Abstract
Background and Aims
The incidence of intrahepatic cholangiocarcinoma (ICC) in non-alcoholic fatty liver disease (NAFLD) is increasing gradually. The prognosis of NAFLD-ICC has not been well studied. We aim to investigate the prognosis of patients with NAFLD-ICC after curative-intent partial hepatectomy (PH).
Methods
Multi-center data from January 2003 to January 2014 were retrospectively analyzed. The prognosis of ICC was analyzed using PSM and compared with hepatitis B virus (HBV)–related ICC.
Results
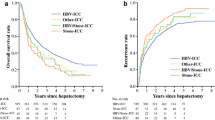
A total of 898 patients with ICC were included in this study. Of them, 199 (22.2%) were NAFLD-ICC, and 699 (77.8%) were HBV-ICC. Multivariate analysis showed that CA19-9 ≥ 37 U/mL, microvascular invasion, tumor size > 5 cm, multiple tumors, and lymph node (LN) metastasis were independent risk factors for early recurrence (ER) in ICC patients. After a 1:1 PSM, NAFLD-ICC has worse 5-year overall survival (OS) (24.0% vs. 48.9%), 5-year recurrence (80.9% vs. 55.0%), and ER (58.5% vs. 30.0%) than that of HBV-ICC (all P < 0.01). Multivariable analysis showed NAFLD was an independent risk factor for OS (hazard ratio [HR] 2.26, 95% CI 1.63–3.13, P < 0.001), tumor recurrence (HR 2.24, 95%CI 1.61–3.10, P < 0.001) and ER (HR 2.23, 95%CI 1.60–3.09, P < 0.001) in patients with ICC after PH. The sensitivity analysis indicated that NAFLD-ICC patients were more likely to experience ER.
Conclusion
Compared with HBV-ICC, NAFLD-ICC has a worse prognosis and was more likely to relapse early. More frequent surveillance should be considered.



Similar content being viewed by others
Data Availability
All data relevant to the study are included in the article or uploaded as online supplemental information.
Abbreviations
- ICC:
-
Intrahepatic cholangiocarcinoma
- HBV:
-
Hepatitis B virus
- NAFLD:
-
Non-alcoholic fatty liver disease
- HCV:
-
Hepatitis C virus
- PH:
-
Partial hepatectomy
- PSM:
-
Propensity score matching
- ER:
-
Early recurrence
- OS:
-
Overall survival
- TTR:
-
Time to recurrence
- HR:
-
Hazard ratio
- CI:
-
Confidence interval
- CA19-9:
-
Carbohydrate antigen 19–9
- AFP:
-
Alpha fetoprotein
- CEA:
-
Carcinoembryonic antigen
- TBIL:
-
Total bilirubin
- ALB:
-
Albumin
- ALT:
-
Alanine aminotransferase
- PLT:
-
Platelet
- PT:
-
Prothrombin time
- LN:
-
Lymph node
References
Massarweh, N. N.; El-Serag, H. B., Epidemiology of hepatocellular carcinoma and intrahepatic cholangiocarcinoma. Cancer Control 2017, 24 (3), 1073274817729245.
Mavros, M. N.; Economopoulos, K. P.; Alexiou, V. G.; Pawlik, T. M., Treatment and prognosis for patients with intrahepatic cholangiocarcinoma: systematic review and meta-analysis. JAMA Surg 2014, 149 (6), 565-74.
Sirica, A. E.; Gores, G. J.; Groopman, J. D.; Selaru, F. M.; Strazzabosco, M.; Wei Wang, X.; Zhu, A. X., Intrahepatic cholangiocarcinoma: continuing challenges and translational advances. Hepatology 2019, 69 (4), 1803-1815.
Wirth, T. C.; Vogel, A., Surveillance in cholangiocellular carcinoma. Best Pract Res Clin Gastroenterol 2016, 30 (6), 987-999.
