Abstract
Purpose
This study aims to evaluate the diagnostic value of pelvic arteriography in patients with pelvic ring fractures and associated large hematomas, in both cases of positive or negative findings of contrast agent extravasation at emergency CT; in those patients with positive DSA subsequently treated with embolization, correlations with clinical–radiological parameters were investigated.
Materials and methods
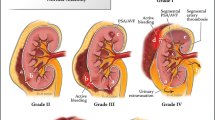
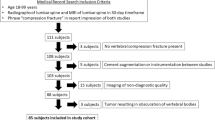
In this single-center retrospective study, patients with acute blunt pelvic trauma showing at CT pelvic ring fractures with associated large (> 3 cm) hematoma, with or without signs of arterial bleeding, were investigated with DSA. Technical success was considered radiographic bleeding control with disappearance of angiographic bleeding; clinical success was defined as clinical bleeding control hemodynamically stable, before applying other surgical maneuvers. Pelvic ring fractures were evaluated according to Tile classification system.
Results
One hundred and fifty-seven patients, mean age 54years, were analyzed. 70.7% had polytrauma; 14.6% patients assumed antiplatelets and/or anticoagulation therapy. False-negative and false-positive rates at CT were 29.6% and 27.1%, respectively. Polytrauma and B3/C1 Tile pattern fractures were significantly associated with bleeding signs at DSA. Seventy-two patients required embolization: 52.8% showed direct signs of DSA bleeding; among these, technical and clinical successes were 88.8% and 81.9%, respectively.
Conclusions
In this study, patients with pelvic ring fractures and concomitant hematomas > 3 cm, with or without contrast extravasation at CT, have been examined in depth with DSA focusing on both direct and indirect angiographic signs of bleeding, finding polytrauma and Tile fracture patterns B3/C1 predictive factors for arterial hemorrhage detection at DSA despite negative CT findings.





Similar content being viewed by others
Change history
28 September 2023
In the original version of this article, the fourth author’s name was published incorrectly as “Edoardo Casciano” instead of “Eduardo Casciano” and has now been corrected.
11 October 2023
A Correction to this paper has been published: https://doi.org/10.1007/s11547-023-01729-z
References
Ierardi AM, Duka E, Lucchina N et al (2016) The role of interventional radiology in abdominopelvic trauma. Br J Radiol 89(1061):20150866
Ierardi AM, Piacentino F, Fontana F et al (2015) The role of endovascular treatment of pelvic fracture bleeding in emergency settings. Eur Radiol 25(7):1854–64
Hoff WS, Holevar M, Nagy KK et al (2002) Eastern asociation for the surgery of Trauma. Practice management guidelines for the evaluation of blunt abdominal trauma: the East practice management guidelines work group. J Trauma 53(3):602–15
Huber-Wagner S, Lefering R, Qvick LM et al (2009) Effect of wholebody CT during trauma resuscitation on survival: a retrospective, multicentre study. Lancet 373(9673):1455–1461
Chidambaram S, Goh EL, Khan MA (2017) A meta-analysis of the efficacy of whole-body computed tomography imaging in the management of trauma and injury. Injury 48(8):1784–1793
Raniga SB, Mittal AK, Bernstein M, Skalski MR, Al-Hadidi AM (2019) Multidetector CT in vascular injuries resulting from pelvic fractures: a primer for diagnostic radiologists. Radiographics 39(7):2111–2129
Dreizin D, Bodanapally U, Boscak A et al (2018) CT prediction model for major arterial injury after blunt pelvic ring disruption. Radiology 287(3):1061–1069
Miller PR, Moore PS, Mansell E, Meredith JW, Chang MC (2005) External fixation or arteriogram in bleeding pelvic fracture: initial therapy guided by markers of arterial hemorrhage. J Trauma 54(3):437–443
Dreizin D, Liang Y, Dent J, Akhter N, Mascarenhas D, Scalea TM (2020) Diagnostic value of CT contrast extravasation for major arterial injury after pelvic fracture: a meta-analysis. Am J Emerg Med 38(11):2335–2342
