Abstract
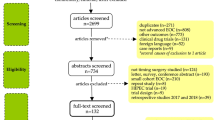
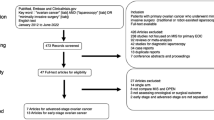
We evaluated the effectiveness, safety and efficacy of robotic interval debulking surgery (IDS) in advanced epithelial ovarian cancer (EOC) treated with neoadjuvant chemotherapy (NACT). We conducted a systematic review of the published relevant studies. Α total of 102 patients were evaluated. Mean operative time ranged from 164 to 312 min (mean ± SD: 246 ± 61 min) while mean estimated blood loss ranged from 106.9 to 262.5 ml (mean ± SD: 168 ± 68 ml) and postoperative blood transfusion rate was 19% (n = 19/98). Complete cytoreduction rate (R0 resection) was achieved in 75 patients (76.5%), whereas residual disease ≤ 1 cm in 21 women (21.5%). Mean hospital stay was 2.4 days. No intraoperative and six postoperative (14.6%) complications were reported. Laparotomy conversion rate was 9.2% (9/98) mostly in the terms of achieving complete cytoreduction and 30-day mortality rate was 9.2% (n = 9/98). The median overall survival varied from 39.7 to 47.2 months, while the progression-free survival ranged from 20.6 to 21.2 months during a median follow-up period from 2 to 86 months (median 25.3 months). A total of 60 women (61%) developed disease recurrence. One of the studies reported significantly improved OS and PFS in patients who underwent robotic IDS when compared to those who had laparotomy either during or before the addition of robotic surgery in the management of advanced ovarian cancer disease (47.2 vs 37.8 vs 37.9, p = 0.004 for OS and 20.6 vs 13.9 vs 11.9, p = 0.005 for PFS, respectively). The same was also observed when controlling the parameters of age and stage for patients in the robotic arm (p = 0.02). Robotic interval debulking surgery can be considered in the management of advanced ovarian cancer patients after receiving neoadjuvant chemotherapy. Larger meta-analyses including multicenter randomized control trials are necessary to specify the exact profile of the patients that could benefit from this treatment strategy.

Similar content being viewed by others
References
Shi C, Gao Y, Yang Y, Zhang L, Yu J, Zhang T (2019) Comparison of efficacy of robotic surgery, laparoscopy, and laparotomy in the treatment of ovarian cancer: a meta-analysis. World J Surg Oncol 17(1):162
Davidson BA, Broadwater G, Crim A, Boccacio R, Bixel K, Backes F et al (2019) Surgical complexity score and role of laparoscopy in women with advanced ovarian cancer treated with neoadjuvant chemotherapy. Gynecol Oncol 152(3):554–559
Chang SJ, Hodeib M, Chang J, Bristow RE (2013) Survival impact of complete cytoreduction to no gross residual disease for advanced-stage ovarian cancer: a meta-analysis. Gynecol Oncol 130(3):493–498
Martinez A, Ngo C, Leblanc E, Gouy S, Luyckx M, Darai E et al (2016) Surgical complexity impact on survival after complete cytoreductive surgery for advanced ovarian cancer. Ann Surg Oncol 23(8):2515–2521
Gueli Alletti S, Bottoni C, Fanfani F, Gallotta V, Chiantera V, Costantini B et al (2016) Minimally invasive interval debulking surgery in ovarian neoplasm (MISSION trial-NCT02324595): a feasibility study. Am J Obstet Gynecol 214(4):503.e1–e6
Menderes G, Black JD, Azodi M (2016) The role of minimally invasive interval debulking surgery in advanced epithelial ovarian cancer. Expert Rev Anticancer Ther 16(9):899–901
Ramirez PT, Frumovitz M, Pareja R, Lopez A, Vieira M, Ribeiro R et al (2018) Minimally invasive versus abdominal radical hysterectomy for cervical cancer. N Engl J Med 379(20):1895–1904
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gotzsche PC, Ioannidis JP et al (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ (Clinical research ed) 339:b2700
Carbajal-Mamani SL, Schweer D, Markham MJ, Esnakula AK, Grajo JR, Castagno JC et al (2020) Robotic-assisted interval cytoreductive surgery in ovarian cancer: a feasibility study. Obstet Gynecol Sci 63(2):150–157
Ackroyd SA, Thomas S, Angel C, Moore R, Meacham PJ, DuBeshter B (2018) Interval robotic cytoreduction following neoadjuvant chemotherapy in advanced ovarian cancer. J Robot Surg 12(2):245–250
Abitbol J, Gotlieb W, Zeng Z, Ramanakumar A, Kessous R, Kogan L et al (2019) Incorporating robotic surgery into the management of ovarian cancer after neoadjuvant chemotherapy. Int J Gynecol Cancer 29(9):1341–1347