Khan, S. A.; Thomas, H. C.; Davidson, B. R.; Taylor-Robinson, S. D., Cholangiocarcinoma. Lancet 2005, 366 (9493), 1303-14.
Corrao, S.; Natoli, G.; Argano, C., Nonalcoholic fatty liver disease is associated with intrahepatic cholangiocarcinoma and not with extrahepatic form: definitive evidence from meta-analysis and trial sequential analysis. Eur J Gastroenterol Hepatol 2021, 33 (1), 62-68.
Petrick, J. L.; Yang, B.; Altekruse, S. F.; Van Dyke, A. L.; Koshiol, J.; Graubard, B. I.; McGlynn, K. A., Risk factors for intrahepatic and extrahepatic cholangiocarcinoma in the United States: a population-based study in SEER-Medicare. PLoS One 2017, 12 (10), e0186643.
Shin, H. R.; Oh, J. K.; Masuyer, E.; Curado, M. P.; Bouvard, V.; Fang, Y. Y.; Wiangnon, S.; Sripa, B.; Hong, S. T., Epidemiology of cholangiocarcinoma: an update focusing on risk factors. Cancer Sci 2010, 101 (3), 579-85.
Zhang, H.; Yang, T.; Wu, M.; Shen, F., Intrahepatic cholangiocarcinoma: Epidemiology, risk factors, diagnosis and surgical management. Cancer Lett 2016, 379 (2), 198-205.
Rizvi, S.; Gores, G. J., Pathogenesis, diagnosis, and management of cholangiocarcinoma. Gastroenterology 2013, 145 (6), 1215-29.
Iida, H.; Kaibori, M.; Tanaka, S.; Takemura, S.; Wada, H.; Hirokawa, F.; Nakai, T.; Hayashi, M.; Eguchi, H.; Kubo, S., Low incidence of lymph node metastasis after resection of hepatitis virus-related intrahepatic cholangiocarcinoma. World J Surg 2017, 41 (4), 1082-1088.
Wang, Q.; Li, J.; Lei, Z.; Wu, D.; Si, A.; Wang, K.; Wang, Y.; Wan, X.; Lau, W. Y.; Shen, F., Prognosis of intrahepatic cholangiocarcinomas with HBV infection is better than those with hepatolithiasis after R0 liver resection: a propensity score matching analysis. Ann Surg Oncol 2017, 24 (6), 1579-1587.
Diehl, A. M.; Day, C., Cause, pathogenesis, and treatment of nonalcoholic steatohepatitis. N Engl J Med 2017, 377 (21), 2063-2072.
Alexander, M.; Loomis, A. K.; Fairburn-Beech, J.; van der Lei, J.; Duarte-Salles, T.; Prieto-Alhambra, D.; Ansell, D.; Pasqua, A.; Lapi, F.; Rijnbeek, P.; Mosseveld, M.; Avillach, P.; Egger, P.; Kendrick, S.; Waterworth, D. M.; Sattar, N.; Alazawi, W., Real-world data reveal a diagnostic gap in non-alcoholic fatty liver disease. BMC Med 2018, 16 (1), 130.
De Lorenzo, S.; Tovoli, F.; Mazzotta, A.; Vasuri, F.; Edeline, J.; Malvi, D.; Boudjema, K.; Renzulli, M.; Jeddou, H.; D'Errico, A.; Turlin, B.; Cescon, M.; Uguen, T.; Granito, A.; Lièvre, A.; Brandi, G., Non-Alcoholic Steatohepatitis as a Risk Factor for Intrahepatic Cholangiocarcinoma and Its Prognostic Role. Cancers (Basel). 2020, 12 (11), 3182. https://doi.org/10.3390/cancers12113182
Reddy, S. K.; Hyder, O.; Marsh, J. W.; Sotiropoulos, G. C.; Paul, A.; Alexandrescu, S.; Marques, H.; Pulitano, C.; Barroso, E.; Aldrighetti, L.; Geller, D. A.; Sempoux, C.; Herlea, V.; Popescu, I.; Anders, R.; Rubbia-Brandt, L.; Gigot, J. F.; Mentha, G.; Pawlik, T. M., Prevalence of nonalcoholic steatohepatitis among patients with resectable intrahepatic cholangiocarcinoma. J Gastrointest Surg 2013, 17 (4), 748-55.
