Abstract
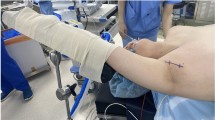
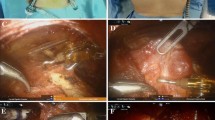
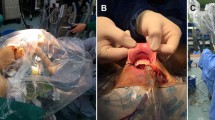
Since the introduction of the single-port (SP) robotic system, SP trans-axillary robot-assisted thyroidectomy (SP-TART) has been performed. We aimed to evaluate the safety and surgical outcomes of SP-TART in a consecutive series of 300 cases. We analyzed 300 patients with thyroid disease who underwent SP-TART from October 2021 to May 2023 in St. Mary’s Hospital in Seoul, Korea. We analyzed the patients’ clinicopathological characteristics and perioperative outcomes according to surgical extent. Of the 300 cases analyzed, 250 patients underwent less than total thyroidectomy (LTT), 31 patients underwent total thyroidectomy (TT), and 19 patients underwent TT with modified radical neck dissection (TT c mRND). The mean operative times for LTT, TT, and for TT c mRND were 69.8 ± 23.6, 104.2 ± 30.7, and 223.7 ± 72.4 min, respectively. Complications, including postoperative bleeding, transient hypoparathyroidism, and vocal cord palsy, were observed in nine, six, and six LTT, TT, and TT c mRND cases. The SP-TART method is a safe and feasible surgical option with a short operative time, good surgical outcome, and excellent cosmetic results.


Similar content being viewed by others
Data availability statement
The data that support the findings of this study are available on request from the corresponding author. The data are not publicly available due to privacy or ethical restrictions.
References
Haugen BR, Alexander EK, Bible KC, Doherty GM, Mandel SJ, Nikiforov YE, Pacini F, Randolph GW, Sawka AM, Schlumberger M, Schuff KG (2016) 2015 American thyroid association management guidelines for adult patients with thyroid nodules and differentiated thyroid cancer: the American thyroid association guidelines task force on thyroid nodules and differentiated thyroid cancer. Thyroid 26(1):1–133
LeClair K, Bell KJ, Furuya-Kanamori L, Doi SA, Francis DO, Davies L (2021) Evaluation of gender inequity in thyroid cancer diagnosis: differences by sex in US thyroid cancer incidence compared with a meta-analysis of subclinical thyroid cancer rates at autopsy. JAMA Int Med 181(10):1351–1358
Choi Y, Lee JH, Kim YH, Lee YS, Chang HS, Park CS, Roh MR (2014) Impact of postthyroidectomy scar on the quality of life of thyroid cancer patients. Ann Dermatol 26(6):693–699
Tae K, Ji YB, Song CM, Ryu J (2019) Robotic and endoscopic thyroid surgery: evolution and advances. Clin Exp Otorhinolaryngol 12(1):1
Chang EH, Kim HY, Koh YW, Chung WY (2017) Overview of robotic thyroidectomy. Gland Surg 6(3):218
de Vries LH, Aykan D, Lodewijk L, Damen JA, Borel Rinkes IH, Vriens MR (2021) Outcomes of minimally invasive thyroid surgery—a systematic review and meta-analysis. Front Endocrinol 12:719397
Pan JH, Zhou H, Zhao XX, Ding H, Wei L, Qin L, Pan YL (2017) Robotic thyroidectomy versus conventional open thyroidectomy for thyroid cancer: a systematic review and meta-analysis. Surg Endosc 31(10):3985–4001
Sun GH, Peress L, Pynnonen MA (2014) Systematic review and meta-analysis of robotic vs conventional thyroidectomy approaches for thyroid disease. Otolaryngol Head Neck Surg 150(4):520–32
Bhettani MK, Rehman M, Ahmed M, Altaf HN, Choudry UK, Khan KH (2019) Role of pre-operative vitamin D supplementation to reduce post-thyroidectomy hypocalcemia; Cohort study. Int J Surg (London, England) 71:85–90
Amin MB, Edge S, Greene F, Byrd DR, Brookland RK, Washington MK, Gershenwald JE, Compton CC, Hess KR, Sullivan DC, Jessup JM, Brierley JD, Gaspar LE, Schilsky RL, Balch CM, Winchester DP, Asare EA, Madera M, Gress DM, Meyer LR (2017) AJCC cancer staging manual, 8th edn. Springer, New York
Kang IK, Park J, Bae JS, Kim JS, Kim K (2022) Safety and feasibility of single-port trans-axillary robotic thyroidectomy: experience through consecutive 100 cases. Medicina (Kaunas, Lithuania) 58(10):1485
Park J, Kang LK, Kim K, Bae JS, Kim JS (2023) The learning curve for single-port transaxillary robotic thyroidectomy (SP-TART): experience through initial 50 cases of lobectomy. Updates Surg 75(3):691–700
