Abstract
Objective
To investigate the correlation among sleep disorders, physical frailty, and depression in elderly patients with chronic kidney disease (CKD), and to explore the mediating role of depression.
Methods
This was a cross-sectional study, simple sampling was used to investigate the elderly CKD patients from one tertiary hospital in Shanghai. Those CKD patients who were diagnosed as CKD1-5 phase and were admitted to the Renal Medicine Ward from January to June 2022 and provided formal consent were considered for inclusion in our study. They were investigated with frailty phenotype (FP), Pittsburgh sleep quality index (PSQI), Center for Epidemiological Studies Depression Scale (CES-D), and self-made general information questionnaire. Linear regression was used to assess the associations between the variables, before this, PROCESS v4.1 was used to transform PSQI, CES-D and FP score to improve its normality, and conduct intermediary analysis. A difference of p < 0.05 was statistically significant.
Results
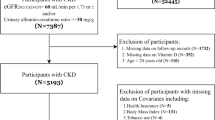
A total of 504 elderly patients with CKD completed the questionnaire survey, aged 60–91. The incidence of sleep disorders among elderly patients with CKD was 60%, and the incidence of physical frailty was 18%. The depression was positively correlated with physical frailty (r = 0.418, p < 0.01) and sleep disorders (r = 0.541, p < 0.01). Physical frailty was positively correlated with sleep disorders (r = 0.320, p < 0.01). The depression plays a significant mediating role in the model, and the effect ratio of depression is 52%.
Conclusion
Depression is a mediating variable between sleep disorders and frailty. Improving depression in elderly patients with CKD accompanied by sleep disorders can help delay the occurrence of frailty.

Similar content being viewed by others
Data availability
The original contributions presented in the study are included in the article/supplementary material, further inquiries can be directed to the corresponding author.
References
Balomenos V, Ntanasi E, Anastasiou CA, Charisis S, Velonakis G, Karavasilis E, Scarmeas N (2021) Association between sleep disturbances and frailty: evidence from a population-based study. J Am Med Dir Assoc 22(3):551–558. https://doi.org/10.1016/j.jamda.2020.08.012
Bao YP, Han Y, Ma J, Wang RJ, Shi L, Wang TY, Lu L (2017) Cooccurrence and bidirectional prediction of sleep disturbances and depression in older adults: Meta-analysis and systematic review. Neurosci Biobehav Rev 75:257–273. https://doi.org/10.1016/j.neubiorev.2017.01.032
Borges MK, Aprahamian I, Romanini CV, Oliveira FM, Mingardi S, Lima NA, Oude VR (2021) Depression as a determinant of frailty in late life. Aging Ment Health 25(12):2279–2285. https://doi.org/10.1080/13607863.2020.1857689
Cohen CI, Benyaminov R, Rahman M, Ngu D, Reinhardt M (2023) Frailty: a Multidimensional biopsychosocial syndrome. Med Clin North Am 107(1):183–197. https://doi.org/10.1016/j.mcna.2022.04.006
Duan D, Yang L, Zhang M, Song X, Ren W (2021) Depression and associated factors in Chinese patients with chronic kidney disease without dialysis: a cross-sectional study. Front Public Health. https://doi.org/10.3389/fpubh.2021.605651
Gallione C, Mastroianni G, Suardi B (2019) Sleep disorders and frailty status in older people: a narrative review]. Prof Inferm 72(1):13–24. https://doi.org/10.7429/pi.2019.721013
Griffiths J, Seesen M, Sirikul W, Siviroj P (2023) Malnutrition, depression, poor sleep quality, and difficulty falling asleep at night are associated with a higher risk of cognitive frailty in older adults during the COVID-19 restrictions. Nutrients. https://doi.org/10.3390/nu15132849
Han Q, Liu B, Lin S, Li J, Liang P, Fu S, Yang Q (2021) Pittsburgh sleep quality index score predicts all-cause mortality in Chinese dialysis patients. Int Urol Nephrol 53(11):2369–2376. https://doi.org/10.1007/s11255-021-02842-6