Chalasani, N.; Younossi, Z.; Lavine, J. E.; Charlton, M.; Cusi, K.; Rinella, M.; Harrison, S. A.; Brunt, E. M.; Sanyal, A. J., The diagnosis and management of nonalcoholic fatty liver disease: practice guidance from the American Association for the Study of Liver Diseases. Hepatology 2018, 67 (1), 328-357.
Amin, M. B.; Greene, F. L.; Edge, S. B.; Compton, C. C.; Gershenwald, J. E.; Brookland, R. K.; Meyer, L.; Gress, D. M.; Byrd, D. R.; Winchester, D. P., The eighth edition AJCC cancer staging manual: continuing to build a bridge from a population-based to a more “personalized” approach to cancer staging. CA Cancer J Clin 2017, 67 (2), 93-99.
Ohira, M.; Kobayashi, T.; Hashimoto, M.; Tazawa, H.; Abe, T.; Oshita, A.; Kohashi, T.; Irei, T.; Oishi, K.; Ohdan, H.; Hiroshima Surgical study group of Clinical, O., Prognostic factors in patients with recurrent intrahepatic cholangiocarcinoma after curative resection: a retrospective cohort study. Int J Surg 2018, 54 (Pt A), 156-162.
Zhao, L.; Ma, X.; Liang, M.; Li, D.; Ma, P.; Wang, S.; Wu, Z.; Zhao, X., Prediction for early recurrence of intrahepatic mass-forming cholangiocarcinoma: quantitative magnetic resonance imaging combined with prognostic immunohistochemical markers. Cancer Imaging 2019, 19 (1), 49.
Zhu, Y.; Mao, Y.; Chen, J.; Qiu, Y.; Guan, Y.; Wang, Z.; He, J., Radiomics-based model for predicting early recurrence of intrahepatic mass-forming cholangiocarcinoma after curative tumor resection. Sci Rep 2021, 11 (1), 18347.
Cotter, T. G.; Rinella, M., Nonalcoholic fatty liver disease 2020: the state of the disease. Gastroenterology 2020, 158 (7), 1851-1864.
Brown, J. C.; Harhay, M. O.; Harhay, M. N., Nonalcoholic fatty liver disease and mortality among cancer survivors. Cancer Epidemiol 2017, 48, 104-109.
Cariou, B., The metabolic triad of non-alcoholic fatty liver disease, visceral adiposity and type 2 diabetes: implications for treatment. Diabetes Obes Metab 2022, 24 Suppl 2, 15-27.
Michelotti, G. A.; Machado, M. V.; Diehl, A. M., NAFLD, NASH and liver cancer. Nat Rev Gastroenterol Hepatol 2013, 10 (11), 656-65.
Zhou, H. B.; Hu, J. Y.; Hu, H. P., Hepatitis B virus infection and intrahepatic cholangiocarcinoma. World J Gastroenterol 2014, 20 (19), 5721-9.
Nguyen, M.H.; Wong, G.; Gane, E.; Kao, J.H.; Dusheiko, G., Hepatitis B Virus: Advances in Prevention, Diagnosis, and Therapy. Clin Microbiol Rev. 2020, 33 (2), e00046-19. https://doi.org/10.1128/CMR.00046-1
Ding, F. X.; Wang, F.; Lu, Y. M.; Li, K.; Wang, K. H.; He, X. W.; Sun, S. H., Multiepitope peptide-loaded virus-like particles as a vaccine against hepatitis B virus-related hepatocellular carcinoma. Hepatology 2009, 49 (5), 1492-502.