Hallinan JT, Tan CH, Pua U (2014) Emergency computed tomography for acute pelvic trauma: where is the bleeder? Clin Radiol 69(5):529–37
Coccolini F, Stahel PF, Montori G et al (2017) Pelvic trauma: WSES classification and guidelines. World J Emerg Surg. 18:12–15
Iacobellis F, Scaglione M, Brillantino A et al (2019) The additional value of the arterial phase in the CT assessment of liver vascular injuries after high-energy blunt trauma. Emerg Radiol 26(6):647–654
Tile M (1988) Pelvic ring fractures: should they be fixed? J Bone Joint Surg Br 70(1):1–12
Niola R, Pinto A, Sparano A, Ignarra R, Romano L, Maglione F (2012) Arterial bleeding in pelvic trauma: priorities in angiographic embolization. Curr Probl Diagn Radiol 41(3):93–101
Filippiadis DK, Binkert C, Pellerin O, Hoffmann RT, Krajina A, Pereira PL (2017) Cirse quality assurance document and standards for classification of complications: the Cirse classification system. Cardiovasc Interv Radiol 40(8):1141–1146
Salim A, Teixeira PG, DuBose J et al (2008) Predictors of positive angiography in pelvic fractures: a prospective study. J Am Coll Surg 207(5):656–662
Kuo L-W, Yang S-J, Fu C-Y, Liao C-H, Wang S-Y, Wu S-C (2016) Relative hypotension increases the probability of the need for angioembolisation in pelvic fracture patients without contrast extravasation on computed tomography scan. Injury 47(1):37–42
Brasel KJ, Pham K, Yang H, Christensen R, Weigelt JA (2007) Significance of contrast extravasation in patients with pelvic fracture. J Trauma Acute Care Surg 62(5):1149–1152
Lee HJ, No HK, Choi NJ et al (2020) The size of pelvic hematoma can be a predictive factor for angioembolization in hemodynamically unstable pelvic trauma. Ann Surg Treat Res 98(3):146–152
Uyeda J, Anderson SW, Kertesz J, Soto JA (2010) Pelvic CT angiography: application to blunt trauma using 64MDCT. Emerg Radiol 17(2):131–7
Lindahl J, Handolin L, Söderlund T, Porras M, Hirvensalo E (2013) Angiographic embolization in the treatment of arterial pelvic hemorrhage: evaluation of prognostic mortality-related factors. Eur J Trauma Emerg Surg 39(1):57–63
Hauschild O, Aghayev E, von Heyden J et al (2012) Angioembolization for pelvic hemorrhage control: results from the German pelvic injury register. J Trauma Acute Care Surg 73(3):679–684
Gourlay D, Hoffer E, Routt M, Bulger E (2005) Pelvic angiography for recurrent traumatic pelvic arterial hemorrhage. J Trauma 59(5):1168–1174
Gurevitz S, Bender B, Tytiun Y, Velkes S, Salai M, Stein M (2005) The role of pelvic fractures in the course of treatment and outcome of trauma patients. Isr Med Assoc J 7(10):623–626
Dreizin D, Nascone J, Davis DL et al (2016) Can MDCT unmask instability in binder-stabilized pelvic ring disruptions? AJR Am J Roentgenol 207(6):1244–1251
Spanjersberg WR, Knops SP, Schep NW, van Lieshout EM, Patka P, Schipper IB (2009) Effectiveness and complications of pelvic circumferential compression devices in patients with unstable pelvic fractures: a systematic review of literature. Injury 40(10):1031–1035
Meinberg E, Agel J, Roberts C, Karam M, Kellam J (2018) Fracture and dislocation classification compendium—2018. J Orthop Trauma 32(1):S1–S10
Burgess AR, Eastridge BJ, Young JW et al (1990) Pelvic ring disruptions: effective classification system and treatment protocols. J Trauma 30(7):848–856
Tile M (1996) Acute pelvic fractures. I. Causation and classification. J Am Acad Orthop Surg 4(3):143–151
Bonde A, Velmahos A, Kalva SP, Mendoza AE, Kaafarani HMA, Nederpelt CJ (2020) Bilateral internal iliac artery embolization for pelvic trauma: effectiveness and safety. Am J Surg 220(2):454–458
Brohi K, Jasmin S, Heron M, Coats T (2003) Acute traumatic coagulopathy. J Trauma 54:1127–1130
Cosgriff N, Moore EE, Sauaia A, Kenny-Moynihan M, Burch JM, Galloway B (1997) Predicting life-threatening coagulopathy in the massively transfused trauma patient: hypothermia and acidoses revisited. J Trauma 42(5):857–861
