21 in human cardiomyopathies. Frontiers in Cardiovascular Medicine, 8, 767064. https://doi.org/10.3389/fcvm.2021.767064
Fujita, S., Ito, T., Mizutani, T., Minoguchi, S., Yamamichi, N., Sakurai, K., & Iba, H. (2008). miR-21 gene expression triggered by AP-1 is sustained through a double-negative feedback mechanism. Journal of Molecular Biology, 378(3), 492–504. https://doi.org/10.1016/j.jmb.2008.03.015
Bezinover, D., & Saner, F. (2019). Organ transplantation in the modern era. BMC Anesthesiology, 19(1), 32. https://doi.org/10.1186/s12871-019-0704-z
Marquez, R. T., Wendlandt, E., Galle, C. S., Keck, K., & McCaffrey, A. P. (2010). MicroRNA-21 is upregulated during the proliferative phase of liver regeneration, targets Pellino-1, and inhibits NF-kappaB signaling. American Journal of Physiology-Gastrointestinal and Liver Physiology, 298(4), G535–G541. https://doi.org/10.1152/ajpgi.00338.2009
Ng, R., Song, G., Roll, G. R., Frandsen, N. M., & Willenbring, H. (2012). A microRNA-21 surge facilitates rapid cyclin D1 translation and cell cycle progression in mouse liver regeneration. The Journal of Clinical Investigation, 122(3), 1097–1108. https://doi.org/10.1172/jci46039
Bai, Y. N., Yu, Z. Y., Luo, L. X., Yi, J., Xia, Q. J., & Zeng, Y. (2014). MicroRNA-21 accelerates hepatocyte proliferation in vitro via PI3K/Akt signaling by targeting PTEN. Biochemical and Biophysical Research Communications, 443(3), 802–807. https://doi.org/10.1016/j.bbrc.2013.12.047
Li, J. J., Chan, W. H., Leung, W. Y., Wang, Y., & Xu, C. S. (2015). MicroRNA-21 promotes proliferation of rat hepatocyte BRL-3A by targeting FASLG. Genetics and Molecular Research, 14(2), 4150–4160. https://doi.org/10.4238/2015.April.27.30
Dippold, R. P., Vadigepalli, R., Gonye, G. E., & Hoek, J. B. (2012). Chronic ethanol feeding enhances miR-21 induction during liver regeneration while inhibiting proliferation in rats. American Journal of Physiology-Gastrointestinal and Liver Physiology, 303(6), G733–G743. https://doi.org/10.1152/ajpgi.00019.2012
Juskeviciute, E., Dippold, R. P., Antony, A. N., Swarup, A., Vadigepalli, R., & Hoek, J. B. (2016). Inhibition of miR-21 rescues liver regeneration after partial hepatectomy in ethanol-fed rats. American Journal of Physiology-Gastrointestinal and Liver Physiology, 311(5), G794–g806. https://doi.org/10.1152/ajpgi.00292.2016
Parrish, A., Srivastava, A., Juskeviciute, E., Hoek, J. B., & Vadigepalli, R. (2021). Dysregulation of miR-21-associated miRNA regulatory networks by chronic ethanol consumption impairs liver regeneration. Physiological Genomics, 53(12), 546–555. https://doi.org/10.1152/physiolgenomics.00113.2021
Maugeri, G., D'Amico, A. G., Musumeci, G., Reglodi, D., & D'Agata, V. (2020). Effects of Pacap on Schwann cells: Focus on nerve injury. International Journal of Molecular Sciences, 21(21). https://doi.org/10.3390/ijms21218233
Strickland, I. T., Richards, L., Holmes, F. E., Wynick, D., Uney, J. B., & Wong, L. F. (2011). Axotomy-induced miR-21 promotes axon growth in adult dorsal root ganglion neurons. PLoS One, 6(8), e23423. https://doi.org/10.1371/journal.pone.0023423
Christie, K. J., Webber, C. A., Martinez, J. A., Singh, B., & Zochodne, D. W. (2010). PTEN inhibition to facilitate intrinsic regenerative outgrowth of adult peripheral axons. The Journal of Neuroscience, 30(27), 9306–9315. https://doi.org/10.1523/jneurosci.6271-09.2010
Kar, A. N., Lee, S. J., Sahoo, P. K., Thames, E., Yoo, S., Houle, J. D., & Twiss, J. L. (2021). MicroRNAs 21 and 199a-3p regulate axon growth potential through modulation of Pten and mTor mRNAs. eNeuro, 8(4). https://doi.org/10.1523/eneuro.0155-21.2021
Ning, X. J., Lu, X. H., Luo, J. C., Chen, C., Gao, Q., Li, Z. Y., & Wang, H. (2020). Molecular mechanism of microRNA-21 promoting Schwann cell proliferation and axon regeneration during injured nerve repair. RNA Biology, 17(10), 1508–1519. https://doi.org/10.1080/15476286.2020.1777767
Ma, Y., Zhou, D., Zhang, H., Tang, L., Qian, F., & Su, J. (2021). Human umbilical cord mesenchymal stem cell-derived extracellular vesicles promote the proliferation of Schwann cells by regulating the PI3K/AKT signaling pathway via transferring miR-21. Stem Cells International, 2021, 1496101. https://doi.org/10.1155/2021/1496101
Yousefifard, M., Rahimi-Movaghar, V., Nasirinezhad, F., Baikpour, M., Safari, S., Saadat, S., Moghadas Jafari, A., Asady, H., Razavi Tousi, S. M., & Hosseini, M. (2016). Neural stem/progenitor cell transplantation for spinal cord injury treatment; A systematic review and meta-analysis. Neuroscience, 322, 377–397. https://doi.org/10.1016/j.neuroscience.2016.02.034
Chen, R., Liu, Y., Su, Q., Yang, Y., Wang, L., Ma, S., Yan, J., Xue, F., & Wang, J. (2017). Hypoxia stimulates proliferation of rat neural stem/progenitor cells by regulating mir-21: An in vitro study. Neuroscience Letters, 661, 71–76. https://doi.org/10.1016/j.neulet.2017.09.037
