Abstract
Purpose
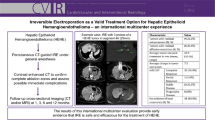
Laser interstitial thermal therapy (LITT) is a minimally invasive cytoreductive treatment option for brain tumors with a risk of vascular injury from catheter placement or thermal energy. This may be of concern with deep-seated tumors that have surrounding end-artery perforators and critical microvasculature. The purpose of this study was to assess the risk of distal ischemia following LITT for deep-seated perivascular brain tumors.
Methods
A retrospective review of a multi-institution database was used to identify patients who underwent LITT between 2013 and 2022 for tumors located within the insula, thalamus, basal ganglia, and anterior perforated substance. Demographic, clinical and volumetric tumor characteristics were collected. The primary outcome was radiographic evidence of distal ischemia on post-ablation magnetic resonance imaging (MRI).
Results
61 LITT ablations for deep-seated perivascular brain tumors were performed. Of the tumors treated, 24 (39%) were low-grade gliomas, 32 (52%) were high-grade gliomas, and 5 (8%) were metastatic. The principal location included 31 (51%) insular, 14 (23%) thalamic, 13 (21%) basal ganglia, and 3 (5%) anterior perforated substance tumors. The average tumor size was 19.6 cm3 with a mean ablation volume of 11.1 cm3. The median extent of ablation was 92% (IQR 30%, 100%). Two patients developed symptomatic intracerebral hemorrhage after LITT. No patient had radiographic evidence of distal ischemia on post-operative diffusion weighted imaging.
Conclusion
We demonstrate that LITT for deep-seated perivascular brain tumors has minimal ischemic risks and is a feasible cytoreductive treatment option for otherwise difficult to access intracranial tumors.



Similar content being viewed by others
Data availability
The dataset utilized during this study is available from the corresponding author upon reasonable request.
Abbreviations
- CSF:
-
Cerebral spinal fluid
- KPS:
-
Karnofsky performance status
- LITT:
-
Laser interstitial thermal therapy
- MRI:
-
Magnetic resonance imaging
- DWI:
-
Diffusion weighted imaging
- OS:
-
Overall survival
- PFS:
-
Progression free survival
References
Kamath AA, Friedman DD, Akbari SHA et al (2019) Glioblastoma treated with magnetic resonance imaging-guided laser interstitial thermal therapy: safety, efficacy, and outcomes. Neurosurgery 84(4):836–843. https://doi.org/10.1093/neuros/nyy375
Patel P, Patel NV, Danish SF (2016) Intracranial MR-guided laser-induced thermal therapy: single-center experience with the visualase thermal therapy system. J Neurosurg 125(4):853–860. https://doi.org/10.3171/2015.7.JNS15244
Sloan AE, Ahluwalia MS, Valerio-Pascua J et al (2013) Results of the neuroblate system first-in-humans phase I clinical trial for recurrent glioblastoma: clinical article. J Neurosurg 118(6):1202–1219. https://doi.org/10.3171/2013.1.JNS1291
Mohammadi AM, Hawasli AH, Rodriguez A et al (2014) The role of laser interstitial thermal therapy in enhancing progression-free survival of difficult-to-access high-grade gliomas: a multicenter study. Cancer Med 3(4):971–979. https://doi.org/10.1002/cam4.266
Thomas JG, Rao G, Kew Y, Prabhu SS (2016) Laser interstitial thermal therapy for newly diagnosed and recurrent glioblastoma. Neurosurg Focus 41(4):E12. https://doi.org/10.3171/2016.7.FOCUS16234
Willie JT, Laxpati NG, Drane DL et al (2014) Real-time magnetic resonance-guided stereotactic laser amygdalohippocampotomy for mesial temporal lobe epilepsy. Neurosurgery 74(6):569–584. https://doi.org/10.1227/NEU.0000000000000343
Pruitt R, Gamble A, Black K, Schulder M, Mehta AD (2017) Complication avoidance in laser interstitial thermal therapy: lessons learned. J Neurosurg 126(4):1238–1245. https://doi.org/10.3171/2016.3.JNS152147
Gempt J, Förschler A, Buchmann N et al (2013) Postoperative ischemic changes following resection of newly diagnosed and recurrent gliomas and their clinical relevance. J Neurosurg 118(4):801–808. https://doi.org/10.3171/2012.12.JNS12125
Hou Z, Huang Z, Li Z et al (2022) Incidence of ischemic complications and technical nuances of arteries preservation for insular gliomas resection. Front Surg 9:956872. https://doi.org/10.3389/fsurg.2022.956872
