Abstract
Objective
Exploring the efficacy of a Radiological-Clinical (Rad-Clinical) model in predicting prognosis of unresectable hepatocellular carcinoma (HCC) patients after drug eluting beads transcatheter arterial chemoembolization (DEB-TACE) to optimize the targeted sequential treatment.
Methods
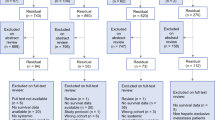
In this retrospective analysis, we included 202 patients with unresectable HCC who received DEB-TACE treatment in 17 institutions from June 2018 to December 2022. Progression-free survival (PFS)-related radiomics features were computationally extracted from HCC patients to build a radiological signature (Rad-signature) model with least absolute shrinkage and selection operator regression. A Rad-Clinical model for postoperative PFS was further constructed according to the Rad-signature and clinical variables by Cox regression analysis. It was presented as a nomogram and evaluated by receiver operating characteristic curves, calibration curves, and decision curve analysis. And further evaluate the application value of Rad-Clinical model in clinical stages and targeted sequential therapy of HCC.
Results
Tumor size, Barcelona Clinic Liver Cancer (BCLC) stage, and radiomics score (Rad-score) were found to be independent risk factors for PFS after DEB-TACE treatment for unresectable HCC, with the Rad-Clinical model being the greatest predictor of PFS in these patients (hazard ratio: 2.08; 95% confidence interval: 1.56–2.78; P < 0.001) along with high 6 months, 12 months, 18 months, and 24 months area under the curves of 0.857, 0.810, 0.843, and 0.838, respectively. In addition, compared to the radiomics and clinical nomograms, the Radiological-Clinical nomogram also significantly improved the classification accuracy for PFS outcomes, based on the net reclassification improvement (45.2%, 95% CI 0.260–0.632, p < 0.05) and integrated discrimination improvement (14.9%, 95% CI 0.064–0.281, p < 0.05). Based on this model, low-risk patients had higher PFS than high-risk patients in BCLC-B and C stages (P = 0.021). Targeted sequential therapy for patients with high and low-risk HCC in BCLC-B stage exhibited significant benefits (P = 0.018, P = 0.012), but patients with high-risk HCC in BCLC-C stage did not benefit much (P = 0.052).
Conclusion
The Rad-Clinical model may be favorable for predicting PFS in patients with unresectable HCC treated with DEB-TACE and for identifying patients who may benefit from targeted sequential therapy.







Similar content being viewed by others
Data availability
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Heimbach JK, Kulik LM, Finn RS et al (2018) AASLD guidelines for the treatment of hepatocellular carcinoma. Hepatology 67(1):358–380. https://doi.org/10.1002/hep.29086
Galle PR, Forner A, Llovet JM et al (2018) EASL clinical practice guidelines: management of hepatocellular carcinoma. J Hepatol 69(1):182–236. https://doi.org/10.1016/j.jhep.2018.03.019
Liu KC, Lv WF, Lu D et al (2021) Initial experience of drug-eluting bead-transcatheter arterial chemoembolization after lipiodol-based transcatheter arterial chemoembolization failure for patients with advanced hepatocellular carcinoma. Cancer Manag Res. https://doi.org/10.2147/cmar.S332571
Wang XH, Long LH, Cui Y et al (2020) MRI-based Radiomics model for preoperative prediction of 5-year survival in patients with hepatocellular carcinoma. Br J Cancer 122(7):1–8. https://doi.org/10.1038/s41416-019-0706-0
