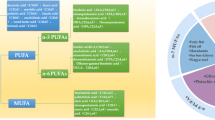
Abstract
Gestational diabetes mellitus (GDM) is a high-prevalence disease and diagnosed in middle pregnancy. Acylcarnitines are a series of fatty acid esters of carnitine and play important roles in fatty acid and carbohydrate metabolism. However, the role of acylcarnitine on the development of GDM remains unclear. This case-control study involving 214 study participants (107 GDM cases and 107 matched controls) was conducted in a cohort, in China, from 2013 to 2015. The levels of carnitine and 36 acylcarnitines in serum samples collected at the early stage of pregnancy were determined by using ultra-high performance liquid chromatography coupled with tandem mass spectrometry. The associations of the levels of the 37 targeted compounds with GDM risk were investigated by using binary conditional logistic regression models. Alterations in acylcarnitine levels were observed 9–17 weeks before GDM diagnosis. The increases in levels of propionyl-carnitine, malonyl-carnitine, isovaleryl-carnitine, palmitoyl-carnitine and linoleoyl-carnitine were associated with GDM risk with odds ratios (ORs) per standard deviation (SD) increment greater than 1 (p<0.05), after adjustment for potential confounding factors (pre-pregnancy body mass index and parity). On the contrary, the increases of decanoyl-carnitine, decenoyl-carnitine, tetradecenoyl-carnitine, tetradecandienoyl-carnitine levels were associated with the reduced risk for GDM (ORs per SD <1, p<0.05). To our knowledge, the present study is the largest case-control study to investigate the association between early-pregnancy acylcarnitine levels in serum and GDM risk. The findings add to the evidence for the association between acylcarnitine levels and GDM risk.
Similar content being viewed by others
References
American Diabetes Association. Diabetes Care, 2019, 42: S13–S28
Sacks DA, Hadden DR, Maresh M, Deerochanawong C, Dyer AR, Metzger BE, Lowe LP, Coustan DR, Hod M, Oats JJN, Persson B, Trimble ER. Diabetes Care, 2012, 35: 526–528
Song C, Lyu Y, Li C, Liu P, Li J, Ma RC, Yang X. Obesity Rev, 2018, 19: 421–429
Tobias DK, Stuart JJ, Li S, Chavarro J, Rimm EB, Rich-Edwards J, Hu FB, Manson JAE, Zhang C. JAMA Intern Med, 2017, 177: 1735–1742
Tam WH, Ma RCW, Ozaki R, Li AM, Chan MHM, Yuen LY, Lao TTH, Yang X, Ho CS, Tutino GE, Chan JCN. Diabetes Care, 2017, 40: 679–686
Landon MB, Rice MM, Varner MW, Casey BM, Reddy UM, Wapner RJ, Rouse DJ, Biggio Jr. JR, Thorp JM, Chien EK, Saade G, Peaceman AM, Blackwell SC, VanDorsten JP. Diabetes Care, 2015, 38: 445–452
Indiveri C, Iacobazzi V, Tonazzi A, Giangregorio N, Infantino V, Convertini P, Console L, Palmieri F. Mol Aspects Med, 2011, 32: 223–233
McCoin CS, Knotts TA, Adams SH. Nat Rev Endocrinol, 2015, 11: 617–625
Aichler M, Borgmann D, Krumsiek J, Buck A, MacDonald PE, Fox JEM, Lyon J, Light PE, Keipert S, Jastroch M, Feuchtinger A, Mueller NS, Sun N, Palmer A, Alexandrov T, Hrabe de Angelis M, Neschen S, Tschöp MH, Walch A. Cell Metab, 2017, 25: 1334–1347.e4
McCabe CF, Perng W. Curr Diab Rep, 2017, 17: 57
Sun L, Liang L, Gao X, Zhang H, Yao P, Hu Y, Ma Y, Wang F, Jin Q, Li H, Li R, Liu Y, Hu FB, Zeng R, Lin X, Wu J. Diabetes Care, 2016, 39: 1563–1570
Powe CE, Tobias DK, Michels KB, Chen WY, Eliassen AH, Manson JAE, Rosner B, Willett WC, Hu FB, Zhang C, Rich-Edwards JW, Rexrode KM. Cancer Epidemiol Biomark Prev, 2017, 26: 321–327
Zhao H, Li H, Chung ACK, Xiang L, Li X, Zheng Y, Luan H, Zhu L, Liu W, Peng Y, Zhao Y, Xu S, Li Y, Cai Z. J Proteome Res, 2019, 18: 292–300
Batchuluun B, Al Rijjal D, Prentice KJ, Eversley JA, Burdett E, Mohan H, Bhattacharjee A, Gunderson EP, Liu Y, Wheeler MB. Diabetes, 2018, 67: 885–897
Nevalainen J, Sairanen M, Appelblom H, Gissler M, Timonen S, Ryynänen M. Rev Diabet Stud, 2016, 13: 236–245