Su, Z., Yuan, Y., Chen, J., Zhu, Y., Qiu, Y., Zhu, F., Huang, A., & He, C. (2011). Reactive astrocytes inhibit the survival and differentiation of oligodendrocyte precursor cells by secreted TNF-α. Journal of Neurotrauma, 28(6), 1089–1100. https://doi.org/10.1089/neu.2010.1597
Li, H. J., Pan, Y. B., Sun, Z. L., Sun, Y. Y., Yang, X. T., & Feng, D. F. (2018). Inhibition of miR-21 ameliorates excessive astrocyte activation and promotes axon regeneration following optic nerve crush. Neuropharmacology, 137, 33–49. https://doi.org/10.1016/j.neuropharm.2018.04.028
Chen, R., Tai, Y., Zhang, Y., Wang, L., Yang, Y., Yang, N., Ma, S., Xue, F., & Wang, J. (2019). MicroRNA-21 attenuates oxygen and glucose deprivation induced apoptotic death in human neural stem cells with inhibition of JNK and p38 MAPK signaling. Neuroscience Letters, 690, 11–16. https://doi.org/10.1016/j.neulet.2018.09.060
Pelisch, N., Rosas Almanza, J., Stehlik, K. E., Aperi, B. V., & Kroner, A. (2020). CCL3 contributes to secondary damage after spinal cord injury. Journal of Neuroinflammation, 17(1), 362. https://doi.org/10.1186/s12974-020-02037-3
Liu, J., Zhang, S., Huang, Y., & Sun, L. (2020). miR-21 protects neonatal rats from hypoxic-ischemic brain damage by targeting CCL3. Apoptosis, 25(3–4), 275–289. https://doi.org/10.1007/s10495-020-01596-3
Xie, W., Yang, S. Y., Zhang, Q., Zhou, Y., Wang, Y., Liu, R., Wang, W., Shi, J., Ning, B., & Jia, T. (2018). Knockdown of MicroRNA- 21 promotes neurological recovery after acute spinal cord injury. Neurochemical Research, 43(8), 1641–1649. https://doi.org/10.1007/s11064-018-2580-1
Su, Y., Chen, Z., Du, H., Liu, R., Wang, W., Li, H., & Ning, B. (2019). Silencing miR-21 induces polarization of astrocytes to the A2 phenotype and improves the formation of synapses by targeting glypican 6 via the signal transducer and activator of transcription- 3 pathway after acute ischemic spinal cord injury. The FASEB Journal, 33(10), 10859–10871. https://doi.org/10.1096/fj.201900743R
Venkatesh, K., Ghosh, S. K., Mullick, M., Manivasagam, G., & Sen, D. (2019). Spinal cord injury: Pathophysiology, treatment strategies, associated challenges, and future implications. Cell and Tissue Research, 377(2), 125–151. https://doi.org/10.1007/s00441-019-03039-1
Liu, R., Wang, W., Wang, S., Xie, W., Li, H., & Ning, B. (2018). MicroRNA-21 regulates astrocytic reaction post-acute phase of spinal cord injury through modulating TGF-β signaling. Aging (Albany NY), 10(6), 1474–1488. https://doi.org/10.18632/aging.101484
Bhalala, O. G., Pan, L., Sahni, V., McGuire, T. L., Gruner, K., Tourtellotte, W. G., & Kessler, J. A. (2012). MicroRNA-21 regulates astrocytic response following spinal cord injury. The Journal of Neuroscience, 32(50), 17935–17947. https://doi.org/10.1523/jneurosci.3860-12.2012
Wang, W., Liu, R., Su, Y., Li, H., Xie, W., & Ning, B. (2018). MicroRNA-21-5p mediates TGF-β-regulated fibrogenic activation of spinal fibroblasts and the formation of fibrotic scars after spinal cord injury. International Journal of Biological Sciences, 14(2), 178–188. https://doi.org/10.7150/ijbs.24074
Yao, C., Wang, J., Zhang, H., Zhou, S., Qian, T., Ding, F., Gu, X., & Yu, B. (2015). Long non-coding RNA uc.217 regulates neurite outgrowth in dorsal root ganglion neurons following peripheral nerve injury. The European Journal of Neuroscience, 42(1), 1718–1725. https://doi.org/10.1111/ejn.12966
Liu, Z. H., Yip, P. K., Adams, L., Davies, M., Lee, J. W., Michael, G. J., Priestley, J. V., & Michael-Titus, A. T. (2015). A single bolus of docosahexaenoic acid promotes neuroplastic changes in the innervation of spinal cord interneurons and motor neurons and improves functional recovery after spinal cord injury. The Journal of Neuroscience, 35(37), 12733–12752. https://doi.org/10.1523/jneurosci.0605-15.2015
Jiang, Y., Zhao, S., Ding, Y., Nong, L., Li, H., Gao, G., Zhou, D., & Xu, N. (2017). MicroRNA-21 promotes neurite outgrowth by regulating PDCD4 in a rat model of spinal cord injury. Molecular Medicine Reports, 16(3), 2522–2528. https://doi.org/10.3892/mmr.2017.6862
Huang, J. H., Yin, X. M., Xu, Y., Xu, C. C., Lin, X., Ye, F. B., Cao, Y., & Lin, F. Y. (2017). Systemic administration of exosomes released from mesenchymal stromal cells attenuates apoptosis, inflammation, and promotes angiogenesis after spinal cord injury in rats. Journal of Neurotrauma, 34(24), 3388–3396. https://doi.org/10.1089/neu.2017.5063
Kang, J., Li, Z., Zhi, Z., Wang, S., & Xu, G. (2019). MiR-21 derived from the exosomes of MSCs regulates the death and differentiation of neurons in patients with spinal cord injury. Gene Therapy, 26(12), 491–503. https://doi.org/10.1038/s41434-019-0101-8
