Abstract
Introduction
Oral microflora is a well-orchestrated and acts as a sequential defense mechanism for any infection related to oral disease. Chronic periodontitis is a disease of a microbial challenge to symbiosis and homeostasis. Periodontal surgery is the most promising cure with repair process during periodontal regeneration. It has an encouraging outcome in terms of early recovery biomarkers.
Objective
Saliva of periodontal surgery subjects with the chronic periodontitis have been evaluated by 1H NMR spectroscopy in search of possible early metabolic differences that could be obtained in order to see the eradication of disease which favours the symbiotic condition.
Method
The study employed 1H NMR spectroscopy on 176 human saliva samples in search of distinctive differences and their spectral data were further subjected to multivariate and quantitative analysis.
Result
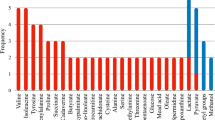
The 1H NMR study of periodontal surgery samples shows clear demarcation and profound metabolic differences when compared with the diseased condition. Several metabolites such as lactate, ethanol, succinate, and glutamate were found to be of higher significance in periodontal surgery in contrast to chronic periodontitis subjects. The PLS-DA model of the studied group resulted in R2 of 0.83 and Q2 of 0.70.
Conclusion
Significant metabolites could be considered as early repair markers for chronic periodontitis disease as they are being restored to achieve symbiosis. The study, therefore, concluded the early recovery process of the diseased subjects with the restoration of possible metabolomic profile similar to the healthy controls.
Graphic abstract






Similar content being viewed by others
Abbreviations
- CPMG:
-
Carr-purcell-meiboom-gill
- NMR:
-
Nuclear magnetic resonance
- NOESY:
-
Nuclear overhauser effect spectroscopy
- PCA:
-
Principal component analysis
- PLS-DA:
-
Partial least square discriminant analysis
- SD:
-
Standard deviation
- SPSS:
-
Statistical package for social science
- TSP:
-
Trimethylsilyl propionate
- VIP:
-
Variables importance in projection
- ROC:
-
Receiver operating characteristic curve
References
Aimetti, M., Cacciatore, S., Graziano, A., & Tenori, L. (2012). Metabonomic analysis of saliva reveals generalized chronic periodontitis signature. Metabolomics, 8(3), 465–474.
Andrei, M., Dinischiotu, A., Didilescu, A. C., Ionita, D., & Demetrescu, I. (2017). Periodontal materials and cell biology for guided tissue and bone regeneration. Annals of Anatomy-Anatomischer Anzeiger, 216, 164–169.
Bharti, S. K., & Roy, R. (2012). Quantitative 1H NMR spectroscopy. TrAC, Trends in Analytical Chemistry, 35, 5–26.
Chandra, A., Yadav, O. P., Narula, S., & Dutta, A. (2016). Epidemiology of periodontal diseases in Indian population since last decade. Journal of International Society of Preventive & Community Dentistry, 6(2), 91.
Chenomx, N. M. R. (2015). Suite. Edmonton: Chenomx Inc.
Chukkapalli, S. S., & Lele, T. P. (2018). Periodontal cell mechanotransduction. Open Biology, 8(9), 180053.
Dame, Z. T., Aziat, F., Mandal, R., Krishnamurthy, R., Bouatra, S., Borzouie, S., et al. (2015). The human saliva metabolome. Metabolomics, 11(6), 1864–1883.
Foresta, C., Ruzza, G., Mioni, R., Guarneri, G., Gribaldo, R., Meneghello, A., et al. (1984). Osteoporosis and decline of gonadal function in the elderly male. Hormones, 19(1), 18–22.
Fosdick, L., & Piez, K. (1953). Chemical studies in periodontal disease: X. Paper chromatographic investigation of the putrefaction associated with periodontitis. Journal of Dental Research, 32(1), 87–100.
García-Villaescusa, A., Morales-Tatay, J. M., Monleón-Salvadó, D., González-Darder, J. M., Bellot-Arcis, C., & Almerich-Silla, J. M. (2018). Using NMR in saliva to identify possible biomarkers of glioblastoma and chronic periodontitis. PLoS ONE, 13(2), e0188710.
Gardner, A., Parkes, H. G., Carpenter, G. H., & So, P.-W. (2018). Developing and standardizing a protocol for quantitative proton nuclear magnetic resonance (1H NMR) spectroscopy of saliva. Journal of Proteome Research, 17(4), 1521–1531.
Gharbia, S. E., & Shah, H. N. (1991). Pathways of glutamate catabolism among Fusobacterium species. Microbiology, 137(5), 1201–1206.
Higham, S., & Edgar, W. (1989). Effects of Parafilm® and cheese chewing on human dental plaque pH and metabolism. Caries Research, 23(1), 42–48.
Kaner, D., Soudan, M., Zhao, H., Gaßmann, G., Schönhauser, A., & Friedmann, A. (2017). Early healing events after periodontal surgery: Observations on soft tissue healing, microcirculation, and wound fluid cytokine levels. International Journal of Molecular Sciences, 18(2), 283.
Kertesz, M. A. (2000). Riding the sulfur cycle–metabolism of sulfonates and sulfate esters in Gram-negative bacteria. FEMS Microbiology Reviews, 24(2), 135–175.
