Abstract
Purpose
Prognostic nutritional index (PNI), a composite indicator of inflammation and nutritional status, has recently been recognized as an independent prognostic marker for chronic kidney disease (CKD). We aimed to investigate PNI and its relationship with mortality in elderly patients with CKD.
Methods
Three hundred and fifty-nine patients over the age of 80 years with stage 3–4 CKD were enrolled in this retrospective study. PNI was used to assess the nutritional status of the patients. Patients were divided into two different groups as deceased and survived and as low PNI (< 39) and high PNI (≥ 39) according to median value of PNI.
Results
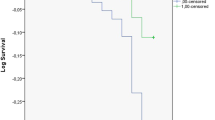
The mean age of the patients was 85.7 ± 3.7 years. One hundred and ninety-five (54.3%) patients died during follow-up. Multivariate analysis revealed that male gender, PNI, proteinuria, and diabetes mellitus (DM) were independent predictors of mortality in elderly patients with CKD. When patients with low PNI were compared to those with high PNI, initiation of dialysis and mortality rate were significantly higher whereas albumin, hemoglobin and lymphocyte count were lower. Pearson correlation analysis showed that PNI was significantly correlated with albumin (r = 1.000, p < 0.001), hemoglobin (r = 0.340, p < 0.001) and eGFR (r = 0.123, p = 0.020). Hemoglobin was an independent predictor of PNI in multivariate analysis.
Conclusion
In this study, we observed that PNI was significantly associated with mortality over the age of 80 years in patients with CKD and can be used to monitor nutritional status in this patient population.
Similar content being viewed by others
Data availability
All relevant data were presented in the manuscript.
References
Lutz W, Sanderson W, Scherbov S (2008) The coming acceleration of global population ageing. Nature 451(7179):716–719. https://doi.org/10.1038/nature06516 (Epub 2008 Jan 20 PMID: 18204438)
United Nations, Department of Economic and Social Affairs, Population Division (2020) World Population Ageing 2020 Highlights: Living arrangements of older persons. https://www.un.org/development/desa/pd/sites/www.un.org.development.desa.pd/files/files/documents/2020/Sep/un_pop_2020_pf_ageing_10_key_messages.pdf. Accessed 28 July 2021
He W, Goodkind D, Kowal P (2015) An aging world. United States Census Bureau, Washington (DC), pp 138–149
Süleymanlar G, Utaş C, Arinsoy T, Ateş K, Altun B, Altiparmak MR et al (2011) A population-based survey of Chronic REnal Disease in Turkey–the CREDIT study. Nephrol Dial Transplant 26(6):1862–1871. https://doi.org/10.1093/ndt/gfq656 (Epub 2010 Nov 4. PMID: 21051501; PMCID: PMC3107767)
Manjunath G, Tighiouart H, Coresh J, Macleod B, Salem DN, Griffith JL et al (2003) Level of kidney function as a risk factor for cardiovascular outcomes in the elderly. Kidney Int 63(3):1121–1129. https://doi.org/10.1046/j.1523-1755.2003.00838.x (PMID: 12631096)
Drion I, van Hateren KJ, Joosten H, Alkhalaf A, Groenier KH, Kleefstra N et al (2012) Chronic kidney disease and mortality risk among older patients with type 2 diabetes mellitus (ZODIAC-24). Age Ageing 41(3):345–350. https://doi.org/10.1093/ageing/afs002 (Epub 2012 Feb 6 PMID: 22314695)
GBD Chronic Kidney Disease Collaboration (2020) Global, regional, and national burden of chronic kidney disease, 1990–2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet 395(10225):709–733. https://doi.org/10.1016/S0140-6736(20)30045-3 (Epub 2020 Feb 13. PMID: 32061315; PMCID: PMC7049905)
