Abstract
Background
Hepatic hemangiomas (HHs) are benign liver lesions often discovered incidentally on imaging for various unrelated pathologies. We herein review the etiology, classification, diagnostic imaging, and management of HHs.
Methods
A comprehensive systematic review was performed utilizing MEDLINE/PubMed and Web of Science databases, with the end of search date being March 1, 2022, regarding HH diagnosis, imaging, and management.
Results
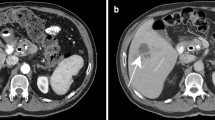
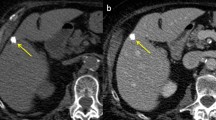
HHs can be broadly classified as capillary hemangiomas or cavernous hemangiomas. While the exact pathophysiology related to the development of HHs remains largely unknown, hormone exposure has been postulated to cause HH growth. HHs appear homogenously hyperechoic on US with distinct margins and posterior acoustic enhancement. While cavernous hemangiomas appear as well-defined hypodense lesions on pre-contrast CT images with the same density as the vasculature, one of the most reliable imaging features for diagnosing cavernous hemangiomas is high signal intensity on T2 weighted images. While most HHs are asymptomatic, some patients can present with pain or compressive symptoms with bleeding/rupture being very rare. Kasabach-Merritt syndrome is a rare but life-threatening condition associated with thrombocytopenia and microangiopathic hemolytic anemia. When HHs are symptomatic or in the setting of Kasabach Merritt syndrome, surgery is indicated. Enucleation is an attractive surgical option for HH as it spares normal liver tissue. Most patients experience symptom relief following surgical resection.
Conclusion
HHs are very common benign liver lesions. High-quality imaging is imperative to distinguish HHs from other liver lesions. Surgery is generally reserved for patients who present with symptoms such as pain, obstruction, or rarely Kasabach-Merritt syndrome. Surgery can involve either formal resection or, in most instances, simple enucleation. Patients generally have good outcomes following surgery with resolution of their symptoms.



Similar content being viewed by others
References
Leon M, Chavez L, Surani S. Hepatic hemangioma: What internists need to know. World journal of gastroenterology. 2020;26(1):11-20.
Bajenaru N, Balaban V, Săvulescu F, Campeanu I, Patrascu T. Hepatic hemangioma -review. J Med Life. 2015;8 Spec Issue(Spec Issue):4-11.
Belghiti J, Cauchy F, Paradis V, Vilgrain V. Diagnosis and management of solid benign liver lesions. Nature reviews Gastroenterology & hepatology. 2014;11(12):737-749.
Roebuck D, Sebire N, Lehmann E, Barnacle A. Rapidly involuting congenital haemangioma (RICH) of the liver. Pediatr Radiol. 2012;42(3):308-314.
Glinkova V, Shevah O, Boaz M, Levine A, Shirin H. Hepatic haemangiomas: possible association with female sex hormones. Gut. 2004;53(9):1352-1355.
Choi BY, Nguyen MH. The diagnosis and management of benign hepatic tumors. Journal of clinical gastroenterology. 2005;39(5):401-412.
Baker ER, Manders E, Whitney CW. Growth of cavernous hemangioma with puberty. Clin Pediatr (Phila). 1985;24(10):596-598.
Sun ZY, Yang L, Yi CG, et al. Possibilities and potential roles of estrogen in the pathogenesis of proliferation hemangiomas formation. Med Hypotheses. 2008;71(2):286-292.
Xiao X, Liu J, Sheng M. Synergistic effect of estrogen and VEGF on the proliferation of hemangioma vascular endothelial cells. J Pediatr Surg. 2004;39(7):1107-1110.
Spitzer D, Krainz R, Graf AH, Menzel C, Staudach A. Pregnancy after ovarian stimulation and intrauterine insemination in a woman with cavernous macrohemangioma of the liver. A case report. J Reprod Med. 1997;42(12):809-812.
Pais-Costa S, Speranzini M, Horta S, Miotto M, Adriano M, Henriques A. Surgical treatment of painful hepatic hemangioma. Einstein. 2009;7.
Braun V, Prey S, Gurioli C, et al. Congenital haemangiomas: a single-centre retrospective review. BMJ Paediatr Open. 2020;4(1):e000816.
Aziz H, Brown ZJ, Eskander MF, et al. A Scoping Review of the Classification, Diagnosis, and Management of Hepatic Adenomas. Journal of gastrointestinal surgery : official journal of the Society for Surgery of the Alimentary Tract. 2022;26(4):965-978.
Dane B, Shanbhogue K, Menias CO, Taffel MT. The humbling hemangioma: uncommon CT and MRI imaging features and mimickers of hepatic hemangiomas. Clinical imaging. 2021;74:55-63.