Xu, G., Ao, R., Zhi, Z., Jia, J., & Yu, B. (2019). MiR-21 and miR-19b delivered by hMSC-derived EVs regulate the apoptosis and differentiation of neurons in patients with spinal cord injury. Journal of Cellular Physiology, 234(7), 10205–10217. https://doi.org/10.1002/jcp.27690
Zhou, X., Chu, X., Yuan, H., Qiu, J., Zhao, C., Xin, D., Li, T., Ma, W., Wang, H., Wang, Z., et al. (2019). Mesenchymal stem cell derived EVs mediate neuroprotection after spinal cord injury in rats via the microRNA-21-5p/FasL gene axis. Biomedicine & Pharmacotherapy, 115, 108818. https://doi.org/10.1016/j.biopha.2019.108818
Ji, W., Jiang, W., Li, M., Li, J., & Li, Z. (2019). miR-21 deficiency contributes to the impaired protective effects of obese rat mesenchymal stem cell-derived exosomes against spinal cord injury. Biochimie, 167, 171–178. https://doi.org/10.1016/j.biochi.2019.10.002
Chang, M., & Nguyen, T. T. (2021). Strategy for treatment of infected diabetic foot ulcers. Accounts of Chemical Research, 54(5), 1080–1093. https://doi.org/10.1021/acs.accounts.0c00864
Xie, J., Wu, W., Zheng, L., Lin, X., Tai, Y., Wang, Y., & Wang, L. (2022). Roles of MicroRNA-21 in skin wound healing: A comprehensive review. Frontiers in Pharmacology, 13, 828627. https://doi.org/10.3389/fphar.2022.828627
Yang, X., Wang, J., Guo, S. L., Fan, K. J., Li, J., Wang, Y. L., Teng, Y., & Yang, X. (2011). MiR-21 promotes keratinocyte migration and re-epithelialization during wound healing. International Journal of Biological Sciences, 7(5), 685–690. https://doi.org/10.7150/ijbs.7.685
Liu, Y., Li, Y., Li, N., Teng, W., Wang, M., Zhang, Y., & Xiao, Z. (2016). TGF-β1 promotes scar fibroblasts proliferation and trans differentiation via up-regulating MicroRNA-21. Scientific Reports, 6, 32231. https://doi.org/10.1038/srep32231
Madhyastha, R., Madhyastha, H., Nakajima, Y., Omura, S., & Maruyama, M. (2012). MicroRNA signature in diabetic wound healing: Promotive role of miR-21 in fibroblast migration. International Wound Journal, 9(4), 355–361. https://doi.org/10.1111/j.1742-481X.2011.00890.x
Madhyastha, R., Madhyastha, H., Pengjam, Y., Nakajima, Y., Omura, S., & Maruyama, M. (2014). NFkappaB activation is essential for miR-21 induction by TGFβ1 in high glucose conditions. Biochemical and Biophysical Research Communications, 451(4), 615–621. https://doi.org/10.1016/j.bbrc.2014.08.035
Zhang, Y., Pan, Y., Liu, Y., Li, X., Tang, L., Duan, M., Li, J., & Zhang, G. (2021). Exosomes derived from human umbilical cord blood mesenchymal stem cells stimulate regenerative wound healing via transforming growth factor-β receptor inhibition. Stem Cell Research & Therapy, 12(1), 434. https://doi.org/10.1186/s13287-021-02517-0
Yang, C., Luo, L., Bai, X., Shen, K., Liu, K., Wang, J., & Hu, D. (2020). Highly-expressed micoRNA-21 in adipose derived stem cell exosomes can enhance the migration and proliferation of the HaCaT cells by increasing the MMP-9 expression through the PI3K/AKT pathway. Archives of Biochemistry and Biophysics, 681, 108259. https://doi.org/10.1016/j.abb.2020.108259
Wang, T., Feng, Y., Sun, H., Zhang, L., Hao, L., Shi, C., Wang, J., Li, R., Ran, X., Su, Y., et al. (2012). miR-21 regulates skin wound healing by targeting multiple aspects of the healing process. The American Journal of Pathology, 181(6), 1911–1920. https://doi.org/10.1016/j.ajpath.2012.08.022
Das, A., Ganesh, K., Khanna, S., Sen, C. K., & Roy, S. (2014). Engulfment of apoptotic cells by macrophages: A role of microRNA-21 in the resolution of wound inflammation. Journal of Immunology, 192(3), 1120–1129. https://doi.org/10.4049/jimmunol.1300613
Ma, R., Li, X., Tewari, N., Liu, Y., Bhawal, U. K., & Zeng, X. (2020). MicroRNA-21 ameliorates the impairment of autophagy in palatal wound healing. Journal of Physiology and Pharmacology, 71(6), 10.26402/jpp.2020.6.14.
Hu, Y., Rao, S. S., Wang, Z. X., Cao, J., Tan, Y. J., Luo, J., Li, H. M., Zhang, W. S., Chen, C. Y., & Xie, H. (2018). Exosomes from human umbilical cord blood accelerate cutaneous wound healing through miR-21-3p-mediated promotion of angiogenesis and fibroblast function. Theranostics, 8(1), 169–184. https://doi.org/10.7150/thno.21234
Huang, C., Luo, W., Wang, Q., Ye, Y., Fan, J., Lin, L., Shi, C., Wei, W., Chen, H., Wu, Y., et al. (2021). Human mesenchymal stem cells promote ischemic repairment and angiogenesis of diabetic foot through exosome miRNA-21-5p. Stem Cell Research, 52, 102235. https://doi.org/10.1016/j.scr.2021.102235
Liu, S. C., Bamodu, O. A., Kuo, K. T., Fong, I. H., Lin, C. C., Yeh, C. T., & Chen, S. G. (2021). Adipose-derived stem cell induced-tissue repair or wound healing is mediated by the concomitant upregulation of miR-21 and miR-29b expression and activation of the AKT signaling pathway. Archives of Biochemistry and Biophysics, 705, 108895. https://doi.org/10.1016/j.abb.2021.108895