Fanetti G, Polesel J, Fratta E, Muraro E, Lupato V, Alfieri S et al (2021) Prognostic nutritional index predicts toxicity in head and neck cancer patients treated with definitive radiotherapy in association with chemotherapy. Nutrients 13(4):1277. https://doi.org/10.3390/nu13041277 (PMID:33924581;PMCID:PMC8070136)
Yuan K, Zhu S, Wang H, Chen J, Zhang X, Xu P et al (2021) Association between malnutrition and long-term mortality in older adults with ischemic stroke. Clin Nutr 40(5):2535–2542. https://doi.org/10.1016/j.clnu.2021.04.018 (Epub ahead of print. PMID: 33932800)
Efe SC, Karagöz A, Doğan C, Bayram Z, Cakmak EO, Kalkan S et al (2021) Prognostic significance of malnutrition scores in elderly patients for prediction of contrast induced acute kidney injury. Int J Clin Pract 28:e14274. https://doi.org/10.1111/ijcp.14274
Zhang H, Tao Y, Wang Z, Lu J (2019) Evaluation of nutritional status and prognostic impact assessed by the prognostic nutritional index in children with chronic kidney disease. Medicine (Baltimore) 98(34):e16713. https://doi.org/10.1097/MD.0000000000016713 (PMID:31441844;PMCID:PMC6716681)
Windahl K, EQUAL study investigators, Irving GF, Almquist T, Lidén MK, Stenvinkel P, Chesnaye NC, Drechsler C, Szymczak M, Krajewska M, Fu EL, Torino C, Porto G, Roderick P, Caskey FJ, Wanner C, Dekker FW, Jager KJ, Evans M (2021) Patient-reported measures and lifestyle are associated with deterioration in nutritional status in CKD stage 4–5: the EQUAL Cohort Study. J Ren Nutr. https://doi.org/10.1053/j.jrn.2021.03.006 (Epub ahead of print. PMID: 33931314)
Onodera T, Goseki N, Kosaki G (1984) Prognostic nutritional index in gastrointestinal surgery of malnourished cancer patients. Nihon Geka Gakkai Zasshi 85(9):1001–1005 (Japanese. PMID: 6438478)
Ahn SS, Jung SM, Song JJ, Park YB, Lee SW (2019) Prognostic nutritional index is associated with disease severity and relapse in ANCA-associated vasculitis. Int J Rheum Dis 22(5):797–804. https://doi.org/10.1111/1756-185X.13507 (Epub 2019 Feb 6 PMID: 30729693)
Peng F, Chen W, Zhou W, Li P, Niu H, Chen Y et al (2017) Low prognostic nutritional index associated with cardiovascular disease mortality in incident peritoneal dialysis patients. Int Urol Nephrol 49(6):1095–1101. https://doi.org/10.1007/s11255-017-1531-0 (Epub 2017 Feb 10 PMID: 28185108)
Kang SH, Cho KH, Park JW, Yoon KW, Do JY (2012) Onodera’s prognostic nutritional index as a risk factor for mortality in peritoneal dialysis patients. J Korean Med Sci 27(11):1354–1358. https://doi.org/10.3346/jkms.2012.27.11.1354 (Epub 2012 Oct 30. PMID: 23166417; PMCID: PMC3492670)
Oluseyi A, Enajite O (2016) Malnutrition in pre-dialysis chronic kidney disease patients in a teaching hospital in Southern Nigeria. Afr Health Sci 16(1):234–241. https://doi.org/10.4314/ahs.v16i1.31 (PMID:27358637;PMCID:PMC4915439)
Lawson JA, Lazarus R, Kelly JJ (2001) Prevalence and prognostic significance of malnutrition in chronic renal insufficiency. J Ren Nutr 11(1):16–22. https://doi.org/10.1016/s1051-2276(01)85914-8 (PMID: 11172449)
Kadiri Mel M, Nechba RB, Oualim Z (2011) Factors predicting malnutrition in hemodialysis patients. Saudi J Kidney Dis Transpl 22(4):695–704 (PMID: 21743213)
Cianciaruso B, Brunori G, Kopple JD, Traverso G, Panarello G, Enia G et al (1995) Crosssectional comparison of malnutrition in continuous ambulatory peritoneal dialysis and hemodialysis patients. Am J Kidney Dis 26(3):475–486. https://doi.org/10.1016/0272-6386(95)90494-8 (PMID: 7645556)