Colakoğlu O, Taşkiran B, Yazici N, Buyraç Z, Unsal B. Safety of biopsy in liver hemangiomas. Turk J Gastroenterol. 2005;16(4):220-223.
Heilo A, Stenwig AE. Liver hemangioma: US-guided 18-gauge core-needle biopsy. Radiology. 1997;204(3):719-722.
Kim JM, Chung WJ, Jang BK, et al. Hemorrhagic hemangioma in the liver: A case report. World journal of gastroenterology. 2015;21(23):7326-7330.
HASHEMI J, ESMAEILZADEH A, DABAGH KAKHAKI VR, HOSSEINI MR. ACCURACY OF GRAY-SCALE AND COLOR DOPPLER SONOGRAPHY IN DIAGNOSIS OF HEPATIC HEMANGIOMA, HEPATOCELLULAR CARCINOMA AND LIVER METASTASIS. IRANIAN JOURNAL OF RADIOLOGY. 2008;5(3):-.
Kim TK, Han JK, Kim AY, Park SJ, Choi BI. Signal from hepatic hemangiomas on power Doppler US: real or artefactual? Ultrasound Med Biol. 1999;25(7):1055-1061.
Klotz T, Montoriol PF, Da Ines D, Petitcolin V, Joubert-Zakeyh J, Garcier JM. Hepatic haemangioma: common and uncommon imaging features. Diagn Interv Imaging. 2013;94(9):849-859.
Vilgrain V, Boulos L, Vullierme MP, Denys A, Terris B, Menu Y. Imaging of atypical hemangiomas of the liver with pathologic correlation. Radiographics. 2000;20(2):379-397.
Mamone G, Di Piazza A, Carollo V, et al. Imaging of hepatic hemangioma: from A to Z. Abdominal radiology (New York). 2020;45(3):672-691.
Mathew RP, Sam M, Raubenheimer M, Patel V, Low G. Hepatic hemangiomas: the various imaging avatars and its mimickers. Radiol Med. 2020;125(9):801-815.
Hasan HY, Hinshaw JL, Borman EJ, Gegios A, Leverson G, Winslow ER. Assessing normal growth of hepatic hemangiomas during long-term follow-up. JAMA surgery. 2014;149(12):1266-1271.
Ribeiro MA, Jr., Papaiordanou F, Gonçalves JM, Chaib E. Spontaneous rupture of hepatic hemangiomas: A review of the literature. World J Hepatol. 2010;2(12):428-433.
Miura JT, Amini A, Schmocker R, et al. Surgical management of hepatic hemangiomas: a multi-institutional experience. HPB : the official journal of the International Hepato Pancreato Biliary Association. 2014;16(10):924-928.
Corigliano N, Mercantini P, Amodio PM, et al. Hemoperitoneum from a spontaneous rupture of a giant hemangioma of the liver: report of a case. Surg Today. 2003;33(6):459-463.
Cao Y, Xiong F, Xiong B, et al. A case of spontaneous hepatic hemangioma rupture: Successful management with transarterial chemoembolization alone. J Interv Med. 2019;2(3):131-133.
Zhang X, Yan L, Li B, et al. Comparison of laparoscopic radiofrequency ablation versus open resection in the treatment of symptomatic-enlarging hepatic hemangiomas: a prospective study. Surgical endoscopy. 2016;30(2):756-763.
Qiu J, Chen S, Wu H. Quality of life can be improved by surgical management of giant hepatic haemangioma with enucleation as the preferred option. HPB : the official journal of the International Hepato Pancreato Biliary Association. 2015;17(6):490-494.
Schnelldorfer T, Ware AL, Smoot R, Schleck CD, Harmsen WS, Nagorney DM. Management of giant hemangioma of the liver: resection versus observation. Journal of the American College of Surgeons. 2010;211(6):724-730.
Etemadi A, Golozar A, Ghassabian A, et al. Cavernous hemangioma of the liver: factors affecting disease progression in general hepatology practice. European journal of gastroenterology & hepatology. 2011;23(4):354-358.
Toro A, Mahfouz AE, Ardiri A, et al. What is changing in indications and treatment of hepatic hemangiomas. A review. Ann Hepatol. 2014;13(4):327-339.
Aslan A, Meyer Zu Vilsendorf A, Kleine M, Bredt M, Bektas H. Adult Kasabach-Merritt Syndrome due to Hepatic Giant Hemangioma. Case Rep Gastroenterol. 2009;3(3):306-312.
Sharma V, Aggarwal A, Singla R, Kalra N, Chawla YK. Giant hemangioma causing budd-Chiari syndrome. J Clin Exp Hepatol. 2014;4(4):380-381.
Ozden I, Emre A, Alper A, et al. Long-term results of surgery for liver hemangiomas. Archives of surgery (Chicago, Ill : 1960). 2000;135(8):978-981.