Pastar, I., Khan, A. A., Stojadinovic, O., Lebrun, E. A., Medina, M. C., Brem, H., Kirsner, R. S., Jimenez, J. J., Leslie, C., & Tomic-Canic, M. (2012). Induction of specific microRNAs inhibits cutaneous wound healing. The Journal of Biological Chemistry, 287(35), 29324–29335. https://doi.org/10.1074/jbc.M112.382135
Liang, L., Stone, R. C., Stojadinovic, O., Ramirez, H., Pastar, I., Maione, A. G., Smith, A., Yanez, V., Veves, A., Kirsner, R. S., et al. (2016). Integrative analysis of miRNA and mRNA paired expression profiling of primary fibroblast derived from diabetic foot ulcers reveals multiple impaired cellular functions. Wound Repair and Regeneration, 24(6), 943–953. https://doi.org/10.1111/wrr.12470
Han, Z., Chen, Y., Zhang, Y., Wei, A., Zhou, J., Li, Q., & Guo, L. (2017). MiR-21/PTEN axis promotes skin wound healing by dendritic cells enhancement. Journal of Cellular Biochemistry, 118(10), 3511–3519. https://doi.org/10.1002/jcb.26026
Li, X., Guo, L., Liu, Y., Su, Y., Xie, Y., Du, J., Wang, S., Wang, H., & Liu, Y. (2018). MicroRNA-21 promotes wound healing via the Smad7-Smad2/3-elastin pathway. Experimental Cell Research, 362(2), 245–251. https://doi.org/10.1016/j.yexcr.2017.11.019
Wu, Y., K. Zhang, R. Liu, H. Zhang, D. Chen, S. Yu, W. Chen, S. Wan, Y. Zhang, Z. Jia, et al. (2020). MicroRNA-21-3p accelerates diabetic wound healing in mice by downregulating SPRY1. Aging 12(15), 15436–15445. https://doi.org/10.18632/aging.103610
Wu, D., Kang, L., Tian, J., Wu, Y., Liu, J., Li, Z., Wu, X., Huang, Y., Gao, B., Wang, H., et al. (2020). Exosomes derived from bone mesenchymal stem cells with the stimulation of Fe(3)O(4) nanoparticles and static magnetic field enhance wound healing through upregulated miR-21-5p. International Journal of Nanomedicine, 15, 7979–7993. https://doi.org/10.2147/ijn.s275650
Li, J., Wei, C., Yang, Y., Gao, Z., Guo, Z., & Qi, F. (2022). Apoptotic bodies extracted from adipose mesenchymal stem cells carry microRNA-21-5p to induce M2 polarization of macrophages and augment skin wound healing by targeting KLF6. Burns. https://doi.org/10.1016/j.burns.2021.12.010
Brahmbhatt, H. D., Gupta, R., Gupta, A., Rastogi, S., Subramani, D., Mobeen, A., Batra, V. V., & Singh, A. (2022). Differential regulation of miR-21-5p delays wound healing of melanocyte-deprived vitiligo skin by modulating the expression of tumor suppressors PDCD4 and Maspin. Journal of Cellular Physiology, 237(2), 1429–1439. https://doi.org/10.1002/jcp.30614
Li, H., Yang, F., Wang, Z., Fu, Q., & Liang, A. (2015). MicroRNA-21 promotes osteogenic differentiation by targeting small mothers against decapentaplegic 7. Molecular Medicine Reports, 12(1), 1561–1567. https://doi.org/10.3892/mmr.2015.3497
Song, Q., Zhong, L., Chen, C., Tang, Z., Liu, H., Zhou, Y., Tang, M., Zhou, L., Zuo, G., Luo, J., et al. (2015). miR-21 synergizes with BMP9 in osteogenic differentiation by activating the BMP9/Smad signaling pathway in murine multilineage cells. International Journal of Molecular Medicine, 36(6), 1497–1506. https://doi.org/10.3892/ijmm.2015.2363
Li, L., & Jiang, D. (2019). Hypoxia-responsive miRNA-21-5p inhibits Runx2 suppression by targeting SMAD7 in MC3T3-E1 cells. Journal of Cellular Biochemistry, 120(10), 16867–16875. https://doi.org/10.1002/jcb.28944
Yang, N., Wang, G., Hu, C., Shi, Y., Liao, L., Shi, S., Cai, Y., Cheng, S., Wang, X., Liu, Y., et al. (2013). Tumor necrosis factor α suppresses the mesenchymal stem cell osteogenesis promoter miR-21 in estrogen deficiency-induced osteoporosis. Journal of Bone and Mineral Research, 28(3), 559–573. https://doi.org/10.1002/jbmr.1798
Zhao, W., Dong, Y., Wu, C., Ma, Y., Jin, Y., & Ji, Y. (2015). MiR-21 overexpression improves osteoporosis by targeting RECK. Molecular and Cellular Biochemistry, 405(1–2), 125–133. https://doi.org/10.1007/s11010-015-2404-4
Huang, Y., Yang, Y., Wang, J., Yao, S., Yao, T., Xu, Y., Chen, Z., Yuan, P., Gao, J., Shen, S., et al. (2021). miR-21-5p targets SKP2 to reduce osteoclastogenesis in a mouse model of osteoporosis. The Journal of Biological Chemistry, 296, 100617. https://doi.org/10.1016/j.jbc.2021.100617
Lee, K. S., Lee, J., Kim, H. K., Yeom, S. H., Woo, C. H., Jung, Y. J., Yun, Y. E., Park, S. Y., Han, J., Kim, E., et al. (2021). Extracellular vesicles from adipose tissue-derived stem cells alleviate osteoporosis through osteoprotegerin and miR-21-5p. J Extracell Vesicles, 10(12), e12152. https://doi.org/10.1002/jev2.12152
Zhou, Y., Qiao, H., Liu, L., Dong, P., Zhu, F., Zhang, J., Liu, L., & Liu, L. (2021). MiR-21 regulates osteogenic and adipogenic differentiation of BMSCs by targeting PTEN. Journal of Musculoskeletal & Neuronal Interactions, 21(4), 568–576.