Hill AL, Flicker L, Hankey GJ, Golledge J, Yeap BB, Almeida OP (2022) Disrupted sleep and risk of depression in later life: a prospective cohort study with extended follow up and a systematic review and meta-analysis. J Affect Disord 309:314–323. https://doi.org/10.1016/j.jad.2022.04.133
Hou Y, Lu Q, Lu Z, Xu F, Cao Z, Li S, Wang Y (2022) Frailty phenotype and mortality: a prospective cohort study. J Am Med Dir Assoc 23(1):182–185. https://doi.org/10.1016/j.jamda.2021.08.030
Jiao J, Wang Y, Zhu C, Li F, Zhu M, Wen X, Xu T (2020) Prevalence and associated factors for frailty among elder patients in China: a multicentre cross-sectional study. BMC Geriatr 20(1):100. https://doi.org/10.1186/s12877-020-1496-1
Jones J (2020) Depression: a side effect of CKD. Clin J Am Soc Nephrol 15(12):1692–1693. https://doi.org/10.2215/CJN.16411020
Kagee A, Bantjes J, Saal W, Sterley A (2020) Predicting caseness of major depressive disorder using the center for epidemiological studies depression scale (CESD-R) among patients receiving HIV care. Gen Hosp Psychiatry 67:70–76. https://doi.org/10.1016/j.genhosppsych.2020.09.005
Kim DS, Kim SW, Gil HW (2022) Emotional and cognitive changes in chronic kidney disease. Korean J Intern Med 37(3):489–501. https://doi.org/10.3904/kjim.2021.492
Li Y, Ning Y, Shen B, Shi Y, Song N, Fang Y, Ding X (2023) Temporal trends in prevalence and mortality for chronic kidney disease in China from 1990 to 2019: an analysis of the Global Burden of Disease Study 2019. Clin Kidney J 16(2):312–321. https://doi.org/10.1093/ckj/sfac218
Liu M, Hou T, Nkimbeng M, Li Y, Taylor JL, Sun X, Szanton SL (2021) Associations between symptoms of pain, insomnia and depression, and frailty in older adults: A cross-sectional analysis of a cohort study. Int J Nurs Stud 117:103873. https://doi.org/10.1016/j.ijnurstu.2021.103873
Liu T, Zhan Y, Wang Y, Li Q, Mao H (2021) Obstructive sleep apnea syndrome and risk of renal impairment: a systematic review and meta-analysis with trial sequential analysis. Sleep Breath 25(1):17–27. https://doi.org/10.1007/s11325-020-02090-5
Liu X, Wang C, Qiao X, Si H, Jin Y (2021) Sleep quality, depression and frailty among Chinese community-dwelling older adults. Geriatr Nurs 42(3):714–720. https://doi.org/10.1016/j.gerinurse.2021.02.020
Lorenz EC, Kennedy CC, Rule AD, LeBrasseur NK, Kirkland JL, Hickson LJ (2021) Frailty in CKD and transplantation. Kidney Int Rep 6(9):2270–2280. https://doi.org/10.1016/j.ekir.2021.05.025
Maștaleru A, Abdulan IM, Ștefăniu R, Lefter N, Sandu IA, Pîslaru AI, Ilie AC (2022) Relationship between frailty and depression in a population from North-Eastern Romania. Int J Environ Res Public Health. https://doi.org/10.3390/ijerph19095731
Monaghan TF, Epstein MR, Bliwise DL, Michelson KP, Wu ZD, Lazar JM, Weiss JP (2020) Time of peak nocturnal diuresis rate between men with secondary nocturnal polyuria versus nocturnal polyuria syndrome. Neurourol Urodyn 39(2):785–792. https://doi.org/10.1002/nau.24283
Moreno-Tamayo K, Manrique-Espinoza B, Rosas-Carrasco O, Pérez-Moreno A, Salinas-Rodríguez A (2017) Sleep complaints are associated with frailty in Mexican older adults in a rural setting. Geriatr Gerontol Int 17(12):2573–2578. https://doi.org/10.1111/ggi.13111
Natale P, Ruospo M, Saglimbene VM, Palmer SC, Strippoli GF (2019) Interventions for improving sleep quality in people with chronic kidney disease. Cochrane Database Syst Rev 5(5):12625. https://doi.org/10.1002/14651858.CD012625.pub2
Park SH, Yu HY (2021) How useful is the center for epidemiologic studies depression scale in screening for depression in adults? An updated systematic review and meta-analysis. Psychiatry Res 302:114037. https://doi.org/10.1016/j.psychres.2021.114037
Ramezani KA, Aghebati N, Mohajer S, Ghavami V (2020) Effect of guided imagery along with breathing relaxation on sleep quality of the elderly patients under abdominal surgery: a randomized clinical trial. Holist Nurs Pract 34(6):334–344. https://doi.org/10.1097/HNP.0000000000000415