American Diabetes Association. Diabetes Care, 2011, 34(Suppl 1): S62–S69
Xiang L, Wei J, Tian XY, Wang B, Chan W, Li S, Tang Z, Zhang H, Cheang WS, Zhao Q, Zhao H, Yang Z, Hong Y, Huang Y, Cai Z. Anal Chem, 2017, 89: 10368–10375
Benjamini Y, Hochberg Y. J Roy Stat Soc B, 1995, 57: 289–300
Thompson DK, Sloane R, Bain JR, Stevens RD, Newgard CB, Pieper CF, Kraus VB. Metabolomics, 2012, 8: 556–565
Roy C, Tremblay PY, Anassour-Laouan-Sidi E, Lucas M, Forest JC, Giguère Y, Ayotte P. Diabetes Res Clin Pract, 2018, 140: 183–190
Tobias DK, Clish C, Mora S, Li J, Liang L, Hu FB, Manson JAE, Zhang C. Clin Chem, 2018, 64: 1203–1210
Zhang S, Zeng X, Ren M, Mao X, Qiao S. J Anim Sci Biotechnol, 2017, 8: 10
Rousseau M, Guénard F, Garneau V, Allam-Ndoul B, Lemieux S, Pérusse L, Vohl MC. Nutrients, 2019, 11: 173
Lynch CJ, Adams SH. Nat Rev Endocrinol, 2014, 10: 723–736
Newgard CB, An J, Bain JR, Muehlbauer MJ, Stevens RD, Lien LF, Haqq AM, Shah SH, Arlotto M, Slentz CA, Rochon J, Gallup D, Ilkayeva O, Wenner BR, Yancy Jr. WS, Eisenson H, Musante G, Surwit RS, Millington DS, Butler MD, Svetkey LP. Cell Metab, 2009, 9: 311–326
Gucciardi A, Pirillo P, Di Gangi IM, Naturale M, Giordano G. Anal Bioanal Chem, 2012, 404: 741–751
Qiu C, Enquobahrie DA, Frederick IO, Sorensen TK, Fernandez MAL, David RM, Bralley JA, Williams MA. Diabetes Res Clin Pract, 2014, 104: 393–400
Wolfgang MJ, Lane MD. FEBS J, 2011, 278: 552–558
Mai M, Tönjes A, Kovacs P, Stumvoll M, Fiedler GM, Leichtle AB, He B. PLoS ONE, 2013, 8: e82459
O’Sullivan AJ. Obes Rev, 2009, 10: 168–177
Lopaschuk GD. Ann Nutr Metab, 2016, 68: 15–20
Bouchouirab FZ, Fortin M, Noll C, Dubé J, Carpentier AC. Can J Diabetes, 2018, 42: 382–388
Zhang D, Christianson J, Liu ZX, Tian L, Choi CS, Neschen S, Dong J, Wood PA, Shulman GI. Cell Metab, 2010, 11: 402–411
Koves TR, Ussher JR, Noland RC, Slentz D, Mosedale M, Ilkayeva O, Bain J, Stevens R, Dyck JRB, Newgard CB, Lopaschuk GD, Muoio DM. Cell Metab, 2008, 7: 45–56
Gelaye B, Clish CB, Denis M, Larrabure G, Tadesse MG, Deik A, Pierce K, Bullock K, Dennis C, Enquobahrie DA, Williams MA. Diabetes Metab, 2019, 45: 39–46
Mihalik SJ, Michaliszyn SF, de las Heras J, Bacha F, Lee SJ, Chace DH, DeJesus VR, Vockley J, Arslanian SA. Diabetes Care, 2012, 35: 605–611
Gall WE, Beebe K, Lawton KA, Adam KP, Mitchell MW, Nakhle PJ, Ryals JA, Milburn MV, Nannipieri M, Camastra S, Natali A, Ferrannini E, Federici M. PLoS ONE, 2010, 5: e10883
Nowak C, Hetty S, Salihovic S, Castillejo-Lopez C, Ganna A, Cook NL, Broeckling CD, Prenni JE, Shen X, Giedraitis V, Ärnlöv J, Lind L, Berne C, Sundström J, Fall T, Ingelsson E. Sci Rep, 2018, 8: 8691
Foghsgaard S, Andreasen C, Vedtofte L, Andersen ES, Bahne E, Strandberg C, Buhl T, Holst JJ, Svare JA, Clausen TD, Mathiesen ER, Damm P, Gluud LL, Knop FK, Vilsbøll T. Diabetes Care, 2017, 40: 109–116
Lekva T, Godang K, Michelsen AE, Qvigstad E, Normann KR, Norwitz ER, Aukrust P, Henriksen T, Bollerslev J, Roland MCP, Ueland T. Sci Rep, 2018, 8: 13392
Acknowledgements
We are grateful to all the participants in this study and Prof. Shau-Ku Huang at Shenzhen University for his valuable comments and suggestions. Dr. Simon Wang at the Language Centre of HKBU has improved the linguistic presentation of the manuscript. This work was supported by the National Natural Science Foundation of China (21437002) and the General Research Fund (12319716) from Research Grants Council of Hong Kong.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Zhao, H., Li, H., Zheng, Y. et al. Association of altered serum acylcarnitine levels in early pregnancy and risk of gestational diabetes mellitus. Sci. China Chem. 63, 126–134 (2020). https://doi.org/10.1007/s11426-019-9580-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11426-019-9580-2