Wu, P. Y., Chen, W., Huang, H., Tang, W., & Liang, J. (2022). Morinda officinalis polysaccharide regulates rat bone mesenchymal stem cell osteogenic-adipogenic differentiation in osteoporosis by upregulating miR-21 and activating the PI3K/AKT pathway. The Kaohsiung Journal of Medical Sciences, 38(7), 675–685. https://doi.org/10.1002/kjm2.12544
You, M., Ai, Z., Zeng, J., Fu, Y., Zhang, L., & Wu, X. (2022). Bone mesenchymal stem cells (BMSCs)-derived exosomal microRNA-21-5p regulates Kruppel-like factor 3 (KLF3) to promote osteoblast proliferation in vitro. Bioengineered, 13(5), 11933–11944. https://doi.org/10.1080/21655979.2022.2067286
Zhao, G., Luo, W. D., Yuan, Y., Lin, F., Guo, L. M., Ma, J. J., Chen, H. B., Tang, H., & Shu, J. (2022). LINC02381, a sponge of miR-21, weakens osteogenic differentiation of hUC-MSCs through KLF12-mediated Wnt4 transcriptional repression. Journal of Bone and Mineral Metabolism, 40(1), 66–80. https://doi.org/10.1007/s00774-021-01277-4
Fang, S., Liu, Z., Wu, S., Chen, X., You, M., Li, Y., Yang, F., Zhang, S., Lai, Y., Liu, P., et al. (2022). Pro-angiognetic and pro-osteogenic effects of human umbilical cord mesenchymal stem cell-derived exosomal miR-21-5p in osteonecrosis of the femoral head. Cell Death Discovery, 8(1), 226. https://doi.org/10.1038/s41420-022-00971-0
Wu, Y., Zhang, Z., Li, J., Zhong, H., Yuan, R., Deng, Z., & Wu, X. (2021). Mechanism of adipose-derived mesenchymal stem cell- derived extracellular vesicles carrying miR-21-5p in hyperoxia-induced lung injury. Stem Cell Reviews and Reports. https://doi.org/10.1007/s12015-021-10311-x
Bao, P., Zhao, W., Mou, M., & Liu, X. (2020). MicroRNA-21 mediates bone marrow mesenchymal stem cells protection of radiation-induced lung injury during the acute phase by regulating polarization of alveolar macrophages. Translational Cancer Research, 9(1), 231–239. https://doi.org/10.21037/tcr.2019.12.77
Deng, C. L., Hu, C. B., Ling, S. T., Zhao, N., Bao, L. H., Zhou, F., Xiong, Y. C., Chen, T., Sui, B. D., Yu, X. R., et al. (2021). Photoreceptor protection by mesenchymal stem cell transplantation identifies exosomal MiR-21 as a therapeutic for retinal degeneration. Cell Death and Differentiation, 28(3), 1041–1061. https://doi.org/10.1038/s41418-020-00636-4
Su, W., Li, Z., Jia, Y., Zhu, Y., Cai, W., Wan, P., Zhang, Y., Zheng, S. G., & Zhuo, Y. (2017). MicroRNA-21a-5p/PDCD4 axis regulates mesenchymal stem cell-induced neuroprotection in acute glaucoma. Journal of Molecular Cell Biology, 9(4), 289–301. https://doi.org/10.1093/jmcb/mjx022
Hoppe, B., Pietsch, S., Franke, M., Engel, S., Groth, M., Platzer, M., & Englert, C. (2015). MiR-21 is required for efficient kidney regeneration in fish. BMC Developmental Biology, 15, 43. https://doi.org/10.1186/s12861-015-0089-2
Ansari, M. (2019). Bone tissue regeneration: Biology, strategies and interface studies. Progress in Biomaterials, 8(4), 223–237. https://doi.org/10.1007/s40204-019-00125-z
Iaquinta, M. R., Mazzoni, E., Bononi, I., Rotondo, J. C., Mazziotta, C., Montesi, M., Sprio, S., Tampieri, A., Tognon, M., & Martini, F. (2019). Adult stem cells for bone regeneration and repair. Frontiers in Cell and Development Biology, 7, 268. https://doi.org/10.3389/fcell.2019.00268
Schönitzer, V., Wirtz, R., Ulrich, V., Berger, T., Karl, A., Mutschler, W., Schieker, M., & Böcker, W. (2014). Sox2 is a potent inhibitor of osteogenic and adipogenic differentiation in human mesenchymal stem cells. Cellular Reprogramming, 16(5), 355–365. https://doi.org/10.1089/cell.2014.0006
Li, X., Guo, L., Liu, Y., Su, Y., Xie, Y., Du, J., Zhou, J., Ding, G., Wang, H., Bai, Y., et al. (2017). MicroRNA-21 promotes osteogenesis of bone marrow mesenchymal stem cells via the Smad7-Smad1/5/8-Runx2 pathway. Biochemical and Biophysical Research Communications, 493(2), 928–933. https://doi.org/10.1016/j.bbrc.2017.09.119
Bacevic, M., Brkovic, B., Albert, A., Rompen, E., Radermecker, R. P., & Lambert, F. (2017). Does oxidative stress play a role in altered characteristics of diabetic bone? A systematic review. Calcified Tissue International, 101(6), 553–563. https://doi.org/10.1007/s00223-017-0327-7
Baćević, M., Brković, B., Lambert, F., Djukić, L., Petrović, N., & Roganović, J. (2019). Leukocyte- and platelet-rich fibrin as graft material improves microRNA-21 expression and decreases oxidative stress in the calvarial defects of diabetic rabbits. Archives of Oral Biology, 102, 231–237. https://doi.org/10.1016/j.archoralbio.2019.05.005
Chen, D., & Wang, Z. (2017). Adrenaline inhibits osteogenesis via repressing miR-21 expression. Cell Biology International, 41(1), 8–15. https://doi.org/10.1002/cbin.10685
Yang, C., Liu, X., Zhao, K., Zhu, Y., Hu, B., Zhou, Y., Wang, M., Wu, Y., Zhang, C., Xu, J., et al. (2019). MiRNA-21 promotes osteogenesis via the PTEN/PI3K/Akt/HIF-1α pathway and enhances bone regeneration in critical size defects. Stem Cell Research & Therapy, 10(1), 65. https://doi.org/10.1186/s13287-019-1168-2
Wan, C., Shao, J., Gilbert, S. R., Riddle, R. C., Long, F., Johnson, R. S., Schipani, E., & Clemens, T. L. (2010). Role of HIF-1alpha in skeletal development. Annals of the New York Academy of Sciences, 1192, 322–326. https://doi.org/10.1111/j.1749-6632.2009.05238.x
Cheng, C. H., Chen, L. R., & Chen, K. H. (2022). Osteoporosis due to hormone imbalance: An overview of the effects of estrogen deficiency and glucocorticoid overuse on bone turnover. International Journal of Molecular Sciences, 23(3). https://doi.org/10.3390/ijms23031376
Zhao, Z., Li, X., Zou, D., Lian, Y., Tian, S., & Dou, Z. (2019). Expression of microRNA-21 in osteoporotic patients and its involvement in the regulation of osteogenic differentiation. Experimental and Therapeutic Medicine, 17(1), 709–714. https://doi.org/10.3892/etm.2018.6998
Thacker, G., Kumar, Y., Khan, M. P., Shukla, N., Kapoor, I., Kanaujiya, J. K., Lochab, S., Ahmed, S., Sanyal, S., Chattopadhyay, N., et al. (2016). Skp2 inhibits osteogenesis by promoting ubiquitin-proteasome degradation of Runx2. Biochimica et Biophysica Acta, 1863(4), 510–519. https://doi.org/10.1016/j.bbamcr.2016.01.010
Jiang, Y., J. Li, X. Xue, Z. Yin, K. Xu, & Su, J. (2022). Engineered extracellular vesicles for bone therapy. Nano Today, 44, 01487. https://doi.org/10.1016/j.nantod.2022.101487.