Ikeda Y, Takami H, Sasaki Y, Kan S, Niimi M (2000) Endoscopic neck surgery by the axillary approach. J Am College Surg 191(3):336–340
Kang SW, Jeong JJ, Yun JS, Sung TY, Lee SC, Lee YS, Nam KH, Chang HS, Chung WY, Park CS (2009) Gasless endoscopic thyroidectomy using trans-axillary approach; surgical outcome of 581 patients. Endocr J 56(3):361–369
Lombardi CP, Raffaelli M, Princi P, De Crea C, Bellantone R (2006) Video-assisted thyroidectomy: report on the experience of a single center in more than four hundred cases. World J Surg 30(5):794–800
Li T, Zhang Z, Chen W, Yu S, Sun B, Deng X, Ge J, Wei Z, Lei S, Li G (2022) Comparison of quality of life and cosmetic result between open and transaxillary endoscopic thyroid lobectomy for papillary thyroid microcarcinoma survivors: a single-center prospective cohort study. Cancer Med 11(22):4146–4156
Lobe TE, Wright SK, Irish MS (2005) Novel uses of surgical robotics in head and neck surgery. J Laparoendosc Adv Surg Tech A 15(6):647–652
Kang SW, Jeong JJ, Yun JS, Sung TY, Lee SC, Lee YS, Nam KH, Chang HS, Chung WY, Park CS (2009) Robot-assisted endoscopic surgery for thyroid cancer: experience with the first 100 patients. Surg Endosc 23(11):2399–2406
Lee J, Nah KY, Kim RM, Ahn YH, Soh EY, Chung WY (2010) Differences in postoperative outcomes, function, and cosmesis: open versus robotic thyroidectomy. Surg Endosc 24(12):3186–3194
Kim JK, Choi SH, Choi SM, Choi HR, Lee CR, Kang SW, Jeong JJ, Nam KH, Chung WY (2022) Single-port transaxillary robotic thyroidectomy (START): 200-cases with two-step retraction method. Surg Endosc 36(4):2688–2696
Chang YW, Lee HY, Kim WY, Kim HY, Lee JB, Son GS (2021) Detailed comparison of the da Vinci Xi and S surgical systems for transaxillary thyroidectomy. Medicine 100(3)
Piccoli M, Mullineris B, Gozzo D, Colli G, Pecchini F, Nigro C, Rochira V (2019) Evolution strategies in transaxillary robotic thyroidectomy: considerations on the first 449 cases performed. J Laparoendosc Adv Surg Tech A 29(4):433–440
Ban EJ, Yoo JY, Kim WW, Son HY, Park S, Lee SH, Lee CR, Kang SW, Jeong JJ, Nam KH, Chung WY (2014) Surgical complications after robotic thyroidectomy for thyroid carcinoma: a single center experience with 3,000 patients. Surg Endosc 28(9):2555–2563
Lee J, Kwon IS, Bae EH, Chung WY (2013) Comparative analysis of oncological outcomes and quality of life after robotic versus conventional open thyroidectomy with modified radical neck dissection in patients with papillary thyroid carcinoma and lateral neck node metastases. J Clin Endocrinol Metab 98(7):2701–2708
Noureldine SI, Jackson NR, Tufano RP, Kandil E (2013) A comparative North American experience of robotic thyroidectomy in a thyroid cancer population. Langenbeck’s Arch Surg 398(8):1069–1074
Ji KS, Oyekunle TO, Thomas SM, Scheri R, Stang M, Roman SA, Sosa JA (2019) Adequacy of lymph node yield for papillary thyroid cancer: an analysis of 23,131 patients. J Surg Res 244:566–573
Beal SH, Chen SL, Schneider PD, Martinez SR (2010) An evaluation of lymph node yield and lymph node ratio in well-differentiated thyroid carcinoma. Am Surg 76(1):28–32
Yu ST, Ge JN, Sun BH, Wei ZG, Xiao ZZ, Zhang ZC, Chen WS, Li TT, Lei ST (2021) Lymph node yield in the initial central neck dissection (CND) associated with the risk of recurrence in papillary thyroid cancer: a reoperative CND cohort study. Oral Oncol 123:105567
Issa K, Stevens MN, Sun Y, Thomas S, Collins A, Cohen J, Esclamado RM, Rocke DJ (2022) A retrospective study of lymph node yield in lateral neck dissection for papillary thyroid carcinoma. Ear Nose Throat J 101(7):456–462
Chung EJ, Cho SJ, Park MW, Rho YS (2019) The impact of the number of harvested central lymph nodes on the lymph node ratio. Auris Nasus Larynx 46(2):267–271
Feng JW, Yang XH, Wu BQ, Sun DL, Jiang Y, Qu Z (2019) Predictive factors for central lymph node and lateral cervical lymph node metastases in papillary thyroid carcinoma. Clin Transl Oncol 21(11):1483–1491