Riley RD, Collins GS, Ensor J, Archer L, Booth S, Mozumder SI, Snell K (2022) Minimum sample size calculations for external validation of a clinical prediction model with a time-to-event outcome. Stat Med 41(7):1280–1295. https://doi.org/10.1002/sim.9275
Safarpour Y, Vaziri ND, Jabbari B (2023) restless legs syndrome in chronic kidney disease- a systematic review. Tremor Other Hyperkinet Mov (NY) 13:10. https://doi.org/10.5334/tohm.752
Santos D, Ferreira L, Pallone JM, Ottaviani AC, Santos-Orlandi AA, Pavarini S, Orlandi FS (2022) Association between frailty and depression among hemodialysis patients: a cross-sectional study. Sao Paulo Med J 140(3):406–411. https://doi.org/10.1590/1516-3180.2021.0556.R1.14092021
Şentürk A, Tekinsoy KP (2018) The effect of lavender oil application via inhalation pathway on hemodialysis patients’ anxiety level and sleep quality. Holist Nurs Pract 32(6):324–335. https://doi.org/10.1097/HNP.0000000000000292
Shirazian S (2019) Depression in CKD: understanding the mechanisms of disease. Kidney Int Rep 4(2):189–190. https://doi.org/10.1016/j.ekir.2018.11.013
Soysal P, Veronese N, Thompson T, Kahl KG, Fernandes BS, Prina AM, Stubbs B (2017) Relationship between depression and frailty in older adults: A systematic review and meta-analysis. Ageing Res Rev 36:78–87. https://doi.org/10.1016/j.arr.2017.03.005
Stevens KI, Graham-Brown M, Lees JS (2023) Let’s get physical: considering and overcoming the barriers to physical activity in CKD. Nephrol Dial Transplant 38(6):1405–1407. https://doi.org/10.1093/ndt/gfad002
Strojnik V, Gabrovec B (2019) Management of frailty at individual level: narrative review of physical activity from the european perspective of joint action on frailty - Ja Advantage. Zdr Varst 58(2):84–90. https://doi.org/10.2478/sjph-2019-0011
Voulgaris A, Marrone O, Bonsignore MR, Steiropoulos P (2019) Chronic kidney disease in patients with obstructive sleep apnea. A narrative review. Sleep Med Rev 47:74–89. https://doi.org/10.1016/j.smrv.2019.07.001
Xu X, Zhou X, Liu W, Ma Q, Deng X, Fang R (2022) Evaluation of the correlation between frailty and sleep quality among elderly patients with osteoporosis: a cross-sectional study. BMC Geriatr 22(1):599. https://doi.org/10.1186/s12877-022-03285-z
Zhao Y, Lu Y, Zhao W, Wang Y, Ge M (2021) Long sleep duration is associated with cognitive frailty among older community-dwelling adults: results from West China Health and aging trend study. BMC Geriatr 21(1):608. https://doi.org/10.1186/s12877-021-02455-9. ([Journal Article; Research Support, Non-U.S. Gov't])
Zitser J, Allen IE, Falgàs N, Le MM, Neylan TC, Kramer JH, Walsh CM (2022) Pittsburgh sleep quality index (PSQI) responses are modulated by total sleep time and wake after sleep onset in healthy older adults. PLoS ONE 17(6):e270095. https://doi.org/10.1371/journal.pone.0270095
Zou C, Chen S, Shen J, Zheng X, Wang L, Guan L, Yang Y (2018) Prevalence and associated factors of depressive symptoms among elderly inpatients of a Chinese tertiary hospital. Clin Interv Aging 13:1755–1762. https://doi.org/10.2147/CIA.S170346
Author information
Authors and Affiliations
Contributions
YW and DS: conceptualization and visualization. JW and PJ: methodology. PJ: software. YW, DS, JW, XL, SP, and PJ: validation, investigation, and supervision. YW, JW, PJ, SP, and DS: formal analysis. DS: resources. YW, SP, and XL: data curation. YW, SP, JW and DS: writing—original draft preparation and writing—review and editing. PJ, SP, and DS: project administration and funding acquisition. All authors contributed to the article and approved the submitted version.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wang, Y., Peng, S., Wu, J. et al. The role of depression between sleep disorders and frailty among elderly patients with chronic kidney disease (CKD) in China: a cross-sectional study. Int Urol Nephrol 56, 2085–2092 (2024). https://doi.org/10.1007/s11255-023-03910-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-023-03910-9