Oka, S., Li, X., Zhang, F., Tewari, N., Ma, R., Zhong, L., Makishima, M., Liu, Y., & Bhawal, U. K. (2021). MicroRNA-21 facilitates osteoblast activity. Biochem Biophys Rep, 25, 100894. https://doi.org/10.1016/j.bbrep.2020.100894
Hu, C. H., Sui, B. D., Du, F. Y., Shuai, Y., Zheng, C. X., Zhao, P., Yu, X. R., & Jin, Y. (2017). MiR-21 deficiency inhibits osteoclast function and prevents bone loss in mice. Scientific Reports, 7, 43191. https://doi.org/10.1038/srep43191
Jiang, L. B., Tian, L., & Zhang, C. G. (2018). Bone marrow stem cells-derived exosomes extracted from osteoporosis patients inhibit osteogenesis via microRNA-21/SMAD7. European Review for Medical and Pharmacological Sciences, 22(19), 6221–6229. https://doi.org/10.26355/eurrev_201810_16028
Sheng, J., Liang, W. D., Xun, C. H., Xu, T., Zhang, J., & Sheng, W. B. (2019). Downregulation of miR-21 promotes tibial fracture healing in rabbits through activating ERK pathway. European Review for Medical and Pharmacological Sciences, 23(23), 10204–10210. https://doi.org/10.26355/eurrev_201912_19655
Wang, S., Liu, Z., Wang, J., Ji, X., Yao, Z., & Wang, X. (2020). MiR-21 promotes osteoclastogenesis through activation of PI3K/Akt signaling by targeting Pten in RAW264.7 cells. Molecular Medicine Reports, 21(3), 1125–1132. https://doi.org/10.3892/mmr.2020.10938
Li, C., Li, C., Yue, J., Huang, X., Chen, M., Gao, J., & Wu, B. (2012). MiR-21 and miR-101 regulate PLAP-1 expression in periodontal ligament cells. Molecular Medicine Reports, 5(5), 1340–1346. https://doi.org/10.3892/mmr.2012.797
Wei, F., Liu, D., Feng, C., Zhang, F., Yang, S., Hu, Y., Ding, G., & Wang, S. (2015). MicroRNA-21 mediates stretch-induced osteogenic differentiation in human periodontal ligament stem cells. Stem Cells and Development, 24(3), 312–319. https://doi.org/10.1089/scd.2014.0191
Sakashita, H., Yamada, S., Kinoshita, M., Kajikawa, T., Iwayama, T., & Murakami, S. (2021). Mice lacking PLAP-1/aspirin counteracts high fat diet-induced metabolic disorder and alveolar bone loss by controlling adipose tissue expansion. Scientific Reports, 11(1), 4970. https://doi.org/10.1038/s41598-021-84512-2
Hong, H., Zheng, J., Liu, L., Mai, L., Wei, X., & Wu, L. (2016). MicroRNA 21 and PLAP-1 regulate periodontal ligament remodeling during tooth movement of rats. International Journal of Clinical and Experimental Pathology, 9(5), 4943–4952.
Chen, N., Sui, B. D., Hu, C. H., Cao, J., Zheng, C. X., Hou, R., Yang, Z. K., Zhao, P., Chen, Q., Yang, Q. J., et al. (2016). MicroRNA-21 contributes to orthodontic tooth movement. Journal of Dental Research, 95(12), 1425–1433. https://doi.org/10.1177/0022034516657043
Chen, D., Wu, L., Liu, L., Gong, Q., Zheng, J., Peng, C., & Deng, J. (2017). Comparison of HIF1A-AS1 and HIF1A-AS2 in regulating HIF-1α and the osteogenic differentiation of PDLCs under hypoxia. International Journal of Molecular Medicine, 40(5), 1529–1536. https://doi.org/10.3892/ijmm.2017.3138
Zhang, X., Chen, D., Zheng, J., Deng, L., Chen, Z., Ling, J., & Wu, L. (2019). Effect of microRNA-21 on hypoxia-inducible factor-1α in orthodontic tooth movement and human periodontal ligament cells under hypoxia. Experimental and Therapeutic Medicine, 17(4), 2830–2836. https://doi.org/10.3892/etm.2019.7248
Kowalski, J., Lapinska, B., Nissan, J., & Lukomska-Szymanska, M. (2021). Factors influencing marginal bone loss around dental implants: A narrative review. Coatings, 11(7), 865. https://doi.org/10.3390/coatings11070865
Wang, Z., Wu, G., Feng, Z., Bai, S., Dong, Y., Wu, G., & Zhao, Y. (2015). Microarc-oxidized titanium surfaces functionalized with microRNA-21-loaded chitosan/hyaluronic acid nanoparticles promote the osteogenic differentiation of human bone marrow mesenchymal stem cells. International Journal of Nanomedicine, 10, 6675–6687. https://doi.org/10.2147/ijn.s94689
Zhang, W., Jia, L., Zhao, B., Xiong, Y., Wang, Y. N., Liang, J., & Xu, X. (2021). Quercetin reverses TNF-α induced osteogenic damage to human periodontal ligament stem cells by suppressing the NF-κB/NLRP3 inflammasome pathway. International Journal of Molecular Medicine, 47(4). https://doi.org/10.3892/ijmm.2021.4872
Yang, N., Li, Y., Wang, G., Ding, Y., Jin, Y., & Xu, Y. (2017). Tumor necrosis factor-α suppresses adipogenic and osteogenic differentiation of human periodontal ligament stem cell by inhibiting miR-21/Spry1 functional axis. Differentiation, 97, 33–43. https://doi.org/10.1016/j.diff.2017.08.004