Tayyem RF, Mrayyan MT (2008) Assessing the prevalence of malnutrition in chronic kidney disease patients in Jordan. J Ren Nutr 18(2):202–209. https://doi.org/10.1053/j.jrn.2007.10.001 (PMID: 18267213)
Prakash J, Raja R, Mishra RN, Vohra R, Sharma N, Wani IA et al (2007) High prevalence of malnutrition and inflammation in undialyzed patients with chronic renal failure in developing countries: a single centre experience from eastern India. Ren Fail 29(7):811–816
Tan R, Long J, Fang S, Mai H, Lu W, Liu Y et al (2016) Nutritional risk screening in patients with chronic kidney disease. Asia Pac J Clin Nutr 25(2):249–256. https://doi.org/10.6133/apjcn.2016.25.2.24 (PMID: 27222407)
Hu Y, Cao Q, Wang H, Yang Y, Xiong Y, Li X et al (2021) Prognostic nutritional index predicts acute kidney injury and mortality of patients in the coronary care unit. Exp Ther Med 21(2):123. https://doi.org/10.3892/etm.2020.9555 (Epub 2020 Dec 3. PMID: 33335586; PMCID: PMC7739862)
Cai L, Yu J, Yu J, Peng Y, Ullah H, Yi C et al (2018) Prognostic value of inflammation-based prognostic scores on outcome in patients undergoing continuous ambulatory peritoneal dialysis. BMC Nephrol 19(1):297. https://doi.org/10.1186/s12882-018-1092-1 (PMID:30367618;PMCID:PMC6204053)
Kato A, Tsuji T, Sakao Y, Ohashi N, Yasuda H, Fujimoto T et al (2013) A comparison of systemic inflammation-based prognostic scores in patients on regular hemodialysis. Nephron Extra 3(1):91–100. https://doi.org/10.1159/000355148 (PMID:24403910;PMCID:PMC3884192)
Faller B, Beuscart JB, Frimat L (2013) Competing-risk analysis of death and dialysis initiation among elderly (≥ 80 years) newly referred to nephrologists: a French prospective study. BMC Nephrol 14:103. https://doi.org/10.1186/1471-2369-14-103 (PMID: 23659341; PMCID: PMC3662583)
Hickson M (2006) Malnutrition and ageing. Postgrad Med J 82(963):2–8. https://doi.org/10.1136/pgmj.2005.037564 (PMID:16397072;PMCID:PMC2563720)
Robertson RG, Montagnini M (2004) Geriatric failure to thrive. Am Fam Physician 70(2):343–350 (PMID: 15291092)
Hassan NK, Gillani SW, Kaoje AA, Fari FM, Elashmouny HM, Sulayman NM et al (2020) A clinical review on nutritional requirements and assessment for type 2 diabetes mellitus with chronic renal disease. Curr Diabetes Rev 16(9):922–930. https://doi.org/10.2174/1573399816666200211120402 (PMID: 32072916)
O’Hare AM, Choi AI, Bertenthal D, Bacchetti P, Garg AX, Kaufman JS et al (2007) Age affects outcomes in chronic kidney disease. J Am Soc Nephrol 18(10):2758–2765. https://doi.org/10.1681/ASN.2007040422 (Epub 2007 Sep 12 PMID: 17855638)
Ikizler TA, Cuppari L (2021) The 2020 updated KDOQI clinical practice guidelines for nutrition in chronic kidney disease. Blood Purif 2:1–5. https://doi.org/10.1159/000513698 (Epub ahead of print. PMID: 33652433)
Guligowska A, Corsonello A, Pigłowska M, Roller-Wirnsberger R, Wirnsberger G, Ärnlöv J, SCOPE investigators et al (2020) Association between kidney function, nutritional status and anthropometric measures in older people: the screening for CKD among Older People across Europe (SCOPE) study. BMC Geriatr 20(Suppl 1):366. https://doi.org/10.1186/s12877-020-01699-1 (PMID: 33008315; PMCID: PMC7531088)
Deschasse G, Lombrail P, Steenpass V, Couturier P, Gavazzi G (2014) Association entre lymphopénie et mortalité chez les sujets âgés admis en unité de médecine aiguë gériatrique [Association between lymphopenia of elderly patients and intrahospital mortality in a geriatric acute care unit]. Geriatr Psychol Neuropsychiatr Vieil 12(1):25–33. https://doi.org/10.1684/pnv.2014.0460 (PMID: 24647236)
