Abstract
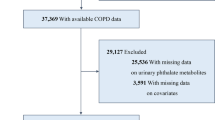
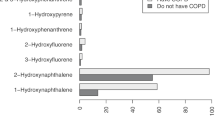
Although existing epidemiological studies have reported the relationship between single polycyclic aromatic hydrocarbon (PAH) exposure and chronic obstructive pulmonary disease (COPD), little is known about the impact of PAH mixture exposure on COPD. Therefore, we aimed to evaluate the associations of single and mixed exposures to PAHs with COPD in US adults using data from NHANES 2013–2016 by fitting three statistical methods, including multiple logistic regression, Bayesian kernel machine regression (BKMR), and quantile-based g-computation (qgcomp) models. This study included 1836 participants aged 40 and older. Multiple logistic regression showed that 2-FLU, 1-PHE, 1-PYR, and 2&3-PHE increased the risk of COPD after adjusting for all covariates. The BKMR model identified positive trends between PAH mixture and the risk of COPD in all adults and males when all PAHs were at or above their 55th percentile compared to all PAHs at their 50th percentile. The qgcomp model suggested that PAH co-exposure increased the risk of COPD (OR:1.44, 95%CI:1.09, 1.90) when each quartile increased in PAH mixture concentration, with 2-FLU having the highest weight. The combined impact also be observed in men. In conclusion, PAHs co-exposure was associated with a higher risk of COPD, especially in males, with the positive impact of 2-FLU being the most important.





Similar content being viewed by others
Data Availability
The data used in this study were obtained for free from NHANES.
References
Abdel-Shafy HI, Mansour M (2016) A review on polycyclic aromatic hydrocarbons: source, environmental impact, effect on human health and remediation. Egypt J Pet 25:107–123
Alhamdow A, Zettergren A, Kull I, Hallberg J, Andersson N, Ekstrom S, Berglund M, Wheelock CE, Essig YJ, Krais AM, Georgelis A, Lindh CH, Melen E, Bergstrom A (2021) Low-level exposure to polycyclic aromatic hydrocarbons is associated with reduced lung function among Swedish young adults. Environ Res 197:111169
Alshaarawy O, Zhu M, Ducatman A, Conway B, Andrew ME (2013) Polycyclic aromatic hydrocarbon biomarkers and serum markers of inflammation. A positive association that is more evident in men. Environ Res 126:98–104
Barnes PJ, Shapiro SD, Pauwels RA (2003) Chronic obstructive pulmonary disease: molecular and cellular mechanisms. Eur Respir J 22:672–688
Barnes PJ (2016) Sex differences in chronic obstructive pulmonary disease mechanisms. Am J Respir Crit Care Med 193:813–814
Bayman EO, Dexter F (2021) Multicollinearity in logistic regression models. Anesth Analg 133:362–365
Bentayeb M, Norback D, Bednarek M, Bernard A, Cai G, Cerrai S, Eleftheriou KK, Gratziou C, Holst GJ, Lavaud F, Nasilowski J, Sestini P, Sarno G, Sigsgaard T, Wieslander G, Zielinski J, Viegi G, Annesi-Maesano I, Study G (2015) Indoor air quality, ventilation and respiratory health in elderly residents living in nursing homes in Europe. Eur Respir J 45:1228–38
Bobb JF, Valeri L, Claus Henn B, Christiani DC, Wright RO, Mazumdar M, Godleski JJ, Coull BA (2015) Bayesian kernel machine regression for estimating the health effects of multi-pollutant mixtures. Biostatistics 16:493–508
Burstyn I, Boffetta P, Heederik D, Partanen T, Kromhout H, Svane O, Langard S, Frentzel-Beyme R, Kauppinen T, Stucker I, Shaham J, Ahrens W, Cenee S, Ferro G, Heikkila P, Hooiveld M, Johansen C, Randem BG, Schill W (2003) Mortality from obstructive lung diseases and exposure to polycyclic aromatic hydrocarbons among asphalt workers. Am J Epidemiol 158:468–478