Chen CH, Chiu LH, Chen HH, Chan C, Liu WM (2016) Comparison of robotic approach, laparoscopic approach and laparotomy in treating epithelial ovarian cancer. Int J Med Robot Comput Assist Surg MRCAS 12(2):268–275
Magrina JF, Zanagnolo V, Noble BN, Kho RM, Magtibay P (2011) Robotic approach for ovarian cancer: perioperative and survival results and comparison with laparoscopy and laparotomy. Gynecol Oncol 121(1):100–105
Feuer GA, Lakhi N, Barker J, Salmieri S, Burrell M (2013) Perioperative and clinical outcomes in the management of epithelial ovarian cancer using a robotic or abdominal approach. Gynecol Oncol 131(3):520–524
Fagotti A, Gueli Alletti S, Corrado G, Cola E, Vizza E, Vieira M et al (2019) The INTERNATIONAL MISSION study: minimally invasive surgery in ovarian neoplasms after neoadjuvant chemotherapy. Int J Gynecol Cancer 29(1):5–9
Nezhat FR, Finger TN, Vetere P, Radjabi AR, Vega M, Averbuch L et al (2014) Comparison of perioperative outcomes and complication rates between conventional versus robotic-assisted laparoscopy in the evaluation and management of early, advanced, and recurrent stage ovarian, fallopian tube, and primary peritoneal cancer. Int J Gynecol Cancer 24(3):600–607
Cardenas-Goicoechea J, Wang Y, McGorray S, Saleem MD, Carbajal Mamani SL, Pomputius AF et al (2019) Minimally invasive interval cytoreductive surgery in ovarian cancer: systematic review and meta-analysis. J Robot Surg 13(1):23–33
Chang SJ, Bristow RE, Chi DS, Cliby WA (2015) Role of aggressive surgical cytoreduction in advanced ovarian cancer. J Gynecol Oncol 26(4):336–342
Wallace S, Kumar A, Mc Gree M, Weaver A, Mariani A, Langstraat C et al (2017) Efforts at maximal cytoreduction improve survival in ovarian cancer patients, even when complete gross resection is not feasible. Gynecol Oncol 145(1):21–26
Nezhat FR, Khalil SS, Finger TN, Vetere PF (2014) A hybrid technique of combined conventional and robotic-assisted laparoscopy for staging and debulking of early, advanced, and recurrent ovarian, fallopian tube, and primary peritoneal cancer. Gynecol Surg 11(1):27–36
Jeon C, Seo HS, Jung YJ, Park CH, Song KY (2018) The Vinci Xi system in robotic gastric cancer surgery: a comparison with the S system. J Minimally Invasive Surg 21(3):112–117
Ngu JC, Tsang CB, Koh DC (2017) The da Vinci Xi: a review of its capabilities, versatility, and potential role in robotic colorectal surgery. Robot Surg 4:77–85
Ndofor BT, Soliman PT, Schmeler KM, Nick AM, Frumovitz M, Ramirez PT (2011) Rate of port-site metastasis is uncommon in patients undergoing robotic surgery for gynecological malignancies. Int J Gynecol Cancer 21(5):936–940
Rauff S, Ng JS (2012) Port-site recurrence in a patient undergoing robot-assisted gynecologic cancer surgery for endometrial cancer—a case report. Gynecol Oncol Case Rep 2(4):127–129
Fagotti A, Petrillo M, Costantini B, Fanfani F, Gallotta V, Chiantera V et al (2014) Minimally invasive secondary cytoreduction plus HIPEC for recurrent ovarian cancer: a case series. Gynecol Oncol 132(2):303–306
van Driel WJ, Koole SN, Sikorska K, Schagen van Leeuwen JH, Schreuder HWR, Hermans RHM et al (2018) Hyperthermic intraperitoneal chemotherapy in ovarian cancer. N Engl J Med 378(3):230–240
Esquivel J, Averbach A (2012) Laparoscopic cytoreductive surgery and HIPEC in patients with limited pseudomyxoma peritonei of appendiceal origin. Gastroenterol Res Pract 2012:981245
Badgwell B, Blum M, Das P, Estrella J, Wang X, Ho L et al (2017) Phase II trial of laparoscopic hyperthermic intraperitoneal chemoperfusion for peritoneal carcinomatosis or positive peritoneal cytology in patients with gastric adenocarcinoma. Ann Surg Oncol 24(11):3338–3344
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Victoria Psomiadou, Anastasia Prodromidou, Alexandros Fotiou, Sofia Lekka and Christos Iavazzo declare that they have no relevant financial or non-financial interests. The authors did not receive support from any organization for the submitted work.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Psomiadou, V., Prodromidou, A., Fotiou, A. et al. Robotic interval debulking surgery for advanced epithelial ovarian cancer: current challenge or future direction? A systematic review. J Robotic Surg 15, 155–163 (2021). https://doi.org/10.1007/s11701-020-01155-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11701-020-01155-7