Lin J, Tang W, Liu W, Yu F, Wu Y, Fang X et al (2020) Decreased B1 and B2 lymphocytes are associated with mortality in elderly patients with chronic kidney diseases. Front Med (Lausanne) 20(7):75. https://doi.org/10.3389/fmed.2020.00075.PMID:32266271;PMCID:PMC7098909
Xiang FF, Zhu JM, Cao XS, Shen B, Zou JZ, Liu ZH et al (2016) Lymphocyte depletion and subset alteration correlate to renal function in chronic kidney disease patients. Ren Fail 38(1):7–14. https://doi.org/10.3109/0886022X.2015.1106871 (Epub 2015 Nov 5 PMID: 26539739)
Bonilla-Palomas JL, Gámez-López AL, Moreno-Conde M, López-Ibáñez MC, Anguita-Sánchez M, de la Sacristana AG et al (2014) Hypoalbuminemia in acute heart failure patients: causes and its impact on hospital and long-term mortality. J Card Fail 20(5):350–358. https://doi.org/10.1016/j.cardfail.2014.01.016 (Epub 2014 Jan 28. PMID: 24486927)
Fock RA, Blatt SL, Beutler B, Pereira J, Tsujita M, de Barros FE et al (2010) Study of lymphocyte subpopulations in bone marrow in a model of protein-energy malnutrition. Nutrition 26(10):1021–1028. https://doi.org/10.1016/j.nut.2009.08.026 (Epub 2009 Dec 29 PMID: 20036516)
Nitsch D, Grams M, Sang Y, Black C, Cirillo M, Djurdjev O et al (2013) Chronic Kidney Disease Prognosis Consortium. Associations of estimated glomerular filtration rate and albuminuria with mortality and renal failure by sex: a meta-analysis. BMJ 346:f324. https://doi.org/10.1136/bmj.f324 (PMID: 23360717; PMCID: PMC3558410)
Pérez-Torres A, González García ME, Ossorio-González M, Álvarez García L, Bajo MA, Del Peso G et al (2021) The Effect of nutritional interventions on long-term patient survival in advanced chronic kidney disease. Nutrients 13(2):621. https://doi.org/10.3390/nu13020621 (PMID:33672996;PMCID:PMC7918910)
Hoshino J (2021) Renal rehabilitation: exercise intervention and nutritional support in dialysis patients. Nutrients 13(5):1444. https://doi.org/10.3390/nu13051444 (PMID:33923264;PMCID:PMC8145577)
de Waal D, Heaslip E, Callas P (2016) Medical nutrition therapy for chronic kidney disease improves biomarkers and slows time to dialysis. J Ren Nutr 26(1):1–9. https://doi.org/10.1053/j.jrn.2015.08.002 (Epub 2015 Sep 26 PMID: 26391566)
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
All authors have contributed significantly, and all authors are in agreement with the content of the manuscript. Each author has participated sufficiently in the work to take public responsibility for the content which include: conception or design, or analysis and interpretation of data, or both; drafting the article or revising it; providing intellectual content of critical importance to the work described and, final approval of the version to be published.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there is no conflict of interest.
Ethics approval
The study design was approved by the institutional review board of Marmara University Hospital (Protocol no: 09.2021.636) and complied with the Declaration of Helsinki.
Consent to participate
All participants provided written informed consent.
Consent for publication
All participants provided informed consent to publish.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Barutcu Atas, D., Tugcu, M., Asicioglu, E. et al. Prognostic nutritional index is a predictor of mortality in elderly patients with chronic kidney disease. Int Urol Nephrol 54, 1155–1162 (2022). https://doi.org/10.1007/s11255-021-03002-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-021-03002-6