Cao L, Zhou Y, Tan A, Shi T, Zhu C, Xiao L, Zhang Z, Yang S, Mu G, Wang X, Wang D, Ma J, Chen W (2020) Oxidative damage mediates the association between polycyclic aromatic hydrocarbon exposure and lung function. Environ Health 19:75
Carratt SA, Kovalchuk N, Ding X, Van Winkle LS (2019) Metabolism and lung toxicity of inhaled naphthalene: effects of postnatal age and sex. Toxicol Sci 170:536–548
Caspard H, Ambrose CS, Tran TN, Chipps BE, Zeiger RS (2020) Associations between individual characteristics and blood eosinophil counts in adults with asthma or COPD. J Allergy Clin Immunol Pract 8:1606-1613 e1
Chen M, Yang T, Meng X, Sun T (2015) Azithromycin attenuates cigarette smoke extract-induced oxidative stress injury in human alveolar epithelial cells. Mol Med Rep 11:3414–3422
Chichester CH, Buckpitt AR, Chang A, Plopper CG (1994) Metabolism and cytotoxicity of naphthalene and its metabolites in isolated murine Clara cells. Mol Pharmacol 45:664–672
Christenson SA, Smith BM, Bafadhel M, Putcha N (2022) Chronic obstructive pulmonary disease. Lancet 399:2227–2242
Faerk G, Colak Y, Afzal S, Nordestgaard BG (2018) Low concentrations of 25-hydroxyvitamin D and long-term prognosis of COPD: a prospective cohort study. Eur J Epidemiol 33:567–577
Fei Q, Weng X, Liu K, Liu S, Chen J, Guo X, Jing C (2022) The relationship between metal exposure and chronic obstructive pulmonary disease in the general US population: NHANES 2015–2016. Int J Environ Res Public Health 19(4):2085
Gao P, da Silva E, Hou L, Denslow ND, Xiang P, Ma LQ (2018) Human exposure to polycyclic aromatic hydrocarbons: metabolomics perspective. Environ Int 119:466–477
Gearhart-Serna LM, Tacam M Jr, Slotkin TA, Devi GR (2021) Analysis of polycyclic aromatic hydrocarbon intake in the US adult population from NHANES 2005–2014 identifies vulnerable subpopulations, suggests interaction between tobacco smoke exposure and sociodemographic factors. Environ Res 201:111614
Gordon SB et al (2014) Respiratory risks from household air pollution in low and middle income countries. Lancet Respir Med 2:823–860
Hudson-Hanley B, Smit E, Branscum A, Hystad P, Kile ML (2021) Trends in urinary metabolites of polycyclic aromatic hydrocarbons (PAHs) in the non-smoking US population, NHANES 2001-2014. Chemosphere 276:130211
Hwang J, Xu C, Grunsted P, Agnew RJ, Malone TR, Clifton S, Thompson K, Xu X (2022) Urinary Metabolites of Polycyclic Aromatic Hydrocarbons in Firefighters: a systematic review and meta-analysis. Int J Environ Res Public Health 19
Ibrahimou B, Azim SI, Sun N (2019) Interaction between blood lead level and chronic obstructive pulmonary disease (COPD) on risk of heart attack or stroke: USA NHANES, 2013–2014. Pulm Pharmacol Ther 58:101805
Jin X, Hua Q, Liu Y, Wu Z, Xu D, Ren Q, Zhao W, Guo X (2021) Organ and tissue-specific distribution of selected polycyclic aromatic hydrocarbons (PAHs) in ApoE-KO mouse. Environ Pollut 286:117219
Jones B, Donovan C, Liu G, Gomez HM, Chimankar V, Harrison CL, Wiegman CH, Adcock IM, Knight DA, Hirota JA, Hansbro PM (2017) Animal models of COPD: what do they tell us? Respirology 22:21–32
Kaluza J, Larsson SC, Orsini N, Linden A, Wolk A (2017) Fruit and vegetable consumption and risk of COPD: a prospective cohort study of men. Thorax 72:500–509
Kaluza J, Harris HR, Linden A, Wolk A (2019) Alcohol consumption and risk of chronic obstructive pulmonary disease: a prospective cohort study of men. Am J Epidemiol 188:907–916