Meng XP, Wang YC, Ju S et al (2020) Radiomics analysis on multiphase contrast-enhanced CT: a survival prediction tool in patients with hepatocellular carcinoma undergoing transarterial chemoembolization. Front Oncol 10:1196. https://doi.org/10.3389/fonc.2020.01196
Hu K, Lu S, Li M et al (2020) A novel pre-treatment model predicting risk of developing refractoriness to transarterial chemoembolization in unresectable hepatocellular carcinoma. J Cancer 11(15):4589–4596. https://doi.org/10.7150/jca.44847
Cannella R, Cammà C, Matteini F et al (2022) Radiomics analysis on gadoxetate disodium-enhanced MRI predicts response to transarterial embolization in patients with HCC. Diagnostics 12(6):1308. https://doi.org/10.3390/diagnostics12061308
Ananchuensook P, Sriphoosanaphan S, Suksawatamnauy S et al (2022) Validation and prognostic value of EZ-ALBI score in patients with intermediate-stage hepatocellular carcinoma treated with trans-arterial chemoembolization. BMC Gastroenterol 22(1):295. https://doi.org/10.1186/s12876-022-02366-y
Hiraoka A, Kumada T, Kariyama K et al (2022) Simple scoring system for predicting TACE unsuitable among intermediate-stage hepatocellular carcinoma patients in the multiple systemic treatment era. Oncology 100(2):65–73. https://doi.org/10.1159/000520292
Han G, Berhane S, Toyoda H et al (2020) Prediction of survival among patients receiving transarterial chemoembolization for hepatocellular carcinoma: a response-based approach. Hepatology 72(1):198–212. https://doi.org/10.1002/hep.31022
Kadalayil L, Benini R, Pallan L et al (2022) A simple prognostic scoring system for patients receiving transarterial embolisation for hepatocellular cancer. Ann Oncol 24(10):2565–2570. https://doi.org/10.1093/annonc/mdt247
Forner A, Reig M, Bruix J et al (2018) Hepatocellular carcinoma. Lancet 391(10127):1301–1314. https://doi.org/10.1016/s0140-6736(18)30010-20
Lambin P, Leijenaar RTH, Deist TM et al (2017) Radiomics: the bridge between medical imaging and personalized medicine. Nat Rev Clin Oncol 14(12):749–762. https://doi.org/10.1038/nrclinonc.2017.141
Miller KD, Nogueira L, Mariotto AB et al (2019) Cancer treatment and survivorship statistics. CA Cancer J Clin 69(5):363–385. https://doi.org/10.3322/caac.21565
Xu H, Guo W, Cui X et al (2019) Three-dimensional texture analysis based on PET/CT images to distinguish hepatocellular carcinoma and hepatic lymphoma. Front Oncol 9:844. https://doi.org/10.3389/fonc.2019.00844
Fu S, Chen S, Liang C et al (2017) Texture analysis of intermediate-advanced hepatocellular carcinoma: prognosis and patients’ selection of transcatheter arterial chemoembolization and sorafenib. Oncotarget 8(23):37855–37865. https://doi.org/10.18632/oncotarget.13675
Vosshenrich J, Zech CJ, Heye T et al (2021) Response prediction of hepatocellular carcinoma undergoing transcatheter arterial chemoembolization: unlocking the potential of CT texture analysis through nested decision tree models. Eur Radiol 31(6):4367–4376. https://doi.org/10.1007/s00330-020-07511-3
Wang XH, Long LH, Cui Y et al (2020) MRI-based radiomics model for preoperative prediction of 5-year survival in patients with hepatocellular carcinoma. Br J Cancer 122(7):978–985. https://doi.org/10.1038/s41416-019-0706-0
Collins GS, Reitsma JB, Altman DG et al (2015) Transparent reporting of a multivariable prediction model for individual prognosis or diagnosis (TRIPOD): the TRIPOD statement. BMJ 350:g7594. https://doi.org/10.1136/bmj.g7594
Lv WF, Liu KC, Lu D et al (2018) Transarterial chemoembolization for hepatocellular carcinoma combined with portal vein tumor thrombosis. Cancer Manag Res 10:4719–4726. https://doi.org/10.2147/cmar.S166527