Farges O, Daradkeh S, Bismuth H. Cavernous hemangiomas of the liver: are there any indications for resection? World journal of surgery. 1995;19(1):19-24.
Zhang W, Huang ZY, Ke CS, et al. Surgical Treatment of Giant Liver Hemangioma Larger Than 10 cm: A Single Center’s Experience With 86 Patients. Medicine. 2015;94(34):e1420.
Singh RK, Kapoor S, Sahni P, Chattopadhyay TK. Giant haemangioma of the liver: is enucleation better than resection? Annals of the Royal College of Surgeons of England. 2007;89(5):490-493.
Lee JH, Yoon CJ, Kim YH, et al. Living-donor liver transplantation for giant hepatic hemangioma with diffuse hemangiomatosis in an adult: a case report. Clin Mol Hepatol. 2018;24(2):163-168.
Jiang H, Chen Z, Prasoon P, Wu H, Zeng Y. Surgical Management for Giant liver Hemangiomas Greater Than 20 cm in size. Gut and liver. 2011;5(2):228-233.
Zimmermann A, Baer HU. Fibrous tumor-liver interface in large hepatic neoplasms: its significance for tumor resection and enucleation. Liver Transpl Surg. 1996;2(3):192-199.
Yedibela S, Alibek S, Müller V, et al. management of hemangioma of the liver: surgical therapy or observation? World journal of surgery. 2013;37(6):1303-1312.
Falappa P, Preziosi P, Cotroneo AR, Danza FM. Hepatic hemangiomas on 33 patients. Evaluation by ultrasound, nuclear medicine, computed tomography and angiography. Diagn Imaging. 1983;52(5):245-254.
Prodromidou A, Machairas N, Garoufalia Z, et al. Liver Transplantation for Giant Hepatic Hemangioma: A Systematic Review. Transplant Proc. 2019;51(2):440-442.
Vagefi PA, Klein I, Gelb B, et al. Emergent orthotopic liver transplantation for hemorrhage from a giant cavernous hepatic hemangioma: case report and review. Journal of gastrointestinal surgery : official journal of the Society for Surgery of the Alimentary Tract. 2011;15(1):209-214.
Meguro M, Soejima Y, Taketomi A, et al. Living donor liver transplantation in a patient with giant hepatic hemangioma complicated by Kasabach-Merritt syndrome: report of a case. Surg Today. 2008;38(5):463-468.
Longeville JH, de la Hall P, Dolan P, et al. treatment of a giant haemangioma of the liver with Kasabach-Merritt syndrome by orthotopic liver transplant a case report. HPB Surg. 1997;10(3):159-162.
Yamamoto T, Kawarada Y, Yano T, Noguchi T, Mizumoto R. Spontaneous rupture of hemangioma of the liver: treatment with transcatheter hepatic arterial embolization. Am J Gastroenterol. 1991;86(11):1645-1649.
Hanks BA, Suhocki PV, DeLong DM, et al. The efficacy and tolerability of transarterial chemo-embolization (TACE) compared with transarterial embolization (TAE) for patients with unresectable hepatocellular carcinoma (HCC). Journal of Clinical Oncology. 2008;26(15_suppl):4595-4595.
Torkian P, Li J, Kaufman JA, Jahangiri Y. Effectiveness of Transarterial Embolization in Treatment of Symptomatic Hepatic Hemangiomas: Systematic Review and Meta-analysis. Cardiovascular and interventional radiology. 2021;44(1):80-91.
Shimizu S, Mizumoto M, Okumura T, et al. Proton beam therapy for a giant hepatic hemangioma: A case report and literature review. Clin Transl Radiat Oncol. 2021;27:152-156.
Biswal BM, Sandhu M, Lal P, Bal CS. Role of radiotherapy in cavernous hemangioma liver. Indian J Gastroenterol. 1995;14(3):95-98.
Creasy GW, Flickinger F, Kraus RE. Maternal liver hemangioma in pregnancy as an incidental finding. Obstet Gynecol. 1985;66(3 Suppl):10s-13s.
Ji Y, Chen S, Xiang B, et al. Clinical features and management of multifocal hepatic hemangiomas in children: a retrospective study. Scientific reports. 2016;6:31744.
Xie QS, Chen ZX, Zhao YJ, Gu H, Geng XP, Liu FB. Outcomes of surgery for giant hepatic hemangioma. BMC surgery. 2021;21(1):186.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Aziz, H., Brown, Z.J., Baghdadi, A. et al. A Comprehensive Review of Hepatic Hemangioma Management. J Gastrointest Surg 26, 1998–2007 (2022). https://doi.org/10.1007/s11605-022-05382-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-022-05382-1