Keil AP, Buckley JP, O’Brien KM, Ferguson KK, Zhao S, White AJ (2020) A quantile-based g-computation approach to addressing the effects of exposure mixtures. Environ Health Perspect 128:47004
Labaki WW, Rosenberg SR (2020) Chronic obstructive pulmonary disease. Ann Intern Med 173:ITC17–ITC32
Lag M, Ovrevik J, Refsnes M, Holme JA (2020) Potential role of polycyclic aromatic hydrocarbons in air pollution-induced non-malignant respiratory diseases. Respir Res 21:299
Li J, Qin C, Lv J, Guo Y, Bian Z, Zhou W, Hu J, Zhang Y, Chen J, Cao W, Yu C, Li L (2019) Solid fuel use and incident COPD in Chinese adults: findings from the China Kadoorie Biobank. Environ Health Perspect 127:57008
Li J, Li X, Xia Y, Fan H, Fan D, Xi X, Ye Q, Zhu Y, Xiao C (2021a) Subgroup analysis of the relationship between polycyclic aromatic hydrocarbons and rheumatoid arthritis: data from the National Health and Nutrition Examination Survey, 2003–2014. Sci Total Environ 775:145841
Li X, Zhong Y, He W, Huang S, Li Q, Guo C, Ma S, Li G, Yu Y (2021b) Co-exposure and health risks of parabens, bisphenols, triclosan, phthalate metabolites and hydroxyl polycyclic aromatic hydrocarbons based on simultaneous detection in urine samples from guangzhou. South China Environ Pollut 272:115990
Li Z, Sandau CD, Romanoff LC, Caudill SP, Sjodin A, Needham LL, Patterson DG Jr (2008) Concentration and profile of 22 urinary polycyclic aromatic hydrocarbon metabolites in the US population. Environ Res 107:320–331
Liang H, Wu X, Yao H, Weng X, Liu S, Chen J, Li Y, Wu Y, Wen L, Chen Q, Jing C (2022) Association of urinary metabolites of non-persistent pesticides with serum sex hormones among the US females: NHANES 2013–2014. Chemosphere 300:134577
Liu H, Tan X, Liu Z, Ma X, Zheng Y, Zhu B, Zheng G, Hu Y, Fang L, Hong G (2021a) Association between diet-related inflammation and COPD: findings from NHANES III. Front Nutr 8:732099
Liu J, Chen X, Qiu X, Zhang H, Lu X, Li H, Chen W, Zhang L, Que C, Zhu T (2021b) Association between exposure to polycyclic aromatic hydrocarbons and lipid peroxidation in patients with chronic obstructive pulmonary disease. Sci Total Environ 780:146660
Liu S, Ben X, Liang H, Fei Q, Guo X, Weng X, Wu Y, Wen L, Wang R, Chen J, Jing C (2021c) Association of acrylamide hemoglobin biomarkers with chronic obstructive pulmonary disease in the general population in the US: NHANES 2013–2016. Food Funct 12:12765–12773
Manisalidis I, Stavropoulou E, Stavropoulos A, Bezirtzoglou E (2020) Environmental and health impacts of air pollution: a review. Front Public Health 8:14
Matera MG, Ora J, Calzetta L, Rogliani P, Cazzola M (2021) Sex differences in COPD management. Expert Rev Clin Pharmacol 14:323–332
Moorthy B, Chu C, Carlin DJ (2015) Polycyclic aromatic hydrocarbons: from metabolism to lung cancer. Toxicol Sci 145:5–15
Mosher CL, Nanna MG, Jawitz OK, Raman V, Farrow NE, Aleem S, Casaburi R, MacIntyre NR, Palmer SM, Myers ER (2022) Cost-effectiveness of pulmonary rehabilitation among US adults with chronic obstructive pulmonary disease. JAMA Netw Open 5:e2218189
Negewo NA, Gibson PG, McDonald VM (2015) COPD and its comorbidities: impact, measurement and mechanisms. Respirology 20:1160–1171
Nwaozuzu CC, Partick-Iwuanyanwu KC, Abah SO (2021) Systematic review of exposure to polycyclic aromatic hydrocarbons and obstructive lung disease. J Health Pollut 11:210903
Oliver JR, Kushwah R, Wu J, Cutz E, Yeger H, Waddell TK, Hu J (2009) Gender differences in pulmonary regenerative response to naphthalene-induced bronchiolar epithelial cell injury. Cell Prolif 42:672–687