Kim, K. M.; Na, J. E.; Shim, S. G.; Sinn, D. H., Comparison of ICC patients with hepatitis B infection to those with no major risk factors for HCC. HPB (Oxford) 2021, 23 (6), 945-953.
Yu, T. H.; Chen, X.; Zhang, X. H.; Zhang, E. C.; Sun, C. X., Clinicopathological characteristics and prognostic factors for intrahepatic cholangiocarcinoma: a population-based study. Sci Rep 2021, 11 (1), 3990.
Yasui, K.; Hashimoto, E.; Tokushige, K.; Koike, K.; Shima, T.; Kanbara, Y.; Saibara, T.; Uto, H.; Takami, S.; Kawanaka, M.; Komorizono, Y.; Okanoue, T.; Japan, N. S. G., Clinical and pathological progression of non-alcoholic steatohepatitis to hepatocellular carcinoma. Hepatol Res 2012, 42 (8), 767-73.
Choi, W. J.; Williams, P. J.; Claasen, M.; Ivanics, T.; Englesakis, M.; Gallinger, S.; Hansen, B.; Sapisochin, G., Systematic Review and Meta-Analysis of Prognostic Factors for Early Recurrence in Intrahepatic Cholangiocarcinoma After Curative-Intent Resection. Ann Surg Oncol 2022. https://doi.org/10.1245/s10434-022-11463-x
Tsilimigras, D. I.; Sahara, K.; Moris, D.; Hyer, J. M.; Paredes, A. Z.; Bagante, F.; Merath, K.; Farooq, A. S.; Ratti, F.; Marques, H. P.; Soubrane, O.; Azoulay, D.; Lam, V.; Poultsides, G. A.; Popescu, I.; Alexandrescu, S.; Martel, G.; Guglielmi, A.; Hugh, T.; Aldrighetti, L.; Endo, I.; Pawlik, T. M., Effect of surgical margin width on patterns of recurrence among patients undergoing R0 hepatectomy for T1 hepatocellular carcinoma: an international multi-institutional analysis. J Gastrointest Surg 2020, 24 (7), 1552-1560.
Xu, X. F.; Xing, H.; Han, J.; Li, Z. L.; Lau, W. Y.; Zhou, Y. H.; Gu, W. M.; Wang, H.; Chen, T. H.; Zeng, Y. Y.; Li, C.; Wu, M. C.; Shen, F.; Yang, T., Risk factors, patterns, and outcomes of late recurrence after liver resection for hepatocellular carcinoma: a multicenter study from China. JAMA Surg 2019, 154 (3), 209-217.
Funding
This study was supported by the National Natural Science Foundation of China [81871988 to C.Z.J. and 82002584 to L.Z.Q], and the Jiangsu Province Key Research and Development Program [BE2019747 to C.Z.J.].
Author information
Authors and Affiliations
Contributions
ZQL, ZJC: study design, financial support, critical revision of the manuscript for important intellectual content, and study supervision; QSY, WHM: study design, patient screening, data collection, data analysis and interpretation, and manuscript writing; FCY, HLT, QRX, XWT, AFS, PHY: patient screening, data collection; All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics Approval
This study was approved by the Ethics Committee of each hospital, and all patients signed an informed consent form before surgery.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Lay Summary
• The prevalence of NAFLD-related ICC is gradually increasing.
• Compared to HBV-ICC, NAFLD-ICC has a worse prognosis and is more likely to relapse early.
• For NAFLD-ICC patients, more frequent surveillance should be considered.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yu, Q., Lei, Z., Ma, W. et al. Postoperative Prognosis of Non-alcoholic Fatty Liver Disease-Associated Intrahepatic Cholangiocarcinoma: a Multi-center Propensity Score Matching Analysis. J Gastrointest Surg 27, 2403–2413 (2023). https://doi.org/10.1007/s11605-023-05794-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-023-05794-7