Chen Y, Xu WJ, Yang Y et al (2022) Nomograms including the controlling nutritional status score in patients with hepatocellular carcinoma undergoing transarterial chemoembolisation for prediction survival: a retrospective analysis. Br J Nutr 128(10):1966–1974. https://doi.org/10.1017/s000711452100492x
Noh B, Park YM, Kwon Y et al (2022) Machine learning-based survival rate prediction of Korean hepatocellular carcinoma patients using multi-center data. BMC Gastroenterol 22(1):85. https://doi.org/10.1186/s12876-022-02182-4
Luo J, Huang Z, Wang M et al (2022) Prognostic role of multiparameter MRI and radiomics in progression of advanced unresectable hepatocellular carcinoma following combined transcatheter arterial chemoembolization and lenvatinib therapy. BMC Gastroenterol 22(1):108. https://doi.org/10.1186/s12876-022-02129-9
Sun ZQ, Shi ZX, Xin YJ et al (2023) Contrast-enhanced CT imaging features combined with clinical factors to predict the effificacy and prognosis for transarterial chemoembolization of hepatocellular carcinoma. Acad Radiol. https://doi.org/10.1016/j.acra.2022.12.031
Fan XL, Wang YH, Chen YH et al (2023) Computed tomography texture analysis combined with preoperative clinical factors serve as a predictor of early efcacy of transcatheter arterial chemoembolization in hepatocellular carcinoma. Abdom Radiol 48(6):2008–2018. https://doi.org/10.1007/s00261-023-03868-3
Aerts HJ (2016) The potential of radiomic-based phenotyping in precision medicine: a review. JAMA Oncol 2(12):1636–1642. https://doi.org/10.1001/jamaoncol.2016.2631
Liu Z, Meng X, Zhang H et al (2020) Predicting distant metastasis and chemotherapy benefit in locally advanced rectal cancer. Nat Commun 11(1):4308. https://doi.org/10.1038/s41467-020-18162-9
Sun KY, Hu HT, Chen SL et al (2020) CT-based radiomics scores predict response to neoadjuvant chemotherapy and survival in patients with gastric cancer. BMC Cancer 20(1):468. https://doi.org/10.1186/s12885-020-06970-7
General Office of National Health Commission (2022) Standard for diagnosis and treatment of primary liver cancer (2022 edition). J Clin Hepatol 38(2):288–303. https://doi.org/10.3969/j.issn.1001-5256.2022.02.009
Villanueva A (2019) Hepatocellular carcinoma. N Encl J Med 380(15):1450–1462. https://doi.org/10.1056/NEJMra1713263
Liu KC, Hao YH, Lv WF et al (2020) Transarterial chemoembolization combined with sorafenib in patients with BCLC stage C hepatocellular carcinoma. Drug Des Devel Ther 14:3461–3468. https://doi.org/10.2147/dddt.S248850
Zhao Y, Wang N, Wu J et al (2021) Radiomics analysis based on contrast-enhanced MRI for prediction of therapeutic response to transarterial chemoembolization in hepatocellular carcinoma. Front Oncol 11:582788. https://doi.org/10.3389/fonc.2021.582788
Li Y, Zhang Y, Fang Q et al (2021) Radiomics analysis of [18F]FDG PET/CT for microvascular invasion and prognosis prediction in very-early- and early-stage hepatocellular carcinoma. Eur J Nucl Med Mol Imag 48(8):2599–2614. https://doi.org/10.1007/s00259-020-05119-9
Acknowledgements
Thank you for the support of the ShuKun (Beijing) Technology Co., Ltd.
Funding
The study was supported by the 2022 Collaborative Innovation Project between Universities and Hefei Comprehensive National Science Center (GXXT-2022-031), 2022 Hefei Health Applied Medicine Research Project (Hwk2022yb033) and Research Funds for Academic and Technological Leaders in Anhui Province of China (2021D299).