Awwad A, Dhillon PS, Ramjas G, Habib SB, Al-Obaydi W (2018) Trans-arterial embolisation (TAE) in haemorrhagic pelvic injury: review of management and mid-term outcome of a major trauma centre. CVIR Endovasc 1(1):32
Cullinane DC, Schiller HJ, Zielinski MD, Bilaniuk JW, Collier BR, Como J et al (2011) Eastern association for the surgery of trauma practice management guidelines for hemorrhage in pelvic fracture-update and systematic review. J Trauma 71(6):1850–1868
Barentsz MW, Vonken EPA, van Herwaarden JA, Leenen LPH, Mali WPTM, van den Bosch MAAJ (2011) Clinical outcome of intra-arterial embolization for treatment of patients with pelvic trauma. Radiol Res Pract 2011:1–7
Metsemakers WJ, Vanderschot P, Jennes E, Nijs S, Heye S, Maleux G (2013) Transcatheter embolotherapy after external surgical stabilization is a valuable treatment algorithm for patients with persistent haemorrhage from unstable pelvic fractures: outcomes of a single centre experience. Injury 44(7):964–968
Brotman S, Soderstrom CA, Oster-Granite M, Cisternino S, Browner B, Cowley RA (1981) Management of severe bleeding in fractures of the pelvis. Surg Gynecol Obstet 153(6):823–826
Morozumi J, Homma H, Ohta S et al (2010) Impact of mobile angiography in the emergency department for controlling pelvic fracture hemorrhage with hemodynamic instability. J Trauma 68(1):90–95
Stassen NA, Bhullar I, Cheng JD, Crandall ML, Friese RS, Guillamondegui OD et al (2012) Eastern association for the surgery of Trauma. Selective nonoperative management of blunt splenic injury: an Eastern association for the surgery of Trauma practice management guideline. J Trauma Acute Care Surg 73(5):S294–S300
Chakraverty S, Flood K, Kessel D et al (2012) CIRSE guidelines: quality improvement guidelines for endovascular treatment of traumatic hemorrhage. Cardiovasc Interv Radiol 35(3):472–82
Yoshikawa S, Shiraishi A, Kishino M et al (2018) Predictive ability and interobserver reliability of computed tomography findings for angioembolization in patients with pelvic fracture. J Trauma Acute Care Surg 84(2):319–324
Verbeek DO, Zijlstra IA, van der Leij C, Ponsen KJ, van Delden OM, Goslings JC (2014) Management of pelvic ring fracture patients with a pelvic ‘‘blush” on early computed tomography. J Trauma Acute Care Surg 76(2):374–379
Agolini SF, Shah K, Jaffe J, Newcomb J, Rhodes M, Reed JF (1997) Arterial embolization is a rapid and effective technique for controlling pelvic fracture hemorrhage. J Trauma 43(3):395–399
Tanizaki S, Maeda S, Matano H, Sera M, Nagai H, Ishida H (2014) Time to pelvic embolization for hemodynamically unstable pelvic fractures may affect the survival for delays up to 60 min. Injury 45(4):738–741
Blackmore CC, Jurkovich GJ, Linnau KF, Cummings P, Hoffer EK, Rivara FP (2003) Assessment of volume of hemorrhage and outcome from pelvic fracture. Arch Surg 138(5):504–508
Funding
The authors have not disclosed any funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Informed consent
Informed consent was obtained from all patients included in the study, if clinical conditions allowed.
Research involving human participants
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
In the original version of this article, the fourth author’s name was published incorrectly as “Edoardo Casciano” instead of “Eduardo Casciano” and has now been corrected.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Giurazza, F., Pane, F., Roccatagliata, P. et al. Pelvic ring fractures with concomitant large hematomas: diagnostic investigation with arteriography and eventual embolization in 157 trauma patients, with or without contrast extravasation at emergency CT. Radiol med 128, 1429–1439 (2023). https://doi.org/10.1007/s11547-023-01714-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11547-023-01714-6