Pathak U, Gupta NC, Suri JC (2020) Risk of COPD due to indoor air pollution from biomass cooking fuel: a systematic review and meta-analysis. Int J Environ Health Res 30:75–88
Rabe KF, Watz H (2017) Chronic obstructive pulmonary disease. Lancet 389:1931–1940
Raherison C, Girodet PO (2009) Epidemiology of COPD. Eur Respir Rev 18:213–221
Rahman HH, Niemann D, Munson-McGee SH (2022) Association between environmental toxic metals, arsenic and polycyclic aromatic hydrocarbons and chronic obstructive pulmonary disease in the US adult population. Environ Sci Pollut Res Int 29:54507–54517
Rosario Filho NA, Urrutia-Pereira M, D’Amato G, Cecchi L, Ansotegui IJ, Galan C, Pomes A, Murrieta-Aguttes M, Caraballo L, Rouadi P, Chong-Neto HJ, Peden DB (2021) Air pollution and indoor settings. World Allergy Organ J 14:100499
Salvi S (2014) Tobacco smoking and environmental risk factors for chronic obstructive pulmonary disease. Clin Chest Med 35:17–27
Shang T, Zhao LJ, Pei LI, Zeng XY, Zhi-Qiang Y (2019) Determination of 10 kinds of monohydroxylated polycyclic aromatic hydrocarbons in human urine by supported liquid extraction followed by liquid chromatography- tandem mass spectrometry Chin J Anal Chem
Sheikh K, Coxson HO, Parraga G (2016) This is what COPD looks like. Respirology 21:224–236
Shen J, Gao S (2008) A solution to separation and multicollinearity in multiple logistic regression. J Data Sci 6:515–531
Sin DD, Cohen SB, Day A, Coxson H, Pare PD (2007) Understanding the biological differences in susceptibility to chronic obstructive pulmonary disease between men and women. Proc Am Thorac Soc 4:671–674
Smith JN, Gaither KA, Pande P (2022) Competitive metabolism of polycyclic aromatic hydrocarbons (PAHs): an assessment using in vitro metabolism and physiologically based pharmacokinetic (PBPK) modeling. Int J Environ Res Public Health 19
Stading R, Gastelum G, Chu C, Jiang W, Moorthy B (2021) Molecular mechanisms of pulmonary carcinogenesis by polycyclic aromatic hydrocarbons (PAHs): implications for human lung cancer. Semin Cancer Biol 76:3–16
Sun L, Ye Z, Ling Y, Cai S, Xu J, Fan C, Zhong Y, Shen Q, Li Y (2020) Relationship between polycyclic aromatic hydrocarbons and rheumatoid arthritis in US general population, NHANES 2003–2012. Sci Total Environ 704:135294
Tam A, Morrish D, Wadsworth S, Dorscheid D, Man SF, Sin DD (2011) The role of female hormones on lung function in chronic lung diseases. BMC Womens Health 11:24
Tian J, Zhou F, Zhang XG, Wang HY, Peng SH, Li X, Cao J, Zhang H (2022) Experience of physical activity in patients with COPD: a systematic review and qualitative meta-synthesis. Geriatr Nurs 47:211–219
Tooker BC, Quinn K, Armstrong M, Bauer AK, Reisdorph N (2021) Comparing the effects of an exposure to a polycyclic aromatic hydrocarbon mixture versus individual polycyclic aromatic hydrocarbons during monocyte to macrophage differentiation: mixture exposure results in altered immune metrics. J Appl Toxicol 41:1568–1583
Van Winkle LS, Gunderson AD, Shimizu JA, Baker GL, Brown CD (2002) Gender differences in naphthalene metabolism and naphthalene-induced acute lung injury. Am J Physiol Lung Cell Mol Physiol 282:L1122–L1134
Vogel CFA, Van Winkle LS, Esser C, Haarmann-Stemmann T (2020) The aryl hydrocarbon receptor as a target of environmental stressors - implications for pollution mediated stress and inflammatory responses. Redox Biol 34:101530
Vogelmeier CF, Roman-Rodriguez M, Singh D, Han MK, Rodriguez-Roisin R, Ferguson GT (2020) Goals of COPD treatment: focus on symptoms and exacerbations. Respir Med 166:105938