Kang SW, Kim MJ, Chung WY (2018) Gasless, transaxillary robotic neck dissection: the technique and evidence. Gland Surg 7(5):466
Ho J, Kim D, Lee JE, Kim JK, Lee CR, Kang SW, Jeong JJ, Nam KH, Chung WY (2023) Single-port transaxillary robotic modified radical neck dissection (STAR-RND): initial experiences. Laryngosc 133(3):709–7014
Holsinger FC, Chung WY (2014) Robotic thyroidectomy. Otolaryngol Clin N Am 47(3):373–378
Yap Z, Kim WW, Kang SW, Lee CR, Lee J, Jeong JJ, Nam KH, Chung WY (2019) Impact of body mass index on robotic transaxillary thyroidectomy. Sci Rep 9(1):8955
Stevenson CE, Gardner DF, Grover AC (2012) Patient factors affecting operative times for single-incision trans-axillary robotic-assisted (STAR) thyroid lobectomy: does size matter? Ann Surg Oncol 19(5):1460–1465
Steurer M, Passler C, Denk DM, Schneider B, Niederle B, Bigenzahn W (2002) Advantages of recurrent laryngeal nerve identification in thyroidectomy and parathyroidectomy and the importance of preoperative and postoperative laryngoscopic examination in more than 1000 nerves at risk. Laryngosc 112(1):124–133
Jeannon JP, Orabi AA, Bruch GA, Abdalsalam HA, Simo R (2009) Diagnosis of recurrent laryngeal nerve palsy after thyroidectomy: a systematic review. Int J Clin Practic 63(4):624–629
Lo CY, Kwok KF, Yuen PW (2000) A prospective evaluation of recurrent laryngeal nerve paralysis during thyroidectomy. Arch Surg (Chicago, IL: 1960) 135(2):204–207
Hayward NJ, Grodski S, Yeung M, Johnson WR, Serpell J (2013) Recurrent laryngeal nerve injury in thyroid surgery: a review. ANZ J Surg 83(1–2):15–21
Merchavy S, Marom T, Forest VI, Hier M, Mlynarek A, McHugh T, Payne R (2015) Comparison of the incidence of postoperative hypocalcemia following total thyroidectomy vs completion thyroidectomy. Otolaryngol Head Neck Surg 152(1):53–56
Bergenfelz A, Jansson S, Kristoffersson A, Mårtensson H, Reihnér E, Wallin G, Lausen I (2008) Complications to thyroid surgery: results as reported in a database from a multicenter audit comprising 3,660 patients. Langenbeck’s Arch Surg 393(5):667–673
Hundahl SA, Cady B, Cunningham MP, Mazzaferri E, McKee RF, Rosai J, Shah JP, Fremgen AM, Stewart AK, Hölzer S, US and German Thyroid Cancer Study Group (2000) Initial results from a prospective cohort study of 5583 cases of thyroid carcinoma treated in the united states during 1996. U.S. and German Thyroid Cancer Study Group. An American College of Surgeons Commission on Cancer Patient Care Evaluation study. Cancer 89(1):202–217
Jensen PV, Jelstrup SM, Homøe P (2015) Long-term outcomes after total thyroidectomy. Dan Med J 62(11):A5156
Rocke DJ, Mulder H, Cyr D, Kahmke R, Lee WT, Puscas L, Schulz K, Witsell DL (2020) The effect of lateral neck dissection on complication rate for total thyroidectomy. Am J Otolaryngol 41(3):102421
Acknowledgements
The authors wish to acknowledge the financial support of the Catholic Medical Center Research Foundation made in the program year of 2022.
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by SA and KSK The first draft of the manuscript was written by SA and all authors commented on previous versions of the manuscript and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interests
The authors have no relevant financial or non-financial interests to disclose.
Ethics approval
This study was conducted in accordance with the Declaration of Helsinki and approved by the Institutional Review Board of Seoul St. Mary’s Hospital, the Catholic University of Korea (approval No.: KC23RASI0236, Date: April 21, 2023).
Consent to participate & consent to publish
This study waived the requirement for informed consent due to the retrospective nature of the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
An, S., Park, J., Kim, K. et al. Safety and surgical outcomes of single-port trans-axillary robot-assisted thyroidectomy: Experience from a consecutive series of 300 patients. J Robotic Surg 18, 13 (2024). https://doi.org/10.1007/s11701-023-01810-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11701-023-01810-9