Patel B, Yang PH, Kim AH (2020) The effect of thermal therapy on the blood-brain barrier and blood-tumor barrier. Int J Hyperth 37(2):35–43. https://doi.org/10.1080/02656736.2020.1783461
Salem U, Kumar VA, Madewell JE et al (2019) Neurosurgical applications of MRI guided laser interstitial thermal therapy (LITT). Cancer Imaging 19(1):65. https://doi.org/10.1186/s40644-019-0250-4
Holste KG, Orringer DA (2020) Laser interstitial thermal therapy. Neuro-Oncol Adv 2(1):vdz035. https://doi.org/10.1093/noajnl/vdz035
Fadel HA, Haider S, Pawloski JA et al (2022) Laser interstitial thermal therapy for first-line treatment of surgically accessible recurrent glioblastoma: outcomes compared with a surgical cohort. Neurosurgery 91(5):701–709. https://doi.org/10.1227/neu.0000000000002093
Loit MP, Rheault F, Gayat E et al (2019) Hotspots of small strokes in glioma surgery: an overlooked risk? Acta Neurochir (Wien) 161(1):91–98. https://doi.org/10.1007/s00701-018-3717-3
Schaller C, Zentner J (1998) Vasospastic reactions in response to the transsylvian approach. Surg Neurol 49(2):170–175. https://doi.org/10.1016/s0090-3019(97)00283-8
Gempt J, Krieg SM, Hüttinger S et al (2013) Postoperative ischemic changes after glioma resection identified by diffusion-weighted magnetic resonance imaging and their association with intraoperative motor evoked potentials. J Neurosurg 119(4):829–836. https://doi.org/10.3171/2013.5.JNS121981
Hwang BY, Eremiev A, Palla A et al (2021) Association of intraoperative end-tidal carbon dioxide level with ablation volume during magnetic resonance–guided laser interstitial thermal therapy for mesial temporal lobe epilepsy. J Neurosurg 137(2):427–433. https://doi.org/10.3171/2021.9.JNS211554
Paul A, Paul A (2018) Computational study of photo-thermal ablation of large blood vessel embedded tumor using localized injection of gold nanoshells. J Therm Biol 78:329–342. https://doi.org/10.1016/j.jtherbio.2018.10.021
Beechar VB, Prabhu SS, Bastos D et al (2018) Volumetric response of progressing Post-SRS lesions treated with laser interstitial thermal therapy. J Neurooncol 137(1):57–65. https://doi.org/10.1007/s11060-017-2694-3
Zeller S, Kaye J, Jumah F et al (2021) Current applications and safety profile of laser interstitial thermal therapy in the pediatric population: a systematic review of the literature. J Neurosurg Pediatr 1(aop):1–8. https://doi.org/10.3171/2021.2.PEDS20721
Nishimura N, Schaffer CB, Friedman B, Tsai PS, Lyden PD, Kleinfeld D (2006) Targeted insult to subsurface cortical blood vessels using ultrashort laser pulses: three models of stroke. Nat Methods 3(2):99–108. https://doi.org/10.1038/nmeth844
Schwarzmaier HJ, Eickmeyer F, von Tempelhoff W et al (2006) MR-guided laser-induced interstitial thermotherapy of recurrent glioblastoma multiforme: preliminary results in 16 patients. Eur J Radiol 59(2):208–215. https://doi.org/10.1016/j.ejrad.2006.05.010
Montemurro N, Anania Y, Cagnazzo F, Perrini P (2020) Survival outcomes in patients with recurrent glioblastoma treated with laser interstitial thermal therapy (LITT): a systematic review. Clin Neurol Neurosurg 195:105942. https://doi.org/10.1016/j.clineuro.2020.105942
Shah AH, Burks JD, Buttrick SS, Debs L, Ivan ME, Komotar RJ (2019) Laser interstitial thermal therapy as a primary treatment for deep inaccessible gliomas. Neurosurgery 84(3):768–777. https://doi.org/10.1093/neuros/nyy238
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
Each author listed contributed to the study design. H.F., J.P., M.S. and S.H. each contributed to data collection, analysis, and draft revisions. R.K, E.L, A.M, M.I, A.R., S.K. and I.L provided commentary on the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Competing interest
The authors have no relevant financial or non-financial interests to disclose.
Ethical approval
This retrospective study was approved by the institutional review board (MRI Volumetrics of Patients Treated with Laser Ablation, IRB #9176) with a waiver of patient consent prior to data collection and analysis.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Reese, J.C., Fadel, H.A., Pawloski, J.A. et al. Laser interstitial thermal therapy for deep-seated perivascular brain tumors is not associated with distal ischemia. J Neurooncol 166, 265–272 (2024). https://doi.org/10.1007/s11060-023-04546-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-023-04546-6