Wang S, Bai Y, Deng Q, Chen Z, Dai J, Li X, Zhang W, Zhang X, He M, Wu T, Guo H (2016) Polycyclic aromatic hydrocarbons exposure and lung function decline among coke-oven workers: a four-year follow-up study. Environ Res 150:14–22
Wang Y, Meng L, Pittman EN, Etheredge A, Hubbard K, Trinidad DA, Kato K, Ye X, Calafat AM (2017) Quantification of urinary mono-hydroxylated metabolites of polycyclic aromatic hydrocarbons by on-line solid phase extraction-high performance liquid chromatography-tandem mass spectrometry. Anal Bioanal Chem 409:931–937
Webber EM, Lin JS, Thomas RG (2022) Screening for chronic obstructive pulmonary disease: updated evidence report and systematic review for the US Preventive Services Task Force. JAMA 327:1812–1816
World Health Organization (2019) Global health estimates: leading causes of death. Cause-specific mortality 2000–2019
Yang L, Wang WC, Lung SC, Sun Z, Chen C, Chen JK, Zou Q, Lin YH, Lin CH (2017) Polycyclic aromatic hydrocarbons are associated with increased risk of chronic obstructive pulmonary disease during haze events in China. Sci Total Environ 574:1649–1658
Yu G, Jin M, Huang Y, Aimuzi R, Zheng T, Nian M, Tian Y, Wang W, Luo Z, Shen L, Wang X, Du Q, Xu W, Zhang J, Shanghai Birth Cohort S (2021) Environmental exposure to perfluoroalkyl substances in early pregnancy, maternal glucose homeostasis and the risk of gestational diabetes: a prospective cohort study. Environ Int 156:106621
Zhou Y, Zou Y, Li X, Chen S, Zhao Z, He F, Zou W, Luo Q, Li W, Pan Y, Deng X, Wang X, Qiu R, Liu S, Zheng J, Zhong N, Ran P (2014) Lung function and incidence of chronic obstructive pulmonary disease after improved cooking fuels and kitchen ventilation: a 9-year prospective cohort study. PLoS Med 11:e1001621
Zysman M, Raherison-Semjen C (2021) Women’s COPD. Front Med (Lausanne) 8:600107
Acknowledgements
We acknowledged all participants involved in our analysis and the staff of the National Center for Health Statistics at the CDC who designed, collected, and managed the NHANES data.
Author information
Authors and Affiliations
Contributions
Lin Wen, Xiaosong Ben, and Zhiyu Yang: formal analysis, writing (original draft and reviewing and editing), conceptualization, and methodology
Yingying Wu and Yuxuan Tan: software, validation, and visualization
Qian Chen, Huanzhu Liang, and Yexin Li: data curation and validation
Xiaomei Wu, Shan Liu, Xueqiong Weng, and Dan Tian: software and investigation
Chunxia Jing: resources, validation, supervision, writing (reviewing and editing), and project administration
Corresponding author
Ethics declarations
Ethics approval and consent to participate
The NHANES agreement has been reviewed and approved by the NCHS Research Ethics Committee. All participants provided written informed consent prior to participation.
Consent for publication
The manuscript is approved by all authors for publication.
Competing interests
The authors declare no competing interests.
Additional information
Responsible Editor: Lotfi Aleya
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wen, L., Ben, X., Yang, Z. et al. Association between co-exposure of polycyclic aromatic hydrocarbons and chronic obstructive pulmonary disease among the US adults: results from the 2013–2016 National Health and Nutrition Examination Survey. Environ Sci Pollut Res 30, 62981–62992 (2023). https://doi.org/10.1007/s11356-023-26413-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11356-023-26413-7