Kilian, M., Chapple, I. L. C., Hannig, M., Marsh, P. D., Meuric, V., Pedersen, A. M. L., et al. (2016). The oral microbiome–an update for oral healthcare professionals. British Dental Journal, 221(10), 657.
Kim, J. J., Kim, C. J., & Camargo, P. M. (2013). Salivary biomarkers in the diagnosis of periodontal diseases. Journal of the California Dental Association, 41(2), 119.
Kolenbrander, P. E., & London, J. (1993). Adhere today, here tomorrow: Oral bacterial adherence. Journal of Bacteriology, 175(11), 3247.
Kornman, K. S., Page, R. C., & Tonetti, M. S. (1997). The host response to the microbial challenge in periodontitis: Assembling the players. Periodontology, 14(1), 33–53.
Markley, J. L., Anderson, M. E., Cui, Q., Eghbalnia, H. R., Lewis, I. A., Hegeman, A. D., et al. (2007). New bioinformatics resources for metabolomics. Biocomputing, 2007, 157–168.
Marsh, P. D., Do, T., Beighton, D., & Devine, D. A. (2016). Influence of saliva on the oral microbiota. Periodontology, 70(1), 80–92.
Melcher, A. (1976). On the repair potential of periodontal tissues. Journal of Periodontology, 47(5), 256–260.
Mombelli, A. (2018). Microbial colonization of the periodontal pocket and its significance for periodontal therapy. Periodontology, 76(1), 85–96.
Omahony, S., Clarke, G., Borre, Y., Dinan, T., & Cryan, J. (2015). Serotonin, tryptophan metabolism and the brain-gut-microbiome axis. Behavioural Brain Research, 277, 32–48.
Page, R. C., & Kornman, K. S. (1997). The pathogenesis of human periodontitis: An introduction. Periodontology, 14(1), 9–11.
Page, R. C., & Schroeder, H. E. (1976). Pathogenesis of inflammatory periodontal disease. A summary of current work. Laboratory Investigation: A Journal of Technical Methods and Pathology, 34(3), 235–249.
Ratcliff, P. A., & Johnson, P. W. (1999). The relationship between oral malodor, gingivitis, and periodontitis. A review. Journal of Periodontology, 70(5), 485–489.
Reynolds, J. J., & Meikle, M. C. (1997). Mechanisms of connective tissue matrix destruction in periodontitis. Periodontology, 14(1), 144–157.
Singh, M. P., Saxena, M., Saimbi, C. S., Arif, J. M., & Roy, R. (2017). Metabolic profiling by 1H NMR spectroscopy of saliva shows clear distinction between control and diseased case of periodontitis. Metabolomics, 13(11), 137.
Susin, C., Fiorini, T., Lee, J., De Stefano, J. A., Dickinson, D. P., & Wikesjö, U. M. (2015). Wound healing following surgical and regenerative periodontal therapy. Periodontology, 68(1), 83–98.
Takahashi, N. (2005). Microbial ecosystem in the oral cavity: Metabolic diversity in an ecological niche and its relationship with oral diseases. International Congress Series. Amsterdam: Elsevier.
Takahashi, N., & Yamada, T. (2000). Pathways for amino acid metabolism by Prevotella intermedia and Prevotella nigrescens. Oral Microbiology and Immunology, 15(2), 96–102.
van der Ploeg, J. R., Eichhorn, E., & Leisinger, T. (2001). Sulfonate-sulfur metabolism and its regulation in Escherichia coli. Archives of Microbiology, 176(1–2), 1–8.
Wishart, D. S., Knox, C., Guo, A. C., Eisner, R., Young, N., Gautam, B., et al. (2009). HMDB: A knowledgebase for the human metabolome. Nucleic Acids Research, 37, D603.
Acknowledgements
The authors are thankful for the grant funded by ICMR, New Delhi (Budget Allotment letter no.-5/4/2-7-12-NCD-II). Manvendra Pratap Singh also expresses his gratitude for the award of the fellowship. Manuscript Communication Number: IU/R&D/2018-MCN000453.
Funding
The authors are thankful for the Grant funded by ICMR, New Delhi (Budget Allotment letter no.-5/4/2-7-12-NCD-II).
Author information
Authors and Affiliations
Contributions
MS, CSS, and RR designed the study. MPS has conducted the experiments. MPS, CSS and RR analyzed the data. The initial draft was written by MPS. CSS, MHS, and RR edited and revised the paper. Project administration of the study has carried under CSS and RR. All authors carefully read and agree to be accountable for all aspects of the work.
Corresponding authors
Ethics declarations
Conflict of interest
The authors have no potential conflict of interest. The disclosure of a potential conflict of interest in the prescribed format has been obtained from all the authors.
Ethical approval
The study was ethically approved and the work was performed in strict accordance with the guidelines of Institutional Ethical Committee of the institute. The selected patients were fully informed and their consents were taken well before the investigations (Ethical approval No.- B-07: CBMR/EMP/IEC/3/26-02-2011). The authors: Manvendra Pratap Singh, Mona Saxena, Charanjit S. Saimbi, Mohammed Haris Siddiqui, and Raja Roy are aware of ethical policy.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Singh, M.P., Saxena, M., Saimbi, C.S. et al. Post-periodontal surgery propounds early repair salivary biomarkers by 1H NMR based metabolomics. Metabolomics 15, 141 (2019). https://doi.org/10.1007/s11306-019-1593-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11306-019-1593-3