Xu, K., Xiao, J., Zheng, K., Feng, X., Zhang, J., Song, D., Wang, C., Shen, X., Zhao, X., Wei, C., et al. (2018). MiR-21/STAT3 signal is involved in odontoblast differentiation of human dental pulp stem cells mediated by TNF-α. Cellular Reprogramming, 20(2), 107–116. https://doi.org/10.1089/cell.2017.0042
Shuhaibar, N., Hand, A. R., & Terasaki, M. (2021). Odontoblast processes of the mouse incisor are plates oriented in the direction of growth. Anat Rec (Hoboken), 304(8), 1820–1827. https://doi.org/10.1002/ar.24570
Singh, S. K., Kagalwala, M. N., Parker-Thornburg, J., Adams, H., & Majumder, S. (2008). REST maintains self-renewal and pluripotency of embryonic stem cells. Nature, 453(7192), 223–227. https://doi.org/10.1038/nature06863
Jørgensen, H. F., Terry, A., Beretta, C., Pereira, C. F., Leleu, M., Chen, Z. F., Kelly, C., Merkenschlager, M., & Fisher, A. G. (2009). REST selectively represses a subset of RE1-containing neuronal genes in mouse embryonic stem cells. Development, 136(5), 715–721. https://doi.org/10.1242/dev.028548
He, Q., & Liu, Z. (2015). Dynamical behaviors of the transcriptional network including REST and miR-21 in embryonic stem cells. Current Bioinformatics, 10(1), 48–58. https://doi.org/10.2174/157489361001150309141100
Pan, G., & Thomson, J. A. (2007). Nanog and transcriptional networks in embryonic stem cell pluripotency. Cell Research, 17(1), 42–49. https://doi.org/10.1038/sj.cr.7310125
Singh, S. K., Marisetty, A., Sathyan, P., Kagalwala, M., Zhao, Z., & Majumder, S. (2015). REST-miR-21-SOX2 axis maintains pluripotency in E14Tg2a.4 embryonic stem cells. Stem Cell Research, 15(2), 305–311. https://doi.org/10.1016/j.scr.2015.05.003
Debnath, T., Deb Nath, N. C., Kim, E. K., & Lee, K. G. (2017). Role of phytochemicals in the modulation of miRNA expression in cancer. Food & Function, 8(10), 3432–3442. https://doi.org/10.1039/c7fo00739f
Kalhori, M.R.R., H. Khodayari, S. Khodayari, M. Vesovic, G. Jackson, M.H.H. Farzaei, & Bishayee, A. (2021). Regulation of long non-coding RNAs by plant secondary metabolites: A novel anticancer therapeutic approach. Cancers, 13(6), 1274. https://doi.org/10.3390/cancers13061274.
Parsamanesh, N., Asghari, A., Sardari, S., Tasbandi, A., Jamialahmadi, T., Xu, S., & Sahebkar, A. (2021). Resveratrol and endothelial function: A literature review. Pharmacological Research, 170, 105725. https://doi.org/10.1016/j.phrs.2021.105725
Campagnolo, P., Hong, X., di Bernardini, E., Smyrnias, I., Hu, Y., & Xu, Q. (2015). Resveratrol-induced vascular progenitor differentiation towards endothelial lineage via MiR-21/Akt/β-catenin is protective in vessel graft models. PLoS One, 10(5), e0125122. https://doi.org/10.1371/journal.pone.0125122
Wang, L., Cui, Y., Tang, M., Hu, X., Luo, H., Hescheler, J., & Xi, J. (2014). Puerarin facilitates T-tubule development of murine embryonic stem cell-derived cardiomyocytes. Cellular Physiology and Biochemistry, 34(2), 383–392. https://doi.org/10.1159/000363007
Yin, M., Yuan, Y., Cui, Y., Hong, X., Luo, H., Hu, X., Tang, M., Hescheler, J., & Xi, J. (2015). Puerarin suppresses the self-renewal of murine embryonic stem cells by inhibition of REST-MiR-21 regulatory pathway. Cellular Physiology and Biochemistry, 37(2), 527–536. https://doi.org/10.1159/000430374
Srinivasulu, C., Ramgopal, M., Ramanjaneyulu, G., Anuradha, C. M., & Suresh Kumar, C. (2018). Syringic acid (SA) – A review of its occurrence, biosynthesis, pharmacological and industrial importance. Biomedicine & Pharmacotherapy, 108, 547–557. https://doi.org/10.1016/j.biopha.2018.09.069
Arumugam, B., Balagangadharan, K., & Selvamurugan, N. (2018). Syringic acid, a phenolic acid, promotes osteoblast differentiation by stimulation of Runx2 expression and targeting of Smad7 by miR-21 in mouse mesenchymal stem cells. J Cell Commun Signal, 12(3), 561–573. https://doi.org/10.1007/s12079-018-0449-3
Yu, Y., S.Y. Oh, H.Y. Kim, J.Y. Choi, S.A. Jo, & Jo, I. (2022). Valproic acid-induced ccn1 promotes osteogenic differentiation by increasing CCN1 protein stability through HDAC1 inhibition in tonsil-derived mesenchymal stem cells. Cells, 11(3). https://doi.org/10.3390/cells11030534.