Author information
Authors and Affiliations
Contributions
KCL, XMZ, WFL, and XWW conceived and supervised the study; RWC, WGZ, JX, LC, MYJ, ZZ, LL, and JL collected the data; DL, YLT, JYD, CLH, WYS, BJ, YBY, YHL, and QSC analyzed data; KCL, XMZ and JYL performed the statistical analysis, XWW, WFL, and KCL received the fund; KCL and XMZ completed the design and conception starting from the article, as well as the literature search in the early stages. We also worked together on data analysis and article writing; WFL and XWW made manuscript revisions. All authors reviewed the results and approved the final version of the manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
All authors have no conflict of interest to disclosure.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Appendix E
Appendix E
DEB-TACE
After digital subtraction angiography (DSA) was performed to determine the tumor blood vessels, a 2.7-F micro-catheter (Cook, USA) was applied to inject 100 to 300um (or 300 to 500um) CalliSpheres drug elating hemispheres (Jiangsu Hengrui Medicine, Jiangshu, China) loaded with 80 mg pirarubicin for tumor embolization, and the main blood supply artery was embolized with a mixture of gelatin sponge particles and contrast agent until the blood supply was completely blocked. We used the modified Response Evaluation Criteria in Solid Tumors (mRECIST) standard to evaluate the changes in the lesions. If there are no active lesions at 1 month after DEB-TACE, enhanced CT imaging will be reviewed and judged every 3 months. If there are active lesions, DEB-TACE treatment will be repeated. The numbers of TACE treatment in this study was 1–5.
CT protocols of the seventeen institutions
All patients underwent unenhanced and triphasic dynamic contrast-enhanced CT scans before DEB-TACE. Enrolled patients at the 17 institutions had similar scan setup: Using the bolus-tracking method, the arterial phase was scanned at 15–20 s after 100-Houndsfeld unit attenuation of the abdominal aorta. The portal venous and delayed phases were obtained at 70 and 180 s, respectively, after contrast injection. Technical details of CT protocols at the seventeen institutions are outlined in Table S1.
Intra-observer and inter-observer agreement
The intra-observer agreement and inter-observer agreement of feature extraction were evaluated by correlation coefficients (ICCs). To compute the intra-observer ICC, 50 CT images were selected randomly and segmented twice in 1 month (At least 10 days apart) by reader A. To compute the inter-observer ICC, the selected images were segmented by two radiologists independently (reader A and reader B). Segmentation was performed to further obtain independent feature extraction to compute the intra-observer and inter-observer ICCs. When the ICC was greater than 0.75, it was considered good agreement, and the remaining segmentation was performed by reader A.
Features extraction and rad-signature model establishment
Feature screening unifies the scales of different features through the Z-score normalization method, so that the antiquated feature scales are distributed between 0 and 1. Firstly, pair-wise correlation analysis was performed to remove redundant radiological features, by using the “find Correlation” function in R package “caret” with the absolute correlation cutoff set at 0.9. Then, we employed the least absolute shrinkage and selection operator (LASSO) Cox regression, a qualified approach for regression of high-dimensional predictors by a penalty to shrink some regression coefficients to exactly zero. This approach selected the most predictive radiomics features from the training cohort. The penalty parameter (lambda) was determined by using a fivefold cross-validation based on minimum error criteria. Selected features were weighed by their respective coefficients obtained from LASSO, and were used to compute a radiomics signature (Rad-signature) with a linear combination. Rad-signature model was constructed by Cox regression.
The R packages used for statistical analysis
We used the “glmnet” package to perform the LASSO-Cox regression. The “rms” package was used for multivariable Cox regression analysis, nomogram construction, and calibration. The “DynNom” package was used to build dynamic nomograms on the web. The R function cox.zph was employed to test the proportional hazards assumption for a Cox regression model fit. The Cindex was calculated and compared using function concordance.index and cindex.comp in the “survcomp” package. Prediction error curves were generated using “pec” package. Decision curve analysis was performed using the “stdca.R” package. We used the “timeROC” package to do the time-dependent ROC curve analysis.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Liu, K., Zheng, X., Lu, D. et al. A multi-institutional study to predict the benefits of DEB-TACE and molecular targeted agent sequential therapy in unresectable hepatocellular carcinoma using a radiological-clinical nomogram. Radiol med 129, 14–28 (2024). https://doi.org/10.1007/s11547-023-01736-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11547-023-01736-0