Akshaya, N., Prasith, P., Abinaya, B., Ashwin, B., Chandran, S. V., & Selvamurugan, N. (2021). Valproic acid, a potential inducer of osteogenesis in mouse mesenchymal stem cells. Current Molecular Pharmacology, 14(1), 27–35. https://doi.org/10.2174/1874467213666200713102410
Wu, X. H., Dou, B., Sun, N. Y., Gao, J., & Liu, X. L. (2020). Astragalus saponin IV promotes osteogenic differentiation of bone marrow mesenchymal stem cells via miR-21/NGF/BMP2/Runx2 pathway. Acta Histochemica, 122(4), 151549. https://doi.org/10.1016/j.acthis.2020.151549
Zhang, D., Zhang, S., Jiang, K., Li, T., & Yan, C. (2020). Bioassay-guided isolation and evaluation of anti-osteoporotic polysaccharides from Morinda officinalis. Journal of Ethnopharmacology, 261, 113113. https://doi.org/10.1016/j.jep.2020.113113
Zhang, D., Fong, C., Jia, Z., Cui, L., Yao, X., & Yang, M. (2016). Icariin stimulates differentiation and suppresses adipocytic transdifferentiation of primary osteoblasts through estrogen receptor-mediated pathway. Calcified Tissue International, 99(2), 187–198. https://doi.org/10.1007/s00223-016-0138-2
Yang, C., Liu, W., Shan, H., Yu, X., Zhang, X., Zeng, B., & Qian, Y. (2021). Naringin inhibits titanium particles-induced upregulation of TNF-α and IL-6 via the p38 MAPK pathway in fibroblasts from hip periprosthetic membrane. Connective Tissue Research, 62(5), 485–494. https://doi.org/10.1080/03008207.2020.1778680
Lian, F., Zhao, C., Qu, J., Lian, Y., Cui, Y., Shan, L., & Yan, J. (2018). Icariin attenuates titanium particle-induced inhibition of osteogenic differentiation and matrix mineralization via miR-21-5p. Cell Biology International, 42(8), 931–939. https://doi.org/10.1002/cbin.10957
Hao, B., Wang, X., Ma, X., Jin, Y., Fan, W., Laba, C., Wujin, C., Wang, Y., & Liang, J. (2020). Preparation of complex microcapsules of soluble polysaccharide from Glycyrrhiza uralensis and its application in wound repair and scar inhibition. International Journal of Biological Macromolecules, 156, 906–917. https://doi.org/10.1016/j.ijbiomac.2020.03.121
Wang, Y., Wang, C., Dang, J., Xue, H., Wang, X., Jin, Y., Yang, M., Leng, F., & Zhang, B. (2021). Structural characteristics of polysaccharide microcapsules from Nostoc commune, and their applications in skin wound healing and pathological repair. Biomedical Materials (Bristol), 16(4). https://doi.org/10.1088/1748-605X/abe978
Statello, L., Guo, C. J., Chen, L. L., & Huarte, M. (2021). Gene regulation by long non-coding RNAs and its biological functions. Nature Reviews Molecular Cell Biology, 22(2), 96–118. https://doi.org/10.1038/s41580-020-00315-9
Poliseno, L., Salmena, L., Zhang, J., Carver, B., Haveman, W. J., & Pandolfi, P. P. (2010). A coding-independent function of gene and pseudogene mRNAs regulates tumour biology. Nature, 465(7301), 1033–1038. https://doi.org/10.1038/nature09144
Wang, Z., Song, Y., Han, X., Qu, P., & Wang, W. (2020). Long noncoding RNA PTENP1 affects the recovery of spinal cord injury by regulating the expression of miR-19b and miR-21. Journal of Cellular Physiology, 235(4), 3634–3645. https://doi.org/10.1002/jcp.29253
Peterson, A., & Nair, L. S. (2022). Hair follicle stem cells for tissue regeneration. Tissue Engineering. Part B, Reviews, 28(4), 695–706. https://doi.org/10.1089/ten.TEB.2021.0098
Cai, B., Zheng, Y., Ma, S., Xing, Q., Wang, X., Yang, B., Yin, G., & Guan, F. (2018). Long non-coding RNA regulates hair follicle stem cell proliferation and differentiation through PI3K/AKT signal pathway. Molecular Medicine Reports, 17(4), 5477–5483. https://doi.org/10.3892/mmr.2018.8546
Fang, Y. L., Chen, X. G., & Godbey, W. T. (2015). Gene delivery in tissue engineering and regenerative medicine. Journal of Biomedical Materials Research. Part B, Applied Biomaterials, 103(8), 1679–1699. https://doi.org/10.1002/jbm.b.33354
Beavers, K. R., Nelson, C. E., & Duvall, C. L. (2015). MiRNA inhibition in tissue engineering and regenerative medicine. Advanced Drug Delivery Reviews, 88, 123–137. https://doi.org/10.1016/j.addr.2014.12.006
Zhang, X., Sun, Y., Liu, J., Yi, Z., Gao, F., Liu, Q., & Chen, Y. (2017). In situ forming hydrogels with long-lasting miR-21 enhances the therapeutic potential of MSC by sustaining stimulation of target gene. Journal of Biomaterials Science. Polymer Edition, 28(15), 1639–1650. https://doi.org/10.1080/09205063.2017.1341675
Feng, H., Li, Z., Xie, W., Wan, Q., Guo, Y., Chen, J., Wang, J., & Pei, X. (2022). Delivery of therapeutic miRNAs using nanoscale zeolitic imidazolate framework for accelerating vascularized bone regeneration. Chemical Engineering Journal, 430. https://doi.org/10.1016/j.cej.2021.132867
Wang, S. Y., Kim, H., Kwak, G., Jo, S. D., Cho, D., Yang, Y., Kwon, I. C., Jeong, J. H., & Kim, S. H. (2020). Development of microRNA-21 mimic nanocarriers for the treatment of cutaneous wounds. Theranostics, 10(7), 3240–3253. https://doi.org/10.7150/thno.39870
Sun, X., Li, X., Qi, H., Hou, X., Zhao, J., Yuan, X., & Ma, X. (2020). MiR-21 nanocapsules promote early bone repair of osteoporotic fractures by stimulating the osteogenic differentiation of bone marrow mesenchymal stem cells. Journal of Orthopaedic Translation, 24, 76–87. https://doi.org/10.1016/j.jot.2020.04.007
Acknowledgements
We would like to acknowledge BioRender software (Biorender.com) that was used to create a graphical abstract.
Funding
This work was supported by Kermanshah University of Medical Sciences (Grant numbers 50001884).
Author information
Authors and Affiliations
Contributions
Mohammad Reza Kalhori: Idea, Methodology, conceptualization, supervision, Funding acquisition, Original draft preparation, and literature search.; Masoud Soleimani: Project administration, Writing - review & editing.; Amir Ali Kalhori: literature search, Software, and original draft preparation, Software.; Parisa Mohamadi: literature search, original draft preparation, Software.; Rasoul Azreh: original draft preparation.; Reza Alibakhshi: Writing - review & editing.; Mohammad Hosien Farzaei: Writing - review & editing. All authors have read and agreed to the published the version of the manuscript to be submitted.
Corresponding author
Ethics declarations
Ethics Approval
Not applicable.
Consent to Participate
Not applicable.
Consent for Publication
All authors consent to the publication of this manuscript.
Conflict of Interest
All authors declare have no relevant financial or non-financial interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kalhori, M.R., Soleimani, M., Alibakhshi, R. et al. The Potential of miR-21 in Stem Cell Differentiation and its Application in Tissue Engineering and Regenerative Medicine. Stem Cell Rev and Rep 19, 1232–1251 (2023). https://doi.org/10.1007/s12015-023-10510-8
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12015-023-10510-8